Blood Tests
Original Editor - John Mitchell
Top Contributors - Rachael Lowe, Scott Buxton, Lucinda hampton, Admin, Kim Jackson, Jin Yoo, Evan Thomas, Naomi O'Reilly, Mariam Hashem, WikiSysop, Adam Vallely Farrell and Mason Trauger
Introduction[edit | edit source]
Blood tests are one of the most common types of medical test. They have many uses, including assessing general health, checking for an infection, seeing how well specific organs are functioning and screening for certain genetic conditions.
Human blood contains thousands of different chemicals and molecules.
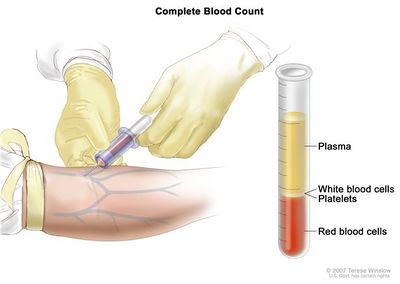
- If blood in a test tube is allowed to stand it separates out into blood cells and the support fluid called plasma. Some tests are done on the blood cells and others just on the plasma.
- Separating blood cells from the support fluids can be speeded up by spinning the test tube of blood in a centrifuge at high speed[1].
Use - to confirm or refute diagnosis
- Prognosis: risk factors
- Monitoring: progress & treatment
- Screening: subclinical presence of pathology
Interpretation
- Is it normal/different?
- Is it consistent with clinical findings?
4 Common “Panels” Ordered[edit | edit source]
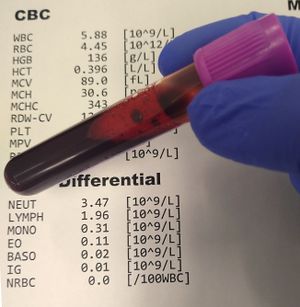
- Complete Blood Count (CBC) - a collection of tests related to the cells in your blood. It usually includes the following results:
- White blood cell count (WBCs): the number of white blood cells per microliter of blood
- Red blood cell count (RBCs): the number of red blood cells per microliter of blood
- Hemoglobin (Hgb): how many grams of this oxygen-carrying protein per deciliter of blood
- Hematocrit (Hct): the fraction of blood that is made up of red blood cells
- Mean corpuscular volume (MCV): the average size of red blood cells
- Platelet count (Plts): how many platelets (a smaller cell involved in clotting blood) per microliter of blood
Uses eg - Anemia may be diagnosed if the red blood cell count, hemoglobin, and hematocrit are lower than normal.
- The white blood cell count usually goes up if a person is fighting an infection. Some medications eg corticosteroids, can cause an increase in the white blood cell count.
- If several types of blood cells (i.e. red blood cells, white blood cells, and platelets) are low, this can be a sign of a problem with the bone marrow.
- Basic metabolic panel (basic electrolyte panel) - Common for electrolytes to be ordered as part of a panel of seven or eight measurements (“chem-7,”), usually includes:
- Sodium, Chloride and Potassium - Medication side-effects can cause electrolytes eg sodium or potassium to be either too high or too low. These electrolytes are often monitored when people take certain types of medications eg certain blood pressure medications, diuretics.
- Carbon dioxide (CO2) - Reflect the acidity of the blood. This can be affected by kidney function and by lung function. Severe infection can also change acid levels in the blood.
- Blood urea nitrogen (BUN) and Creatinine (often accompanied by an estimated “glomerular filtration rate,” or “eGFR”result) - Most commonly used to monitor kidney function. Both of these measurements can go up if kidney function is temporarily impaired (e.g. by dehydration or a medication side-effect) or chronically impaired.
- Glucose - Represent the amount of sugar in the blood. If they are higher than normal, this could be due to undiagnosed diabetes or inadequately controlled diabetes. If the glucose levels are on the low side ie hypoglycemia, it is often caused by diabetes medications, and may indicate a need to reduce the dosage of these drugs.
- Comprehensive metabolic panel - includes the items above in the basic metabolic panel, and includes an additional seven items ( sometimes referred to as a “chem-14” panel). Uses:
- Calcium - Calcium levels are usually regulated by the kidneys and by certain hormones ( not usually a good way to assess calcium intake or total calcium stores in the bones and body). High or low blood calcium levels can cause symptoms, including cognitive dysfunction, and usually indicate an underlying health problem. They can also be caused by certain types of medication.
- Total protein
- Albumin - Albumin is one of the key proteins in the bloodstream. It is synthesized by the liver. Low albumin levels may indicate a problem with the liver or a problem maintaining albumin in the bloodstream. Malnutrition may cause low albumin levels.
