Epilepsy
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
Globally, epilepsy is one of the most common neurological diseases, particularly among children. Epilepsy is not a single disorder; it has many causes that share the hallmark of a seizure, when brain function is disrupted, often dramatically.
- When seizures remain isolated in just one part of the brain, they can be very small and can even pass by unnoticed.
- When seizures involve large parts of the brain, the consequent event is what people typically associate with an “epileptic fit”. ie person’s muscles stiffen, they lose consciousness and fall to the floor, and their body starts jerking rhythmically, these types of seizures are called “tonic-clonic” seizures[1]
Seizures and epilepsy have been documented since the earliest civilizations. Most individuals with epilepsy were thought to be possessed being thought that the gods “seized” a person at the time a convulsion[2].
- Epilepsy is characterized by unpredictable seizures and can cause other health problems.
- It is is a spectrum condition with a wide range of seizure types and control varying from person-to-person.
- Public misunderstandings of epilepsy cause challenges that are often worse than the seizures.[3]
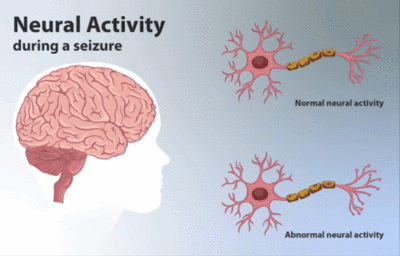
Image 1: Depiction of neural activity during a seizure. This has been shown in comparison to normal neural activity.
What is Epilepsy[edit | edit source]
Epilepsy is a chronic disorder, the hallmark of which is recurrent, unprovoked seizures. A person is diagnosed with epilepsy if they have two unprovoked seizures (or one unprovoked seizure with the likelihood of more) that were not caused by some known and reversible medical condition eg alcohol withdrawal, hypoglycemia.[3] Epilepsy means the same thing as "seizure disorders."
- A seizure is an abnormal, unregulated electrical discharge that occurs within the brain’s cortical gray matter and transiently interrupts normal brain function.
- A seizure typically causes altered awareness, abnormal sensations, focal involuntary movements, or convulsions (widespread violent involuntary contraction of voluntary muscles).[4]
- The mechanisms that allow the central nervous system to develop into a complex structure and the mechanisms that provide plasticity, which are so important to its ability to function in a changing environment, do not come without risk—the risk of epilepsy[2].
Image 2: Neural signaling in the human brain.
Etiology[edit | edit source]
The reason why epilepsy develops is not fully understood. Common causes of seizures vary by age of onset:
- Before age 2: Fever, hereditary or congenital neurologic disorders, birth injuries, and inherited or acquired metabolic disorders
- Ages 2 to 14: Idiopathic seizure disorders
- Adults: Cerebral trauma, alcohol withdrawal, tumors, strokes, and an unknown cause (in 50%)
- Older people: Tumors and strokes[4]
Image: Protective helmet for a baby with epilepsy.
Cerebral Palsy[edit | edit source]
According to the Centers for Disease Control and Prevention (CDC), around 35% of all children with cerebral palsy will experience seizures. There are different types of seizures, and the symptoms will depend upon what form the child experiences.
- Absence Seizures: Stare into space and have small and subtle body movements, such as eye blinking and lip smacking.
- Atonic Seizures:Temporary loss of muscle control and may collapse onto the floor without warning.
- Clonic Seizures:Marked by jerking muscle movement in the arms, face, and neck.
- Myoclonic Seizures:Temporary jerking movements in the arms and legs.
- Tonic-clonic Seizures:Most severe type of seizures, marked by body shakes, loss of consciousness, the body stiffening, and in some instances, loss of bladder control.[5]
Classification[edit | edit source]
There are more than 40 types of epilepsy, which are divided into two groups according to the site of seizure onset. In 2017, the International League Against Epilepsy (ILAE) developed a new classification system for seizures.
Initial classification is by type of onset:
- Generalized onset (seizures begin diffusely in the brain).
- Focal onset (seizures begin in a specific region of the brain and predominantly impact parts of the body controlled by the affected area)
- Unknown onset
All seizures are then classified (if possible) as
- Motor onset
- Nonmotor onset
Diagnosis[edit | edit source]
Diagnosing seizures and the type of epilepsy is like putting the pieces of a puzzle together and includes information from many people and different tests.
- Knowing if a person is having a seizure and diagnosing the type of seizure or epilepsy syndrome can be difficult.
- The treatment of seizures depends on an accurate diagnosis.
- Making sure a person has epilepsy and knowing what kind of epilepsy is a critical first step.
- What happens during a seizure is one of the most important pieces of information for accurate diagnosis.
Information gathered includes details of the medical history, blood tests, EEG tests, and brain imaging tests eg CT and MRI scans[3].
