Scleroderma
Original Editors - Amanda Schoenfelder and Katie Williams from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Bridget Ward, Katie Williams, Amanda Schoenfelder, Lucinda hampton, Admin, Elaine Lonnemann, Khloud Shreif, WikiSysop, Sehriban Ozmen, Wendy Walker and Kim Jackson
Introduction[edit | edit source]
Scleroderma, a rare connective tissue disorder with a complex unknown pathogenesis[1], that involves changes to the skin, and can also involve changes to the blood vessels and internal organs. It is a chronic, progressive autoimmune disorder where inflammation and the overproduction of collagen accumulate in the body[2].
Classification[edit | edit source]
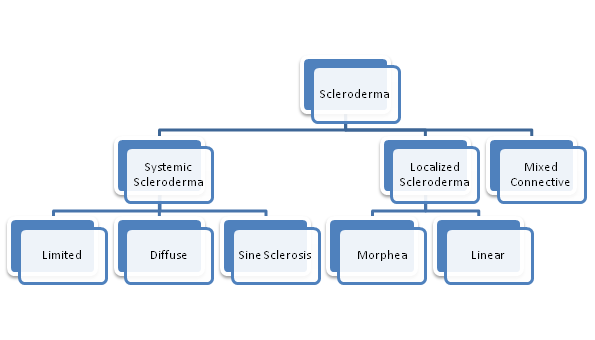
There are two main types of Scleroderma- Systemic and Localized[2].
Systemic Scleroderma (SSc) may affect the skin and multiple systems such as the integumentary, cardiopulmonary, vascular, gastrointestinal, genitourinary, or musculoskeletal. There are three forms of Systemic Scleroderma.
- With Diffuse Scleroderma skin thickening occurs more rapidly and involves more skin areas than in limited. In addition, people with diffuse scleroderma have a higher risk of developing “sclerosis” or fibrous hardening of the internal organs.[3]
- Sine Scleroderma involves organ fibrosis with no skin involvement. This is rare. [4]
- With Limited Scleroderma (includes CREST syndrome) skin thickening is less widespread, typically confined to the fingers, hands and face, and develops slowly over years. Internal problems occur, but they are less frequent and tend to be less severe than in diffuse scleroderma.[3] CREST is an acronym using the letters of the conditions involved; Calcinosis, Raynaud’s, Esophageal dysmotility, Sclerodactyly and Telangiectasia. The video below gives some good examples of these.
Localized Scleroderma usually affects the skin and related tissues in part of the body. Two of the main types of Localized Scleroderma are below [5]
- Morphea is characterized by waxy patches on the skin of varying sizes, shapes and color. The skin under the patches may thicken. The patches may enlarge or shrink, and often may disappear spontaneously within three to five years.[3] In some, rare, cases muscle weakness may be associated.
- Linear Scleroderma starts as a streak or line of hardened, waxy skin on an arm or leg or on the head and neck. Linear scleroderma tends to involve deeper layers of the skin as well as the surface layers, and sometimes affects the motion of the joints, which lie underneath.[3]
Mixed Connective Tissue Disease or Scleroderma Overlap syndrome is when Scleroderma is diagnosed when another disease, such as systemic lupus erythematosus and polymyositis, has been previously diagnosed[6].
Epidemiology[edit | edit source]
Scleroderma is a rare disease, with differing prevalence due to ethnicity, gender, and geographic area. Systemic sclerosis SSc is more common in European, North, and South American patients than in East Asian patients, with the Highest prevalence (47 in 100,000) is among indigenous peoples in Canada[7].
In line with other autoimmune diseases, women are at greater risk than men (ratio 4.6:1)[8]but males tend to have more severe SSc[7]. Thirty percent of those with scleroderma have the systemic form of scleroderma and sine scleroderma accounted for nearly 10% of patients with systemic sclerosis[9]. This type appears to be more common in adults. Localised scleroderma is more common in children[5].
Estimates vary.
- In France, the cutaneous form predominates, with the incidence of systemic sclerosis estimated at 158.3 per million in 2002[8].
