Generalised Anxiety Disorder
Original Editors - Dana Moorer & Kaelin Hocker from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Ellen Baumann, Dana Moorer, Vidya Acharya, Admin, Kim Jackson, Lucinda hampton, Andeela Hafeez, Kaelin Hocker, WikiSysop, Candace Goh, Lauren Lopez, Aminat Abolade, Elaine Lonnemann and Wendy Walker
Definition/Description[edit | edit source]
Generalised anxiety disorder (GAD) is one of the most common mental disorders. Up to 20% of adults are affected by anxiety disorders each year. Generalised anxiety disorder produces fear, worry, and a constant feeling of being overwhelmed. Generalised anxiety disorder is characterised by persistent, excessive, and unrealistic worry about everyday things.
- This worry could be multifocal such as finance, family, health, and the future.
- It is excessive, difficult to control, and is often accompanied by many non-specific psychological and physical symptoms[1]
GAD can be considered primary or secondary depending on the onset.
- If GAD occurs early in life without any other diagnosis then it is considered primary.
- If GAD develops later in life and there are other disorders present, it is considered secondary in nature. [2]
Epidemiology[edit | edit source]
In the general population, the lifetime prevalence of GAD is 5.1%, with a 12‐month prevalence measured at 3.1%.
- Within the primary care setting, the WHO collaborative study on Psychological Disorders in Primary Health Care study reported that GAD formed the second largest category of psychological disorders, with a prevalence of just under 7.9%.
- A survey of high utilisers of medical health care found a particularly high prevalence rate of GAD at 22%, and the prevalence of GAD in patients visiting physicians' offices has been shown to be twice that found in the community.
- Women have a higher prevalence rate for GAD than men, with the median age of onset occurring during the early 20s.[4]
Symptoms[edit | edit source]
GAD can be a challenge to diagnose. People consider panic attacks a hallmark of all anxiety disorders, but GAD is different in that there are generally no panic attacks associated with the condition. As a result of this misconception, without the experience of panic attacks, a person may think they are "just worrying too much". Their struggles with constant worry may be minimised or dismissed and, in turn, not properly diagnosed or treated.
The DSM-5 outlines specific criteria to help professionals diagnose generalised anxiety disorder. Having a standard set of symptoms to reference when assessing clients helps them to more accurately diagnose mental health concerns and, in turn, create a more effective plan of care.
Criteria for Diagnosing GAD: When assessing for GAD, clinical professionals are looking for the following:
- The presence of excessive anxiety and worry about a variety of topics, events, or activities. Worry occurs more often than not for at least six months and is clearly excessive.
- The worry is experienced as very challenging to control. The worry in both adults and children may easily shift from one topic to another.
- The anxiety and worry are accompanied by at least three of the following physical or cognitive symptoms (In children, only one of these symptoms is necessary for a diagnosis of GAD):
- Edginess or restlessness
- Easily tired; more fatigued than usual
- Impaired concentration or feeling as though the mind goes blank
- Irritability (which may or may not be observable to others)
- Increased muscle aches or soreness
- Difficulty sleeping (due to trouble falling asleep or staying asleep, restlessness at night, or unsatisfying sleep)[6]
Causes[edit | edit source]
There is no singular cause of GAD that has been identified. Evidence has shown that multiple factors are usually at play, influencing the development of GAD. Some of the common factors include things like genetic predisposition, brain chemistry, family background, social influence, and life experiences. See examples below:
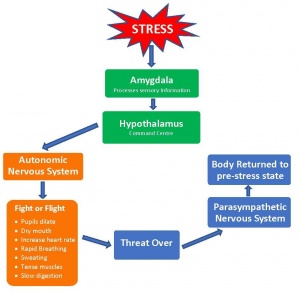
- The limbic system is a collection of brain structures that, among other functions, is involved in the regulation of many of basic emotional reactions. The amygdala, in particular, is the part of the limbic system involved in the automatic fear response, as well as in the integration of memory and emotion. The amygdala is an important player in people's ability to discern and feel fear, so it may not be a surprise that imaging studies of people diagnosed with GAD show elevated amygdala activity during the processing of negative emotions. [6]It is this heightened activity within the amygdala that researchers believe might influence the inaccurate interpretations of social behavior for patients with GAD.
