Reactive Arthritis
Original Editors - Stéphanie Dartevelle
Top Contributors - Jennifer Colgan, Meredith Alvey, Admin, Kim Jackson, Vidya Acharya, Elaine Lonnemann, Lucinda hampton, Rucha Gadgil, Carina Therese Magtibay, 127.0.0.1, Megan Sarason, Wendy Walker and Claire Knott
Definition/Description[edit | edit source]
Reactive arthritis (ReA) is inflammatory arthritis (in the subset of Spondyloarthritis) which manifests after several days to weeks after a gastrointestinal or genitourinary infection. It is also described as a classic triad of arthritis, urethritis and, conjunctivitis. However, a majority of patients do not present with the classic triad.
It was previously called "Reiter syndrome", named after Hans Reiter, who first described this syndrome. The name, Reiter syndrome fell from favour as Hans Reiter was a Nazi member under whose leadership the war prisoners were subject to many inhumane experiments.[1]
Today, it is believed that the disorder is due to an aberrant autoimmune response to the gastrointestinal infection caused by Salmonella, Shigella, Campylobacter or chlamydia.
Causes[edit | edit source]
ReA can not be transmitted from person to person. However, the bacteria that triggered the disease can be passed on from one person to another.[2] ReA usually follows venereal disease or an episode of bacillary dysentery, which is a bacterial infection characterized by blood in the stool. Up to 85% of people with ReA possess the HLA-B27 alloantigen. Individuals with the appropriate genetic background can develop ReA through an enteric infection.[3]
Bacteria that most often cause infections and ReA are Chlamydia, Salmonella, Shigella, Yersinia, and Campylobacter. These can be manifested from sexually transmitted diseases or contaminated food.[4][2]
Etiology[edit | edit source]
Reactive arthritis is known to be triggered by a bacterial infection, particularly of the genitourinary (Chlamydia trachomatis, Neisseria gonorrhea, Mycoplasma hominis, and Ureaplasma urealyticum) or gastrointestinal (GI) tract (Salmonella enteritidis, Shigella flexneri, and disenteriae, Yersinia enterocolitica, Campylobacter jejuni, Clostridium difficile). The incidence is about 2% to 4% after a urogenital infection mainly with chlamydia trachomatis and varies from 0% to 15% after gastrointestinal infections with Salmonella, Shigella, Campylobacter, or Yersinia. This might be affected by the epidemiological, environmental factors, the pathogenicity of the bacteria, and differences in the study designs. The enteric ReA occurs commonly following enteric infections. However, chlamydia associated ReA is endemic, especially in developed countries.
Rare cases have been reported after administration of Bacillus Calmette Guerin vaccine ( BCG) treatment for bladder cancer.[1]
Epidemiology[edit | edit source]
Reactive arthritis is relatively rare, and the incidence in population-based studies is reported to be 0.6 to 27 per 100,000. Reactive arthritis is more common in adult males in the second and third decades of their life.
About 1-3% of patients with nonspecific urethritis will develop an episode of arthritis. Overall, higher disease activity and worse functional capacity are seen in the lower socioeconomic populations.
Clinically Relevant Anatomy[edit | edit source]
Reactive arthritis is not limited to inflamed joints, as it can also lead to symptoms in other body systems. For example in the ophthalmological, genitourinary, dermatological, musculoskeletal and gastrointestinal systems.[5][6]
Characteristics/Clinical Presentation[edit | edit source]
Symptoms can be found in different parts of the body. [5] [7]
Urethritis, conjunctivitis, and arthritis are the three symptoms classically associated with ReA
- Urethritis discharge is intermittent and may be asymptomatic.
- Conjunctivitis is usually minimal.
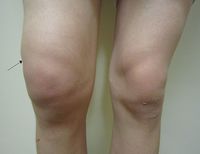
- The arthritis is usually asymmetrical and polyarticular occurring in the large joints of the lower extremities, including the knees, ankles, and 1st metatarsophalangeal. In some cases, hand joints may be involved. Individuals can also present with fungal infections (uveitis, keratitis) of the cornea.
Individuals can present with three musculoskeletal manifestations
- acute inflammatory arthritis,
- inflammatory back pain, and
- enthesitis (inflammation of the tendon at its insertion onto bone).
