Autism Spectrum Disorder
'Original Editor - Kirenga Bamurange Liliane Top Contributors - Kirenga Bamurange Liliane, Lucinda hampton, Jess Bell, Kim Jackson, Naomi O'Reilly, Nupur Smit Shah and Robin Tacchetti
Introduction[edit | edit source]
Autism, referred to as Autism Spectrum Disorder (ASD), is a neurodevelopmental disorder that affects the way an individual with ASD relates to others and to their environment.[1][2]
ASD traits may be evident in childhood, but some individuals will not be diagnosed until later in life. ASD can affect an individual's education and employment opportunities, and may add stress to the families providing care and support.[3] Some individuals may have significant disabilities and require ongoing care while others live independently.[3]
The following video explores the neuroscience of ASD. It also looks at potential factors and mechanisms associated with ASD (2 minutes).
Aetiology/Epidemiology[edit | edit source]
"ASD is a neurobiological disorder influenced by both genetic and environmental factors affecting the developing brain."[2]
Research into the aetiological mechanisms of ASD is ongoing, and at present, no single cause for this condition has been identified.[2]
- The reported prevalence of ASD is 1 in 68 individuals.[4]
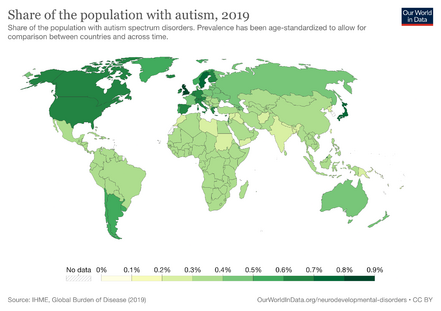
- Prevalence rates vary between countries.[5]
- The general prevalence of ASD is increasing globally.[5] However, it should be noted that this might be due to increased awareness of ASD, potential overdiagnosis, or diagnostic criteria that are over-inclusive.[4]
ASD in Low Resource Settings[edit | edit source]
The prevalence of ASD in many low and middle-income countries (LMIC) is unknown.[3] Research about the ASD diagnosis process in LMICs is still limited. The mean age at diagnosis of ASD is very similar across LMICs but it is older than in high-income countries.[6] Studies are required, specifically, epidemiological studies, to define the extent of the problem of ASD in LMICs.[7]
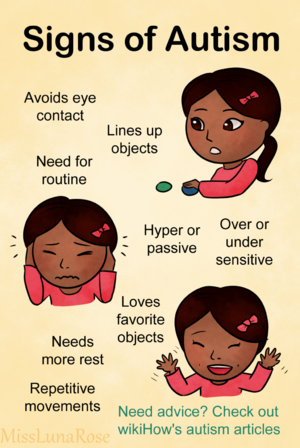
Signs and Symptoms[edit | edit source]
Signs of ASD usually appear in the second year of life.[8] Individuals with ASD might struggle with the following:[1]
- communicating their needs and desires (social impairements)
- interpretating other people
- processing sensory and cognitive information
- repetitive behaviour
Early signs of ASD may include:[9]
- Not responding to their own name
- Not pointing at objects / things of interest
- Avoiding eye contact
- Displaying a preference to be alone
- Not playing "pretend" or "make-believe" games
- Lack of speech / delayed speech
- Having difficulty understanding or showing that they understand another person's feelings or their own feelings
- Getting upset by small changes
- Providing unrelated answers to questions
- Obsessive interests
- Having no social skills or fewer social skills than expected
- Resisting or avoiding physical contact
- Having little safety or danger awareness
- Reversing pronouns - for example, they may say "I" instead of "you"
Other behaviours associated with ASD include:[9]
- Extreme anxiety / unusual phobias
- Lining up objects and toys
- Always playing with toys the same way every time
- Causing injury to self
- Lack of fear or excessive fear
- Short attention span
- Unusual sleeping / eating habits
Children and young people with ASD have different intellectual abilities. Individuals with ASD might have limited or no verbal communication, and very limited adaptive behaviour.[10] [3]
Co-occurring Conditions[edit | edit source]
Individuals with ASD frequently have co-occurring conditions (eg epilepsy, depression, anxiety and attention deficit hyperactivity disorder) and other challenging behaviours (eg difficulty sleeping and self-injury). The level of intellectual functioning also varies greatly among individuals with ASD. Some may experience profound impairment whereas others have average or higher IQs.[3][12]
Risk Factors[edit | edit source]
The following factors have been linked to ASD:[2]
- hereditary factors, parental history of psychiatric disorders, pre-term births
- increased parental age (both maternal and paternal age)
- history of autoimmune disease in mother (diabetes, thyroid disease and psoriasis have been suggested, but research findings are inconsistent)
- prenatal exposure to thalidomide and valproic acid
- some genetic disorders are more likely to co-occur with ASD, including fragile X syndrome,[13] tuberous sclerosis, Down syndrome, Rett syndrome - but these genetic conditions do not account for many cases of ASD overall
- maternal infection
- immune activation during pregnancy
- obstetric factors, including:
- uterine bleeding
- caesarian section
- low birth weight
- preterm delivery
- low Apgar scores
Diagnosis[edit | edit source]
A range of health professionals can diagnose ASD, and ideally multiple disciplines will be involved in the diagnosis.[14]
- A diagnosis that is made using both clinician observation and caregiver reports is considered more reliable than a diagnosis based on observation or caregiver reports alone.