- Life Experiences: Although genetic and biologic factors clearly contribute to the development of GAD, a greater percentage of the risk for GAD lies in complex psychological, environmental, and social factors.
- Experiencing Trauma: Mental health researchers have found that trauma in childhood can increase a person's risk of developing GAD. Difficult experiences such as physical and mental abuse, neglect, the death of a loved one, abandonment, divorce, or isolation can all be contributing factors.
- Children learn from caregivers and other important people close to them how to handle challenging, stressful situations. When they model less effective methods of stressful management, children tend to do the same. These early social learning experiences can influence the development of long-lasting anxiety.
- Using everyday addictive substances like caffeine can heighten feelings of worry or nervousness, contributing to the development of anxiety. Our culture tends to ask more and more of us, pushing us to perform, and leaving us to fear feeling left behind, socially, financially, physically, or otherwise.
- Research has shown that two main factors of anxiety, specifically related to women, were being afraid of and/or humiliated by a current partner or ex-partner. Dangerous and fearful experiences within intimate relationships can also influence the development of anxiety.
- Of people who are on social media, it has been shown that approximately 30% are plugged into social media for 15 hours or more per week. Researchers are finding that the use of social media, particularly in excess, can greatly impact mental health, sometimes resulting in anxiety and depression. Interacting with others through social media can also present us with the same challenges as when we are interacting in people, such as feelings of loneliness, rejection, abandonment, or humiliation.[6].
Treatment[edit | edit source]
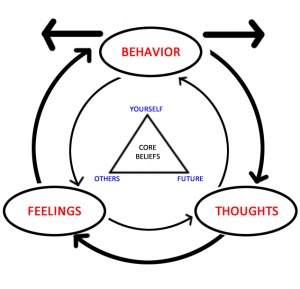
The most effective generalised anxiety disorder treatment is psychological therapy – cognitive behavioural therapy (CBT) – which includes the following:
- Education: learning about why you worry and feel anxious, and how it affects you.
- Change in thinking: identifying and shifting unhelpful thinking patterns and beliefs.
- Change in behaviour: scheduling in appropriate times to worry, rather than worrying all the time.
- Facing your fears: gradually putting you in situations that make you anxious will help you learn to face and cope with those situations, rather than avoid or try to escape them.[7]
A Cochrane review
- Provided robust evidence that psychological therapy using a cognitive behavioural approach is effective in the treatment of generalised anxiety disorder (GAD). Forty six percent of patients assigned to cognitive behavioural therapy (CBT) showed clinical response at post‐treatment, in contrast with 14% in waiting list/treatment as usual groups, and anxiety, worry and depression symptoms were also significantly reduced. There is a lack of evidence for longer‐term effectiveness of psychological therapy in treating GAD.
Whilst the overall attrition rate from psychological therapy using a CBT approach is reasonably low at 15%, this review suggests that patients who attended group therapy were more likely to drop out of treatment, and those attending individual therapy were more likely to persist with treatment. Attrition rates in the elderly were also significantly higher. Reasons for dropout were under‐reported in studies, and may not only have been due to low acceptability or effectiveness of psychological therapy[4].
Medication[edit | edit source]
Medication may also be required in some cases and is known to be effective when taken alongside psychological treatment.[8]
- See also The influence of antidepressant medication on physiological processes.
- Medications for anxiety work by interacting with brain chemicals (neurotransmitters). Particular medications may block the absorption or enhance the action of one or more of these chemicals.
The different types of medications used in the treatment of anxiety include:
- selective serotonin reuptake inhibitors (SSRIs)
- serotonin and norepinephrine reuptake inhibitors (SNRIs)
- anxiolytics
- tri-cyclic antidepressant
Physical Therapy Management[edit | edit source]
Physical therapists need to be aware of the symptoms of anxiety due to the fact that more and more patients are being diagnosed with generalized anxiety disorder.
See also Mental Health, Physical Activity and Physiotherapy
- There are no specific physical therapy interventions that relate directly to GAD.
- The job of the physical therapist (when appropriate) to refer the patient to his/her primary physician in order for the patient to have the proper medical management of their disorder.
Anxiety can cause many clinical symptoms that may mimic a musculoskeletal disorder including muscle tension/ muscle aches. It is important to distinguish what is the source of this muscle tension. This is when a thorough history is important in gathering the necessary information and determining if this is true within the scope of practice.