It is uncommon for all three musculoskeletal manifestations to present at one time. Enthesitis most commonly occurs at the insertion of the Achilles tendon onto the calcaneus causing heel pain. Enthesitis may also occur at the ischial tuberosity, iliac crest, tibial tuberosity, and ribs, with patient complaints of musculoskeletal pain at these sites. It is imperative that a complete and thorough history should be done on these patients during their initial evaluation to rule out presence of ReA
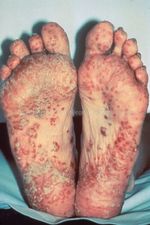
ReA can have integumentary manifestations similar to psoriasis, a condition that causes dry, erythematous skin lesions that can occur in small patches or cover large surfaces. It commonly involves the toes, nails, and soles of feet.
The initial illness typically resolves in 3-4 months, however, 50% of patients experience reoccurrence of symptoms and components of the syndrome over a period of years. Joint deformity and ankylosis, as well as sacroiliitis and spondylitis, may occur with chronic or recurrent RS.
Associated Co-morbidities and Systemic Involvement [edit | edit source]
Musculoskeletal manifestations are acute inflammatory arthritis, inflammatory back pain (in severe cases), and enthesitis. Enthesitis is inflammation at the insertion of tendons and ligaments into bones. Dactylitis or "sausage digit", plantar fascitis, and Achilles tendinitis are the most common sites.[3][4][8][2]
Skin lesions are very similar to those of psoriasis[4][8]
Constitutional symptoms include fatigue, malaise, fever, and weight loss[4][8][2]
Cardiovascular involvement with aortitis, aortic insufficiency, and conduction defects occur rarely.[4]
ReA is associated with and maybe the presenting symptom of HIV.[3] It is also associated with or triggered by Shigella, Salmonella, Yersinia, Campylobacter, and Chlamydia.[4][8][2]
Enhancing Healthcare Team Outcomes[edit | edit source]
Reactive arthritis is a multiorgan disorder that is best managed by a team of healthcare professionals that includes a rheumatologist, ophthalmologist, gastroenterologist, physical therapist, nurse, and pharmacist. The general physicians should explore the detailed history of sexual contacts and genital symptoms.[1]
- The pharmacist should educate the patient on the types of drugs used, their benefits and side effects.
- A consult with a dermatologist is recommended to assess skin lesions and recommend treatment.
- Physiotherapists should provide patient education to help improve physical conditioning, function, and quality of life.
- A nurse practitioner should educate the patient about safe sex practices to prevent STDs.
- A mental health nurse should follow patients with anxiety and depression,
- An ophthalmologist consul is advised as they remain at high risk for visual problems
Medications[edit | edit source]
- If an infectious agent has been identified as a trigger for reactive arthritis, antimicrobial therapy is strongly recommended often for a long term of 3 to 6 months. It can significantly shorten the time to remission. [16] Treatment of the underlying concomitant infection, if present should be initiated without delay. Patients who do not have active infection do not benefit from antibiotic therapy.[1]
- No treatment is necessary for conjunctivitis or mucocutaneous lesions, although topical opthalmic glucocorticosteroidsiritis may be required to treat iritis. Arthritis is treated with NSAIDs in doses similar to those used for rheumatoid arthritis.
- Enthesopathy may need to be treated with local injection of corticosteroids, to decrease inflammation at the site of the injection.[4][9]
- Surgery is rarely indicated but may include synovectomy, fusion, or tendon repair.[9]
The goals of therapy in reactive arthritis is to provide symptomatic relief and prevent chronic complications.
- Non-steroidal anti-inflammatory drugs (NSAIDS) are the initial treatment of choice in the acute phase.
- Intra-articular or local glucocorticoids as in case of enthesitis or bursitis can be used if the patient has mono/oligoarthritis. Systemic use of glucocorticoids is limited to severe polyarthritis, cardiac and ocular manifestations.
- Mechanical devices like orthotics and insoles can be useful.
- Disease-modifying antirheumatic drugs (DMARDs), mainly Sulphasalazine have been shown to be effective in both acute and chronic ReA.
- Other agents such as methotrexate and azathioprine have shown to be useful in chronic arthritis. They are indicated in patients who have failed Nonsteroidal anti-inflammatory drug (NSAID) therapy. Biologicals such as tumor necrosis factor (TNF) blocking agents (e.g., and infliximab and etanercept have been suggested in the treatment of reactive arthritis. However, further studies are needed to determine their definitive indications.[1]
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
Due to various manifestations of the disease occurring at different times, a diagnosis may take months to establish. The combination of peripheral arthritis with urethritis lasting longer than 1 month is necessary before the diagnosis can be confirmed. Laboratory tests typically reveal an aggressive inflammatory process. Elevated erythrocyte sedimentation rate (ESR) and C-reactive protein are detected. Other common findings include thrombocytosis and leukocytosis. The presence of certain bacteria in urine samples, genital swabs, and stool cultures can be used to identify the infection through laboratory tests.
