Heavy Metal Toxicity
Original Editors - Chase Almgren from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Chase Almgren, Lucinda hampton, Kim Jackson, Admin, Elaine Lonnemann, 127.0.0.1, Wendy Walker and WikiSysop
Introduction[edit | edit source]
Heavy metal (HM) toxicity is a generic term for an above average level of metal in the blood which may result in undesirable side-effects.[1] Humans are exposed to HMs through inhalation, ingestion, or contact with the skin. Environmental pollution with HMs can result in contamination of air, water, sewage, seawater, waterways, and can accumulate in plants, crops, seafood, and meat and indirectly affect humans. Some occupations have increased risk for particular HMs exposure and toxicity[2].
Accumulating evidence suggests that all age groups and organs are susceptible to metal induced toxicity, although the impact on the central nervous system is more severe and long-lasting in both developing and adult human brain. There are no clinically proven treatments to those affected by heavy metal toxicity.[3]
- Heavy metal (HM) toxicity is underestimated in the community.
- Heavy metals can affect the nervous, pulmonary, cardiovascular, renal, skin, reproductive, and skeletal systems in varying degrees.
- Heavy metals cause harm to proteins like enzymes, DNA, membrane lipids, and disrupt normal cellular functions.
- Young children are affected more than adults.
- Affected pregnant women can pass on the toxic HMs to the developing fetus and produce much harm.
- The toxicity of HMs can be acute and chronic[2].
HMs and the Nervous System[edit | edit source]
The brain is sensitive to HMs and suffers a lot with contamination in comparison to the other parts of the body. If the exposure of heavy metals becomes prolonged, they will have deleterious effects on the nervous system. Heavy metals toxicity is responsible for many neurodegenerative diseases eg Alzheimer’s disease, Parkinson’s disease, amyotrophic lateral sclerosis, multiple sclerosis, and attention-deficit hypertensive disorders. There is data regarding the significant association or correlation between the exposure of heavy metals and neurotoxicity. This is deemed to be due to: oxidative stress; the participation of certain proteins/enzymes; the interruption in the normal secretion of neurotransmitters on account of heavy metal exposure. The resultant effects and intensity of diseases can be prevented by taking the adequate preventive measures[4].
Etiology[edit | edit source]
HMs are dense, naturally occurring elements that cause health hazards by accumulation in the environment and living beings.
- The common list of non-essential HM that cause toxicity includes Arsenic (As), Cadmium (Cd), Lead (Pb), Mercury (Hg)
- Those essential to humans in trace quantities for various cellular activities include: Cobalt (Co), Copper (Cu), chromium (Cr), Iron (Fe), Manganese (Mn), Molybdenum (Mo), Nickel (Ni), Selenium (Se) and Zinc (Zn).
Exposure to HMs can be natural or occupational.
Epidemiology[edit | edit source]
HM toxicity is worldwide.
- The incidence and magnitude of the toxicities of individual HMs vary with the geographical location, natural soil content, habits, customs, location of industries, regulatory measures to contain pollution, healthcare facilities to detect HM toxicity, and individual factors like nutritional status, and genetics.
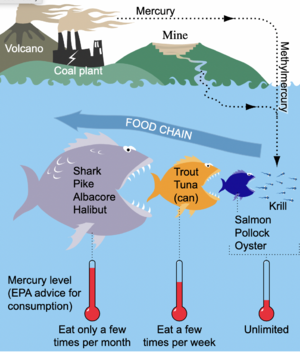
- When an HM is released into the air, water, or soil, it can be absorbed by plants, crops, consumed by cattle and fish, and finally, end up in humans to complete the food chain.
- Industrial and workplace exposure can result in HM toxicity by inhalation, ingestion, or skin contact[2].
Lead Toxicity[edit | edit source]
Common sources of lead which may be harmful to humans are lead based paints, soldered around the rims of food cans (more common outside of the United States), plumbing, older bath tubs, and imported dishware.[1] Occupational exposure to lead is one of the most prevalent overexposures. Industries with high potential exposures include construction work, most smelter operations, radiator repair shops, and firing ranges[2]. Lead particles may also travel through the air during older house renovation projects
- Young children need be ultra careful around lead based products as the minimal level to declare lead toxicity (10mg/dl) is smaller than that for adults(24mg/dl).[1] The blood-brain barrier is unformed in infants and lead readily diffuses across. Children and infants are commonly exposed to lead particles during floor activities, and through the hand-to-mouth stages of development.[1]
- Adults are more likely to be exposed to lead during the renovation of old houses, manufacturing of brass, bullets, solder, stained-glass/ pottery designs, and frequent use of metallic wick candles. [1][5]
Acute lead toxicity can cause gastrointestinal problems such as nausea, vomiting, loss of appetite, stomach cramps, and constipation. It can also cause sleeping problems, fatigue, mood changes, headache, joint/muscle aches, anemia, and a decreased sexual drive.
Long term problems with lead exposure include nervous system, genitourinary system, and blood-forming system problems. Chronic exposure to lead can lead to death[6].
Arsenic Toxicity[edit | edit source]
Common sources of exposure to higher-than-average levels of arsenic include near or in hazardous waste sites. Arsenic exposure may come from glass infiltrates, pesticides, wood preservatives, paints and during the process of smelting copper zinc, and lead. Exposure to high levels of arsenic can cause death.[1][5][2]
Long term effects of arsenic exposure include gross pigmentation with hyperkeratinization, wart formation, dermatitis, vasospasticity, Raynaud's phenomenon, decreased nerve conduction velocity, lung cancer, conjunctivitis, peripheral neuropathies, encephalopathy, laryngitis, bronchitis, rhinitis, and death[7].