- Some estimates predict that about 300,000 Americans have scleroderma.[10] Some predict 75,000 to 100,000 [4]
It is more common in females than males, and between the ages of 20 to 50 [4]
Those with a family member who has scleroderma, or another autoimmune disease such as lupus, may have a slightly higher risk of developing scleroderma. [10]
Race and ethnic background, may influence the risk of getting scleroderma, the age of onset, and the pattern or severity of internal organ involvement. Choctaw Native Americans and African-Americans are more likely than Americans of European descent to develop the type of scleroderma that affects internal organs.[11]
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
A diagnosis of scleroderma can be difficult because symptoms may be similar to that’s of other disease. Diagnosis will be based on:
- Medical history
- Physical examination. See below for symptoms of ‘Systemic Involvement’
- X-rays and CT for bony investigations
- MRI and US for soft tissue examiantion
- Lab tests can also confirm a suspected diagnosis[12][13]:Topoisomerase-1 antibody or Scl-70 antibodies is a marker of systemic sclerosis.; Anticentromere antibodies, or ACA, is a marker of CREST; ESR is found to be increased in those with disease activity or relapse; AMF is positive in those with Mixed Scleroderma
Not all people with scleroderma have these antibodies and because not all people with the antibodies have scleroderma, lab test results alone cannot confirm the diagnosis.
A skin biopsy (the surgical removal of a small sample of skin for microscopic examination) can aid in or help confirm a diagnosis.
Diagnosing scleroderma is easiest when a person has typical symptoms and rapid skin thickening. In other cases, a diagnosis may take months, or even years, as the disease unfolds and reveals itself and as the doctor is able to rule out some other potential causes of the symptoms.[14][10]
Etiology/Causes[edit | edit source]
The cause of scleroderma is unknown, but it cannot be transmitted from person to person. Several factors that may increase a person's risk of getting scleroderma include:
- Abnormal immune or inflammatory activity: In scleroderma, the immune system is thought to stimulate cells called fibroblasts so they produce too much collagen. People who already have rheumatic or autoimmune disorders are at increased risk due to previous abnormal autoimmune activity[5]
- Genetic makeup: Although genes seem to put certain people at risk for scleroderma and play a role in its course, the disease is not passed from parent to child like some genetic diseases. Research indicates that variations in genes relating to the the body’s immune system, eg.those in the HLA-complex, IRF5 and STAT4, may increase the risk of developing scleroderma. [3][14][15]
- Environmental triggers: Research suggests that exposure to some environmental factors may trigger scleroderma-like disease in people who are genetically predisposed to it. Suspected triggers may include viral or bacterial infections [5][14][15]
- Hormones: Women develop scleroderma more often than men. Scientists suspect that hormonal differences between women and men play a part in the disease. However, the role of estrogen or other female hormones has not been proven.[14][11]
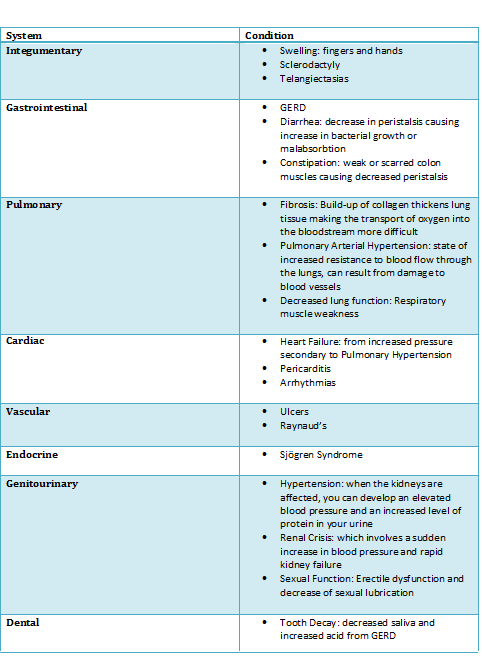
Systemic Involvement[edit | edit source]
Medical Management[edit | edit source]
Currently, there is no treatment that controls or stops the underlying problem—the overproduction of collagen—in all forms of scleroderma. Treatment and management focus on relieving symptoms and limiting damage. Importantly treatment goals need be holistic and individualised for the client, aiming to optimise their quality of life, as well as preventing further organ damage. Patient Education regarding the disease and advocating involvement in regular exercises, healthy diet and lifestyle is important.[1]
Several different specialists may be involved in the care of one person since scleroderma can affect many different organs and organ systems. Typically, care will be managed by a rheumatologist, who may refer the patient to other specialists, depending on the specific problems they are having.[14]
These specialists can include:
• Dermatologist for the treatment of skin symptoms
• Nephrologist for kidney complications
• Cardiologist for heart complications
• Gastroenterologist for problems of the digestive tract
• Pulmonary specialist for lung involvement
Medications used to treat scleroderma may include: [10][16]
- Anti-inflammatory medicines such as corticosteroids
- Immune-suppressing medications such as methotrexate and cytoxan.