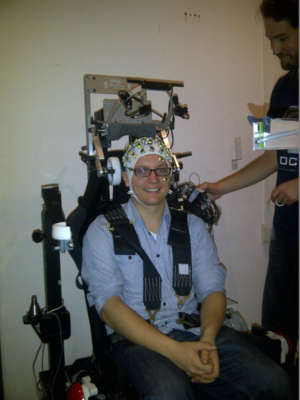
Image: EEG being performed on human volunteer. EEG is the key tool for the diagnosis of epilepsy. Surface EEG provides the best overview of the approximate location of the epileptogenic zone.[6]
Treatment[edit | edit source]
Saying someone has epilepsy is a little like saying that they’re sick. Its cause is diverse and can be from many things eg the result of a head injury, an inherited genetic condition, or any other disorder that affects the brain. In some cases, epilepsy is associated with other brain problems and intellectual disability. But mostly, people with epilepsy are normal between seizures and can participate in normal activities. If seizures are not controlled, then operating dangerous machines, like cars, or swimming unsupervised must be avoided[1].
Treatment involves:
- Elimination of the cause if possible
- Avoidance of or precautions during situations when loss of consciousness could be life threatening
- Drugs to control seizures
- Surgery if ≥ 2 drugs in therapeutic doses do not control seizures[4]
Most epilepsy is well controlled with medications. Options for treatment have expanded with new drugs available, more precise diagnosis based on sophisticated imaging, and better understanding of the mechanism of epilepsy in each individual patient. In some cases, very precise detection of brain lesions can allow for a surgical cure of epilepsy. Even devices used as brain implants have been developed that can control severe epilepsy[1].
Outlook for People with Epilepsy
- About 50 to 60% (5 to 6 out of every 10 people) will be seizure free after using the first seizure medication tried.
- A second seizure medication may help 11 to 20 out of every 100 people become seizure free. Adding more drugs usually doesn’t help the chance of seizure control.
- 25 out of every 100 adults will develop uncontrolled epilepsy.
- Others will have continued seizures and side effects, but we don’t know if other treatments may help.
- In children with new-onset seizures, 74 out of 100 become seizure free within 2 years. (Berg et al 2001)
- Uncontrolled epilepsy may be seen in 9 out of 100 children followed for a number of years
Physiotherapy[edit | edit source]
Physiotherapy Includes: Health Promotion and Education
People with epilepsy should include exercise as a complementary therapy not only for seizure control but also for non-seizure conditions such as physical health promotion and psychosocial adjustment and improvement in mental state. People with epilepsy should be encouraged to exercise and efforts should be made to remove any barriers to exercise. To reach these goals, support of health authorities, social workers, sport instructors, and campaigns to inform and stimulate patients to become more active are necessary.
- Exercise improves fitness, energy and mood and relieves stress.
- Improving overall health and wellbeing in this way can help reduce seizures and the impact of epilepsy for some people. It also makes people feel more in control of their health.
- Exercise releases ‘feel good’ hormones into the brain, helps to keep the muscles active, reduces fat levels in the body and increases oxygen flow to the brain. It can also increase bone density
- The neuroprotective and antiepileptogenic actions of exercise strengthen the role of exercise intervention as complementary non pharmacological treatment of epilepsy[7].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 The Conversation Epilepsy: sorting the myths from the facts of a common disorder https://theconversation.com/epilepsy-sorting-the-myths-from-the-facts-of-a-common-disorder-47276 (accessed 4.1.2021)
- ↑ 2.0 2.1 Scharfman HE. The neurobiology of epilepsy. Current neurology and neuroscience reports. 2007 Jul 1;7(4):348-54.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2492886/ (accessed 4.1.2021)
- ↑ 3.0 3.1 3.2 Epilepsy Foundation Epilepsy Available from: https://www.epilepsy.com/learn/about-epilepsy-basics/what-epilepsy (accessed 4.1.2021)
- ↑ 4.0 4.1 4.2 MSD manual Seizure disorder Available from:https://www.msdmanuals.com/en-au/professional/neurologic-disorders/seizure-disorders/seizure-disorders (accessed 4.1.2021)
- ↑ Cerebral Palsy and Associated Conditions
- ↑ Liman MN, Al Sawaf A. Epilepsy EEG. StatPearls [Internet]. 2020 Jun 14..Available from:https://www.ncbi.nlm.nih.gov/books/NBK558912/ (accessed 4.1.2021)
- ↑ YAKASAI AM. THE ROLE OF PHYSICAL THERAPY IN THE MANAGEMENT OF CHILDREN WITH EPILEPSY.Available from:https://www.numss.com/Thesis/ABDULSALAM%20MOHAMMED%20YAKASAI%20PHYSIOTHERAPY%20INTERVENTION%20IN%20CHILDREN%20WITH%20EPILEPSY.pdf (accessed 4.1.2021)