Anatomy of the Human Heart
Original Editor - Uchechukwu Chukwuemeka
Top Contributors - Uchechukwu Chukwuemeka, Lucinda hampton, Kim Jackson, George Prudden, Joao Costa, Sai Kripa, Admin and Adam Vallely Farrell
Introduction[edit | edit source]
The heart is a muscular organ that serves to collect deoxygenated blood from all parts of the body, carries it to the lungs to be oxygenated and release carbon dioxide. Then, it transports the oxygenated blood from the lungs and distributes it to all the body parts[1]
- The heart pumps around 7,200 litres of blood in a day throughout the body[2].
- The heart is situated at the centre of the chest and points slightly towards the left.
- On average, the heart beats about 100,000 times a day, i.e., around 3 billion beats in a lifetime.
- An adult heart beats about 60 to 80 times per minute, and newborn babies heart beats faster than an adult which is about 70 to 190 beats per minute.
Anatomy[edit | edit source]
The heart is a conical hollow muscular organ situated in the middle mediastinum and is enclosed within the pericardium. It is positioned posteriorly to the body of the sternum with one-third situated on the right and two-thirds on the left of the midline. The heart measures 12 x 8.5 x 6 cm and weighs ~310 g (males) and ~255 g (females). It pumps blood to various parts of the body to meet their nutritive requirements. The Greek name for the heart is cardia from which we have the adjective cardia. [3]
Relations
- Anteriorly: the body of the sternum, and adjoining costal cartilages; left lung, and pleura (apex)
- Posteriorly: oesophagus, descending thoracic aorta, azygos, hemiazygos veins, and thoracic duct
- Superficially : bifurcation of the main pulmonary trunk
- Inferiorly: diaphragm
- Laterally: lungs, pleura[4]
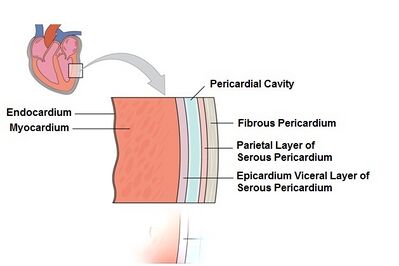
Layers of the Heart Walls[edit | edit source]
The heart wall consists of three layers enclosed in the pericardium[1][5][6]:
- Epicardium - the outer layer of the wall of the heart and is formed by the visceral layer of the serous pericardium.
- Myocardium - the muscular middle layer of the wall of the heart and has excitable tissue and the conducting system.
- Endocardium .[4]
- A middle concentric layer
- A subendocardial layer.
The rest of the heart is composed mainly of the subepicardial and subendocardial layers.
Structure and Function[edit | edit source]
The heart is subdivided by septa into right and left halves, and a constriction subdivides each half of the organ into two cavities, the upper cavity being called the atrium, the lower the ventricle. The heart, therefore, consists of four chambers:
- right atrium
- left atrium
- right ventricle
- left ventricle[4].