Positive gonococcal cultures and a rapid response to penicillin therapy differentiate acute gonococcal arthritis from ReA in sexually active young patients, as individuals with ReA will not respond to the penicillin treatment. Radiographic abnormalities may include asymmetric involvement of the lower extremity diarthroses, amphiarthroses, symphyses, and entheses in the affected joints. Poorly defined bony erosions with adjacent bony proliferation or paravertebral ossification may present on x-ray review. [3][4][8][2]
An MRI is the diagnostic imaging of choice to help diagnose ReA. The affected bone will present with a moth-eaten appearance, bony expansion, and loss of cortical definition. Bone scans can also be used in conjunction with an MRI and will exhibit increase uptake. The bony destruction lesions can cross epiphyseal growth plates, joints, and discs.[10]
Differential Diagnosis [edit | edit source]
Below is a list of other conditions with similar symptoms:[11] [8]
- Psoriatic Arthritis
- Pityriasis Rubra Pilaris
- Lichen Planus
- Lupus Erythematosus
- Dermatomyositis
- Behcet's Disease
- Arthritis associated with Gonococcal Disease
- Rheumatoid Arthritis
- Septic Arthritis
- Mycosis Fungoides
- Subcorneal Pustulosis of Sneddon-Wilkinson
- Atopic Dermatitis
- Acute Exanthematous Pustulosis
- Other causes of Exfoliative Dermatitis
Diagnostic Procedures[edit | edit source]
Microbiological and serological studies are needed. [5]
The following laboratory tests are completed: CBC (=complete blood count), ESR (= erythrocyte sedimentation rate), CRP (= C-reactive protein), RF (= rheumatoid factor), ANA (= antinuclear antibody), HLA-B27 (=Human leukocyte antigen B27). [6]
Usually, ESR and CRP are higher in the acute phase and become normal in the chronic stage. RF and ANA are analysed to rule out other causes of arthritis. HLA-B27 is tested as the presence of this antigen is associated with a higher risk of developing reactive arthritis. [6]
Evidence of the disease in the form of limited spinal movements or radiological syndesmophytes may already be evident. Radiographs may show syndesmophytes in the presence or absence of spinal symptoms.
Possible microorganisms causing reactive arthritis include:
- Chlamydia trachomatis
- Shigella flexneri
- Salmonella enteritidis
- Salmonella typhimurium
- Yersinia enterocolitica
- Yersinia pseudotuberculosis
- Campylobacter Jejuni [5][6][7][12]
A few characteristics must be examined, to analyze the probability of reactive arthritis:
- Mono- or oligoarthritis of the lower extremities.
- Exclusion of other diagnoses including septic or traumatic arthritis and the other rarer conditions=> 1+2 = probability ReA 40%
- Previous infection = probability ReA 60% (most relevant criterion)
- History of symptomatic preceding infection with Chlamydia trachomatis = probability ReA 90%.[6]
Outcome Measures[edit | edit source]
Appropriate outcome measures are specific to the affected joint(s). Measurements of swelling (i.e. circumference of joint) and effusion tests may be used to document a reduction in joint swelling over time.
Outcome measures used can be:
- Disease activity index for the assessment of reactive arthritis (DAREA)[13]
- Arthritis Impact Measures I and II
See Outcome Measures Database for joint-specific outcome measures.
Outcomes[edit | edit source]
- The progression of reactive arthritis is variable, but in most people, the disorder is self-limited with the resolution of the symptoms occurring by 6-18 months. Mortality is very rare today and is usually due to the treatments.
- Causes related to sexually transmitted infections have a worse outcome than those caused by gastrointestinal infections.
- Despite a cure, recurrences are known to occur in 25-50% of cases, especially those who are HLA-B27 positive.
- Reactivation may signal a new infection or stress.
- About 20% of patients will have a long-term disease that results in enthesitis and destructive arthritis.
- Elevation of ESR, lack of response to NSAIDs and involvement of the hip joint usually is indicative of poor outcome[1]
Physical Therapy Management[edit | edit source]
Physical Therapy is helpful during the recovery phase of the disease (after exacerbation of symptoms has ceased). Physical Therapy should follow a program similar to that given to a patient with arthritis.
- Patient education - this is necessary to promote joint protection and proper body mechanics when performing daily activities to maintain joint integrity.
- Exercise regimen - that includes regular aerobic activity, as well as exercises that promote the joint range of motion and muscles strengthening should be utilized.
