Diabetes and Health-Related Quality of Life
Introduction[edit | edit source]
Improved Quality of life (QOL) has been regarded as a key goal of healthcare interventions for Diabetes (DM) management programs.
DM is a significant and growing healthcare challenge primarily because of increased physical inactivity, consumption of unhealthy diets, obesity and sedentary lifestyles. DM is a major cause of blindness, kidney failure, heart attacks, stroke and lower limb amputation. DM and its complications have contributed tremendously to the burden of mortality and disability worldwide.[1]
Diabetes often leads to the development of physical disabilities that, in turn, can harm a patient's quality of life (QOL). Literature suggests that people with diabetes have lower QOL in general and that depression among people with type 2 diabetes (T2DM) further reduced the QOL.[2] Researches have further established that depression in type I diabetes patient was more than 3 times higher than normal range and 2 times higher in type 2 diabetes patients. [3]
The importance of optimizing health-related QOL (HRQOL) has increasingly been recognized, not only because it represents an important goal for health care on its own but also because of the associations between poor HRQOL and adverse outcomes in people with type 2 diabetes, including poor response to therapy, disease progression, and even mortality.[4]
Global Burden of Type 2 Diabetes[edit | edit source]
T2DM is a global public health crisis that threatens the economies of all nations, particularly developing countries. In 2019, it was estimated that about 85-95% of all people living with diabetes in developing countries suffer from T2DM[5][6]. Diabetes mellitus (DM) and related complications have reached epidemic levels. According to the International Diabetes Federation (IDF) 2021 report:
- 10.5 percent of adults aged 20–79 years (537 million adults) had DM globally in 2021
- Of the above, 90% had type 2 diabetes mellitus (T2DM).
- The prevalence and incidence of DM are increasing worldwide, and a rapid progression has been reported in middle- and low-income countries.[1]
- The IDF predicts a 46 percent increase in the DM population between 2022 and 2045 on a world level. The highest tendency is reported on the African continent, with a 134 percent increase. [7]
- Furthermore, estimates have established that 240 million people are currently living with undiagnosed diabetes worldwide.[7]
Quality of Life[edit | edit source]
Quality of life (QOL) is a multidimensional concept that measures a person’s well-being. As stated by the World Health Organisation (WHO), QOL can be defined as the "individual's perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards and concerns."[8] The discussion and use of QOL as a measurable outcome in health has increased in recent decades as healthcare has shifted from a disease-focused biomedical model to a more holistic, well-being focused biopsychosocial model. QOL has also become more important with improvements in medical treatments and disease management, leading to longer lives for people, particularly those living with chronic diseases. Examples of QOL assessments are the WHOQOL-BREF and WHOQOL-100.
Diabetes and HRQoL[edit | edit source]
T2DM is a complex and serious chronic disease that imposes a significant burden on patients and society in a term of morbidity and premature mortality [10]. In the long term, diabetic patients have to face many complications. HRQoL is an important outcome for persons with T2DM and is used to evaluate the impact of the disease and its treatment on individuals and healthcare costs. The disease itself can have a negative impact on the quality of life.
QoL studies have been recognized as an essential health outcome of all medical interventions and have become a core issue in diabetes care. They provide clinicians with important information to support clinical decision-making, taking both biomedical and psychosocial into consideration.
Persons with T2DM report lower HRQoL than the general population[11]. The leading causes of health-related quality of life (HRQoL) diminution are:
- Diabetes-related complications
- Episodes and fear of hypoglycemia
- Change in lifestyle[12].
Several factors have been identified as predictors of HRQoL and diabetes-related quality of life in T2DM, including the following:
- older age,
- female sex,
- depressive symptoms,
- number of diabetic complications,
- presence of comorbidities, and
- insulin use [13].
Physical Health Domain[edit | edit source]
The physical health domain assesses the impact of the disease on the
- activities of daily living
- dependence on medical substances
- a lack of energy and initiative,
- restricted mobility
- capacity to work[14].
Research findings: Diabetes had a greater impact on the HRQoL of
- Females and older patients (50 years and more)[15]
- Those with a low level of education, sedentary work, and long duration of diabetes [16].
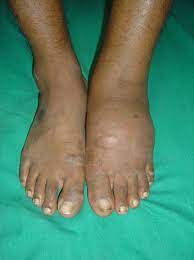
- Foot problems, most frequently reported foot problems were pain and problems due to badly fitting footwear[17]
- Those with peripheral neuropathy also had lower HRQol [18].
Impact on Cognitive Function[edit | edit source]
Both type 1 and type 2 diabetes are associated with mild to moderate decrements in cognitive function.