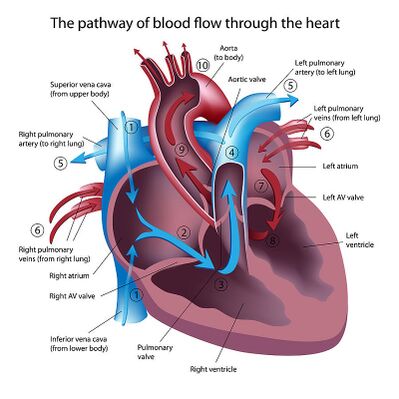
It is best to remember the four chambers and four valves in order of the series that blood travels through the heart:
- Venous blood returning from the body drains into the right atrium via the SVC, IVC and coronary sinus
- The right atrium pumps blood through the tricuspid valve into the right ventricle
- The right ventricle pumps blood through the pulmonary semilunar valve into the pulmonary trunk to be oxygenated in the lungs
- Blood returning from the lungs drains into the left atrium via the four pulmonary veins
- The left atrium pumps blood through the bicuspid (mitral) valve into the left ventricle
- The left ventricle pumps blood through the aortic semilunar valve into the ascending aorta to supply the body.[4]
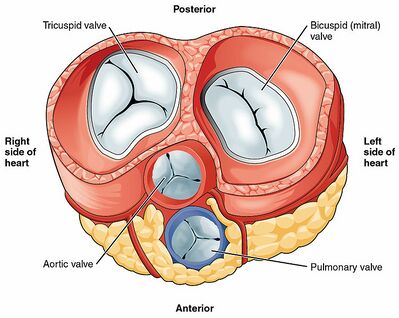
Heart Valves[edit | edit source]
The valves of the heart maintain unidirectional flow of the blood and prevent its regurgitation in the opposite direction. There are two pairs of valves in the heart, a pair of atrioventricular valves and a pair of semilunar valves. Apart, it has four valves. All four valves of the heart have a singular purpose: allowing forward flow of blood but preventing backward flow.[7] The outflow of each chamber is guarded by a heart valve:
Atrioventricular valves between the atria and ventricles
- tricuspid valve (R side of the heart)
- mitral valve/bicuspid valve (left side of the heart)
Semilunar valves which are located in the outflow tracts of the ventricles
- aortic valve (L side heart)
- pulmonary valve (R side heart)[4]
See also Cardiac Valve Defects
Blood Supply[edit | edit source]
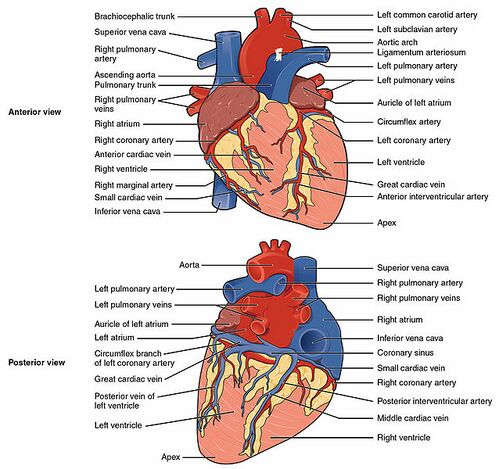
The heart is supplied by two coronary arteries:
- Left main coronary artery carries 80% of the flow to the heart muscle. It is a short artery that divides into two branches
- Left anterior descending artery that supplies anterior two-thirds of the inter-ventricular septum and adjoining part of the left ventricular anterior wall
- Circumflex coronary artery that supplies blood to the lateral and posterior portions of the left ventricle.
2. Right coronary artery: branches supply the right ventricle, right atrium, and left ventricle's inferior wall.
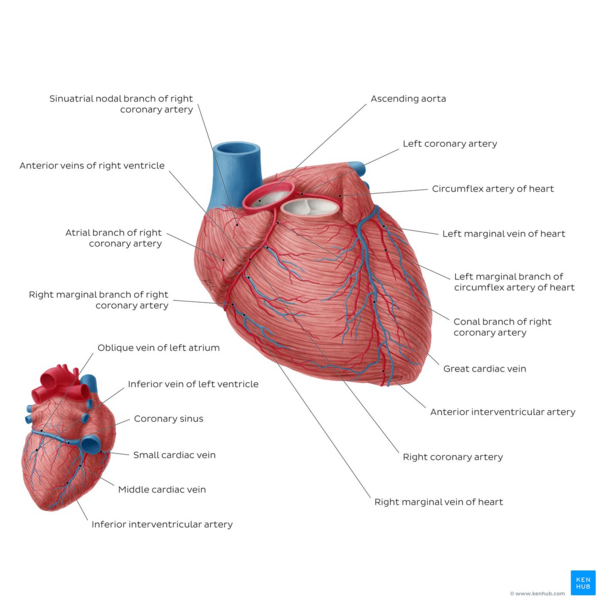
Coronary arteries and veins course over the surface of the heart. Most coronary veins coalesce into the coronary sinus that runs in the left posterior atrioventricular groove and opens into the right atrium. Other small veins, called thebesian veins, open directly into all four chambers of the heart.[7]
Image: Overview of the coronary arteries and cardiac veins - anterior and posterior views[8]
See also Coronary Artery Disease
Venous drainage and Lymphatics[edit | edit source]
Venous drainage is via the variable coronary veins and the coronary sinus[4].