- Diagnoses made later in life are often made in individuals with other conditions, including anxiety, hyperactivity, or mood disorders that may have exacerbated or hidden the ASD.[14]
- It is necessary to follow-up and reassess children diagnosed with ASDs, especially during the preschool years.[15]
- There are currently no clear biomarkers or diagnostic measures for ASD. ASD is, therefore, diagnosed when individuals meet certain descriptive criteria.[2]
Different approaches/tools are used to help screen for ASD, including:[16]
- The Modified Checklist for Autism in Toddlers, Revised (M-CHAT-R). This 20-question screening tool explores a child's behaviour. It is for children aged 16-30 months. See here for more information.
- CARS: Childhood Autism Rating Scale.[17] This scale can be used in children aged over 2 years.
- ADOS : Autism Diagnostic Observation Schedule.[17] This is a standardised, semi-structured observational assessment that looks at social interaction, communication, play and imaginative use of materials.
Please note that Asperger’s syndrome was previously used to describe individuals who have a high-functioning form of ASD. There is, however, no longer a separate diagnosis for Asperger's syndrome, although some people may prefer to keep using this term.[1]
Prognosis[edit | edit source]
ASD is a lifelong condition. Early intervention gives the best results.[18]
Treatment[edit | edit source]
There are range of treatment options for individuals with ASD. Selecting an appropriate treatment should be collaborative, and involve the individual, caregivers and health professionals.
Some common treatments for ASD include:
- Behavioural therapies: these aim to improve specific behaviours and help an individual develop skills. This approach tends to use standard behaviour strategies (i.e. reward behaviours that are considered appropriate or acceptable, ignore / discourage behaviours that are considered inappropriate or unacceptable).[19]
- Occupational therapy: concentrates on adaptive skills needed for activities of daily living (ADLs).
- Sensory therapy: there are a number of sensory interventions developed to help address sensory-challenges.[19]
- Speech therapy: to help improve a child's understanding / use of language.[20][21]
- Physiotherapy: to help improve physical and motor skills. You can read more about the Physiotherapy Management of ASD here: Autism Spectrum Disorder and Motor Development
- Complementary and alternative treatments including animal therapy, art therapy, music therapy, and relaxation therapies are supplementary treatment options for people with ASD.[21]
- Medications may be used to treat symptoms of ASD, including:
- antipsychotic medications for repetitive behavior patterns / aggression
- serotonin reuptake inhibitors (SSRIs)
- stimulants, and other antipsychotics for problematic behaviours (like aggression) etc.[4]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 The spectrum What is autism? Available:https://thespectrum.org.au/autism/#what-is-asperger%E2%80%99s-syndrome? (accessed 5.1.2023)
- ↑ 2.0 2.1 2.2 2.3 2.4 Hodges H, Fealko C, Soares N. Autism spectrum disorder: definition, epidemiology, causes, and clinical evaluation. Translational pediatrics. 2020 Feb; 9(Suppl 1): S55.
