Non-Communicable Diseases
Original Editors - Rachael Lowe
Top Contributors - Admin, Kim Jackson, Tarina van der Stockt, Lucinda hampton, Evan Thomas, Naomi O'Reilly, Tony Lowe, Vidya Acharya, Rucha Gadgil, Robin Tacchetti, 127.0.0.1 and George Prudden
Introduction[edit | edit source]
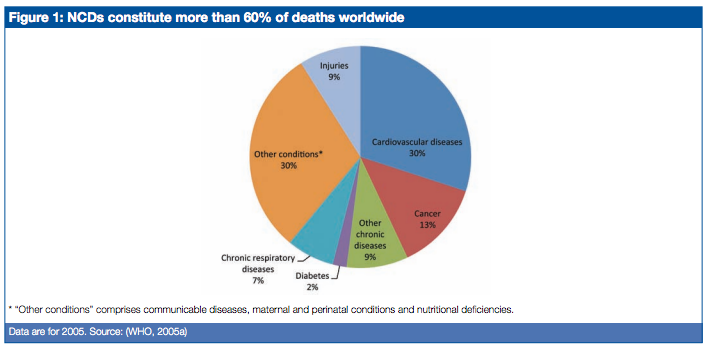
Non-Communicable Diseases (NCDs) are also termed chronic diseases. NCDs are collectively responsible for 71% of all deaths worldwide[1][2]. Almost three quarters of all NCD deaths, and 82% of the 16 million people who died prematurely, or before reaching 70 years of age, occur in low- and middle-income countries.[3][4]. NCDs also account for 48% of the healthy life years lost (Disability Adjusted Life Years–DALYs) worldwide (versus 40% for communicable diseases, maternal and perinatal conditions and nutritional deficiencies, and 1% for injuries).[5]
What are NCDs[edit | edit source]
Non-communicable diseases are a diverse group of chronic diseases that are not communicable, meaning you can't catch them from another person. They are defined as diseases of long duration, generally slow progression and they are the major cause of adult mortality and morbidity worldwide[6]. Non-communicable diseases are identified by WHO as “Group II Diseases,” a category that aggregates (based on ICD-10 code) the following conditions/causes of death: Malignant neoplasms, other neoplasms, diabetes mellitus, endocrine disorders, neuropsychiatric conditions, sense organ diseases, cardiovascular diseases, respiratory diseases (e.g. COPD, asthma, other), digestive diseases, genitourinary diseases, skin diseases, musculoskeletal diseases (e.g. rheumatoid arthritis), congenital anomalies (e.g. cleft palate, down syndrome), and oral conditions (e.g. dental caries). These are distinguished from Group I diseases (communicable, maternal, perinatal and nutritional conditions) and Group III diseases (unintentional and intentional injuries)[5].
Four main diseases are generally considered to be dominant in NCD mortality and morbidity: cardiovascular diseases (including heart disease and stroke), diabetes, cancer and chronic respiratory diseases (including chronic obstructive pulmonary disease and asthma):
In addition to these 4 main diseases, mental disorders are considered to be major contributors to the economic losses stemming from NCDs[5]. Vigo et al[8] describe Five types of mental illness (major depressive disorder, anxiety disorders, schizophrenia, dysthymia, bipolar disorder) that appeared in the top 20 causes of global burden of disease (GBD) in 2013 and argue that the global burden of mental illness is underestimated due to the following five issues:
- The overlap between psychiatric and neurological disorders
- The grouping of suicide and behaviours associated with self-injury as a separate category outside the boundary of mental illness
- The conflation of all chronic pain syndromes with musculoskeletal disorders
- The exclusion of personality disorders in mental illness disease burden calculations
- Inadequate consideration of the contribution of severe mental illness to mortality from associated causes
NCD Risk Factors[edit | edit source]
These disease groups are linked by common risk factors:
- Social Determinants of Health (this is the environment in which we are born, live and grow and the opportunities we are given in those environments)
- Tobacco
- Alcohol
- Poor Nutrition
- Physical Inactivity
Non-modifiable Risk Factors refer to characteristics that cannot be changed by an individual (or the environment) and include age, sex, and genetic make-up. Although they cannot be the primary targets of interventions, they remain important factors since they affect and partly determine the effectiveness of many prevention and treatment approaches.
Modifiable Risk Factors refer to characteristics that societies or individuals can change to improve health outcomes. WHO typically refers to four major ones for NCDs: poor diet, physical inactivity, tobacco use, and harmful alcohol use.
The Global status report on noncommunicable diseases 2010[9] reports that contrary to popular opinion, available data demonstrate that nearly 80% of Non-Communicable Disease (NCD) deaths occur in low and middle-income countries. NCDs are caused, to a large extent, by four behavioural risk factors that are pervasive aspects of economic transition, rapid urbanisation and 21st-century lifestyles: tobacco use, unhealthy diet, insufficient physical activity and the harmful use of alcohol. The greatest effects of these risk factors fall increasingly on low and middle-income countries, and on poorer people within all countries, mirroring the underlying socioeconomic determinants. Among these populations, a vicious cycle may ensue: poverty exposes people to behavioural risk factors for NCDs and, in turn, the resulting NCDs may become an important driver to the downward spiral that leads families towards poverty.