The lymphatic vessels drain mainly into:
- Brachiocephalic nodes, in front of brachiocephalic veins
- Tracheobronchial nodes, located at the distal end of the trachea[9].[6]
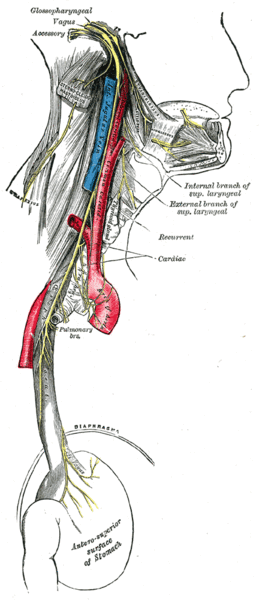
Nerve Supply[edit | edit source]
The main control of the heart resides with the medulla oblongata. There is an area called the cardioacceleratory centre, or pressor centre, in the upper part of the medulla oblongata, and an area called the cardioinhibitory centre, or depressor centre, in the lower part. Together they are called the cardioregulatory centre, since they interact to control heart rate, etc.
The nervous supply to the heart is autonomic, consisting of both sympathetic and parasympathetic parts. The sympathetic fibres arise from the pressor centre, while the parasympathetic fibres arise in the depressor centre. See also Vagal Tone
- The sympathetic nervous system acts on the sinoatrial node, speeding up the depolarisation rate, and therefore increasing the heart rate.
- The parasympathetic system works in reverse in order to slow the heart rate down.
- The heart itself has a natural pacemaker, the sinoatrial node, which does not need a nervous supply to function. If you sever all the nerves to the heart, then it will continue to beat. In fact, it will beat faster than normal, since there is normally a parasympathetic supply slowing the heart down.[10]
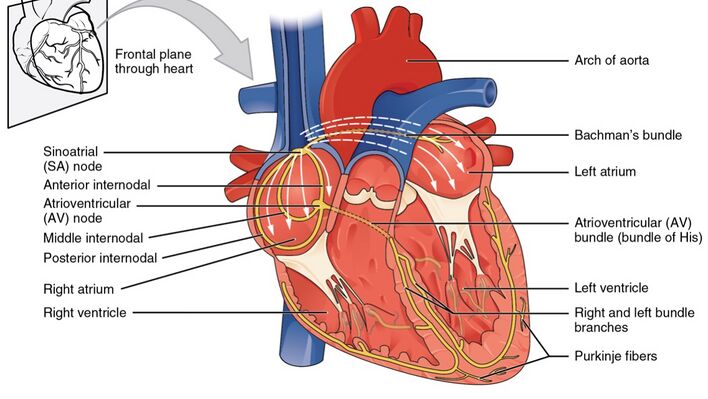
Heart Conduction System[edit | edit source]
An electrical conduction system regulates the pumping of the heart and timing of contraction of various chambers. Heart muscle contracts in response to the electrical stimulus received system generates electrical impulses and conducts them throughout the muscle of the heart, stimulating the heart to contract and pump blood. Among the major elements in the cardiac conduction system are the sinus node, atrioventricular node, and the autonomic nervous system.
- The sinus node is the heart's natural pacemaker. The sinus node is a cluster of cells situated in the upper part of the wall of the right atrium. The electrical impulses are generated there. (The sinus node is also called the sinoatrial node.)
- The electrical signal generated by the sinus node moves from cell to cell down through the heart until it reaches the atrioventricular node (the AV node), a cluster of cells situated in the center of the heart between the atria and ventricles.
