Septic (Infectious) Arthritis
Original Editors - Kelli House and Kelly Condren, Student Physical Therapists from Bellarmine University's Differential Diagnosis of Complex Patient Problems project.
Top Contributors - Amy Bramble, Kelli House, Kim Jackson, Lucinda hampton, Admin, Elaine Lonnemann, WikiSysop, 127.0.0.1, Jill Thompson, Wendy Walker, Lauren Lopez, Khloud Shreif and Nupur Smit Shah
Definition/Description[edit | edit source]
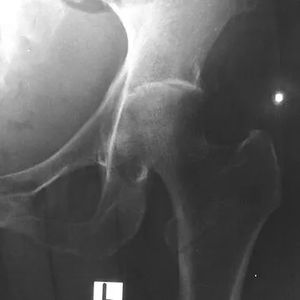
Septic arthritis is also commonly referred to as bacterial or infectious arthritis. Septic arthritis is an intensely painful infection in a joint. [1]Bacteria, viruses, and fungi may invade the joint through various routes that cause inflammation of the synovial membrane. [2] With the onset of inflammation, cytokines and proteases are released, thus resulting in potential joint destruction. [3] The infection is located in the synovial or periarticular tissues and is most commonly bacterial. [4] The image shows Septic arthritis of the left hip joint with melioidosis.
Though uncommon, septic arthritis is an orthopedic emergency that can cause significant joint damage leading to increased morbidity and mortality.[5] Bacteria or other foreign pathogens can infect either one joint or, if left untreated, can spread and cause further systemic damage. Patients and caregivers need to be educated about the severity of this condition and the potential for increased morbidity even after successful antibiotic treatment.
Septic arthritis may occur at any age but is more likely in children and older adults. The most commonly targeted joints in the body are the knee, hip, shoulder, ankle, and wrists. [6]
Epidemiology[edit | edit source]
The incidence of septic arthritis is between 2 to 6 cases per 100,000 people however rates vary based on the presence of risk factors.
- Septic arthritis is more common in children than in adults.
- The incidence of septic arthritis peaks between ages 2 and 3 years and has a male predominance.
- Subgroups of children at high risk include neonates, hemophiliacs with hemarthroses, immunocompromised (e.g., sickle cell anemia, human immunodeficiency virus infection), and those treated with chemotherapy.
- Risk factors in adults include age older than 80, diabetes mellitus, rheumatoid arthritis, recent joint surgery, joint prosthesis, previous intra-articular injection, skin infections and cutaneous ulcers, Human immunodeficiency virus, osteoarthritis, sexual activity (especially in cases of suspected gonococcal septic arthritis), other causes of sepsis[5]
- A large population-based study in the UK showed that the incidence of septic arthritis is increasing. Rates are increasing most rapidly in the >75 years age group, which is likely the result of increasing co-morbidities[7].
Etiology[edit | edit source]
The bacterial or viral infection enters the joint via the bloodstream in three different ways:
- Direct inoculation via surgery, arthroscopy, injection, central lines, or total joint replacements.
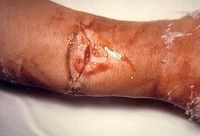
- A wound that that breaks the skin such as a bite, cut, or open fracture.
- Another systemic infection such as osteomyelitis, cellulitis, diverticulitis, or an abscess reaches the joint causing another infection.
Multiple Etiologies in the Pediatric Age Group[edit | edit source]
Staphylococcus aureus is the most common bacterial pathogen overall. The hip joint is most commonly affected in children.
Some etiologic agents are associated with specific age groups and underlying medical conditions.
- Kingella kingae is the most common gram-negative bacterial cause in children younger than 2 to 3 years.
- Group B Streptococcus, Staphylococcus aureus, Neisseria gonorrhea, and gram-negative Bacilli are common among neonates.
- Neisseria gonorrhea is a concern in sexually active adolescents.
- Salmonella species infection is associated with sickle cell disease.