- T2DM is usually diagnosed at an older age and is commonly associated with obesity, insulin resistance, hypertension and dyslipidemia, all of which can have a negative impact on the brain.
- The underlying mechanism and the risk factors that may lead to the development of more severe cognitive dysfunction like dementia in some but not all people with diabetes are not well understood.
More studies are needed to understand the impact of mild to moderate decrements in cognitive function in the daily lives of people with diabetes.
- Mild to moderate degree of cognitive impairment likely does not cause clinically significant problems in the day-to-day activities of most people with diabetes. However, it may present problems during more stressful and challenging situations.
- People at the extremes of age are more likely to be at increased risk of developing clinically significant decline in cognitive function[19].
Social Health Domain[edit | edit source]
The social domain assesses personal relationships, social support and sexual activity[14].
- Social relationships were one of the main areas affected by people living with T2DM.
People value their relationships with themselves and with others. When an individual is no longer able to physically, emotionally, or sexually relate to self and others, quality of life is often negatively affected[20].
Measurement of HRQoL[edit | edit source]
There are arrays of instruments (outcome measures) to assess HRQoL in type 2 diabetes. These outcome measures can be generic or diabetes-specific. Most of these outcome measures are patient-reported outcomes. Outcome measures that assessed functional status and psychological well-being have been identified in the literature as a sub-set of generic outcome measures in type 2 diabetes[21].
- Generic HRQoL measures: They are generic preference-based measures that provide valuable health status information of patients with diabetes and allow comparisons with the general population and chronic health diseases[21][22][1]. See Table 1 below for examples of generic measures used in type 2 diabetes.
- Psychological HRQoL measures: These assess functional status and psychological well-being (anxiety and depression) of the patient with type 2 diabetes[21]. See the table for types (Table 1).
- Diabetes-specific HRQoL measures: These assess a specific aspect of diabetes, such as the presence of diabetes symptoms, attitudes, worries, self-care, treatment satisfaction, adherence to the diabetic regimen, locus of control, and social and family support[21]. See the Table 1 for types of diabetes-specific measures.
Selecting Appropriate HRQoL Measures[edit | edit source]
Finding ideal tools to measure HRQoL in routine data collection among patients with diabetes could be tasking due to numerous such measures. Selection of suitable outcome measure is based on several factors that had been stated in the literature. However, it has been recommended to use the Appraisal of Diabetes Scale in combination with the SF-12 in clinical settings[23][2]. Also, Audit of Diabetes-Dependent Quality of Life (ADDQoL), Diabetes Care Profile (DCP) and WBQ were promising diabetes-specific tools because of their good internal reliability, external and construct validity[24]. The outcome measures are summarized in the table below.
HRQoL measures used in type 2 diabetic populations[edit | edit source]
|
|---|
Role of Physiotherapy[edit | edit source]
The ultimate aim of diabetes care is to improve the quality of life of the individuals [26]. Physical complications of diabetes can be in the form of muscle weakness, pain, loss of balance and lower limb dysfunction, all of which can ultimately influence the HRQoL of individuals [27]. Physiotherapists play a crucial role in the management of the physical symptoms of diabetes. By incorporating individualized physical activity and patient education in the management of diabetes, complications can be prevented.
Likewise, for individuals with physical complications of diabetes, physiotherapists employ techniques such as:
- Exercise therapy: Exercise therapy through physical activity plays a substantial role in managing diabetes. By developing a structured and individualized regimen, exercise can help improve the strength of weak muscles, gait pattern and balance. Hence, engaging in physical activities positively affects the physical aspect of HRQoL of individuals with diabetes [28].
