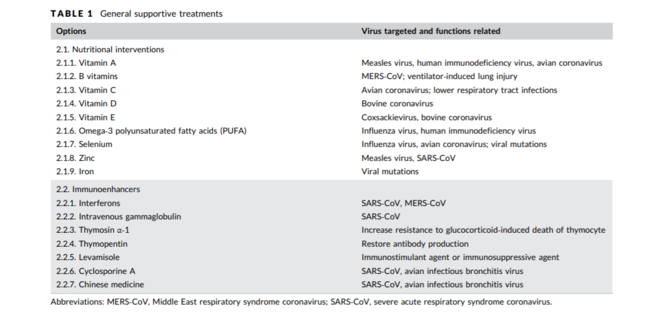
COVID-19 and Nutrition
Original Editor - Wanda van Niekerk
Top Contributors - Wanda van Niekerk, Lucinda hampton, Kim Jackson, Nikhil Benhur Abburi, Jess Bell, Olajumoke Ogunleye, Admin, Tarina van der Stockt and Uchechukwu Chukwuemeka
Introduction[edit | edit source]
The COVID-19 pandemic is posing severe threats to international health and the economy.
- At the moment there is still no cure for the disease
- Alternative methods need to be found to control the spread of the virus.[1]
COVID-19 is caused by specific Coronavirus (SARS-CoV 2). Coronaviruses primarily cause enzootic infections in animals but is capable of transferring to humans and causing infections eg
- Severe Acute Respiratory Syndrome (SARS) in 2002
- Middle East Respiratory Syndrome (MERS) in 2012.
- Both Zoonotic Diseases
The outbreaks of SARS, MERS and COVID-19 demonstrates how lethal Coronaviruses can be when they cross the species barrier and infect humans.[2]
- Interestingly, the genome structure of COVID-19 is 82% identical to that of the SARS- CoV genome.[3] Lessons learned from the SARS (2002) outbreak could be applied or tried to apply to COVID-19.
Symptoms of COVID-19 include
- Fever, cough, respiratory symptoms, shortness of breath, breathing difficulties, fatigue and a sore throat.
- A minority group of people will present with more severe symptoms and will need to be hospitalised, most often with pneumonia, and in some instances, the illness can include ARDS, sepsis and septic shock.[4]
- Not a cure for COVID-19 but healthy patterns of eating optimize the function of the immune system, improve immunometabolism, and are a modifiable contributor to the development of chronic disease that is highly associated with COVID-19 deaths.
- May have a positive impact on COVID-19 as it may be a way to support people at higher risk for the disease i.e. older people and people with pre-existing conditions (non-communicable diseases).
COVID-19 and Pre-existing Conditions[edit | edit source]
Evident that certain people are more at risk for severe illness if they contract the coronavirus.
- People at higher risk are often older people and people with one or more pre-existing conditions (non-communicable diseases).
- Global burden of pre-existing conditions is high, worldwide one in three of all adults suffer from multiple chronic conditions.[5]
Who is contracting COVID-19?[edit | edit source]
- Older people (65+ years)
- Diabetes (Type 1 and 2)
- Lung pneumonia
- Pre-diabetes
- Lung disease
- Cardiovascular disease
- Chronic obstructive pulmonary disease (COPD)
- Cerebrovascular disease
- Hypertension
- Bronchitis
- Emphysema
- Lung cancer
- Cystic fibrosis
- Asthma [6]
The world faces unique circumstances in this time, especially with regards to COVID-19 and the impact it has with regards to outcomes for people living with pre-existing (comorbid) conditions.[6]
- Statistics from Italy on Coronavirus deaths and pre-existing conditions indicate that: 14.4% of deaths had one pre-existing condition; 21.1% of deaths had two pre-existing conditions; 60.9% had three or more pre-existing conditions.[7]
- Worldometers has a section on COVID-19 by Comorbidity showing current statistics.
Physiotherapy Considerations for Clients with Pre-existing Conditions during COVID-19[edit | edit source]
Client History[edit | edit source]
As physiotherapists, we often treat people with pre-existing conditions and it is important to gather information about these specific conditions when taking a patients’ history, whether in a practice situation or via telehealth in the current global pandemic state. It gives you a good opportunity to educate your clients about pre-existing and chronic diseases, especially in times like we are facing now. We need to educate our clients on how to manage these conditions in various scenarios such as under lockdown or stay at home situations as well as later on when we are able to socialise more.