- Patients on prolonged antibiotic therapy are at risk for fungal infections.
- Puncture wounds and injection drug use are associated with joint infection due to Pseudomonas aeruginosa.
Etiology in Adults[edit | edit source]
Staphylococcus aureus is the most common infecting organism in adults. The knee is the most commonly affected joint in adults followed by the hip.
- Streptococcus pneumonia is less common, but still a significant source of infection in adults.
- Salmonella in patients with sickle cell,
- Pseudomonas in trauma/puncture wounds.
- In young sexually active patients, nontraumatic acute monoarthritis is most frequently caused by Neisseria gonorrhea. In high-risk patients, Neisseria gonorrhea should be cultured from other sites such as the oropharynx, vagina, cervix, urethra or anus as the organism grows poorly from cultured synovial fluid.
- Fungal and mycobacterial organisms present insidiously and may be more difficult to diagnose. The acid-fast smear of synovial fluid is often negative, but synovial biopsy is positive in 95% of cases. [5]
Associated Risk Factors[edit | edit source]
Two of the most important factors that put a patient at risk are a pre-existing joint pathology, especially Rheumatoid Arthritis, or a recent prosthetic joint surgery.[3][8] Other risk factors to be considered are:
- Increasing age
- History of infection of any kind
- Autoimmune conditions such as Systemic Lupus Erythematosus
- Scleroderma or mixed connective tissue disease
- Diabetes
- Sarcoidosis
- Human bite or tick bite
- Fracture
- Central line placement
- Indwelling catheter
- Immunocompromised condition eg Human Immunodeficiency Virus (HIV)
- Chronic joint damage (RA, OA)
- Sexually transmitted infection
- Injection drug user
- Alcoholism
- Recent immunization
- Malnutrition
- Skin breakdown
- Rarely seen is a case of Infectious Arthritis as a complication from ACL reconstruction due to contaminated bone-tendon-bone allografts.
Characteristics/Clinical Presentation[edit | edit source]
The typical presentation of septic arthritis in children and adults includes:[2][3][4]
- Acute, rapid onset of pain
- Unable to move the joint through active and passive range of motion
- Typically only one joint (can be bilateral or more than one joint depending on the type of infection)
- Unable to bear any weight on the joint
- Effusion
- Joint warmth
- Skin rash
- Low-grade fever
- Lymphadenopathy
- The joints of the arms and legs are the most commonly affected in adults (especially the knees)
- The hip joint is most commonly affected in children
Symptoms in Newborns/Infants: [9]
- Cries when the infected joint is moved
- Fever
- Unable to move the limb
- Irritability
Note: A patient may be taking medications for other types of arthritis that may mask the original signs and symptoms of septic arthritis. Early diagnosis for proper treatment is critical. [1]
Prognosis[edit | edit source]
Despite antibiotic use, there is a 7% to 15% mortality rate for in-hospital septic arthritis. Morbidity from septic arthritis occurs in one-third of patients. Both morbidity and mortality increase with patient age, comorbid conditions including pre-existing joint disease, and prior synthetic intra-articular material. Hence the need for a high index of suspicion, early diagnosis and prompt treatment for septic arthritis particularly in patients with known predisposing risk factors and comorbid conditions.[5]
Medical Management [edit | edit source]
The course of treatment for septic arthritis is case dependent. There is no conclusive evidence on the most effective way to begin[10]. However, it is a combination of antibiotics, joint fluid removal, infection drainage, and/or total joint surgery. The course of treatment also depends on the type of joint invasion (bacterial, STD bacterial, viral etc..). The first round antibiotics can be directed at the most likely pathogen, then the joint can be tested to see what further treatment may be necessary such as needle joint aspiration or drainage to release the fluid. Another option is to perform joint aspiration before a round of antibiotics is chosen. If the infection is severe enough following a round of antibiotics and aspiration for fluid removal, surgery or even replacement of the entire joint may be necessary. [4]
Antibiotic Treatment[edit | edit source]
Typically, the sexually transmitted related bacteria (gonococcal) is treated with antibiotics that other sexually transmitted infections are treated with. For example, doxycycline, ciproflaxin, and azithromyocin, amongst many others. The non-sexually transmitted bacterial infections can be treated with common antibiotics such as penecillin, vancomyocin, (etc), depending on the severity and resistance tendencies of the bacterial strain. [4][6] Below is non-exhaustive list of antibiotics commonly used in the treatment of septic arthritis: [6]
- Ceftriaxone (Rocephin)- Effective against gram-negative enteric rods
- Ciprofloxacin (Cipro) - Treat N gonorrhoeae and gram-negative enteric rods.