Efforts to Combat NCDs[edit | edit source]
The United Nations (UN) and the World Health Organisation (WHO) have called for a 25% reduction by 2025 in mortality from NCDs, adopting the slogan “25 by 25.” Hunter[10] in his article summarising NCDs argues that in order to reach this goal the following treatments must be addressed:
- Disease Burden
- Economic Effects
- Prevalence of Risk Factors
- Infectious Diseases, Malnutrition, and other diseases of poverty that contribute to NCDs
The Global Status Report on Non-Communicable Disease 2014 is the second in a triennial series tracking worldwide progress in prevention and control of NCDs. The most important message of the second global report on NCDs is that, today, the global community has the chance to change the course of the NCD epidemic.
The Global Action Plan for the Prevention and Control of NCDs 2013-2020 provides a road map and a menu of policy options for all Member States and other stakeholders, to take coordinated and coherent action, at all levels, local to global, to attain the nine voluntary global targets, including that of a 25% relative reduction in premature mortality from cardiovascular diseases, cancer, diabetes or chronic respiratory diseases by 2025. The main focus of this action plan is on the four major NCDs, “Cardiovascular Disease, Cancer, Chronic Respiratory Disease and Diabetes”, but also highlight the four shared behavioural risk factors, “Tobacco Use, Unhealthy Diet, Physical Inactivity and Harmful use of Alcohol”.
Role of Physiotherapy in NCDs[edit | edit source]
Physiotherapists specialise in human movement, physical activity, promoting health, fitness, and wellness. They identify physical impairments, limitations, and disabilities that prevent people from being as active and independent as they might be, and then they find ways of overcoming them. The profession of physiotherapy helps millions of people every year to prevent non-communicable diseases and their risk factors – most importantly obesity. Through targeted rehabilitation methods they also manage the effects of NCDs to optimise health when they are present.
The World Health Organisation points out that physical inactivity is one of the leading risk factors for global mortality, causing 3.2 million deaths annually, and that physical activity can reduce non-communicable diseases, it is clear that the physiotherapy profession has a major part to play.
People with chronic health problems can improve their health by learning how to increase physical activity levels and exercise safely under the guidance and instruction of physiotherapists. The scoping review suggests exercise-based rehabilitation programs can be implemented in low resource settings[11]. Activity has to be introduced carefully if a person is overweight, unfit, older, or has a chronic disease. Physiotherapists do this by examining the person, recommending exercises that are safe and appropriate for them, and educating them about how to look for signs of trouble. This makes them the ideal professionals to prescribe physical activity and exercise programmes for non-communicable diseases.
Physiotherapy doesn’t just mean more healthy people, but more productive people who can contribute to countries’ economies. Their services are provided in an atmosphere of trust and respect for human dignity and underpinned by sound clinical reasoning and scientific evidence.The message is clear: physiotherapists are the movement, physical activity, and exercise experts and a resource in the battle against non-communicable disease that should never be overlooked.
Resources[edit | edit source]
WHO Non-Communicable Disease: Country Profile 2011
The World Economic Forum and the Harvard School of Public Health: The Global Economic Burden of Non-communicable Diseases.
Prevention and control of NCDs: Guidelines for primary health care in low-resource settings
References[edit | edit source]
- ↑ Noncommunicable diseases, WHO, 1 June 2018 [http://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases]
- ↑ Bista B, Dhimal M, Bhattarai S, Neupane T, Xu YY, Pandey AR, Townsend N, Gyanwali P, Jha AK. Prevalence of non-communicable diseases risk factors and their determinants: Results from STEPS survey 2019, Nepal. PloS one. 2021 Jul 30;16(7):e0253605.
- ↑ WHO. Noncommunicable diseases and their risk factors http://www.who.int/ncds/en/ accessed 15 July 2016
- ↑ Dahal S, Sah RB, Niraula SR, Karkee R, Chakravartty A. Prevalence and determinants of non-communicable disease risk factors among adult population of Kathmandu. Plos one. 2021 Sep 8;16(9):e0257037.
- ↑ 5.0 5.1 5.2 Bloom, D.E., Cafiero, E.T., Jané-Llopis, E., Abrahams-Gessel, S., Bloom, L.R., Fathima, S., Feigl, A.B., Gaziano, T., Mowafi, M., Pandya, A., Prettner, K., Rosenberg, L., Seligman, B., Stein, A.Z., & Weinstein, C. (2011). The Global Economic Burden of Noncommunicable Diseases. Geneva: World Economic Forum
- ↑ World Health Organization. (WHO 2005a). Preventing chronic diseases: a vital investment. WHO global report. Geneva: World Health Organization.
- ↑ Budreviciute A, Damiati S, Sabir DK, Onder K, Schuller-Goetzburg P, Plakys G, Katileviciute A, Khoja S, Kodzius R. Management and prevention strategies for non-communicable diseases (NCDs) and their risk factors. Frontiers in public health. 2020:788.
- ↑ Vigo D, Thornicroft G, Atun R. Estimating the true global burden of mental illness. The Lancet Psychiatry. 2016 Feb 29;3(2):171-8.
- ↑ Alwan A. Global status report on noncommunicable diseases 2010. World Health Organization; 2011.
- ↑ Hunter DJ, Reddy KS. Noncommunicable diseases. New England Journal of Medicine. 2013 Oct 3;369(14):1336-43.
- ↑ Heine M, Lupton-Smith A, Pakosh M, Grace SL, Derman W, Hanekom SD. Exercise-based rehabilitation for major non-communicable diseases in low-resource settings: a scoping review. BMJ Global Health. 2019 Nov 1;4(6).