Medication History[edit | edit source]
Another good way to gain information about a clients’ medical history is to review their medication history. Often our clients will be taking drugs that are immunosuppressive in nature, for certain conditions such as pain, autoimmune diseases, Human Immunodeficiency Virus (HIV) and cancer.
Drugs that Suppress the Immune System[edit | edit source]
- Morphine and other Opiods[8]
- For example, codeine, demerol, hydrocodone
- Sometimes prescribed for chronic pain
- Prescribed to patients on ventilators
- When consulting with your chronic pain clients, if possible avoid prescribing these types of medication via telehealth to your clients and rather focus on other ways to manage and prevent their pain
- Causes nutritional deficiencies with regards to vitamin A, vitamin B's, Amino Acids, Zinc, Iron, Calcium, Chromium, Magnesium, and Potassium[8]
- Disease-modifying anti-rheumatic drugs
- For example, ciclosporin, cyclophospamite, and hydroxychloroquine
- Corticosteroids
- For example, Ethamethasone (celestone), prednisone, and prednisolone
- Non-steroidal anti-inflammatory drugs (NSAID's)
- For example, aspirin, celecoxib (celebrex), ibuprofen (motrin, advil), and naproxen (aleve)
- Research is limited on NSAID’s and its adverse effects on the immune system
- Potentially the short term or long term use of NSAID's may inhibit the body’s natural immune response and repair
- Bancos et al[9] (2009) reported that:
- A panel of widely used NSAID’S may blunt antibody synthesis in human B cells
- The reduction in antibody production was concentration (dosage) and time (short term vs long term use) dependent.
- Through decreasing antibody synthesis, NSAID’s may have the ability to weaken the immune system - this can have serious consequences for various populations such as children, the elderly and immune-compromised individuals.[9]
As NSAID’s are one of the most commonly used drugs and freely available over the counter, it is often recommended for all age categories and prescribed for relieving transient pain or in cases of inflammatory conditions/diseases.[9] Physiotherapists need to be aware of this and educate their clients about the use of NSAID’s and its possible effect on the body’s immune system.
COVID-19 and Diabetes[edit | edit source]
As mentioned there are many pre-existing or chronic conditions and all of them are risk factors for COVID-19. As an example Diabetes is discussed in consideration to COVID-19 as there is a link to lower respiratory tract infection and diabetes.
An individual with Diabetes may have:[10]
- An increased susceptibility to different kinds of respiratory infections (diabetes had been identified as an independent risk factor for developing lower respiratory tract infections)
- Increased frequency in pulmonary infections and this may be associated with increased morbidity and mortality
- Increased susceptibility to pneumococcal infections as a result of reduced defense capability of antibodies to protein antigens
- Increased risk of pulmonary tuberculosis (4-5 times more than in the non-diabetic population) due to a malfunction of monocytes
- 6 times more likely to be hospitalized due to influenza virus or flu-like infections (including the coronaviruses) compared to a healthy individual
Effect of a Poor Diet[edit | edit source]
An unhealthy diet is one of the major risk factors for a range of chronic diseases such as cardiovascular disease, diabetes, and obesity. A poor diet will lead to nutrient deficiency and this will likely lead to chronic disease.
Recent literature has shown that a poor or bad diet causes more deaths globally than either smoking or hypertension.[11] In 2017, the study of 195 countries, linked poor diet to 11 million deaths globally. That translates to 22% of deaths among adults in 2017.[11]
Poor nutrition drives chronic health conditions! Eating habits that have stronger links to higher death rates include[11]:
- Diets high in sodium
- Diets low in whole grains, fruit, vegetables, nuts, and seeds
People need to eat fewer processed foods and more "whole" plant-based foods.[11] Although there are differences in typical diets across the world, on the whole, unbalanced diets are a health threat across the globe and not just impacting death rates but also the quality of life.
In the United States, 1 out of 4 children and adults had lower dietary intakes of micronutrients such as Vitamins A, C, D, and E, magnesium. One in three Americans may be deficient in calcium, Zn, Se, Copper, Iron, Amino acids, fatty acids, and folate.[12] From worldwide studies, it is evident that nutritional deficiencies are a global problem and it gives you an idea of how people all over the world are coming into this COVID-19 pandemic with a disadvantage.