Mercury Toxicity[edit | edit source]
Mercury exposure can be in the forms of inhalion, ingestion, or topically through the skin.[1] Common sources of mercury exposure include mining, production, and transportation of mercury, as well as mining and refining of gold and silver ores. High mercury exposure results in permanent nervous system and kidney damage. Another common source of mercury is through the food chain; one animal is exposed and passes it to the top of the food chain through ingestion. [2][1]
Short-term effects of mercury toxicity include lung damage, nausea, vomiting, diarrhea, hypertension, tachycardia, skin rashes, and eye irritation.
With chronic exposure to mercury, the nervous system is susceptible to damage. Brain and kidney damage is common with high levels of mercury exposure. Other common systemic side-effects are irritability, shyness, tremors, vision and hearing problems, and memory deficits[8].
Protection of the food chain from contamination by mercury is an important task in the protection of health of the human population.[9]
Characteristics/Clinical Presentation[edit | edit source]
Characteristics of heavy metal poisoning are vague as patients will present depending on the route and level of exposure.
- Acute exposure is usually dramatic in presentation. Inhalation of HMs causes respiratory symptoms, topical contamination, skin lesions, and ingestion mimics acute gastroenteritis or dysentery.
- Chronic exposure is more difficult to detect. Depending on the organ system involved, the symptoms will vary. Typical findings may be present only in selected cases, while the majority may be non-specific[2].[7]
Treatment[edit | edit source]
The patient is removed from toxic exposure. The HM may be hastened out of the body by gastric lavage, activated charcoal, and skin decontamination. Supportive care can be in the form of intravenous fluids, oxygen, ventilatory, and circulatory support as needed. In severe cases, hemodialysis, plasma exchanges, and extracorporeal membrane oxygenation (ECMO) may be necessary.
- The emphasis should be on prevention. In certain circumstances, total prevention is impossible, and minimization of contamination should be the goal.
- The chelating agents used as a treatment in HM toxicity are not devoid of side-effects. Some metal ions are redistributed to other tissues like the brain and thereby increase neurotoxicity. Others chelate essential trace elements and produce a deficiency state while yet others can cause hepatotoxicity.[2]
Associated Co-morbidities[edit | edit source]
The following co-morbidities are not found with all types of heavy metal toxicity but are common:[10]
- Attention Deficit Disorder
- Alzheimer's disease
- Amyotrophic Lateral Sclerosis (Lou Gehrig's Disease)
- Asthma
- Arthritis
- Autism Spectrum disorders
- Autoimmune disorders
- Candidiasis (Yeast Infection)
- Chronic Fatigue Syndrome
- Epilepsy
- Fibromyalgia
- Gulf War Syndrome
- Hypertension
- Insomnia
- Infertility
- Kidney disease
- Liver disease
- Multiple Sclerosis
- Parkinson's
- Schizophrenia
- Thyroid Disorders
Physical Therapy Management[edit | edit source]
Physical therapy has minimal effect on depleting heavy metals from the body. There is no current "best evidence" for the treatment of patients with heavy metal toxicity. Physical therapy is aimed towards management of side effects and associated co-morbidities of heavy metal toxicity.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Goodman CC, Fuller KS. Pathology clinical implications for the physical therapist. 3rd ed. St. Louis: Saunders Elsevier, 2009
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Rajkumar V, Gupta V. Heavy metal toxicity.2020 Available: https://www.ncbi.nlm.nih.gov/books/NBK560920/(accessed 1.4.2022)
- ↑ Kothapalli CR. Differential impact of heavy metals on neurotoxicity during development and in aging central nervous system. Current Opinion in Toxicology. 2021 Jun 1;26:33-8.Available:https://www.sciencedirect.com/science/article/abs/pii/S2468202021000164 (accessed 1.4.2022)
- ↑ Rehman Q, Rehman K, Akash MS. Heavy metals and neurological disorders: from exposure to preventive interventions. InEnvironmental contaminants and neurological disorders 2021 (pp. 69-87). Springer, Cham.Available: https://link.springer.com/chapter/10.1007/978-3-030-66376-6_4(accessed 1.4.2022)
- ↑ 5.0 5.1 Life Extension. Heavy Metal Toxicity. http://www.lef.org/protocols/prtcl-156.shtml. Accessed: March 31, 2011.
- ↑ United States Department of Labor Occupational Safety and Health Administration. Safety and Health Topics Lead. http://www.osha.gov/SLTC/lead/. Accessed: April 4, 2011.
- ↑ 7.0 7.1 Agency for toxic substances and disease registry. Toxicological profile for arsenic. http://www.atsdr.cdc.gov/toxprofiles/tp.asp?id=22&tid=3#bookmark07. Accessed: April 4, 2011
- ↑ Agency for toxic substances and disease registry. ToxFAQs for mercury. http://www.atsdr.cdc.gov/toxfaqs/TF.asp?id=113&tid=24. Accessed: April 4, 2011.
- ↑ Kimakova T, Kuzmova L, Nevolna Z, Bencko V. Fish and fish products as risk factors of mercury exposure. Annals of agricultural and environmental medicine. 2018 Sep 25;25(3):488-93.Available:https://pubmed.ncbi.nlm.nih.gov/30260185/ (accessed 1.4.2022)
- ↑ Even Better Health. Safe Detoxification for Heavy Metal Toxicity. http://www.evenbetterhealth.com/heavy-metal-poisoning.php. Accessed: April 4, 2011.