Kidney
Original Editor - Manisha Shrestha
Top Contributors - Manisha Shrestha and Lucinda hampton
Introduction[edit | edit source]
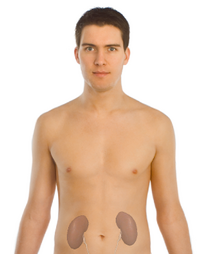
The kidneys are paired retroperitoneal organs that lie at the level of the T12 to L3 vertebral bodies, well protected by muscle, fat, and ribs[1].
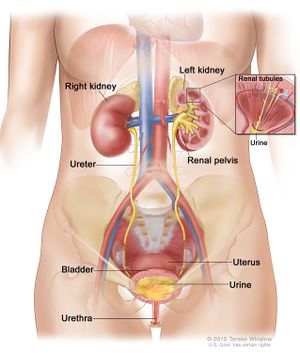
Healthy kidneys filter about a half cup of blood every minute, removing wastes and extra water to make urine. The urine flows from the kidneys to the bladder through two thin tubes of muscle called ureters, one on each side of the bladder. The bladder stores urine. Your kidneys, ureters, and bladder are part of the urinary tract[2].
Location[edit | edit source]
The kidneys are located on the posterior abdominal wall, with one on either side of the vertebral column, in the perirenal space. The long axis of the kidney is parallel to the lateral border of the psoas muscle and lies on the quadratus lumborum muscle. In addition, the kidneys lie at an oblique angle, that is the superior renal pole is more medial and posteriorly than the inferior pole. Due to the right lobe of the liver, the right kidney usually lies slightly lower than the left kidney.
The 10 minute video below shows the external gross anatomy of the kidney
Importance[edit | edit source]
The kidneys remove wastes and extra fluid from the body. They also remove acid that is produced by the cells of the body and maintain a healthy balance of water, salts, and minerals (eg sodium, calcium, phosphorus, and potassium) in our blood. Without this balance, nerves, muscles, and other tissues in the body may not work normally.[2]
Primary Function
- It is a major excretory organ for elimination of metabolic wastes from the body.[4]
- It regulates plasma osmolarity by modulating the amount of water, solutes, and electrolytes in the blood.
Secondary Function
- It ensures long term acid-base balance
- It also produces erythropoietin which stimulates the production of red blood cell.
- It also produces renin for blood pressure regulation
- It carries out the conversion of vitamin D to its active form, ultimately helps in calcium absorption.[5][6]
How do the Kidneys work?[edit | edit source]
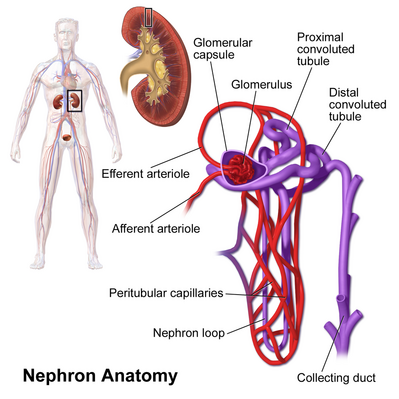
Each of your kidneys is made up of about a million filtering units called nephrons. Each nephron includes a filter, called the glomerulus, and a tubule. The nephrons work through a two-step process: the glomerulus filters your blood, and the tubule returns needed substances to your blood and removes wastes.
- The glomerulus filters your blood: As blood flows into each nephron, it enters a cluster of tiny blood vessels—the glomerulus. The thin walls of the glomerulus allow smaller molecules, wastes, and fluid—mostly water—to pass into the tubule. Larger molecules, such as proteins and blood cells, stay in the blood vessel.
- The tubule returns needed substances to your blood and removes wastes: A blood vessel runs alongside the tubule. As the filtered fluid moves along the tubule, the blood vessel reabsorbs almost all of the water, along with minerals and nutrients your body needs. The tubule helps remove excess acid from the blood. The remaining fluid and wastes in the tubule become urine[2].
The 4 minute video below outlines the internal gross anatomy of the kidneys
[7] The following 6 minute video shows the microscopic anatomy of the kidney.