- Motivation Interviewing: The physiotherapist aims to create long-term changes to the patient's lifestyle with motivational interviewing. More than just exercises, the physiotherapist tries to engage the patient's motivation in the therapeutic process to create a therapeutic alliance and enhance greater daily behaviour changes. [29]
Role of Occupational Therapy[edit | edit source]
The role of occupational therapy in diabetes care is to improve treatment adherence, diabetes self-management abilities, and health-related quality of life.[30] Occupational therapists use activity-based treatments and psychosocial interventions that target multiple levels of influence, such as individual capacity, family, organization, and community. Intervention sessions are held in participants’ homes or community locations. They also use text messaging to provide information and reminders.[31]
Occupational therapists facilitate self-management by making patients responsible for their nutrition, physical activities, insulin therapy, and glucose monitoring and also assist with psychosocial adaptations to chronic illness[30]. The intervention places a strong emphasis on developing habits and routines. Because habits depend on contextual cues, therapists help by assisting patients to modify cues if the original cue does not work (e.g., if setting an alarm does not help in remembering to take medicine, utilizing a visual cue of placing evening medication on the nightstand may help).[31]
Resilient, Empowered, Active Living with Diabetes Program[edit | edit source]
The REAL Diabetes program (Resilient, Empowered, Active Living with Diabetes), an occupational therapy intervention focusing on the lifestyle-related activities, habits, and goals of ethnically diverse young adults with low socioeconomic status having type 1 or type 2 diabetes showed significant improvement in blood glucose control, diabetes-related quality of life, and blood glucose monitoring habits [32][33]. The program [30] provides a set of possible treatment options from which OT can select activities relevant to the patient's needs instead of fixed therapies that the patient needs to complete. The intervention comprises 7 following modules:
- Assessment and goal setting
- Basic self-management knowledge and skills
- Self-advocacy in health care and community settings
- Establishment and maintenance of health-promoting habits and routines
- Seeking and receiving social support
- Enhancing emotional well-being
- Self-reflection and strategies to maintain long-term health.
First, the therapist carries out the initial assessment. Next, the occupational therapist offers personalised interventions based on the information from other modules and the patient's individual goals and personal factors (like readiness to change, personal preferences, and their prescribed diabetes management regimen).[30]Thus, the occupational therapist provides education, support patient in changing their behaviours and habits, plan ADLs in a systematic manner, and develop skills to self-manage diabetes, all of which contribute to improving quality of life.[34] .
Outcome Measures[edit | edit source]
The following tools can be used by occupational therapists in patients with diabetes in order to identify and prioritise activities, coping strategies, and emotional well-being: [35]
- Canadian occupational performance measure (COPM): it helps assess an individual’s perceived occupational performance in self-care, productivity, and leisure.
- Diabetes Empowerment scale (DES) and its short form (DES-SF): measures diabetes-related psychosocial self-efficacy
- World Health Organisation-five well-being index (WHO-5): is a psychometric evaluation of emotional well-being, depression, and quality of life
- Brief COPE: measures strategies for coping with stress-effective approach coping (active coping, acceptance, positive reframing, planning, use of emotional or instrumental support) and ineffective avoidant coping (denial, self-distraction, substance use, behavioural disengagement, venting and self-blame)
Conclusion[edit | edit source]
People with diabetes have a worse quality of life than those without diabetes, specifically in physical functioning and well-being.
Better glucose control generally improves quality of life, and some psychosocial factors (health-related beliefs, social support, coping style, and personality) have a powerful effect on quality of life either directly or through their capacity to buffer the negative effects of diabetes[36]. Also, physiotherapists play a significant role in managing the physical complications of diabetes to improve quality of life.
It is clear that different measures can be utilized to manage the quality of life change because of T2DM, which needs strategic health policy.
References[edit | edit source]
- ↑ 1.0 1.1 Alshayban D, Joseph R. Health-related quality of life among patients with type 2 diabetes mellitus in Eastern Province, Saudi Arabia: a cross-sectional study. PLoS One. 2020 Jan 10;15(1):e0227573. Available:https://journals.plos.org/plosone/article?id=10.1371%2Fjournal.pone.0227573#sec013 (accessed 22.9.2021)
- ↑ Mishra SR, Sharma A, Bhandari PM, Bhochhibhoya S, Thapa K. Depression and health-related quality of life among patients with type 2 diabetes mellitus: a cross-sectional study in Nepal. PloS one. 2015 Nov 23;10(11):e0141385.Available: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0141385#sec014(accessed 22.9.2021)
- ↑ Roy T, Lloyd CE. Epidemiology of depression and diabetes: a systematic review. J Affect Disord. 2012 Oct;142 Suppl:S8-21. doi: 10.1016/S0165-0327(12)70004-6. PMID: 23062861.
- ↑ Landman GW, Van Hateren KJ, Kleefstra N, Groenier KH, Gans RO, Bilo HJ. Health-related quality of life and mortality in a general and elderly population of patients with type 2 diabetes (ZODIAC-18). Diabetes care. 2010 Nov 1;33(11):2378-82. Available:https://care.diabetesjournals.org/content/33/11/2378 (accessed 22.9.2021)
- ↑ Fekadu G, Bula K, Bayisa G, Turi E, Tolossa T, Kasaye HK. Challenges And Factors Associated With Poor Glycemic Control Among Type 2 Diabetes Mellitus Patients At Nekemte Referral Hospital, Western Ethiopia. J Multidiscip Healthc. 2019;12:963-974. Published 2019 Nov 22. doi:10.2147/JMDH.S232691
- ↑ Guariguata L, Whiting D, Weil C, Unwin N. The International Diabetes Federation diabetes atlas methodology for estimating global and national prevalence of diabetes in adults. Diabetes Res Clin Pract. 2011 Dec;94(3):322-32. doi: 10.1016/j.diabres.2011.10.040.