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
Scleroderma can affect many different organs and organ systems. Additional medications are based on the symptoms that the individual experiences.
Examples of other treatments for specific symptoms include:[10][16]
- Medicines for heartburn or swallowing problems - antacid drugs, especially proton- pump inhibitors
- Blood pressure medications (particularly ACE inhibitors) for high blood pressure or kidney problems
- Light therapy to relieve skin thickening
- Cyclophosphamide and mycophenolate can be effective in treating interstitial lung disease
- Medications to treat pulmonary hypertension include prostacyclin-like drugs, endothelin receptor antagonists and PDE-5 inhibitors. These work to open up the blood vessels in the lungs.
- Medications to treat Raynaud's phenomenon- calcium channel blockers, PDE-5 inhibitors to open up narrowed blood vessels and improve circulation.
- Intestinal dysfunction
- Medicines to increase saliva secretion in the mouth to reduce effects of Sjogren’s Syndrome (a chronic autoimmune disease in which a person’s white blood cells attack their moisture-producing glands)
Physical Therapy Management[edit | edit source]
Physical therapy can be very beneficial in the treatment of scleroderma. Due to the musculoskeletal damage often seen in scleroderma patients, physiotherapy is often needed to prevent lasting damages.[8] Physical therapists/ Physiotherapists, together with other health professionals such as Occupational Therapists, can design a program of regular stretching and gentle exercise to help:
• Manage pain
• Improve strength
• Improve/maintain mobility
• Minimize joint contractures
• Improve circulation. Education re protecting vulnerable skin areas and keeping them warm
• Enhance/maintain performance of activities of daily living in order to encourage independence[14][3]
In the context of physical therapy, various techniques and exercises can be used to aid individuals in regaining or enhancing their physical capabilities including; massage, hydrotherapy, electrical stimulation therapy, exercise movement methods, or physiotherapy techniques. Although randomized controlled trials have evaluated these interventions for their suitability in the treatment of systemic sclerosis (SSc), the results have demonstrated some level of inconsistency[17].
Aerobic exercise such as walking, jogging, cycling, and dancing to enhance cardiovascular efficiency and encompasses a wide range of physical activities, resistance training contributes to the development of muscle strength, anaerobic endurance, and muscle size it may be like lifting groceries, climbing stairs, or transitioning from sitting to standing, or range of motion exercise like stretching, yoga help to enhance the range of motion of specific joints. These sample of exercises can be carried individually or in group even indoors or outdoors[18].
Other Health Professionals[edit | edit source]
- Other health professionals such as psychologists, and social workers may play a role in patient care.[14][3]
- Dentists, orthodontists, and speech therapists may be involved in the management of complications that arise from thickening of mouth and face tissues. [14]
Research about the most effective management and treatment is ongoing. [14][11]
Prognosis SSC[edit | edit source]
SSc has with high mortality. The prognosis in SSc has improved since the 1990's with the 5-year survival rates now up to 80%. Unfortunately patients with advanced pulmonary arterial hypertension have a poorer outlook, with a 50% 2-year survival rate. Additionally patients with SSc-related pulmonary arterial hypertension are worse off when compared to those with idiopathic pulmonary arterial hypertension.[1]
Differential Diagnosis[edit | edit source]
A number of other diseases have symptoms similar to those seen in scleroderma.
These include:
- Eosinophilic fasciitis (EF): This rare disease involves the fascia, the thin connective tissue around the muscles. The fascia becomes swollen, inflamed and thick. The skin on the arms, legs, neck, abdomen or feet can be involved. Unlike scleroderma, the fingers are not involved. A skin biopsy distinguishes between the two diseases.
- Nephrogenic Systemic Fibrosis: An uncommon disease of fibrosis of the skin and organs, caused by gadolinium exposure ( used in imaging) in those patients with renal insufficiency.
