Chronic Leg Ulcers
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Aminat Abolade
Introduction[edit | edit source]
Chronic leg ulcer is defined as a defect in the skin below the level of knee persisting for more than six weeks and shows no tendency to heal after three or more months. Chronic ulceration of the lower legs is a relatively common condition amongst adults, one that causes pain and social distress.
The condition affects 1% of the adult population and 3.6% of people older than 65 years.
- Leg ulcers are debilitating and greatly reduce patients' quality of life. The common causes are venous disease, arterial disease, and neuropathy. Less common causes are metabolic disorders, hematological disorders, and infective diseases.
- As many factors lead to chronic lower leg ulceration, an interdisciplinary approach to the systematic assessment of the patient is required, in order to ascertain the pathogenesis, definitive diagnosis, and optimal treatment.
- The researchers are inventing newer modalities of treatments for patients with chronic leg ulceration, so that they can have better quality life and reduction in personal financial burden.[1]
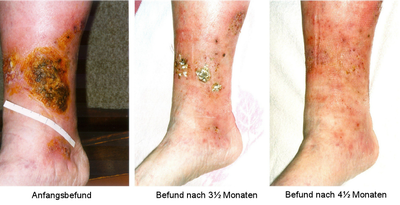
Image1: Example of the healing process of a chronic venous stasis ulcer of the lower leg under therapy with wIRA.
Aetiopathogenesis[edit | edit source]
It has been reported that ulcers related to venous insufficiency constitute 70%, arterial disease 10%, and ulcers of mixed etiology 15% of leg ulcer presentations. The remaining 5% of leg ulcers result from less common pathophysiological causes (this latter group comprise considerable challenges in diagnosis, assessment, and management).[1]
- It is estimated 1% of adults, 3.6% of individuals over age 65, and 5% of those over 80 to have a chronic lower leg ulcer. These numbers are anticipated to increase as the current population ages.
- Risk Factors include: Age, Diabetes, stroke, peripheral vascular and other cardiovascular diseases, cognitive issues, poor nutritional status, socioeconomic complications and neurological disorders.
- Aging: Physiologic changes of aging skin contributes to seniors being at higher risk for chronic lower leg wounds eg decreased vascular and skin nerve supply, tissue thinning, and collagen reduction can impair wound healing in the elderly.[2]
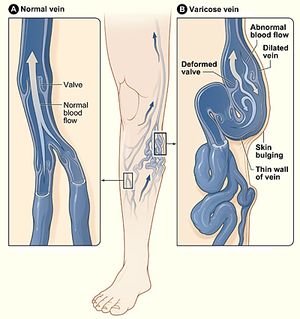
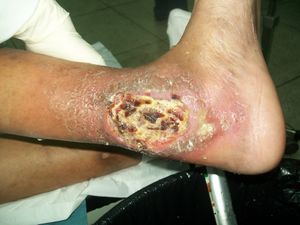
- Venous ulcers are usually located in the gaiter area between the ankle and the calf, often on the medial aspect of the leg. Venous ulcers arise from venous valve incompetence. Venous ulceration is a chronic disease, which is characterized by periods of exacerbation and remission. Venous ulcers often take a long time to heal, which results in physical and psychological discomfort and negatively affects a patient’s functional status.
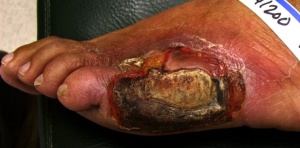
- Arterial leg ulcers occur as a result of reduced arterial blood flow and subsequent tissue perfusion. Peripheral Arterial disease due to atherosclerosis, diabetes with microvascular or macrovascular disease, and/or vasculitis could lead to ischemic leg resulting in ulceration. Arterial ulceration typically occurs over the toes, heels, and bony prominences of the foot. The ulcer appears “punched out” with well-demarcated edges and a pale, nongranulating, and necrotic base.
- Diabetic foot ulcers are common and estimated to affect 15% of all diabetic individuals during their lifetime.
- Pressure ulcers usually occur over bony prominences eg the heel but can occur on any part of the body subjected to pressure. Approximately 70% of all pressure ulcers occur in the geriatric population. Pressure ulcers can be a major source of infection and lead to complications such as septicemia, osteomyelitis, and even death.