- ↑ 7.0 7.1 Sun, H., Saeedi, P., Karuranga, S., Pinkepank, M., Ogurtsova, K., Duncan, B. B., Stein, C., Basit, A., Chan, J. C., Mbanya, J. C., Pavkov, M. E., Ramachandaran, A., Wild, S. H., James, S., Herman, W. H., Zhang, P., Bommer, C., Kuo, S., Boyko, E. J., & Magliano, D. J. (2022). IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Research and Clinical Practice, 183, 109119. https://doi.org/10.1016/j.diabres.2021.109119
- ↑ Willem Kuyken, John Orley, Mick Power, Helen Herrman, Hilary Schofield, B. Murphy, Željko Metelko, Silvija Szabo, Mirjana Pibernik-Okanović, N. Quemada, A. Caria, S. Rajkumar, S. Kumar, Shekhar Saxena, Dan Bar-On, M. Amir, M. Tazaki, A. Noji, G. Vanheck, . . . G. Burkovsky. (1995). The World Health Organization quality of life assessment (WHOQOL): Position paper from the World Health Organization. Social Science &Amp; Medicine, 41(10), 1403–1409. https://doi.org/10.1016/0277-9536(95)00112-k
- ↑ "Quality of life: What matters to you?"YouTube, uploaded by OECD, 31 May 2016,www.youtube.com/watch?v=yYNjXRVFnTc
- ↑ Roglic G, N Unwin. Mortality Attributable to Diabetes: estimates for the year 2010. Diabetes Res Clin Pract. 2010;87(1):15-9. DOI:10.1016/j.diabres.2009.10.006.
- ↑ Ribu L, Hanestad BR, Moum T, Birkeland K, Rustoen T. A comparison of the health-related quality of life in patients with diabetic foot ulcers, with a diabetes group and a non-diabetes group from the general population. Qual Life Res. 2007; 16:179–189
- ↑ Akinci F, Yildirim A, Gözü H, Sargın H, Orbay E, Sargin M. Assessment of health-related quality of life (HRQoL) of patients with type 2 diabetes in Turkey. Diabetes Research and Clinical Practice. 2008; 79:117–123
- ↑ Wexler DJ, Grant R, Wittenberg E, Bosch JL, Cagliero E, Delahanty L, et al. Correlates of health-related quality of life in type diabetes. Diabetologia. 2006: 49(7):1489–1497
- ↑ 14.0 14.1 Skevington SM. Advancing cross-cultural research on quality of life. Observations are drawn from WHOQOL development. World Health Organisation Quality of Life Assessment. Quality of life Research. 2002; 11(2):135-144.
- ↑ Werfalli M, Kassanjee R, Kalula S, Kowal P, Phaswana-Mafuya N, Levitt NS. Diabetes in South African older adults: prevalence and impact on quality of life and functional disability - as assessed using SAGE Wave 1 data. Glob Health Action. 2018;11(1):1449924. doi:10.1080/16549716.2018.1449924
- ↑ Ronak N, Hussein, Saadia A, Khtheer, Tariq S, AlHadithi.Impact of diabetes on physical and psychological aspects of quality of life of diabetic in Erbil city. Iraq 2010; 4(2):4959.
- ↑ Sundaram M, Kavookjian J, Patrick JH, Miller LA, Madhavan SS, Scott VG. Quality of life, health status and clinical outcomes in Type 2 diabetes patients. Qual Life Res. 2007; 16(2):165–177.
- ↑ Smide B, Lukwale J, Msoka A, Wikblad K. Self-reported health and glycaemic control in Tanzanian and Swedish people with diabetes. Journal of Advanced Nursing. 2002; 37(2):182-191.
