Raynaud's Phenomenon
Definition[edit | edit source]
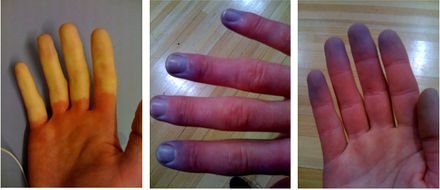
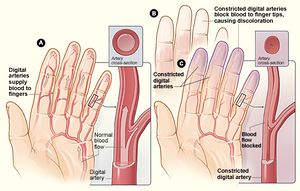
Raynaud's Phenomenon (RP) is a disorder characterized by an episodic color change of the extremities in response to cold exposure or emotional stress. It is represented by fingers that have turned white, then blue and finally become red which represent vasospasm, deoxygenation, and reperfusion hyperemia.[1] It affects primarily the blood vessels in the fingers and toes, but the nose, lips, or ear lobes vessels may also be affected.[2]
This phenomenon is named after ' Maurice Raynaud, a medical student who defined the first case in 1862 as " episodic, symmetric, acral vasospasm characterized pallor, cyanosis, and a sense of fullness or tautness, which may be painful."[3]
Types of RP[edit | edit source]
RP occurs as a primary form on its own or as a secondary form due to an underlying disease [4]. It is referred to as "Raynaud's disease" or " primary Raynaud's phenomenon" when it occurs alone and isn't associated with an underlying condition. It is referred to as Secondary Raynaud's when it's the result of associated diseases and tends to be more serious than the primary form[5].
Causes of RP[edit | edit source]
The causes of both primary and secondary Raynaud's phenomenon are unknown. It's maybe linked to some blood disorders by increasing blood thickness due to excess platelets or red blood cells.[4] Both abnormal nerve control of the blood-vessel diameter and nerve sensitivity to cold exposure may also be contributing factors. [6]
The following causes can be found: [5]
- An attack can be triggered by cold temperature in cases such as putting hands in cold water, taking something from the freezer, or exposure to cold air.
- Attacks can also be triggered by emotional stress
Other causes may include:[4]
- Blood disorders.
- The Sensitivity of special receptors that control the narrowing of blood vessels.
- Secondary causes of Raynaud’s include lupus, scleroderma, and other diseases.
As well as:[5]
- The disease of the arteries.
- Carpal Tunnel Syndrome.
- Repetitive action or vibration.
- Smoking.
- Injuries to the hands and feet such as wrist fracture, surgery, or frostbite.
- Certain medications such as medications for high blood pressure, migraine, hyperactivity, and chemotherapy.
Signs and Symptoms[edit | edit source]
The symptoms of RP depend on the severity, frequency, and duration of the blood vessel spasm.[6] These may include:
- Skin decoloration.
- Mild tingling and digits' numbness.
- Pain due to irritation of sensory nerves.
- Swollen and painful hands
- Ulceration of the tips of the digits because of poor oxygen supply.
- Gangrene is caused by a prolonged lack of oxygen.
Diagnosis of RP[edit | edit source]
RP itself is not a diagnosis and there is no blood test to diagnose it. However, a thorough assessment should be done and should be comprised by[1][5]:
- A detailed history including occupation and smoking history.
- A physical examination of hands to specifically look for signs of connective tissue disease.
- A full blood count.
- Nailfold capillaroscopy to look for deformities or swelling of the tiny blood vessels.
Management/Treatment of RP[edit | edit source]
There is no cure for RP but it can be managed with a proper and well-planed treatment based on the patient's symptoms, age, severity, and overall health. The treatment may include:[4]
- Avoiding exposure to cold.
- Keeping warm with gloves, socks, a scarf, and a hat.
- Stopping smoking.
- Wearing finger guards over fingers with sores.
- Avoiding trauma or vibrations to the hand (such as with vibrating tools).
- Taking blood pressure medicines during the winter months to help reduce constriction of the blood vessels.
- Patient's education.
The treatment includes medical therapy as well in form of antihypertensives, such as calcium-channel blockers (CCB) or sartanes, and vasodilating agents, such as intravenous iloprost[7]. RP patients with no other symptoms than the skin discoloration extremities may require only home-remedy measures to prevent complications[6].
Prevention of RP[edit | edit source]
The prevention of RP can be done by:[1]
- Avoiding all the precipitating factors such as exposure to heat or cold and smoking.
- Avoiding medications that aggravate symptoms of RP.
Risk factors of RP[edit | edit source]
The following factors can increase the risk of developing RP [6]:
- Underlying diseases such as Scleroderma, Lupus, Rheumatoid Arthritis, or Sjögren's syndrome.
- Cigarette smoking
- Injury or trauma
- Side effects of certain medicines
- Chemical exposure
Complications of RP[edit | edit source]
People with RP can develop critical ischemia and the development of digital ulcers (DU), that potentially cause superinfection, necrosis, and amputation [7].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Herrick, AL. Raynaud’s phenomenon. Journal of Scleroderma and Related Disorders. 2019; 4(2): 89–101.
- ↑ Raynaud's Phenomenon. Available from: https://my.clevelandclinic.org/health/diseases/9849-raynauds-phenomenon (Accessed, 16th January 2021).
- ↑ Raynaud Phenomenon. Available from: https://emedicine.medscape.com/article/331197-overview (Accessed, 16 January 2021).
- ↑ 4.0 4.1 4.2 4.3 Raynaud's Phenomenon. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/raynauds-phenomenon#:~:text=Raynaud's%20phenomenon%20is%20a%20problem,%2C%20stress%2C%20or%20emotional%20upset.( Accessed, 16 January 2021).
- ↑ 5.0 5.1 5.2 5.3 Raynaud's disease. Available from: https://www.mayoclinic.org/diseases-conditions/raynauds-disease/symptoms-causes/syc-20363571 (Accessed, 17 January 2021).
- ↑ 6.0 6.1 6.2 6.3 Raynaud's Phenomenon and Disease. Available from: https://www.medicinenet.com/raynauds_phenomenon/article.htm (Accessed, 16 January 2021)
- ↑ 7.0 7.1 Korsten P, Müller GA, Rademacher JG, Zeisberg M, Tampe B. Rheopheresis for digital ulcers and Raynaud's phenomenon in systemic sclerosis refractory to conventional treatments. Frontiers in medicine. 2019 Sep 18;6:208.
- ↑ Johns Hopkins Rheumatology. Raynaud’s Phenomenon: What You Should Know | Johns Hopkins Medicine. Available from: http://https://www.youtube.com/watch?v=Jv0kEFCYF5M [last accessed 27/1/2021]
- ↑ Brigham And Women's Hospital. Raynaud’s Phenomenon Video – Brigham and Women’s Hospital. Available from: http://www.youtube.com/watch?v=Aml-vSYWHrg [last accessed 27/1/2021]