Nutrition and Social Determinants of Health[edit | edit source]
Nutrition is a social determinant of health. In order for physiotherapists to effectively counsel and advise their clients on nutritional intervention options as part of their treatment, it is important to be aware of the various factors that can contribute to diet-related disparities. These include[13]:
- Social Inequality
- Various factors are related to social inequality. These can include:
- Ethnicity
- Physical environment
- Language barriers
- Disability
- Immigrant status
- Residence (urban vs rural)
- For example, a lack of access to supermarkets with fresh produce may lead to a diet low in fresh fruit and vegetables.
- Education
- the level of education does impact knowledge of dietary recommendations and which foods are healthy vs less healthy.
- Income
- affects whether a person can afford to purchase healthy foods
- Various factors are related to social inequality. These can include:
- Psychosocial Factors
- Psychosocial factors may affect dietary intakes and therefore the risk of chronic disease. It has been shown that basic nutritional education by various professionals, including physiotherapists, can have an impact on a person’s health education and they are more likely to develop healthy eating habits. Belief in the relationship between diet and disease also affects healthy dietary intakes, as well as strong social support and familiarity with good nutritional guidelines.[14]
- Environmental Factors
- These can include the availability of healthy food choices (proximity, access, and cost of healthy foods to be considered) Learned behaviours such childhood dietary patterns also influence current/adult behaviours.
- Pollution needs to be considered as well.
- Cultural Factors
- Certain cultures eat certain food and these cultural factors influence the dietary preferences and behaviour of populations.
- Dietary Acculturation
- Dietary acculturation can be defined as “the extent to which immigrants adopt the dietary patterns of their host countries."[15]
Dietary Reference Intakes[edit | edit source]
Dietary Reference Intakes (DRIs) refers to a set of reference values that are used to plan and assess the nutrient intakes of healthy people.[16] The dietary reference intakes apply to healthy populations. Special guidance should be provided to populations with greatly increased nutritional requirements.
Dietary Reference Intakes include the following references:
- Recommended Dietary Allowance (RDA):
- an estimation of how much of a nutrient you need, based on your age, sex, and pregnancy status to maintain baseline health, not optimal health (therefore it does not take into consideration chronic disease, inflammatory conditions, or recovery from surgery, injury or infection and activity level).[17]
- Adequate Intake (AI):
- how much of a nutrient you need to avoid an obvious deficiency disease[17]
- Tolerable Upper Limit (UL):
- how much of a nutrient you can safely take without overdose[17]
Specific Nutritional Needs for Specific Populations during COVID-19[edit | edit source]
Specific Nutritional Needs of Older People[edit | edit source]
Population aging is a global trend and although it is a positive that most people live longer it also presents challenges with respect to health, quality of life, and economics.[18] The World Health Organisation (WHO) criteria on aging set the beginning of old age at 65 years, followed by the early elderly stage between 65 and 74 years, and 75+ years is considered late elderly.[19]
Healthy aging can be described as “leading a healthy, active, social and independent life in late years, through maintaining vitality and good quality of life for as long as possible.”[18]
Nutrition is an area that can be addressed to benefit older people and enhance healthy aging in a population. With aging, there is also an increased likelihood of developing[20]:
- Chronic diseases
- Decreased functional ability
- Cognitive decline
- Disability
Factors associated with aging that leads to inadequate nutrient intake are[18]:
- Impaired appetite
- Reduced food intake
- Repetitive dietary choices
- these will have consequences on:
- Weight
- Nutritional status
- Quality of life
- Mortality risk
- these will have consequences on:
Aging adults are more susceptible to[18]:
- A decrease in body weight
- A loss of muscle mass
Impaired appetite in older people may lead to reduced food intake. This can result in difficulties achieving recommended intakes for macro-nutrients such as protein and micro-nutrients such as vitamin D. This leads to reduced body weight and muscle mass.[18]
Good protein intake is necessary for older people to support[21]:
- Healing
- Skin integrity
- Immunity
- Recovery from illness
The recommended protein reference nutrient intake is 0.8 g protein/kg body-weight in healthy adults of all ages.[22] There are emerging evidence-based studies that recommend that increased protein intake may be beneficial to older people, especially those with chronic diseases.[23] Recent evidence shows that the recommended amounts of protein may be too low for elderly people. Seniors may need 1.0-1.3 grams of protein for every kilogram of body weight. eg if you weight 82 kg this could mean consuming 80-104 grams of protein every day, regardless of your calorie intake.[24]
Calcium and Vitamin D are recommended for older people to[25]:
- Prevent bone loss
- Maintain existing bone density
This may reduce the risk of falls and fractures.[25]
Intakes higher than the recommended nutritional intake have been shown to be beneficial for Vitamins A, B, E, Calcium, and Zinc.[26]
Causes of nutritional deficiencies such as physical and physiological changes in the body may lead to a reduced metabolic rate and loss of muscle mass in older people. This can lead to sarcopenia (the progressive depletion of muscle mass and loss in strength, which is associated with a risk of adverse outcomes) in older people.