Management of Chronic Leg Ulcers[edit | edit source]
An ideal management plan for patients with chronic leg ulcers should involve an early strategic and coordinated approach to delivering the correct treatment option for each individual patient, based on accurate assessment of the underlying pathophysiology.
The management of leg ulcers should include a detailed wound assessment, investigations, wound debridement, and treatment. Successful management of leg ulcers requires a clear diagnosis, establishment of a treatment plan, accurate monitoring, and adherence to the plan as the ulcer decreases in size. Education and training is vital for all those involved in caring for patients with chronic ulceration[1].
- If ulcer is infected it will be treated with antibiotics to avoid further complications.
- Compression bandages are also used to help ease swelling, close the wound, and prevent infection.
- Specific ointments may be to applied to the ulcer.
- In severe cases orthotics or braces to improve gait pattern and prevent future ulcers.
- Pentoxifylline (prescription drug used to improve the symptoms of intermittent claudication due to occlusive artery disease) may be prescribed.
- Aspirin to prevent blood clots in the legs may also be prescribed[3].
Physiotherapy[edit | edit source]
Physiotherapists are important members of wound care teams. We have extensive knowledge of anatomy, physiology, electrophysical agents, and biomechanics to optimize functional strength, balance, and mobility. We can use this knowledge to provide a holistic approach to our senior populations with chronic lower leg wounds. Physical activity has also shown favourable impacts on psychosocial issues such as self-esteem, depression, anxiety, and stress.
The calf muscle pump is the primary mechanism to return blood to the heart from the lower extremities. When impaired, venous hypertension results from blood pooling in the lower extremities.
- Over 70% of individuals presenting with a venous leg ulcer have an impaired calf muscle pump.
- Providing resistive calf muscle strengthening exercises (eg heal lifts, resistive dorsiflexion/plantar flexion exercises, walking with adequate ankle range) and/or improving ankle range of motion, have been shown in the literature to enhance lower extremity hemodynamics and positive trends towards venous leg ulcer healing.[2]
Exercise is recommended as an adjuvant treatment for venous leg ulceration (VLU) to improve calf muscle pump function.
- Prescribing exercise for treating VLU may have an added beneficial effect when used in addition to compression and it appears that the combination of progressive resistance exercises and aerobic activity may be the most effective form of exercise regimen.
- The evidence may now be sufficient to suggest clinicians and suitable patients could consider simple progressive resistance exercises eg heel raises, and 30 minutes walking at least 3 times per week.
- Adherence to such a regimen suggests that for every 4 patients treated with prescribed exercise plus compression, 1 more patient might heal than if using compression alone[4].
Education, including eg
- Important to keep any wounds clean to prevent infection. Wash the wound with mild soap and water daily. Also, change any bandages and dressings at least once daily to keep the area dry, so it can heal (follow specific routine doctor gives).
- Wear good walking shoes
- Get regular, mild to moderate exercise with compression bandages covering ulcer
- Elevating your legs during rest periods
- Never use home or alternative methods in lieu of traditional medical treatment without checking with your doctor. These remedies may very well be beneficial, but they can also aggravate the condition depending on the preparation and stage of your ulcers[3].
Other treatments to support clients with chronic lower leg ulcers include: Gait training with or without aids; transfer techniques; mobility; pressure redistribution; electrophysical agents; muscle strengthening; balance training.[2]
Wound management products[edit | edit source]
Passive dressings:
- Use the ‘passive’ or the ‘plug and conceal’ concept, including gauze, lint, non-stick dressings and tulle dressings. These products fulfill very few of the properties of an ideal dressing and have very limited, if any, use as primary dressing, but some are useful as secondary dressings.
Interactive dressings:
- These dressings help to control the micro-environment by combining with the exudate to form either a hydrophilic gel or, by means of semipermeable membranes, controlling the flow of exudate from the wound into the dressing. They may also stimulate activity in the healing cascade and speed up the healing process.
