Immune System
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Nupur Smit Shah
Introduction[edit | edit source]
The overall function of the immune system is to prevent or limit infection.
The Immune response is the body's ability to stay safe by affording protection against harmful agents and involves lines of defense against most microbes as well as specialized and highly specific response to a particular offender.
This immune response classifies as either:
- Natural Barriers
- Innate Immune response (often our first line of defense against anything foreign) - defends the body against a pathogen in a similar fashion at all times. These natural mechanisms include
- Various cytokines, complement system (a complex system of more than 30 proteins that act in concert to help eliminate infectious microorganisms. Causes the lysis of foreign and infected cells, the phagocytosis of foreign particles and cell debris, and the inflammation of surrounding tissue), lysozymes, bacterial flora
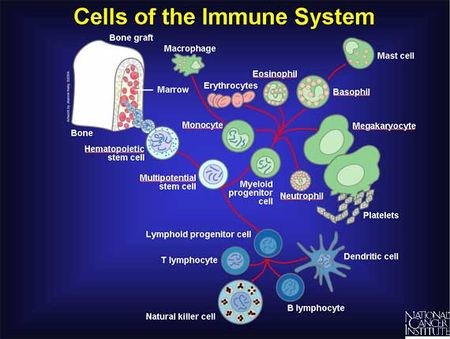
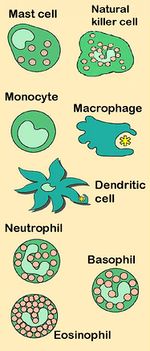
- Numerous cells including neutrophils, basophils, eosinophils, monocytes, macrophages, reticuloendothelial system, natural killer cells (NK cells), epithelial cells, endothelial cells, red blood cells, and platelets.
- Adaptive acquired Immune response (will utilize the ability of specific lymphocytes and their products (immunoglobulins, and cytokines) to generate a response against the invading microbes, its typical features are:
- Specificity: as the triggering mechanism is a particular pathogen, immunogen or antigen.
- Heterogeneity: signifies the production of millions of different effectors of the immune response (antibodies) against millions of intruders.
- Memory: The immune system has the ability not only to recognize the pathogen on its second contact but to generate a faster and stronger response.[1]
The two subsystems within the immune system (innate and the adaptive immune system) are closely linked and work together whenever a germ or harmful substance triggers an immune response.
Natural Barriers[edit | edit source]
- The Skin
- Usually bars invading microorganisms unless it is physically disrupted (eg, by arthropod vectors, injury, IV catheters, surgical incision).
- Mucous membranes
- Many mucous membranes are bathed in secretions that have antimicrobial properties (eg, cervical mucus, prostatic fluid, and tears containing lysozyme, which splits the muramic acid linkage in bacterial cell walls, especially in gram-positive organisms).
- Local secretions also contain immunoglobulins, principally IgG and secretory IgA, which prevent microorganisms from attaching to host cells, and proteins that bind iron, which is essential for many microorganisms.
- Respiratory tract
- If invading organisms reach the tracheobronchial tree, the mucociliary epithelium transports them away from the lung. Coughing also helps remove organisms.
- If the organisms reach the alveoli, alveolar macrophages and tissue histiocytes engulf them.
- These defenses can be overcome by large numbers of organisms, by compromised effectiveness resulting from air pollutants (eg, cigarette smoke), interference with protective mechanisms (eg, endotracheal intubation, tracheostomy), or by inborn defects (eg, cystic fibrosis).
- GI tract
- Barriers include the acid pH of the stomach and the antibacterial activity of pancreatic enzymes, bile, and intestinal secretions.
- Peristalsis and the normal loss of epithelial cells remove microorganisms.
- If peristalsis is slowed (eg, because of drugs such as belladonna or opium alkaloids), this removal is delayed and prolongs some infections, eg symptomatic shigellosis.
- Compromised GI defense mechanisms may predispose patients to particular infections (eg, achlorhydria predisposes to salmonellosis).
- Normal bowel flora can inhibit pathogens - alteration of this flora with antibiotics can allow overgrowth of inherently pathogenic microorganisms.