Nutritional Interventions in Viral Infections[edit | edit source]
Vitamin D[edit | edit source]
- The "sunshine" hormone
- expose arms and legs, or chest and back to direct sunlight for between 10 - 30 minutes a day, taking in consideration the pigment of your skin.
- A nutrient as well as a hormone
- Can be synthesized in our body with the help of sunlight[1]
- Plays a role in bone integrity[1]
- Stimulates the maturation of cells, including immune cells
- Reports of healthy adults with low levels of Vitamin D, mostly at the end of winter[27]
- People who are housebound, institutionalized, night workers may have Vitamin D deficiency (something to consider in the current pandemic!)
- Many elderly people also have limited exposure to sunlight-so there is a chance of Vitamin D deficiency[28]
- COVID-19 was first identified in Winter of 2019 in the Northern Hemisphere - affects mostly middle-aged and elderly people
- Vitamin D reduces the risk of acute respiratory infections[29]
- Vitamin D supplementation is safe and protects against acute respiratory tract infection[29]
- In animal studies:
- a decrease Vitamin D status reported in calves had been reported to cause the infection of bovine coronavirus[30]
- The average daily recommendation is 600 IU
- The tolerable upper limit is 4 000 IU
Vitamin A[edit | edit source]
- Fat-soluble vitamin
- Three active forms of vitamin A in the body - retinol, retinal, and retinoic acid
- Called the “anti-infective” vitamin and many of the body’s defences against infection depend on adequate supply[1]
- An impaired immune response could be due to the deficiency of vitamin A[31]
- Vitamin A deficiency is strongly involved in measles and diarrhea and measles can become severe in vitamin A-deficient children[32]
- Vitamin A supplementation reduced morbidity and mortality in infectious diseases such as measles, diarrheal disease, measles-related pneumonia, HIV infection and malaria[33]
- Vitamin A supplementation provides some protection against complications of life-threatening infections, such as malaria, lung diseases and HIV[34]
- In animal studies:
- low vitamin A diets compromise the effectiveness of inactivated bovine coronavirus vaccines and render calves more susceptible to infectious disease[35]
- The effect of infection with infectious bronchitis virus (IBV), a kind of coronavirus, was more pronounced in chickens fed a lower vitamin A diet[36]
- Recommended daily allowance 900 (males) and 700 (females) ug retinol activity equivalents
- Tolerable upper limit 3 000 ug/day
B Vitamins[edit | edit source]
- Water-soluble vitamins
- Work as part of coenzymes
- Each B vitamin has special functions
- Vitamin B2
- Vitamin B3
- could enhance the killing of Staphylococcus aureus[39]
- effective in prophylactic and therapeutic settings[39]
- significantly inhibited neutrophil infiltration into the lungs with strong anti-inflammatory effect during ventilator-induced lung injury, it led, however, to the development of significant hypoxemia[40]
- Vitamin B6
- needed in protein metabolism
- Participates in over 100 reactions in body tissues
- Plays an important role in body immune function
- Shortage of B vitamins may weaken host immune response - recommended to supplement to virus-infected patients to enhance their immune system[1]
Vitamin C[edit | edit source]
- Water-soluble vitamin
- Also called ascorbic acid
- Plays a role in the synthesis of collagen in connective tissue
- Acts as an anti-oxidant
- Supports immune function[41]
- May function as a weak anti-histamine agent to provide relief from flu-like symptoms such as sneezing, a runny or stuffy nose, and swollen sinuses[42]
- A significantly lower incidence of pneumonia in vitamin C -supplemented groups, suggests that vitamin C may prevent the susceptibility to lower respiratory tract infections under certain conditions.[43]
- In animal studies:
- Protects against infection caused by coronavirus[44]
- COVID-19 causes lower respiratory tract infection - vitamin C could be an effective choice as part of the treatment plan[1]
- Recommended daily allowance 90mg/day
- Tolerable upper limit 2000mg/day
Zinc[edit | edit source]
- Dietary trace mineral
- Found in different shellfish