Techniques may include:
- Patient Education: It is important for the patient to understand what brings on their anxiety. Explaining that keeping a diary of their anxiety and rating it on a scale of 0-10 can be helpful for the patient.
- Exercise: Research on anxiety and exercise has shown that benefits of exercise include the reduction of anxiety and improved mood. This relationship is not clearly understood; however, it has been found that working out can help increase relaxation and keep the anxiety symptoms from returning once the patient is feeling better.[9] Exercise can help anxiety by releasing "feel-good" brain chemicals (which include neurotransmitters and endorphins). Exercise can also increase the body temperature and in turn produce calming effects. There are also psychologic and emotional benefits of exercise that include increased confidence, taking the mind of worries, increased socialisation (within a gym setting), and coping in a healthy way. Aerobic exercise is best for the management of anxiety; however, any exercise to get the patient moving is a positive. Workplace physical activity and yoga programmes are associated with a significant reduction in depressive symptoms and anxiety, respectively[10].
- Deep breathing exercises
- Progressive muscle relaxation can help release muscle tension.[7]
- Meditation. Research shows that meditation boosts activity on the left side of the prefrontal cortex, the area of the brain responsible for feelings of serenity and joy.[7]
- Other stress management techniques could include: yoga; music therapy; education reincorporating a well-balanced diet and making getting adequate amounts of sleep each night (help to manage stress and anxiety).[11]
Case Reports[edit | edit source]
Generalised anxiety disorder and clinical worry episodes in young women
Generalised Anxiety Disorder Case Study 2017
References[edit | edit source]
- ↑ Generalized Anxiety Disorder (GAD) S. Munir, Veronica Takov Published 2019 Psychology Available:https://www.semanticscholar.org/paper/Generalized-Anxiety-Disorder-(GAD)-Munir-Takov/c3b76e491023740d6f77d1e229f7c53ade96fe92 (Accesssed 11.7.2021)
- ↑ Katzman MA. Current Considerations in the Treatment of Generalized Anxiety Disorder. CNS Drugs. 2009;23(2):103–20
- ↑ Osmosis Generalized anxiety disorder (GAD) - causes, symptoms & treatment Available from:https://www.youtube.com/watch?v=9mPwQTiMSj8
- ↑ 4.0 4.1 Hunot V, Churchill R, Teixeira V, Silva de Lima M. Psychological therapies for generalised anxiety disorder. Cochrane Database of Systematic Reviews 2007, Available: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD001848.pub4/full Accessed 11 July 2021.
- ↑ Anxiety Disorders Manitoba Generalized Anxiety Disorders Available from https://www.youtube.com/watch?v=KbY4HG4Uod4
- ↑ 6.0 6.1 6.2 Very Well Mind GAD Available: https://www.verywellmind.com/dsm-5-criteria-for-generalized-anxiety-disorder-1393147 (accessed 11.7.2021)
- ↑ 7.0 7.1 7.2 Generalized Anxiety Disorder (GAD): Symptoms, Self Help ... [Internet]. [cited 2017Mar28]. Available from: https://www.bing.com/cr?IG=8FC29D1F1EE841D1A800C4AAB0544B80&CID=0DE2894FDDE06D7628B2832CDC706CAD&rd=1&h=ssbrYq8ttVKTvvDLYjLkBqJxQAFdzrKYuHppIbQBNpw&v=1&r=https%3a%2f%2fwww.helpguide.org%2farticles%2fanxiety%2fgeneralized-anxiety-disorder-gad.htm&p=DevEx,5061.1
- ↑ Reach out GAD Available: https://au.reachout.com/articles/generalised-anxiety-disorder (accessed 11.7.2021)
- ↑ Generalized anxiety disorder [Internet]. MedlinePlus Medical Encyclopedia. [cited 2017Mar27]. Available from: https://medlineplus.gov/ency/article/000917.htm
- ↑ Chu AH, Koh D, Moy FM, Müller-Riemenschneider F. Do workplace physical activity interventions improve mental health outcomes?. Occupational Medicine. 2014 May 17;64(4):235-45.
- ↑ Tips to Manage Anxiety and Stress, Anxiety and Depression. Anxiety and Depression Association of America, ADAA. [cited 2017Mar28].https://adaa.org/tips-manage-anxiety-and-stress