Gut Brain Axis (GBA)
Original Editor - lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
One of the most cutting-edge areas of research involves the gut-brain axis (GBA) ie the connection between the brain, gut, and microbiome and its potentially huge influence over our health.
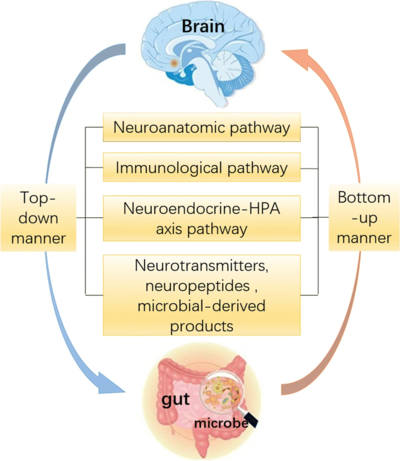
Our gut and brain are closely connected. They communicate with each other through the GBA, a bidirectional link between the central nervous system and the enteric nervous system (ENS) of the body. The ENS is a web of sensory neurons, motor neurons, and interneurons embedded in the wall of the gastrointesinal system, stretching from the lower third of the esophagus right through to the rectum. It links, via direct and indirect pathways, cognitive and emotional centres in the brain, with peripheral intestinal functions.
The GBA involves complex crosstalk with the brain sending messages to the gut and vice versa.
- This interaction occurs between the endocrine (hypothalamic-pituitary-adrenal axis), immune (cytokine and chemokines) and the autonomic nervous systems (ANS)[1].
- Plays a role in irritable bowel syndrome, celiac disease, and colitis.
- Stress signals from the brain can influence digestion through this axis, and the gut can also send signals that similarly influence the brain. Gut microbes appear to play a key role in sending and receiving these signals.
- The exponential growth of evidence detailing the bidirectional interactions between the gut microbiome and the brain supports a comprehensive model that integrates the central nervous, gastrointestinal, and immune systems with this newly discovered organ[2].
Gut Microbiota[edit | edit source]
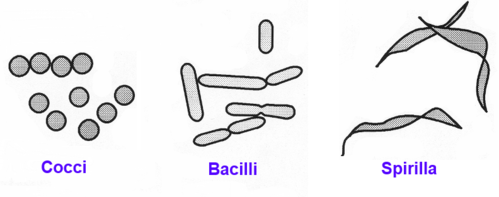
Gut microbiota is an assortment of microorganisms inhabiting the length and width of the mammalian gastrointestinal tract. The composition of this microbial community is host specific, evolving throughout an individual's lifetime and susceptible to both exogenous and endogenous modifications. A newborn is first exposed to the mother’s vaginal microbiota which influences the offsprings microbial signature. Studies show that the gut microbiota is central to the development and maturation of the human CNS and ENS in these early postnatal weeks.[1]
- Estimates of the number of bacterial species present in the human gut vary widely between different studies, but it has been generally accepted that it contains ∼500 to 1,000 species.
- It is estimated that the human microbiota is 10 times greater than the number of human cells present in our bodies. The microbiota colonizes virtually every surface of the human body that is exposed to the external environment eg on our skin and in the genitourinary, gastrointestinal, and respiratory tracts. The most heavily colonized organ is the gastrointestinal tract (GIT); the colon is estimated to contain over 70% of all the microbes in the human body.
- The human gut has an estimated surface area of a tennis court (200 m2) and, as such a large organ, represents a major surface for microbial colonization and the GIT is rich in molecules that can be used as nutrients by microbes, making it a preferred site for colonization.
- The overall balance in the composition of the gut microbial community, as well as the presence or absence of key species capable of effecting specific responses, is important in ensuring homeostasis or lack thereof at the intestinal mucosa and beyond.
- The majority of the gut microbiota is composed of strict anaerobes, which dominate the facultative anaerobes and aerobes by two to three orders of magnitude. There have been over 50 bacterial phyla described to date with the human gut microbiota being dominated by only 2 of them: the Bacteroidetes and the Firmicutes[3].
- Production of Microbial Metabolites: Many species of Lactobacillus and Bifidobacterium produce gamma-aminobutyric acid (GABA), which is the main inhibitory neurotransmitter in the brain. Other bacteria have been shown to produce the neurotransmitters serotonin and dopamine. Bacteria also produce short-chain fatty acid that are able to stimulate sympathetic nervous system, mucosal serotonin release and thus influence the memory and learning process in the brain[4].
- Gut microbiota can regulate host tryptophan levels, which is a main serotonin precursor. Peripherally, serotonin is involved in the regulation of GI secretion, motility (smooth muscle contraction and relaxation), and pain perception, whereas in the brain serotonin is implicated in regulating mood and cognition[5]. A dysfunctional serotonergic system is considered to be one of the main factors contributing to the development of depression (approximately 95% of Serotonin is produced by cells in the gut mucosal).
The Gut Brain Link[edit | edit source]
The gut and the brain links:
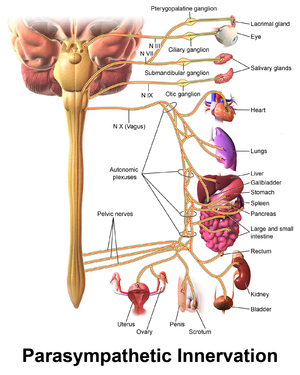
- The gastrointestinal tract is connected to the brain through the Vagus nerve. The vagus nerve links the heart, gastrointestinal tract, and lungs to the brain (like a cable that links the heart, gastrointestinal tract and lungs to the brain). Sensory neurons carry feedback from the intestinal end to the brain stem which then engages the hypothalamus (which is a brain region that controls hunger and emotions) and limbic system (the emotional nervous system). Similarly, descending projections from the limbic system (activated via stress) influence autonomic activity of the gut.