- Cefixime (Suprax) –Broad activity against gram-negative bacteria, by binding to one or more of the penicillin-binding proteins. Arrests bacterial cell wall synthesis and inhibits bacterial growth.
- Oxacillin - Oxacillin is useful against methicillin-sensitive S aureus (MSSA).
- Vancomycin (Vancocin) - An anti-infective agent used against methicillin-sensitive S aureus (MSSA), methicillin-resistant coagulase-negative S aureus (CONS), and ampicillin-resistant enterococci in patients allergic to penicillin.
- Linezolid (Zyvox) - An alternative antibiotic that is used in patients allergic to vancomycin and for the treatment of vancomycin-resistant enterococci.
Management regarding antibiotic choice, dosage, route of administration, and duration of treatment is unknown in the treatment of septic arthritis. In addition, no evidence has shown if closed aspiration or open arthroscopy is better at removing materials from a joint that’s infected.[8]
Joint Drainage and Surgical Interventions[edit | edit source]
Joint Drainage and Surgical options are often used in combination with antibiotic treatment. Much like antibiotics, the choice of whether to use joint aspiration, arthroscopy, or total joint replacement is case dependent. There is no current definitive evidence on whether one treatment is more effective than the other. However, the most positive outcomes, in general, come from using one of these options. The main goal of this treatment is to continuously remove the accumulation of pus within the joint until it no longer forms. This is most commonly used in combination with the antibiotics to remove the pus both from the joint itself and via the bloodstream. [4][10]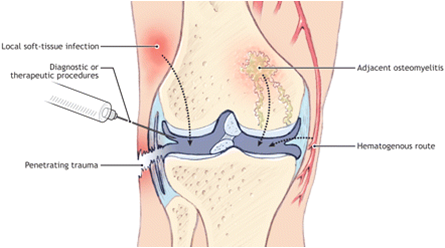 [11]
[11]
Diagnostic Tests/Lab Tests/Lab Values [1][edit | edit source]
Joint Aspiration[edit | edit source]
Needle joint aspiration can be used as both a diagnostic tool and a treatment. A portion of the fluid can be taken out by aspiration needle to determine the type of bacteria causing the infection thus determining further course of treatment.
Other Diagnostic Lab Values[edit | edit source]
- Arthrocentesis with synovial fluid examination and culture
- Increased White blood cell count
- Increased Erythrocyte sedimentation rate (ESR)
- Increased Temperature
- Increased C-Reactive Protein (CRP)
- Imaging studies are used to rule out other conditions
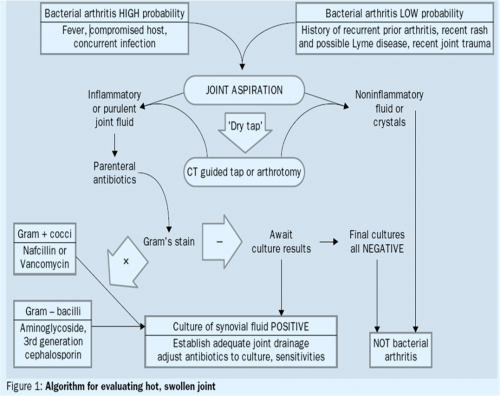
Below is an algorithm developed from a systematic review of bacterial septic arthritis patients for evaluating a hot swollen joint:
Physical Therapy Management[edit | edit source]
Patients with septic arthritis are usually managed initially in the inpatient hospital setting and require an interprofessional team of caregivers including the primary care provider, physical and occupational therapist, nurses and wound care team. At the time of discharge, some patients can return home while others with increased debility may need ongoing physical therapy at either an acute or subacute rehabilitation facility. The social workers in the hospital help to ensure a smooth transition from inpatient to outpatient care.[5].
