Connective Tissue Disorders
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Elaine Lonnemann and Admin
Introduction[edit | edit source]
The connective tissue disorders (CTDs) form a large heterogeneous group of conditions that are linked by a disease process that primarily involves the connective soft tissues of the body and often the vasculature too, due to shared structural proteins, such as collagen and elastin.[1] There are over 200 documented disorders of connective tissue[2]
Diseases of the connective tissue can be divided into
- A group of relatively uncommon genetic disorders that affect the primary structure of connective tissue eg Marfan syndrome and osteogenesis imperfecta.
- A number of acquired disorders in which the connective tissues are the site of several more or less distinctive immunological and inflammatory reactions eg rheumatoid arthritis, systemic lupus erythematosus, rheumatic fever, and osteoarthritis[3].
Anatomy & Physiology[edit | edit source]
A “tissue” in simple terms is a collection of similar cells. The human body is basically made of four different types of tissues.
- Epithelial tissue
- Connective tissue - the most abundant and diverse type of animal tissue
- Muscular tissue
- Nervous tissue.
Similar to a framework of a house, connective tissue serves to provide structure, support, and protection throughout the human body.[2]
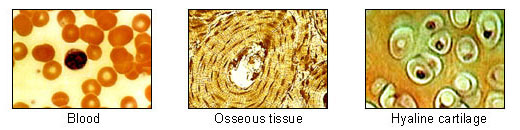
Connective tissue is an umbrella that encompasses a variety of tissue types, including loose and dense connective tissue, adipose, cartilage, bone, and blood. Although connective tissue is diverse, all connective tissue consists of three main components:
- Ground substance
- Fibers
- Cells
Together, the ground substance and fibers make up the extracellular matrix, which is the structural support of surrounding cells throughout the body. The composition of the extracellular matrix varies tremendously from organ to organ, which allows for the diverse types of connective tissue.
Examples of Connective tissue:
- In the abdominal cavity, most organs are suspended from the abdominal wall by a membranous band (the mesentery) which is supported by connective tissue, others are embedded in adipose tissue (a form of connective tissue in which the cells are specialized for the synthesis and storage of energy-rich reserves of fat, or lipid).
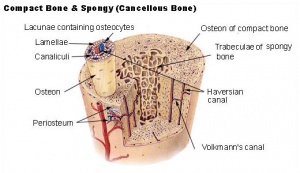
- The entire body is supported from within by a skeleton composed of bone, a type of connective tissue endowed with great resistance to stress owing to its highly ordered laminated structure and to its hardness, which results from deposition of mineral salts in its fibres and amorphous matrix.
- The individual bones of the skeleton are held firmly together by ligaments, and muscles are attached to bone by tendons, both of which are examples of dense connective tissue in which many fibre bundles are associated in parallel array to provide great tensile strength.
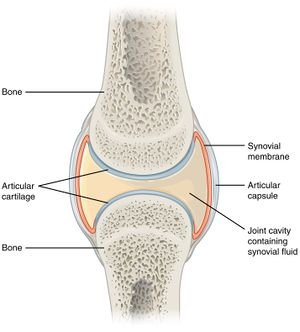
- At joints, the articular surfaces of the bones are covered with cartilage, a connective tissue with an abundant intercellular substance that gives it a firm consistency well adapted to permitting smooth gliding movements between the apposed surfaces.
- The synovial membrane, which lines the margins of the joint cavity and lubricates and nourishes the joint surfaces, is also a form of connective tissue.
- Blood vessels, both large and small, course through connective tissue, which is therefore closely associated with the nourishment of tissues and organs throughout the body.
Hereditary Disorders Of Connective Tissue[edit | edit source]
Hereditary disorders of connective tissue are a heterogeneous group of generalized single-gene-determined disorders that affect one or another of the primary elements of the connective tissues (collagen, elastin, or ground substance [glycosaminoglycans]). Many cause skeletal and joint abnormalities that may interfere seriously with normal growth and development. These conditions are rare compared with the acquired connective tissue diseases.[3] Examples include:
- Marfan syndrome
- Ehlers-Danlos syndrome
- osteogenesis imperfecta
- Stickler syndrome
- epidermolysis bullosa
- arterial tortuosity syndrome
- Loeys-Dietz syndrome[1]
Acquired Diseases Of Connective Tissue[edit | edit source]
The acquired connective tissue diseases display certain common clinical features, including inflammation of the joints (polyarthralgia and arthritis), serous (fluid-exuding) membranes (pleurisy and pericarditis), and small blood vessels (vasculitis) and a high frequency of involvement of various internal organs that are particularly rich in connective tissue (e.g., the lungs). The walls of inflamed blood vessels, portions of which may become necrotic, are often found to contain characteristic deposits of hyaline (translucent) material called fibrinoid[3].
Classic connective tissue diseases
- systemic lupus erythematosus (SLE)
- systemic sclerosis (SSc)
- Sjogren syndrome (SS)
- mixed connective tissue disease (MCTD)
- polymyositis
- dermatomyositis
- Polymyalgia Rheumatica
Seronegative connective tissue diseases
Connective Tissue Disorder Treatment[edit | edit source]
There is currently no cure for any of the connective tissue diseases. Breakthroughs in genetic therapies, where certain problem genes are silenced, hold promise for the single-gene diseases of connective tissue.
For autoimmune diseases of connective tissue, treatment is aimed at helping to reduce the symptoms. Newer therapies for conditions such as psoriasis and arthritis can suppress the immune disorder that causes the inflammation.
- Medicines may be given to prevent immune system from attacking healthy cells or to to stop the disease from getting worse. Topical creams or lotions to control a rash or other symptoms that affect skin may be needed.
- Prescription pain medicine may be given.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever.
- Steroids may be given to reduce swelling and pain.
Management includes
- Rest as needed. eg good sleep hygeine, resting joints if they are stiff or painful, support devices such as crutches or splints to help joints rest.
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, lean meats, fish, and low-fat dairy products.
- Physical therapists can create an exercise plan - help increase energy, keep stiff joints flexible and increase range of motion.
- An occupational therapist can help with daily activities to alleviate pain or swelling.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause blood vessel and lung damage.
- Manage stress. Stress may slow healing and lead to illness.
Managing Flare ups
- Apply ice or heat - Ice helps reduce pain and swelling, and may help prevent tissue damage.
- Elevation can help reduce swelling and pain, especially in joints. Elevate the area as often as possible.
- Keep hands and feet warm. Certain connective tissue disorders can cause hands and feet to become cold and painful. Over time, ulcers or gangrene (tissue death) may develop if frequent or severe attacks are not prevented. Clients should dress warmly in cold weather, including gloves and thick socks and wiggle fingers or toes to improve circulation[4].
See Individual Disease Links for more depth.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Radiopedia CTD's Available from: https://radiopaedia.org/articles/connective-tissue-disease?lang=us(last accessed 21.2.2021)
- ↑ 2.0 2.1 Nezwek TA, Varacallo M. Physiology, Connective Tissue. StatPearls [Internet]. 2020 Aug 16.Available from: https://www.ncbi.nlm.nih.gov/books/NBK542226/(accessed 21.2.2021)
- ↑ 3.0 3.1 3.2 Britannica CTD Available from: https://www.britannica.com/science/connective-tissue-disease(accessed 21.2.2021)
- ↑ Drugs.com CTDs Available from:https://www.drugs.com/cg/connective-tissue-disorders.html (accessed 21.2.2021)