- ↑ Moheet A, Mangia S, Seaquist ER. Impact of diabetes on cognitive function and brain structure. Annals of the New York Academy of Sciences. 2015 Sep;1353:60. Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4837888/ (accessed 23.9.2021)
- ↑ Biraguma J. Peripheral neuropathy and quality of life of adults living with HIV/AIDS in Rulindo district in Rwanda: A cross-sectional study [dissertation]. South Africa: University of the Western Cape. 2009
- ↑ 21.0 21.1 21.2 21.3 21.4 Luscombe FA. Health-Related Quality of Life Measurement in Type 2 Diabetes. Value in health. 2000; 3 (Suppl.1): S15-28
- ↑ Mulhern B, Meadows K. The construct validity and responsiveness of the EQ-5D, SF-6D and Diabetes Health Profile-18 in type 2 diabetes. Health and Quality of Life Outcomes 2014, 12:42. DOI:10.1186/1477-7525-12-42.
- ↑ Nair R, Kachan P. Outcome tools for diabetes-specific quality of life. Can Fam Physician. 2017; 63:e310-5
- ↑ Levterova BA, Dimitrova DD, Levterov GE, Dragova EA. Instruments for disease-specific quality-of-life measurement in patients with type 2 diabetes mellitus--a systematic review. Folia Med (Plovdiv). 2013; 55(1):83-92.
- ↑ El Achhab Y, Nejjari C, Chikri M, Lyoussi B. Disease-specific health-related quality of life instruments among adults diabetic: A systematic review. Diabetes Research and Clinical Practice. 2008; 80(2):171–184
- ↑ Jing, X., Chen, J., Dong, Y. et al. Related factors of quality of life of type 2 diabetes patients: a systematic review and meta-analysis. Health Qual Life Outcomes 2018;16, 189 . https://doi.org/10.1186/s12955-018-1021-9
- ↑ Jahantigh Akbari N, Hosseinifar M, Naimi SS, Mikaili S, Rahbar S. The efficacy of physiotherapy interventions in mitigating the symptoms and complications of diabetic peripheral neuropathy: A systematic review. Journal of Diabetes & Metabolic Disorders. 2020;19(2):1995–2004.
- ↑ Kaur, Jaspreet and Singh et al.. Physiotherapy and rehabilitation in the management of Diabetes mellitus: A Review. Indian Journal of Scientific Research.2015,6;171-181. https://www.researchgate.net/publication/303182927_Physiotherapy_and_rehabilitation_in_the_management_of_Diabetes_mellitus_A_Review
- ↑ Grant P. Motivational interviewing in diabetes care, By MP Steinberg and WR Miller: New York, NY: Guilford Press, 2015. Clin Med (Lond). 2016 Apr;16(2):205. doi: 10.7861/clinmedicine.16-2-205. PMCID: PMC4952982.
- ↑ 30.0 30.1 30.2 30.3 Shen X, Shen X. The role of occupational therapy in secondary prevention of diabetes. International Journal of Endocrinology. 2019 Jul 24;2019.
- ↑ 31.0 31.1 Pyatak EA, Carandang K, Vigen C, Blanchard J, Sequeira PA, Wood JR, Spruijt-Metz D, Whittemore R, Peters AL. Resilient, Empowered, Active Living with Diabetes (REAL Diabetes) study: Methodology and baseline characteristics of a randomized controlled trial evaluating an occupation-based diabetes management intervention for young adults. Contemporary clinical trials. 2017 Mar 1;54:8-17.
- ↑ Pyatak, E.A., Carandang, K., Vigen, C.L., Blanchard, J., Diaz, J., Concha-Chavez, A., Sequeira, P.A., Wood, J.R., Whittemore, R., Spruijt-Metz, D. and Peters, A.L., 2018. Occupational therapy intervention improves glycemic control and quality of life among young adults with diabetes: The Resilient, Empowered, Active Living with Diabetes (REAL Diabetes) randomized controlled trial. Diabetes care, 41(4), pp.696-704.
- ↑ Pyatak EA, Carandang K, Vigen C, Blanchard J, Sequeira PA, Wood JR, Spruijt-Metz D, Whittemore R, Peters AL. Resilient, Empowered, Active Living with Diabetes (REAL Diabetes) study: Methodology and baseline characteristics of a randomized controlled trial evaluating an occupation-based diabetes management intervention for young adults. Contemp Clin Trials. 2017 Mar;54:8-17.
- ↑ Christopherson K, Janssen M, Merchlewicz N. Occupational Therapy Interventions for People with Type 2 Diabetes in Rural Communities.
- ↑ Bahadır Ağce Z, Ekici G. Person-centred, occupation-based intervention program supported with problem-solving therapy for type 2 diabetes: a randomized controlled trial. Health and Quality of Life Outcomes. 2020 Dec;18(1):1-4.
- ↑ Rubin RR, Peyrot M. Quality of life and diabetes. Diabetes Metab Res Rev. 1999;15(3):205-218.