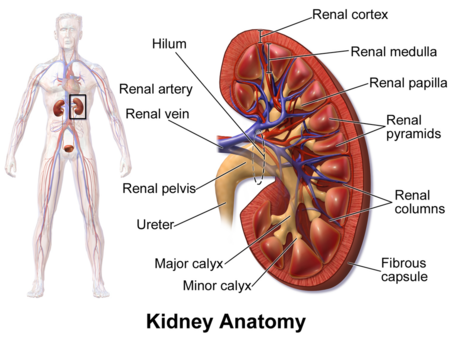
Blood supply of Kidney[edit | edit source]
Blood flows into your kidney through the renal artery. This large blood vessel branches into smaller and smaller blood vessels until the blood reaches the nephrons. In the nephron, your blood is filtered by the tiny blood vessels of the glomeruli and then flows out of your kidney through the renal vein.
Your blood circulates through your kidneys many times a day. In a single day, your kidneys filter about 142 litres of blood. Most of the water and other substances that filter through your glomeruli are returned to your blood by the tubules. Only 1 to 2 litres become urine.[2]
Nerve supply of kidney[edit | edit source]
- Kidney and nervous system communicates via renal plexus .
- Renal nerve arise from superior mesenteric ganglion and enter the hilum of each kidney and follow branches of renal artery to reach individual nephrons.
- These nerves consist mostly of sympathetic fibers that trigger vasoconstriction in kidney.
- Sensory input from the kidney travels to the T10 -11 levels of spinal cord and is sensed in the corresponding dermatome. thus, pain in the flank region may be referred from corresponding kidney.[9]
Renal Function Tests (RFT)[edit | edit source]
RFT is ordered, if the doctor
- Suspects a person's kidneys may not be working properly which is known from signs and symptoms
- If a person has other conditions that can harm the kidneys, such as diabetes or high blood pressure
Tests of renal function are useful for:
- Identifying the presence of renal disease
- Monitoring the response of kidneys to treatment
- Determining the progression of renal disease
Physiotherapy: Renal Rehabilitation[edit | edit source]
Physiotherapists treating clients with the following conditions may be involved in Renal rehabilitation (RR)
- Nephritis/nephrosis,
- Chronic kidney diseases eg Polycystic Kidney Disease, Diabetic kidney. Alcoholic kidney
- Dialysis therapy
- Kidney transplantation
The physiotherapist input in the RR is to design a good comprehensive exercise program. They are held over 6-12 weeks with classes ranging between 1-2 hours, with participants committed to performing exercises at home on at least two other days a week
References[edit | edit source]
- ↑ Radiopedia The Kidneys Available:https://radiopaedia.org/articles/kidneys (accessed 3.10.2021)
- ↑ 2.0 2.1 2.2 2.3 NIH Your Kidneys & How They Work Available: https://www.niddk.nih.gov/health-information/kidney-disease/kidneys-how-they-work (accessed 3.10.2021)
- ↑ Anatomic Wisdom. The External Gross Anatomy of the Kidney. Available from: https://www.youtube.com/watch?v=OmMzMBSsaU4. [Lasted accessed: 2021-4-30]
- ↑ Finco DR. Kidney function. In Clinical biochemistry of domestic animals 1997 Jan 1 (pp. 441-484). Academic Press.
- ↑ Ogobuiro I, Tuma F. Physiology, renal. StatPearls [Internet]. 2019 Feb 10.
- ↑ Microscopic Anatomy of the Kidney. Available from: https://bio.libretexts.org/Courses/Lumen_Learning/Book%3A_Biology_of_Aging_(Lumen)/13%3A_The_Urinary_System/13.05%3A_Microscopic_Anatomy_of_the_Kidney. Lasted Accessed: 2021-5-2
- ↑ Kidneys and Urinary System LO2 - Internal Gross Anatomy. Available from: https://www.youtube.com/watch?v=25CO_f7o_c4. [lasted accessed: 2021-4-30]
- ↑ Microscopic structure of kidney-Nephron. Available from: https://www.youtube.com/watch?v=OoIZ1N-haL8. [Lasted accessed: 2021-4-30]
- ↑ Kidney. From Wikipedia, the free encyclopedia Available from: https://en.wikipedia.org/wiki/Kidney. Lasted accessed: 2021-5-2