- Bacterial products stimulate neuroendocrine (gut hormone) signalling. Neuropeptides are the most diverse class of signaling molecules in the brain engaged in many physiological functions). These neuropeptides then enter the bloodstream and/or directly influence the enteric nervous system.
- The gut associated lymphoid tissue comprises 70% of the body’s immune system and can be conceptualised as the largest immune organ in the body.
Health Implications[edit | edit source]
The gut-brain axis refers to the two-way connection and communication between the gut and the brain. What is happening in the gut can directly influence our brain function and behaviour.
A correct communication between the gut bacteria and the brain is important in order to have adequate mental health. The GBA makes this communication possible. Scientists are still trying to understand exactly how this axis works. However, it is clear that there is an association between a healthy brain and the GBA.
- Diet is probably the most important strategy for maintaining a healthy GBA. A balanced diet, including fish, vegetables, cereals, fruits, and water is important to keep both a functional GBA and a good mood. The food that we consume has a direct impact on our bacteria and their home, our bodies[6].
- Patients suffering from depression may benefit from this research on the GBA. These patients might be able to improve their condition by eating a healthy diet. Our habits, such as diet, definitely influence our moods, so we should take care with our diets. Eat well and be happy!
- Changes in the GBA, caused by things like stress, can lead to digestive conditions such as IBS. This is due to activation of the body’s fight-or-flight response and changes in the gut microbiota.
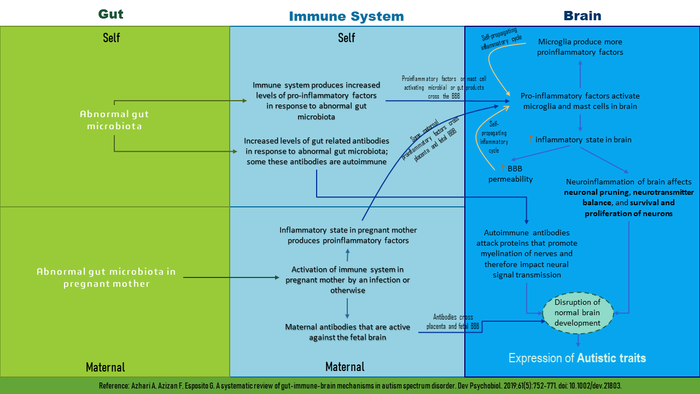
- Autism, a neurodevelopmental disorder, is characterized by a high level of social interaction insufficiency, impairment in language, and repetitive behavior. The gut–brain axis (GBA) is considered a bidirectional communication pathway between the gut and the brain. Growing evidence shows that the GBA contributes to the etiology of autism. The phenotypic behaviors of autism and the gastrointestinal problems that are comorbidity in autism are associated with modified gut microbiota[7]. See Image
- Dysbiosis in the gut microbiome is a direct factor that influences the GBA’ normal functioning and leads to mental health conditions like depression and anxiety.
- Data from preclinical and clinical studies have shown remarkable potential for novel treatment targets not only in functional gastrointestinal disorders but in a wide range of psychiatric and neurologic disorders, including Parkinson's disease, autism spectrum disorders, anxiety, and depression, among many others[2]
Image: Role of GBA in pathophysiology of Autism
See also
- Traumatic Experiences: Vagus Nerve, Microbiome, Heart Rate Variability (HRV) and Effects of Exercise
- Microbiome and exercise
References[edit | edit source]
- ↑ 1.0 1.1 Psyche Scene hub The Simplified Guide to the Gut-Brain Axis – How the Gut and The Brain Talk to Each Other Available from:https://psychscenehub.com/psychinsights/the-simplified-guide-to-the-gut-brain-axis/ (accessed 2.2.2021)
- ↑ 2.0 2.1 Martin CR, Osadchiy V, Kalani A, Mayer EA. The brain-gut-microbiome axis. Cellular and molecular gastroenterology and hepatology. 2018 Jan 1;6(2):133-48.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6047317/ (accessed 2.2.2021)
- ↑ Sekirov I, Russell SL, Antunes LC, Finlay BB. Gut microbiota in health and disease. Physiological reviews. 2010 Jul 1.Available from: https://journals.physiology.org/doi/full/10.1152/physrev.00045.2009?rfr_dat=cr_pub++0pubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org (accessed 2.2.2021)
- ↑ Diet vs disease The Gut-Brain Axis Explained in Plain English Available from:https://www.dietvsdisease.org/gut-brain-axis/ (accessed 2.2.2021)
- ↑ Lukić I, Getselter D, Koren O, Elliott E. Role of tryptophan in microbiota-induced depressive-like behavior: evidence from tryptophan depletion study. Frontiers in behavioral neuroscience. 2019 Jun 4;13:123 Available from:.https://www.frontiersin.org/articles/10.3389/fnbeh.2019.00123/full#h2 (accessed 3.2.2021)
- ↑ Frontiers Happy Gut Bacteria, Happy Brain: The Microbiota-Gut-Brain Axis Available fromhttps://kids.frontiersin.org/article/10.3389/frym.2019.00015 (accessed 3.2.2021)
- ↑ El-Ansary A, Bhat RS. Targeting gut microbiota as a possible therapeutic intervention in autism. InAutism 360° 2020 Jan 1 (pp. 301-327). Academic Press.AVAILABLE FROM:https://www.sciencedirect.com/science/article/pii/B9780128184660000174 (accessed 3.2.2021)