The initial treatment of infectious arthritis is outside of the scope of physical therapy. It is important, first, for the physical therapist to recognize the signs and symptoms of the infection and refer out for other medical treatment. Subjective history, in combination with the physical therapist’s objective findings, is important in order to recognize the risk factors that make septic arthritis the likely diagnosis. It is important to immobilize the joint in this stage to best manage the patient’s pain and to decrease the likelihood of doing further damage to the joint until proper treatment can occur.
Once the patient receives a round of antibiotic treatment in combination with either joint aspiration, debridement, or arthroscopy, the patient may then be referred back to physical therapy including
- educate on how to properly protect the affected joint.
- Gentle mobilization of the infected joint can begin if the patient is responding well following 5 days of medical treatment.
- Once the infection is well-managed, current evidence states the patient will usually respond best to aggressive physical therapy to allow maximum post-infection functioning.
- Physical therapy needs to consist of allowing the joint to be in its functional position and positioning the joint to allow passive range of motion activities.
Differential Diagnosis[edit | edit source]
Differential diagnosis of acute monoarticular arthritis include:[5]
- Infection: Bacterial, fungal, viral, spirochete, mycoplasma
- Crystal-induced arthropathies: Acute gout, pseudogout, calcium oxalate, cholesterol, hydroxyapatite crystals
- Osteoarthritis
- Intra-articular injury: Fracture, meniscal tear, osteonecrosis, foreign body, plant thorn synovitis
- Inflammatory arthritis: Rheumatoid arthritis, Bechet syndrome, seronegative spondyloarthropathies such as ankylosing spondylitis, psoriatic arthritis, reactive arthritis, inflammatory bowel disease-related arthritis; Sarcoid, systemic Lupus erythematosus, Still disease
- Systemic infection: Bacterial endocarditis, human immunodeficiency virus, Lyme arthritis
- Tumor: Metastasis, pigmented villonodular synovitis
- Other: Hemarthrosis, clotting disorders or anticoagulant therapy, neuropathic arthropathy, dialysis-related amyloidosis, avascular necrosis
Conclusion[edit | edit source]
Septic arthritis is an uncommon orthopedic emergency that requires a high level of suspicion for diagnosis in a patient with risk factors. There are high morbidity and mortality in elderly patients and those with previous arthritis or intra-articular prosthesis even with adequate treatment. Septic arthritis usually presents as an acute monoarticular joint inflammation which has a broad differential diagnosis. Arthrocentesis is a crucial component in the diagnostic algorithm. Joint drainage either by daily needle aspiration, arthroscopy or arthrotomy is usually done as soon as possible by orthopedic surgery, but interventional radiology consultation may be required for axial joint drainage. Infectious disease consultation early in treatment ensures adequate antibiotic coverage and duration of therapy based on culture results. Progressive physiotherapy for affected joints is vital for the preservation of function and reduced ongoing disability.[5]
Case Reports/ Case Studies[edit | edit source]
Septic arthritis in patients with pre-existing inflammatory arthritis: case based review
A 56 year old female with a history of inflammatory arthritis presents with additional symptoms indicative of a joint infection. This case highlights the importance of distinguishing septic arthritis from the symptoms of a chronic inflammatory arthritis condition through both subjective and objective evaluation.