- The AV node serves as a gate that slows the electrical current before the signal is permitted to pass down through to the ventricles. This delay ensures that the atria have a chance to fully contract before the ventricles are stimulated. After passing the AV node, the electrical current travels to the ventricles along special fibers embedded in the walls of the lower part of the heart.
- The autonomic nervous system (the same part of the nervous system as controls the blood pressure) controls the firing of the sinus node to trigger the start of the cardiac cycle. The autonomic nervous system can transmit a message quickly to the sinus node so it in turn can increase the heart rate to twice normal within only 3 to 5 seconds. This quick response is important during exercise when the heart has to increase its beating speed to keep up with the body's increased demand for oxygen.[11]
Relevance to Physiotherapy[edit | edit source]
- Education- Educating your clients re heart health, both for those with a heart condition and those without. Inform them of the hearts health importance, because it pumps blood and oxygen to all of your organs. When the heart doesn’t get the care it needs, serious problems can develop in the lining of the arteries, which then lead to plaque formation which leads to Heart Disease. General advice includes
- A heart healthy diet is a pattern of food you eat over days, weeks and months.
- Regular physical activity reduces your risk of having a heart attack or developing heart disease.
- Quitting smoking decreases your risk of heart attack and stroke almost straight away.
- Understanding and controlling cholesterol and blood pressure is key to your heart health. [12]
2. See our many pages on heart related health issues eg Cardiac Rehabilitation; Myocardial Infarction; Atrial Fibrillation; Acute Coronary Syndrome; Physical Activity and Cardiovascular Disease.
Videos[edit | edit source]
This 10 minute video is a good summary of the heart.[13]
References[edit | edit source]
- ↑ 1.0 1.1 Kenny, WL,Wilmore, JH, Costill, DL. Cardiovascular System and its Control. In Physiology of Sport and Exercise, 5rdedn. Human Kinetics, 2011. 140-150.
- ↑ Inovqheart Heart Available from: https://www.inovaheart.org/upload/docs/Healthcare%20Services/Heart%20and%20Vascular/fast-facts-about-the-heart.pdf
- ↑ Chaurasia BD. Human Anatomy Regional and Applied Dissection and Clinical. Vol 1. CBS Publishers and Distributors Pvt Ltd, 2010
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Radiopedia Heart Available: https://radiopaedia.org/articles/heart?lang=gb (accessed 17.6.2021)
- ↑ Malouf, JF, Edwards, WD, Tajil, AJ, Seward, JB. Functional anatomy of the heart. In: Fuster, F, Alexander, RW, O’Rourke, RA editors. Hurst’s: The Heart. 10th edn. McGraw-Hill Inc., 2001. p19–62.
- ↑ 6.0 6.1 Drake, RL, Vogl, W, Mitchell, AW, Gray, H. Gray's anatomy for Students 2nd ed. Philadelphia : Churchill Livingstone/Elsevier, 2010.
- ↑ 7.0 7.1 Rehman I, Rehman A. Anatomy, Thorax, Heart. [Updated 2020 Dec 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan Available:https://www.ncbi.nlm.nih.gov/books/NBK470256/ (accessed 17.6.2021)
- ↑ Overview of the coronary arteries and cardiac veins - anterior and posterior views image - © Kenhub https://www.kenhub.com/en/library/anatomy/heart
- ↑ Moore, KL, Dalley, AF. Clinically oriented anatomy. 6th ed. Philadelphia: Lippincott Williams & Wilkins. 2009
- ↑ Basic heart Anatomy Nervous Supply Heart Available: https://www.liverpool.ac.uk/~trh/local_html/heartdisease/nerve_supply_to_the_heart.htm (accessed18.7.2021)
- ↑ Medicine net Conduction system heart Available:https://www.medicinenet.com/heart_conduction_system/definition.htm (accessed 18.7.2021)
- ↑ Hear Foundation Heart Health Education Available:https://www.heartfoundation.org.au/heart-health-education/keeping-your-heart-healthy (accessed 18.7.2021)
- ↑ Anatomy of the heart video - © Kenhub https://www.kenhub.com/en/library/anatomy/heart