- Bilirubin (total) - Bilirubin is produced by the liver, and usually drains down the bile ducts and into the small intestine. Some bilirubin is also related to the breakdown of red blood cells. An increase in bilirubin can be caused by gallstones or another issue blocking the bile ducts.
- Alkaline phosphatase - Found throughout the body, but especially in bile ducts and also in bone. Higher levels are often caused by either a blockage in the liver or by a problem affecting bone metabolism.
- AST (aspartate aminotransferase) and ALT (alanine aminotransferase) - AST and ALT are enzymes contained in liver cells. An elevation in these enzymes often indicates a problem affecting the liver. This can be caused by medications or by a variety of other health conditions.
- Lipid (cholesterol) panel - measure the different types of cholesterol and related fats in the bloodstream. The panel usually includes:
- Total cholesterol
- High-density lipoprotein (HDL) cholesterol, sometimes known as “good” cholesterol
- Triglycerides
- Low-density lipoprotein (LDL) cholesterol, sometimes known as “bad” cholesterol
- LDL results are usually calculated, based on the other three results
People are often asked to fast before having their cholesterol checked. This is because triglycerides can increase after eating, and this can cause a falsely low LDL to be calculated. Recent finding however concluded that in most cases, it’s not necessary for people to fast; it’s inconvenient and only makes a small difference in test results.
What the lipid panel is often used for - usually to evaluate cardiovascular risk
- Higher than normal total or LDL cholesterol levels are sometimes treated with a medication eg statins. They can also be reduced by dietary changes[2]
Other Tests[edit | edit source]
- Tests related to thyroid function - used to screen for thyroid disorders, or to help calibrate the dosage of thyroid replacement medications. The most commonly used tests are:
- Thyroid stimulating hormone (TSH)
- Free thyroxine (“free T4” or FT4)
- In more complicated situations, other tests related to thyroid function may also be ordered.
- Tests related to vitamin B12 levels - measure the serum levels of vitamin B12 and provide information as to whether the level is adequate for the body’s needs. The two tests involved are Vitamin B12 and Methylmalonic acid
- Vitamin B12 deficiency is quite common in older adults, and can be related to common problems such as fatigue, memory problems, and walking difficulties.
- Methylmalonic acid levels in the body are related to vitamin B12 levels, and can help confirm a vitamin B12 deficiency.
- Glycated hemoglobin ( Hemoglobin A1C) - Used to monitor the blood sugar control of people with diabetes.
- Whereas a blood glucose level (which can be checked by fingerstick or as part of a basic metabolic panel) reports the blood gluose level at a specific moment in time, a hemoglobin A1C reflects how high a person’s blood sugar has been, on average, over the prior three months.
- Prothrombin time (PT) and International Normalized Ratio (INR) - used as a measure of how quickly a person’s blood clots. People taking the blood-thinner warfarin (brand name Coumadin) must have this regularly monitored.
- Brain natriuretic peptide (BNP) test - mainly checked because they relate to heart function (not brain function!). BNP levels go up when a person’s has “heart failure.”
- Ferritin - measures the body’s serum ferritin level ( related to iron stores in the body). Used as part of an evaluation for anemia (low red blood cell count).
- A low ferritin level is suggestive of iron-deficiency, which is a common cause of anemia.
- Studies estimate that only a third of anemias in older adults are due to deficiencies in iron or other essential elements.
- It’s important to confirm iron deficiency by checking ferritin or other tests, before relying on iron to treat anemia.
- Ferritin levels are also influenced by inflammation, which tends to make ferritin levels rise.[2]
- Erythrocyte Sedimentation Rate (ESR) - assesses the rate at which red blood cells will settle (due to gravity) out of plasma while in solution. This process of settling/falling is referred to as "sedimentation," and is used to identify conditions which cause inflammation, as these conditions will increase the sedimentation rate. This is because red blood cells carry a negative charge, while inflammatory proteins are positive; these proteins allow for the blood cells to "clump together" (called a rouleaux formation), and these clumps settle quicker as a result. Conditions this test may be used to monitor include: [3]
- Cancer
- Infection
- Lupus
- Arteritis
- Polymyalgia Rheumatica
- Rheumatoid Arthritis
- Systemic vasculitis
In-depth Look at Blood Tests[edit | edit source]
see also Lab Value Interpretation
NB reference ranges apply to adults only and are laboratory-specific and not applicable to every lab result
Water and sodium
- Na: 135-145 mmol/l
↓Na - Hyponatremia (from skin, kidneys, gut) – weakness, postural hypotension, syncope, wt loss, cv changes, decreased skin turgor.