- GU tract
- Barriers include the length of the urethra (20 cm) in men, the acid pH of the vagina in women, the hypertonic state of the kidney medulla, and the urine urea concentration.
- The kidneys also produce and excrete large amounts of Tamm-Horsfall mucoprotein, which binds certain bacteria, facilitating their harmless removal.[2]
Innate Immune Response[edit | edit source]
The primary function of innate immunity is the recruitment of immune cells to sites of infection and inflammation through
- Production of cytokines (small proteins involved in cell-cell communication).
- Cytokine production leads to the release of antibodies and other proteins and glycoproteins which activate the complement system ie a biochemical cascade that functions to identify and coat foreign antigens, rendering them susceptible to phagocytosis.
- The innate immune response also promotes clearance of dead cells or antibody complexes and removes foreign substances present in organs, tissues, blood and lymph.
- It can also activate the adaptive immune response through a process known as antigen presentation.[2]
Numerous cells are involved in the innate immune response eg phagocytes (macrophages and neutrophils), dendritic cells, mast cells, basophils, eosinophils, natural killer (NK) cells and lymphocytes (T cells).
Phagocytes sub-divided into two main cell types both of which share a similar function - to engulf (phagocytose) microbes.
- Neutrophils are short-lived cells Additionally neutrophils contain granules that, when released, assist in the elimination of pathogenic microbes.
- Macrophages are long-lived cells that not only play a role in phagocytosis, but are also involved in antigen presentation to T cells[2].
Adaptive Acquired Immune Response[edit | edit source]
- Activite immunity comes from exposure to a pathogen. See image R
- Surface markers on the pathogen surface act as antigens, which are binding sites for antibodies.
- Antibodies are Y-shaped protein molecules, which can exist on their own or attach to the membrane of special cells.
- The body doesn't keep a store of antibodies on hand to take down an infection immediately.
- A process called clonal selection and expansion builds up sufficient antibodies[3].
Key Points[edit | edit source]
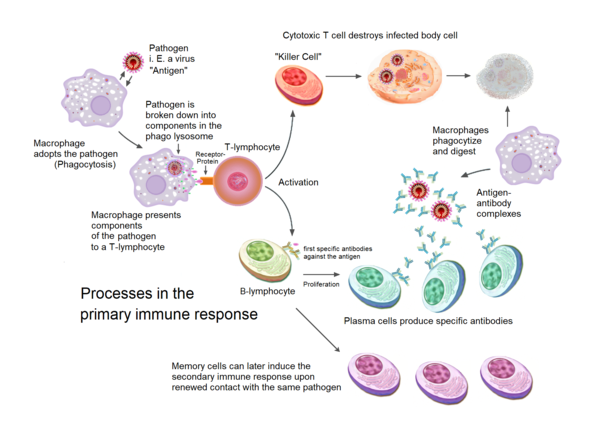
- Active immunity requires exposure to a pathogen or to the antigen of a pathogen.
- Exposure to the antigen leads to the production of antibodies. These antibodies essentially mark a cell for destruction by special blood cells called lymphocytes.
- Cells involved in active immunity are T cells (cytotoxic T cells, helper T cells, memory T cells, and suppressor T cells), B cells (memory B cells and plasma cells), and antigen-presenting cells (B cells, dendritic cells, and macrophages).
- There is a delay between exposure to the antigen and acquiring immunity. The first exposure leads to what is called a primary response. If a person is exposed to the pathogen again later, the response is much faster and stronger. This is called a secondary response.
- Active immunity lasts a long time. It can endure for years or an entire life.
- There are few side effects of active immunity. [3]
Passive Immunity[edit | edit source]
Active immunity occurs when an individual produces antibodies to a disease through his or her own immune system, passive immunity is provided when a person is given antibodies.
- This can happen in utero or through antibody-containing blood products—such as immune globulin, or a substance made from human blood plasma—administered when immediate protection from a specific disease is needed.
- Passive immunity is conferred from outside the body, so it doesn't require exposure to an infectious agent or its antigen.