- Important for the maintenance and development of immune cells of both the innate and adaptive immune system[45]
- Zinc deficiency results in dysfunction of both humoral and cell-mediated immunity and increases susceptibility to infectious diseases[46]
- Zinc supplementation given to zinc-deficient children could reduce measles-related morbidity and mortality caused by lower respiratory tract infections[47]
- Increasing the concentration of intracellular zinc with zinc-ionophores like pyrithione can efficiently impair the replication of a variety of RNA viruses[48]
- Combination of zinc and pyrithione in at low concentrations inhibits the replication of SARS coronavirus (SARS-CoV)[48]
- Recommended daily allowance 15 mg
- Tolerable upper limit 40 mg
N-acetylcysteine (NAC)[edit | edit source]
- Powerful anti-oxidant[49]
- Scavenges free oxygen radicals
- Acts as a mucolytic agent that mellows tenacious mucous discharge[49]
- Addition of NAC therapy for community-acquired pneumonia reduced TNF - a and increased total antioxidant capacity[49]
- Treatment with NAC may help reduce oxidative and inflammatory damage in pneumonia patients[49]
COVID -19 and Nutrition - Recommendations for Prevention and Immune optimization?[edit | edit source]
Micro-nutrients with the strongest evidence for immune support are:
- Vitamin C
- Vitamin D
- Zinc
Other nutrients that may help include:
- Vitamin A
- Vitamin E
- Selenium
- Omega 3’s
- B vitamins
- Plant Phytonutrients (from plant-based foods) may have antioxidant, anti-inflammatory and anti-viral effects
Chinese medicine and medicinal herbs (evidence still emerging on this)
World Health Organisation: Nutrition Advice during the COVID-19 outbreak[edit | edit source]
Good nutrition and hydration are important. A well-balanced diet keeps you healthy, strengthens the immune system, and reduces the risk of chronic disease and infectious disease. It is recommended that a diet with a variety of fresh food and unprocessed foods is followed daily, to provide the body with the necessary vitamins, minerals, dietary fibre, protein, and antioxidants.[50]
Eat fresh and unprocessed foods every day[edit | edit source]
- Include fruits, vegetables, legumes, nuts and whole grains and foods from animal sources (e.g. meat, fish, etc)
- Daily portion recommendations:
- 2 cups of fruit (4 servings)
- 2.5 cups of vegetables (5 servings)
- 180 g grains
- 160 g meat and beans (red meat 1-2 times/week and poultry or fish 2-3 times/week)
- Snack on raw vegetables and fruit, rather than foods that are high in sugar, fat or salt
- Avoid overcooking vegetables and fruit - to avoid the loss of important vitamins
- If using canned fruit or vegetables - choose wisely, avoid varieties with added salt and sugar
Drink enough water every day[edit | edit source]
- Water is essential
- It transports nutrients and compounds in blood, regulates body temperature, gets rid of waste and lubricates and cushions joints
- Drink 8 - 10 cups of water daily
- Water is the best choice, other drinks can also be consumed such as lemon juice (diluted in water and unsweetened), tea and coffee. Avoid consuming too much caffeine, sweetened fruit juices, fizzy drinks and drinks high in sugar
Eat moderate amounts of fat and oil[edit | edit source]
- Eat unsaturated fats rather than saturated fats
- Choose meat that is low in fat
- Avoid processed meats as it is high in salt and fat
- Avoid industrially produced trans fat - fast food, fried food, etc
Eat less salt and sugar[edit | edit source]
- When cooking and preparing food, limit the amount of salt
- Limit daily salt intake to less than 5g (1 teaspoon)
- Avoid foods high in salt and sugar
- Limit intake of soft drinks and sodas that are high in sugar
- Choose fresh fruits instead of sweet snacks such as cookies, cake and chocolate
Immune Boosting Foods[edit | edit source]
Conclusion[edit | edit source]
A healthy, "whole" food plant-based diet helps:
- to prevent chronic disease (people at higher risk for Covid-19)
- people with chronic pain
- people struggling with obesity
- people with Diabetes
- people with cardiovascular disease
- cognitive dysfunction like anxiety and depression
Resources[edit | edit source]