- There are six classes of interactive dressings, classified according to their functionality (The choice of dressing will depend on the wound type and depth, level of exudate and the presence of bacteria):
- Film dressings: consist of a thin, poly-urethane membrane coated with a layer of acrylic adhesive
- Hydroactive dressings: multi-layered highly absorbent polymer dressings with a surface adhesive and a waterproof outer layer are similar to hydrocolloids, however, instead of forming a gel in contact with exudate, the fluid is trapped within the product itself, to maintain a moist environment.
- Hydrocolloid dressings: combination of polymers held in a fine suspension. When placed on a wound, the polymers combine with the exudate and form a soft, moist gel-like mass. They also encourage autolysis to aid in the removal of slough from a wound.
- Hydrofibre dressings: have some of the properties of alginates in that they are a fibre rope or dressing that forms a firm gel in contact with fluid.
- Foam dressings: soft, open-celled hydrophobic/hydrophilic non-adherent dressings that may be single or multiple layered and meet many of the properties of an ideal dressing
- Alginate absorbent fibre dressings: Alginates are the calcium or sodium/calcium salts of alginic acid, composed of manuronic and guluronic acids obtained from seaweed. When applied to a wound, the sodium salts present in the wound exchanges with the calcium in the alginate to form sodium alginate which is a hydrophilic gel. This gel has the ability to absorb exudate into itself while maintaining a moist environment at the interface between the dressing and the tissue[5].
Bandages
- Used from ancient times. In the past 15 years there has been an explosion in the types of bandages available. The bandage may be needed for several reasons:
- Retention: keeping a dressing in place
- Musculoskeletal support: supporting an injured joint
- Compression: assisting venous return from the lower leg.[6]
Recent Advances in Management[edit | edit source]
Several researchers are still discovering other modalities of treatment. Including:
- The discovery of miRNAs (microRNAs) has opened up vast therapeutic opportunities. miRNAs are small noncoding RNA molecules which play pivotal roles in wound healing. These small regulatory RNAs, have the ability to regulate gene expression. miRNAs can inhibit gene expression by halting translation, by binding to a specific location on messengerRNA, preventing the molecule from being translated. The knowledge of miRNA function in the regulation of wound healing and developing improved miRNA modulation techniques in the skin will help in translating this knowledge into more effective therapies.[7]
- Chronic wounds are characterized by changes in cell receptors (integrins). The activation or inhibition of integrin receptors by various agents may provide an excellent means of influencing wound healing.
- Venous leg ulcers can be healed with a spray formulation of allogeneic neonatal keratinocytes and fibroblasts without the need for tissue engineering, at an optimum dose of cells per mL every 14 days[1]
Image: A computational model of Double-stranded RNA.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Agale SV. Chronic leg ulcers: epidemiology, aetiopathogenesis, and management. Ulcers. 2013 Apr 22;2013.Available from: https://www.hindawi.com/journals/ulcers/2013/413604/ (accessed 12.3.2021)
- ↑ 2.0 2.1 2.2 CPA Leg Ulcers Available from: https://physiotherapy.ca/impact-chronic-lower-leg-ulcers-within-senior-population-and-role-exercise-fall-2014(accessed 12.3.2021)
- ↑ 3.0 3.1 Health Line Leg Ulcers Available from: https://www.healthline.com/health/leg-ulcers#home-remedies(accessed 12.3.2021)
- ↑ Jull A, Slark J, Parsons J. Prescribed exercise with compression vs compression alone in treating patients with venous leg ulcers: a systematic review and meta-analysis. JAMA dermatology. 2018 Nov 1;154(11):1304-11.Available from:https://jamanetwork.com/journals/jamadermatology/fullarticle/2705273 (accessed 12.3.2021)
- ↑ DVA gov au Wound care module Available from:https://www.dva.gov.au/sites/default/files/files/providers/woundcare/dressband.pdf (last accessed 12.3.2021)
- ↑ RACGP Ulcer Management Available from:https://www.racgp.org.au/afp/2014/september/ulcer-dressings-and-management/ (accessed 12.3.2021)
- ↑ Banerjee J, Sen CK. microRNA and wound healing. InmicroRNA: Medical Evidence 2015 (pp. 291-305). Springer, Cham.Available from:https://pubmed.ncbi.nlm.nih.gov/26663189/ (accessed 13.3.2021)