- Aerobic exercise should include low impact activities, such as swimming, walking, or recumbant bike, depending on the patient's cardiovascular level.
- Strengthening should target muscles surrounding the affected joints with the purpose of improving its support system.
- for the acute joint inflammation, provide advice to avoid overuse.[6] [14]
- If enthesitis is present, heel support and orthosis can be considered to decrease pain and thus improve mobility. [6] [14] [12] [15] You may choose to recommend a short period of non-weight bearing, to decrease the inflammation and limit the pressure of the body on the inflamed joints.
- Stretching and ROM exercises should be completed to prevent muscle atrophy, especially if several joints are involved. [6] [14] The objective of physiotherapy is to avoid stiffness and deformities and to promote mobility and strength.[12][16]
- When recovery takes place, patients must be advised not to overload their joints too soon, to avoid minor traumas which can cause a relapse. [5] [14]
Immobilization and inactivity are discouraged as they can lead to decreased range of motion, contractures, joint stiffness, decreased muscle strength and decreased flexibility, as well as overall decreased cardiovascular fitness, which can cause a cascade effect on other body systems. Goals of treatment should include pain relief, improved activities of daily living, reduce joint swelling, prevention of joint damage and disability.[2][9][17]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Cheeti A, Chakraborty RK, Ramphul K. Reactive Arthritis (Reiter Syndrome). Available from: https://www.ncbi.nlm.nih.gov/books/NBK499831/ (last accessed 24.12.2019)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Developed by R. Reiter's Syndrome. CRS - Adult Health Advisor [serial on the Internet]. (2009, July), [cited April 5, 2010]; 1. Available from: Health Source - Consumer Edition.
- ↑ 3.0 3.1 3.2 3.3 Goodman CC, Fuller KS. Pathology Implications for the Physical Therapist. 3rd ed. St. Louis, MO: Saunders Elsevier; 2009.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 Porter RS, Kaplan JL. The Merck manual of diagnosis and therapy. Merck Sharp & Dohme Corp.; 2011.
- ↑ 5.0 5.1 5.2 5.3 5.4 Toivanen A, Toivanen P. Reactive arthritis. Best Practice & Research Clinical Rheumatology. 2004 Oct 1;18(5):689-703.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 Kim PS, Klausmeier TL, Orr DP. Reactive arthritis: a review. J Adolesc Health 2009;44:309–315. (A1)
- ↑ 7.0 7.1 Leirisalo-Repo M. Reactive arthritis. Scand J Rheumatol 2005;34:251–259. (A1)
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL. Harrison's Manual of Medicine. 16th ed. McGraw-Hill, 2005
- ↑ 9.0 9.1 9.2 Reactive Arthritis (Reiter's Syndrome). Treatment Strategies. 2009 Jan 10. In ProQuest Medical Library. Cited 2010, Mar 20. Available from: http://www.proquest.com/;DocumentID:1871950901
- ↑ Lonnemann E. Spondylogenic & Immunological Disorders. [PowerPoint]. Louisville, KY: Bellarmine University Doctorate of Physical Therapy Program; 2014.
- ↑ ↑ Reiter Syndrome. In:ProQuest Medical Library. Avaiable from: http://www.proquest.com/;DocumentID:1871990641. Cited 2010 Mar 20
- ↑ 12.0 12.1 12.2 Koehler L, Kuipers JG, Zeidler H. Managing seronegative spondarthritides. Rheumatol 2000;39:360-368. (A1)
- ↑ G. Eberl, A. Studnicka‐Benke, H. Hitzelhammer, F. Gschnait, J. S. Smolen, Development of a disease activity index for the assessment of reactive arthritis (DAREA), Rheumatology, Volume 39, Issue 2, February 2000, Pages 148–155.
- ↑ 14.0 14.1 14.2 14.3 Toivanen A. Managing reactive arthritis. Rheumatol 2000;39:117-121. (D)
- ↑ Olivieri I, Barozzi L, Padula A. Enthesiopathy: clinical manifestations, imaging and treatment. Baillieres Clin Rheumatol 1998;12(4). (A1)
- ↑ Rihl M, Klos A, Köhler L, Kuipers JG. Reactive arthritis. Best Pract Res Clin Rheumatol 2006;20(6):1119-1137. (D)
- ↑ Mayoclinic.com Website. Reactive Arthritis: Treatment and Drugs. Accessed March 4, 2010. Available at:http://www.mayoclinic.com/health/reactive-arthritis/DS00486/DSECTION=treatments-and-drugs