- Potential Interventions for novel coronavirus in China: A systematic review
- Obesity, respiratory disease and pulmonary infections
- Evidence That Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths
- N-acetylcysteine improves oxidative stress and inflammatory response in patients with community acquired pneumonia: A randomized controlled trial
- Nutrition amid the COVID-19 pandemic: a multi-level framework for action
- "Nutrition for Immunity during COVID-19."Extra Helpings: From the "Food as Medicine" Series[51]
- NNEdPro - Combatting COVID-19: A 10-point summary on diet, nutrition and the role of micronutrients[52]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Zhang L, Liu Y. Potential interventions for novel coronavirus in China: A systematic review. J Med Virol. 2020;92(5):479–490. doi:10.1002/jmv.25707
- ↑ Schoeman D, Fielding BC. Coronavirus envelope protein: current knowledge. Virol J. 2019;16:69 10.1186/s12985-019-1182-0
- ↑ Zhang N, Wang L, Deng X, et al. Recent advances in the detection of respiratory virus infection in humans. J Med Virol. 2020;92(4):408‐417. 10.1002/jmv.25674
- ↑ World Health Organisation. Clinical management of severe acute respiratory infection when novel coronavirus (2019-nCoV) infection is suspected. January 2020. https://www.who.int/docs/default-source/coronaviruse/clinical-management-of-novel-cov.pdf [last accessed 24 April 2020]
- ↑ Hajat C, Stein E. The global burden of multiple chronic conditions: A narrative review. Prev Med Rep. 2018;12:284–293. Published 2018 Oct 19. doi:10.1016/j.pmedr.2018.10.008
- ↑ 6.0 6.1 Wang B, Li R, Lu Z, Huang Y. Does comorbidity increase the risk of patients with COVID-19: evidence from meta-analysis. Aging (Albany NY). 2020; 12:6049-6057. https://doi.org/10.18632/aging.103000
- ↑ Characteristics of SARS-CoV-2 patients dying in Italy. Report based on available data on April 23th , 2020. Available from https://www.epicentro.iss.it/en/coronavirus/bollettino/Report-COVID-2019_23_april_2020.pdf [last accessed 26 April 2020).
- ↑ 8.0 8.1 Nabipour S, Ayu Said M, Hussain Habil M. Burden and nutritional deficiencies in opiate addiction- systematic review article. Iran J Public Health. 2014;43(8):1022–1032.
- ↑ 9.0 9.1 9.2 Bancos S, Bernard MP, Topham DJ, Phipps RP. Ibuprofen and other widely used non-steroidal anti-inflammatory drugs inhibit antibody production in human cells. Cell Immunol. 2009;258(1):18–28. doi:10.1016/j.cellimm.2009.03.007
- ↑ Klekotka RB, Mizgała E, Król W. The etiology of lower respiratory tract infections in people with diabetes. Pneumonol Alergol Pol. 2015;83(5):401-8. doi: 10.5603/PiAP.2015.0065.
- ↑ 11.0 11.1 11.2 11.3 GBD 2017 Diet Collaborators. Health effects of dietary risks in 195 countries, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2019;393(10184):1958–1972. doi:10.1016/S0140-6736(19)30041-8
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6899507/
- ↑ Satia JA. Diet-related disparities: understanding the problem and accelerating solutions. J Am Diet Assoc. 2009;109(4):610–615. doi:10.1016/j.jada.2008.12.019
- ↑ Watters JL, Satia JA, Galanko JA. Associations of psychosocial factors with fruit and vegetable intake among African-Americans. Public Health Nutr. 2007 Jul;10(7):701–11.
- ↑ Satia-Abouta J, Patterson RE, Neuhouser ML, Elder J. Dietary Acculturation: Applications to Nutrition Research and Dietetics. J Am Diet Assoc. 2002;102:1105–1118.
- ↑ US Department of Health and Human Services. Dietary Reference Intakes (DRIs). Available from https://health.gov/our-work/food-nutrition/dietary-reference-intakes-dris [last accessed 26 April 2020]
- ↑ 17.0 17.1 17.2 Institute of Medicine (US) Standing Committee on the Scientific Evaluation of Dietary Reference Intakes and its Panel on Folate, Other B Vitamins, and Choline. Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Biotin, and Choline. Washington (DC): National Academies Press (US); 1998. 1, Introduction to Dietary Reference Intakes. Available from: https://www.ncbi.nlm.nih.gov/books/NBK114332/
- ↑ 18.0 18.1 18.2 18.3 18.4 Baugreet S, Hamill RM, Kerry JP, McCarthy SN. Mitigating nutrition and health deficiencies in older adults: a role for food innovation?. Journal of food science. 2017 Apr;82(4):848-55.