- There is no delay in the action of passive immunity. Its response to an infectious agent is immediate.
- Passive immunity is not as long-lasting as active immunity. It is typically only effective for a few days[3].
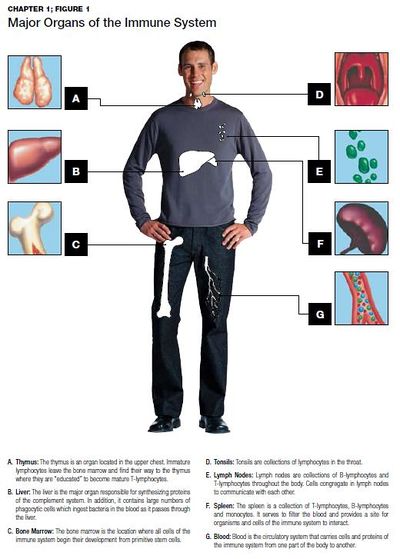
Organs Involved[edit | edit source]
The organ systems involved in the immune response are primarily lymphoid organs which include, spleen, thymus, bone marrow, lymph nodes, tonsils, and liver.
The lymphoid organ system classifies according to the following:
- Primary lymphoid organs (thymus and bone marrow), where T and B cells first express antigen receptors and become mature functionally.
- Secondary lymphoid organs like the spleen, tonsils, lymph nodes, the cutaneous and mucosal immune system; this is where B and T lymphocytes recognize foreign antigens and develop appropriate immune responses.
- T lymphocytes mature in the thymus, where these cells reach a stage of functional competence
- B lymphocytes mature in the bone marrow the site of generation of all circulating blood cells.
- Excessive release of cytokines stimulated by these organisms can cause tissue damage, such as endotoxin shock syndrome[1].
Pathophysiology[edit | edit source]
The immune system protects the body against many diseases including recurrent infections, allergy, tumor, and autoimmunity. The consequences of an altered immunity will manifest in the development of many immunological disorders some of which are listed below:
- Crohn disease
- Melanoma
- Systemic lupus erythematosus SLE
- Rheumatoid arthritis RA
- Acquired immunodeficiency syndrome
- Food or drug Allergy[1]
- Asthma
Why Some COVID-19 Patients Crash: The Body's Immune System Might Be To Blame
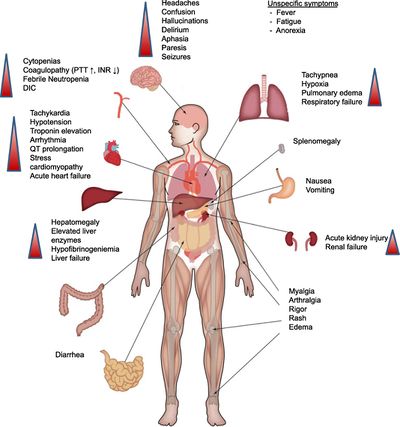
- Critically important studies emerging from China suggest that for many patients who die of Covid-19, it may be their own immune system, rather than the virus itself, that deals the fatal blow. This is called a cytokine storm (see image R)
- Cytokines are small proteins released by many different cells in the body, including those of the immune system where they coordinate the body’s response against infection and trigger inflammation.
- Cytokine storms are a common complication not only of covid-19 and flu but of other respiratory diseases caused by coronaviruses such as SARS and MERS. They are also associated with non-infectious diseases such as multiple sclerosis and pancreatitis.[4]
Immunodeficiency[edit | edit source]
Immunodeficiency - a state in which the immune system's ability to fight infectious disease is compromised or entirely absent. Immunodeficiency disorders may result from:
- Primary congenital defect (primary immunodeficiency)
- Acquired from a secondary cause (secondary immunodeficiency) eg viral (eg viral hepatitis) or bacterial infections, malnutrition or treatment with drugs that induce immunosuppression eg chemotherapy or radiation.
- Certain diseases can also directly or indirectly impair the immune system eg leukemia and multiple myeloma.