- Generalized scleroderma-like skin thickening: This may occur with scleromyxedema, graft-versus-host disease, porphyria cutanea tarda, and human adjuvant disease
- Raynauds phenomena: This may occur in isolation, as well as part of the scleroderma disease process.[19]
Case Report/ Case Study[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Adigun R, Goyal A, Hariz A. Systemic sclerosis. Available:https://www.ncbi.nlm.nih.gov/books/NBK430875/ (last accessed 31.3.2024)
- ↑ 2.0 2.1 Rosendahl AH, Schönborn K, Krieg T. Pathophysiology of systemic sclerosis (scleroderma). The Kaohsiung journal of medical sciences. 2022 Mar;38(3):187-95.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 Rosendahl AH, Schönborn K, Krieg T. Pathophysiology of systemic sclerosis (scleroderma). The Kaohsiung journal of medical sciences. 2022 Mar;38(3):187-95.
- ↑ 4.0 4.1 4.2 Arthritis Foundation. Scleroderma information sheet. https://www.arthritis.org/about-arthritis/types/scleroderma ( accessed 15.3.2018)
- ↑ 5.0 5.1 5.2 5.3 Careta MF, Romiti R. Localized scleroderma: clinical spectrum and therapeutic update. Anais brasileiros de dermatologia. 2015 Jan;90:62-73.
- ↑ Sato F, Sato M, Yamano T, Yamaguchi K, Miyake T. A Case of Mixed Connective Tissue Disease That Transformed Into Systemic Lupus Erythematosus After a Long Clinical Course. Cureus. 2023 Apr 27;15(4).
- ↑ 7.0 7.1 Calderon LM, Pope JE. Scleroderma epidemiology update. Current Opinion in Rheumatology. 2021 Mar 1;33(2):122-7.
- ↑ 8.0 8.1 8.2 Odonwodo A, Badri T, Hariz A. Scleroderma. InStatPearls [Internet] 2022 Aug 1. StatPearls Publishing.Available:https://www.ncbi.nlm.nih.gov/books/NBK537335/ (accessed 2.9.2023)
- ↑ Lescoat A, Huang S, Carreira PE, Siegert E, de Vries-Bouwstra J, Distler JH, Smith V, Del Galdo F, Anic B, Damjanov N, Rednic S. Cutaneous Manifestations, Clinical Characteristics, and Prognosis of Patients With Systemic Sclerosis Sine Scleroderma: Data From the International EUSTAR Database. JAMA dermatology. 2023 Aug 1;159(8):837-47. BibTeXEndNoteRefManRefWorks
- ↑ 10.0 10.1 10.2 10.3 10.4 American Academy of Dermatology Association. scleroderma: diagnosis and treatment.
- ↑ 11.0 11.1 11.2 11.3 Mayo Foundation for Medical Education and Research. Patient Care and Health Information. Sclerodermahttp://www.mayoclinic.com/health/scleroderma/DS00362 ( accessed 8 April 2018)
- ↑ Marzano AV, Menni S, Parodi A, Borghi A, Fuligni A, Fabbri P, Caputo R. Localized scleroderma in adults and children. Clinical and laboratory investigations on 239 cases. European Journal of Dermatology. 2003 Apr 15;13(2):171-6.
- ↑ Careta MF, Romiti R. Localized scleroderma: clinical spectrum and therapeutic update. Anais brasileiros de dermatologia. 2015 Jan;90:62-73.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 14.7 14.8 National Institute of Arthritis and Musculoskeletal and Skin Diseases. Health Topics. Scleroderma.
- ↑ 15.0 15.1 US National Library of Medicine. Genetics Home Reference. Systemic Scleroderma. http://ghr.nlm.nih.gov/condition/systemicscleroderma / (accessed 8 April 2018)
- ↑ 16.0 16.1 Shah AA, Wigley FM. My approach to the treatment of scleroderma. In Mayo Clinic Proceedings 2013 Apr 1 (Vol. 88, No. 4, pp. 377-393).
- ↑ Poole JL. Musculoskeletal rehabilitation in the person with scleroderma. Current opinion in rheumatology. 2010 Mar 1;22(2):205-12.
- ↑ Frade S, Cameron M, Espinosa-Cuervo G, Suarez-Almazor ME, Lopez-Olivo MA. Exercise and physical therapy for systemic sclerosis. The Cochrane Database of Systematic Reviews. 2022;2022(3).
- ↑ Medscape. Drugs and Diseases. Rheumatology. Scleroderma. Differential Diagnosis. http://emedicine.medscape.com/article/331864-differential ( accessed 8 April 2018)