- ↑ 3.0 3.1 3.2 3.3 3.4 World health organisation Autism Available:https://www.who.int/news-room/fact-sheets/detail/autism-spectrum-disorders (accessed 5.1.2023)
- ↑ 4.0 4.1 4.2 Mughal S, Faizy RM, Saadabadi A. Autism spectrum disorder (regressive autism, child disintegrative disorder). New York: StatPearls‑NCBI Bookshelf. 2020.Available:https://www.ncbi.nlm.nih.gov/books/NBK525976/ (accessed 5.1.2023)
- ↑ 5.0 5.1 Salari N, Rasoulpoor S, Rasoulpoor S, Shohaimi S, Jafarpour S, Abdoli N, Khaledi-Paveh B, Mohammadi M. The global prevalence of autism spectrum disorder: a comprehensive systematic review and meta-analysis. Ital J Pediatr. 2022 Jul 8;48(1):112.
- ↑ Samms-Vaughan ME. The status of early identification and early intervention in autism spectrum disorders in lower- and middle-income countries. Int J Speech Lang Pathol. 2014 Feb;16(1):30-5.
- ↑ Bakare MO, Munir KM. Autism spectrum disorders (ASD) in Africa: a perspective. African journal of psychiatry. 2011 Jul 1;14(3):208-10.
- ↑ Nilsson Jobs E, Bölte S, Falck-Ytter T. Spotting signs of autism in 3-year-olds: comparing information from parents and preschool Staff. J Autism Dev Disord. 2019 Mar;49(3):1232-41.
- ↑ 9.0 9.1 National Autism Association. Signs of Autism. Available from https://nationalautismassociation.org/resources/signs-of-autism/ (last accessed 2 June 2023).
- ↑ Steinbrenner JR, Hume K, Odom SL, Morin KL, Nowell SW, Tomaszewski B, Szendrey S, McIntyre NS, Yücesoy-Özkan S, Savage MN. Evidence-Based Practices for Children, Youth, and Young Adults with Autism. FPG Child Development Institute. 2020.
- ↑ Neuroscientifically challenged. 2-Minute Neuroscience: Autism. Available from: https://www.youtube.com/watch?v=tEBsTX2OVgI [Accessed, 5.1.2023]
- ↑ Autism Research Institute. Average or high IQ in individuals with ASD may be higher than previously estimated. Available from: https://autism.org/average-or-high-iq-in-individuals-with-asd-may-be-higher-than-previously-estimated/ (last accessed 28 April 2023).
- ↑ Niu M, Han Y, Dy ABC, Du J, Jin H, Qin J, et al. Autism Symptoms in Fragile X Syndrome. J Child Neurol. 2017 Sep;32(10):903-9.
- ↑ 14.0 14.1 Lord C, Elsabbagh M, Baird G, Veenstra-Vanderweele J. Autism spectrum disorder. The Lancet. 2018 Aug 11;392(10146):508-20.
- ↑ Fernell E, Eriksson MA, Gillberg C. Early diagnosis of autism and impact on prognosis: a narrative review. Clinical epidemiology. 2013;5:33.
- ↑ Centers for Disease Control and Prevention. Screening and Diagnosis of Autism Spectrum Disorder for Healthcare Providers. Available from: https://www.cdc.gov/ncbddd/autism/hcp-screening.html (last accessed 29 April 2023).
- ↑ 17.0 17.1 Parmeggiani A, Corinaldesi A, Posar A. Early features of autism spectrum disorder: a cross-sectional study. Italian journal of pediatrics. 2019 Dec;45(1):1-8.
- ↑ Autism Research Institute. Prognosis. Available from: https://autism.org/autism-prognosis/ (last accessed 29 April 2023).
- ↑ 19.0 19.1 Autism research institute Treatment Information and Resources Available:https://www.autism.org/treatment/ (accessed 5.1.2023)
- ↑ Alpert JS. Autism: A Spectrum Disorder. The American Journal of Medicine. 2021 Jun 1;134(6):701-2.
- ↑ 21.0 21.1 Treatment and Intervention Services for Autism Spectrum Disorder. Available from: https://www.cdc.gov/ncbddd/autism/treatment.html ( Accessed, 17/03/2022).