- Immunodeficiency is also the hallmark of acquired immunodeficiency syndrome (AIDS), caused by the human immunodeficiency virus (HIV). HIV directly infects Th cells and also impairs other immune system responses indirectly.[5]
Antibiotics[edit | edit source]
Help the immune system by killing the offending bacteria directly.
- Antibiotics
- Work on bacterial infections.
- Are chemicals that kill the bacteria cells but do not affect the cells that make up your body.
- Different antibiotics work on different parts of bacterial machinery, so each one is more or less effective on specific types of bacteria.
One problem with antibiotics is that they lose effectiveness over time.
- If you take an antibiotic it will normally kill all of the bacteria it targets over the course of a week or 10 days. You will feel better very quickly (in just a day or two) because the antibiotic kills the majority of the targeted bacteria very quickly.
- Occasionally one of the bacterial offspring will contain a mutation that is able to survive the specific antibiotic. This bacteria will then reproduce and the whole disease mutates.
- Eventually the new strain is infecting everyone and the old antibiotic has no effect on it. This process has become more and more of a problem over time and has become a significant concern in the medical community.[6]
Vaccines[edit | edit source]
A vaccine is a weakened form of a disease. It is either a killed form of the disease, or it is a similar but less virulent strain. Once inside your body your immune system mounts the same defense, but because the disease is different or weaker you get few or no symptoms of the disease. Now, when the real disease invades your body, your body is able to eliminate it immediately.
- Vaccines exist for all sorts of diseases, both viral and bacterial: measles, mumps, whooping cough, tuberculosis, smallpox, polio, typhoid, etc.
- Many diseases cannot be cured by vaccines eg common cold and Influenza. These diseases either mutate so quickly or have so many different strains in the wild that it is impossible to inject all of them into your body. Each time you get the flu, for example, you are getting a different strain of the same disease.[6]
Historical Note[edit | edit source]
Two scientists who discovered key functions of the immune system, Louis Pasteur (image at R) and Robert Koch, should have been able to see their work as complementary, but they wound up rivals.
- Pasteur, (born December 27, 1822, Dole, France - died September 28, 1895, Saint-Cloud), French chemist and microbiologist who was one of the most important founders of medical microbiology. [7]
- Koch, (born Dec. 11, 1843 - died May 27, 1910, Baden-Baden, Ger.), German physician and one of the founders of bacteriology. He discovered the anthrax disease cycle (1876) and the bacteria responsible for tuberculosis (1882) and cholera (1883).
Both helped establish the germ theory of disease but were rivals all their lives - possibly fuelled by nationalism, a language barrier, criticisms of each other's work and jealousy[8].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Vaillant AA, Jan A. Physiology, Immune Response.Available from:https://www.ncbi.nlm.nih.gov/books/NBK539801/ (last accessed 18.6.2020)
- ↑ 2.0 2.1 2.2 Merck Manuals Professional Version. Host Defense Mechanisms Against Infection. http://www.merckmanuals.com/professional/infectious-diseases/biology-of-infectious-disease/host-defense-mechanisms-against-infection. (Last Accessed: 19.6.2020)
- ↑ 3.0 3.1 3.2 Thought co Immunity available from:https://www.thoughtco.com/active-immunity-and-passive-immunity-4134137 (last accessed 19.6.2020)
- ↑ New scientist. Cytokine storm Available from:https://www.newscientist.com/term/cytokine-storm/ (last accessed 20.6.2020)
- ↑ BMC An introduction to immunology and immunopathology Available from:https://aacijournal.biomedcentral.com/articles/10.1186/1710-1492-7-S1-S1 (last accessed 19.6.2020)
- ↑ 6.0 6.1 How stuff works Immune system Available from:https://health.howstuffworks.com/human-body/systems/immune/immune-system15.htm (last accessed 19.6.2020)
- ↑ Britannica Pasteur Available from:https://www.britannica.com/biography/Louis-Pasteur (last accessed 20.6.2020)
- ↑ Mental Floss 12 Fantastic Facts About the Immune System Available from:https://www.mentalfloss.com/article/520326/12-fantastic-facts-about-immune-system