Staphylococcus lugdunensis Septic Arthritis of a Native Knee: A Case Report
A 35 year old male is diagnosed with a rare bacterial infection in the knee joint causing septic arthritis. This case addresses a rare risk factor (ACL revision) demonstrating this can occur in a younger population and the importance of immediate diagnosis and proper treatment in order to significantly reduce the recovery timeline.
Immunoglobulin G deficiency-associated septic arthritis identified following corticosteroid injection and knee arthroscopy
A 53 year old with immune deficiency presents with septic arthritis possibly due to complications of a series of corticosteroid injections and arthroscopic surgeries, and history of recurrent infections. This case addresses several risk factors possible contributing to his septic arthritis and the need to be aware of other underlying systemic causes that may require further evaluation.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Mayo Clinic [Internet]. Mayo Foundation for Medical Education and Research; 2015 [cited 2017 April 4]. Availablefrom: http://www.mayoclinic.com/health/bone-and-joint-infections/DS00545
- ↑ 2.0 2.1 Goodman CC, Fuller KS. Pathology: implications for the physical therapist. 4th ed. St. Louis: Saunders Elsevier; 2014.
- ↑ 3.0 3.1 3.2 Goodman CC, Snyder TEK. Differential diagnosis for physical therapists: screening for referral. 5th ed. St. Louis: Saunders Elsevier; 2012.
- ↑ 4.0 4.1 4.2 4.3 4.4 The Merck Manual [Internet]. Whitehouse Station: Merck Sharp & Dohme Corp.; 2014 [cited 2017 April 4]. Available from: http://www.merckmanuals.com/professional/musculoskeletal_and_connective_tissue_disorders/infections_of_joints_and_bones/acute_infectious_arthritis.html#v907387
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 Momodu II, Savaliya V. Septic Arthritis. InStatPearls [Internet] 2019 Apr 2. StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538176/ (last accessed 25.12.2019)
- ↑ 6.0 6.1 6.2 Brusch, J. Medscape [Internet]. Septic Arthritis; 2016 [updated 2016 October 21; [cited 2017 April 4] Available from: http://emedicine.medscape.com/article/236299-overview#aw2aab6b2b3aa
- ↑ Rutherford AI, Subesinghe S, Bharucha T, Ibrahim F, Kleymann A, Galloway JB. A population study of the reported incidence of native joint septic arthritis in the United Kingdom between 1998 and 2013. Rheumatology. 2016 Sep 16;55(12):2176-80. Available from: https://academic.oup.com/rheumatology/article/55/12/2176/2631602 (last accessed 25.12.2019)
- ↑ 8.0 8.1 Matthews CJ, Kingsley G, Field M, Jones A, Weston VC, Phillips M, et al. Management of septic arthritis: a systematic review. Ann Rheum Dis. 2007 [cited 2017 April 4]; 66: 440-45. Available from NCBI with Full Text: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1856038/pdf/440.pdf
- ↑ Pub med [Internet]. Bethesda: National Center for Biotechnology Information; 2012 [cited 2017 April 4]. Available from : http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001466/
- ↑ 10.0 10.1 Matthews CJ, Weston VC, Jones A, Field M, Coakley G. Bacterial septic arthritis in adults. The Lancet. [Internet] [Cited 2017 March 28] ;2010;375(9717):846-855. Available from: http://www.sciencedirect.com/science/article/pii/S0140673609615956
- ↑ Kherani R, Shojania K. Septic arthritis in patients with preexisting inflammatory arthritis. Canadian Medical Association Journal [Internet]. 2007 May 22 [cited 2017 April 4];176(11):1605–8. Available from: http://www.cmaj.ca/content/176/11/1605.full.pdf html?sid=6119ba81-df57-4f78-9118-4f8142ea4cb7
- ↑ 12.0 12.1 YouTube. Septic arthritis of the knee arthroscopic debridement. Available at: http://www.youtube.com/watch?v=0AOv06XWCps. (Accessed 2017 April 3).