↑Na - Hypernatremia (incr. intake, decr. Excretion) – oedema, pulmonary oedema, HT, effusions
Potassium
- K: 3.4-5.2 mmol/l
↓K- Hypokalemia (alkalosis, RF, D&V,diuretics) – Weakness, ileus, hypotonia, confusion, depression, arrhythmias, alkalosis.
↑K- Hyperkalemia (catabolism, acidosis, RF) – Cardiac arrest with VF.
Renal Function Tests - Urea & creatinine
- U: 2.5-6.5 mmol/l Cr: 60-120μmol/l Both should rise together in renal failure. Creat is the more accurate measurement, urea is affected more by diet and dehydration. Creatinine Clearance Crcl: 100-120mls/min
Measures glomerular filtration rate and permeability
Thyroid diseases
- Hyperthyroidism (Graves disease, multinodular goiter, adenoma) – weight loss, sweating, palpitation, angina, tremor, diarrhea, muscle weakness, goiter, eyelid retraction.
- Hypothyroidism (Hashimotos disease, post surgery, congenital, secondary to pituitary/hypothalamic disease)
- lethargy, cold intolerance, dry coarse skin & hair, hoarseness, wt gain, slow reflexes & muscle relaxation. Others including: anaemia, psychosis, constipation bradycardia, CTS, infertility.
Thyroid Function Testing:
- TSH 0.3-5mU/l
- >15mU/l - 1° hypothyroidism
- 0.3-5mU/l - euthyroid (normal)
- <0.3mU/l - Further investigations!
Interpretation complicated by:
-Many medications, hormones
-Any acute illness – “sick euthyroidism” all thyroid tests are low.
-Recovery – TSH raised.
Glucose:
- Fasting 3-5.5 mmol/l
- >7.8 – diagnostic of DM
- 5.5-7.8 – impaired glucose tolerance
- Hyperglycaemia Thirst, polyuria, dehydration, hypotension, tachycardia, drowsiness.
(and for IDDM, DKA) ketosis, hyperventilation, vomiting. - Hypoglycaemia Tiredness, confusion, detachment, ataxia, blurred vision, dizziness, paraesthesia, hemiparesis, convulsions, coma
Lactate
<2.0 mmol/l
↑ mainly due to tissue hypoxia (decreased perfusion or decr. PO2)
Albumin
alb: 36-50 g/l
- Maintains oncotic pressure (keeps fluid in vessels)
- Transports small drugs, calcium & hormones
- ↓ (Many causes incl. malnutrition, liver disease, overhydration, incr. cap. Permeability, protein-losing states, burns, haemorrhage, general catabolism-sepsis, fever, malignancy, trauma)
- Symptoms – edema! (Unresponsive to diuretics or elevation)
C-reactive protein
CRP: <5mg/l
An ‘acute phase’ protein
-Monitoring infections (>100, more likely to be bacterial)
-Distinguishing between AI diseases and active infection
-Monitoring RA Rx
-Checking for post-op infection
Uric acid
0.1-0.4 mmol/l
Incr. production/decr. Excretion → gout (exquisite pain and inflammation often in 1st MTP joint)
>0.54 mM → 50% chance of developing gout
Tumour Markers
- Chemicals related to the presence/progress of a tumour
- Either secreted by tumours or cell surface antigens
Conclusion[edit | edit source]
- A blood test/ laboratory test is a test in which a sample of blood is withdrawn from the body to analyze the level of substances or cells (such as glucose, hemoglobin, or white blood cells)
- It may indicate the presence or probable development of a particular disease or medical condition (such as diabetes, cardiovascular disease, or cancer) or serve to indicate the degree of function of a specific organ (such as the liver or kidney).
- Laboratory value tests are one factor in determining the overall health of our patients. For many tests, the normal ranges will vary depending on age, gender, race, or other factors[4]
References[edit | edit source]
- ↑ Family Dr Common lab tests Available from:http://www.familydoctor.co.nz/categories/preventive-health/common-laboratory-tests-a-patients-guide/ (last accessed 4.7.2020)
- ↑ 2.0 2.1 Better health Understanding 10 common blood tests Available from:https://betterhealthwhileaging.net/understanding-10-common-blood-tests-in-aging/ (last accessed 4.7.2020)
- ↑ Tishkowski K, Gupta V. Erythrocyte Sedimentation Rate. StatPearls [Internet]. 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557485/
- ↑ Physicaltherapy.com. Available from: http://www.physicaltherapy.com/articles/essential-role-lab-values-and-3637 (last accessed 5.7.2020)