- ↑ World Health Organisation (WHO). Ageing and Health. Available from https://www.who.int/news-room/fact-sheets/detail/ageing-and-health [last accessed 26 April 2020]
- ↑ Christensen K, Doblhammer G, Rau R, Vaupel JW. Ageing populations: the challenges ahead. Lancet. 2009;374(9696):1196–1208. doi:10.1016/S0140-6736(09)61460-4
- ↑ Chernoff R. Protein and older adults. J Am Coll Nutr. 2004 Dec;23(6 Suppl):627S-630S.
- ↑ Deutz NE, Bauer JM, Barazzoni R, et al. Protein intake and exercise for optimal muscle function with aging: recommendations from the ESPEN Expert Group. Clin Nutr. 2014;33(6):929–936. doi:10.1016/j.clnu.2014.04.007
- ↑ Nowson C, O'Connell S. Protein Requirements and Recommendations for Older People: A Review. Nutrients. 2015;7(8):6874–6899. Published 2015 Aug 14. doi:10.3390/nu7085311
- ↑ Traylor DA, Gorissen SH, Phillips SM. Perspective: protein requirements and optimal intakes in aging: are we ready to recommend more than the recommended daily allowance?. Advances in Nutrition. 2018 May 1;9(3):171-82.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5952928/ (accessed 7.12..2021)
- ↑ 25.0 25.1 Lamberg-Allardt C, Brustad M, Meyer HE, Steingrimsdottir L. Vitamin D - a systematic literature review for the 5th edition of the Nordic Nutrition Recommendations. Food Nutr Res. 2013;57:10.3402/fnr.v57i0.22671. Published 2013 Oct 3. doi:10.3402/fnr.v57i0.22671
- ↑ Kaiser M, Bandinelli S, Lunenfeld B. 2010. Frailty and the role of nutrition in older people. A review of the current literature. Acta Biomed 81(Suppl. 1):37–45
- ↑ Tangpricha V, Pearce EN, Chen TC, Holick MF. Vitamin D insufficiency among free‐living healthy young adults. Am J Med. 2002;112:659‐662. 10.1016/s0002-9343(02)01091-4
- ↑ Holick MF. Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers, and cardiovascular disease. Am J Clin Nutr. 2004;80:1678S‐1688S. 10.1093/ajcn/80.6.1678S
- ↑ 29.0 29.1 Martineau AR, Jolliffe DA, Hooper RL, et al. Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ. 2017;356:i6583. Published 2017 Feb 15. doi:10.1136/bmj.i6583
- ↑ Nonnecke BJ, McGill JL, Ridpath JF, Sacco RE, Lippolis JD, Reinhardt TA. Acute phase response elicited by experimental bovine diarrhea virus (BVDV) infection is associated with decreased vitamin D and E status of vitamin‐replete preruminant calves. J Dairy Sci. 2014;97:5566‐5579. 10.3168/jds.2014-8293
- ↑ Guillin OM, Vindry C, Ohlmann T, Chavatte L. Selenium, selenoproteins and viral infection. Nutrients. 2019;11:2101 10.3390/nu11092101
- ↑ Kantoch M, Litwinska B, Szkoda M, Siennicka J. Importance of vitamin A deficiency in pathology and immunology of viral infections. Rocz Panstw Zakl Hig. 2002;53:385‐392
- ↑ . Semba RD. Vitamin A and immunity to viral, bacterial and protozoan infections. Proc Nutr Soc. 1999;58:719‐727. 10.1017/s0029665199000944
- ↑ Villamor E, Mbise R, Spiegelman D, et al. Vitamin A supplements ameliorate the adverse effect of HIV‐1, malaria, and diarrheal infections on child growth. Pediatrics. 2002;109:e6 10.1542/peds.109.1.e6
- ↑ Jee J, Hoet AE, Azevedo MP, et al. Effects of dietary vitamin A content on antibody responses of feedlot calves inoculated intramuscularly with an inactivated bovine coronavirus vaccine. Am J Vet Res. 2013;74:1353‐1362. 10.2460/ajvr.74.10.1353
- ↑ West CE, Sijtsma SR, Kouwenhoven B, Rombout JH, van der Zijpp AJ. Epithelia‐damaging virus infections affect vitamin A status in chickens. J Nutr. 1992;122:333‐339. 10.1093/jn/122.2.333
- ↑ 37.0 37.1 Powers HJ. Riboflavin (vitamin B‐2) and health. Am J Clin Nutr. 2003;77:1352‐1360.10.1093/ajcn/77.6.1352
- ↑ Keil SD, Bowen R, Marschner S. Inactivation of Middle East respiratory syndrome coronavirus (MERS‐CoV) in plasma products using a riboflavin‐based and ultraviolet light‐based photochemical treatment. Transfusion. 2016;56:2948‐2952. 10.1111/trf.13860
- ↑ 39.0 39.1 Kyme P, Thoennissen NH, Tseng CW, et al. C/EBPepsilon mediates nicotinamide‐enhanced clearance of Staphylococcus aureus in mice. J Clin Invest. 2012;122:3316‐3329. 10.1172/JCI62070
- ↑ Jones HD, Yoo J, Crother TR, et al. Nicotinamide exacerbates hypoxemia in ventilator‐induced lung injury independent of neutrophil infiltration. PLOS One. 2015;10:e0123460 10.1371/journal.pone.0123460
- ↑ Hemila H. Vitamin C and SARS coronavirus. J Antimicrob Chemother. 2003;52:1049‐1050. 10.1093/jac/dkh002
- ↑ Field CJ, Johnson IR, Schley PD. Nutrients and their role in host resistance to infection. J Leukoc Biol. 2002;71:16‐32
- ↑ Hemila H. Vitamin C intake and susceptibility to pneumonia. Pediatr Infect Dis J. 1997;16:836‐837. 10.1097/00006454-199709000-00003
- ↑ Atherton JG, Kratzing CC, Fisher A. The effect of ascorbic acid on infection chick‐embryo ciliated tracheal organ cultures by coronavirus. Arch Virol. 1978;56:195‐199. 10.1007/bf01317848
- ↑ Maares M, Haase H. Zinc and immunity: an essential interrelation. Arch Biochem Biophys. 2016;611:58‐65. 10.1016/j.abb.2016.03.022
- ↑ Tuerk MJ, Fazel N. Zinc deficiency. Curr Opin Gastroenterol. 2009;25:136‐143. 10.1097/MOG.0b013e328321b395
- ↑ Awotiwon AA, Oduwole O, Sinha A, Okwundu CI. Zinc supplementation for the treatment of measles in children. Cochrane Database Syst Rev. 2017;2017(6):CD011177 10.1002/14651858.CD011177.pub3
- ↑ 48.0 48.1 te Velthuis AJW, van den Worm SHE, Sims AC, Baric RS, Snijder EJ, van Hemert MJ. Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture. PLOS Pathog. 2010;6:e1001176 10.1371/journal.ppat.1001176
- ↑ 49.0 49.1 49.2 49.3 Zhang Q, Ju Y, Ma Y, Wang T. N-acetylcysteine improves oxidative stress and inflammatory response in patients with community acquired pneumonia: A randomized controlled trial. Medicine (Baltimore). 2018;97(45):e13087. doi:10.1097/MD.0000000000013087
- ↑ World Health Organisation. Nutrition. Nutrition advice for adults during the COVID-19 outbreak. Available from http://www.emro.who.int/nutrition/nutrition-infocus/nutrition-advice-for-adults-during-the-covid-19-outbreak.html [last accessed 26 April 2020]
- ↑ Monash Food as Medicine. "Nutrition for Immunity during COVID-19" Extra Helpings: From the 'Food as Medicine' series. Published on 7 April 2020. Available fromhttps://www.youtube.com/watch?v=9RcnGNHKfSs [last accessed 30 April 2020]
- ↑ Fallon E, McAuliffe S & Ray S. on behalf of the NNEdPro Global Centre for Nutrition and Health (Design by M Abrantes; Reviewed by E Beck, L Buckner, J Bradfield, D Crocombe, M McGirr & K Martin) 26th March 2020. Combatting COVID-19: A 10 point summary on diet, nutrition and the role of micronutrients.