Cardiac Valve Defects
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Aminat Abolade
Introduction[edit | edit source]
Key Facts
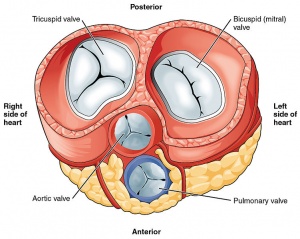
- Heart valves control blood flow to, from and within the heart.
- Damage to heart valves impairs the heart’s function.
- Heart valve disease is damage to the heart’s valve/s.
- Heart valve disease can be a treatable condition through medication or surgery[1]
Heart valve disease accounts for up to a third of heart diseases and is very common within the ageing population. When symptomatic, valve disease can have a significant negative effect on the patient’s ability to carry out daily physical activities and is also significantly associated with an increased risk of mortality and morbidity[2](see also Cardiac Depression Scale)
Types Of Valve Disease[edit | edit source]
There are a few types of heart valve disease. Some people may have a combination of more than one type of valve problem.
- Stenosis: valve doesn't work properly because the valve flaps are thick or stiff. This can reduce blood flow straining heart. Eg:
- One of the most common valve anomalies is aortic stenosis (AS), which is mainly caused by congenital defects, calcification on the valve, or Rheumatic valve disease. With aortic stenosis, the valve does not open fully, and thus, the heart must work harder to eject blood through the ventricle. As the heart continues to increase its workload to overcome the stenotic valve, the left ventricle can hypertrophy and subsequently develop pathologies such as heart failure[3].
2. Regurgitation (or insufficiency): valve flaps are ‘leaky’ and don't close properly. This lets blood leak back through the valve and makes the heart work harder to circulate blood around your body. Eg:
- Aortic regurgitation (AR). The common causes of AR are endocarditis, aortic dissection, and aortic leaflet rupture. In AR, the valves fail to shut completely thus allowing backflow of blood at the end of systole. This backflow decreases the total ejection fraction and creates a volume-overload state that will lead to an increased workload by the left ventricle and eventual left ventricular hypertrophy[3]
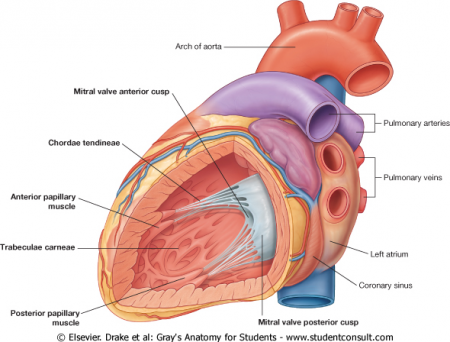
- Mitral valve prolapse (MVP). The most common causes of MVP include idiopathic degeneration of the valve, connective tissue disorders such as Marfan syndrome, and genetic causes. The pathophysiology of MVP involves inadequate positioning of the valve leaflets which create an overlapping, unsupported valve that loses its tension. This pathology causes the valve to prolapse out into the left atrium during systole, creating an opening that can cause regurgitation of blood into the left atrium.
3. Atresia: condition in which the valve isn't formed correctly, and tissue blocks the blood flow between the heart chambers. Eg:
- Aortic valvular atresia is a congenital condition in which the aortic valvular cusps are fused at birth. It frequently forms as a spectrum of malformations of the left ventricular outflow tract (LVOT). Most commonly, the defect presents as aortic stenosis, though in rare cases, it can manifest as complete atresia. When atretic, the valve can be dome-shaped, monocuspid, bicuspid, or even quadricuspid, and the associated leaflets are dysplastic or fused, not permitting flow through the abnormal valve[4].
Signs and Symptoms[edit | edit source]
Heart valve disease symptoms can be mild, moderate, or severe.
The signs and symptoms of heart valve disease include:
- Abnormal sound when listening with stethoscope (heart murmur)
- Chest pain
- Fainting, dizziness or light-headedness
- Irregular heartbeat
- Palpitations
- Shortness of breath
- Swelling of ankles and feet
- Tiredness
One of the first signs of heart valve disease is often a heart murmur. The murmur is heard when blood flows through a heart valve that doesn’t open or close properly (some people with a normal heart can have a murmur)[1].
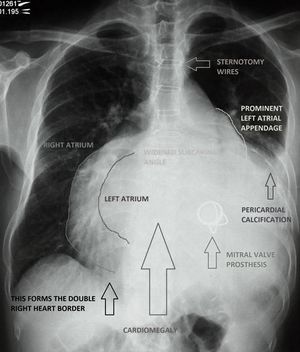
Image 3: Xray: Cardiomegaly; Pericardial calcification; Median sternotomy; Mitral valve replacement.
Causes[edit | edit source]
It's not always possible to tell what causes heart valve disease. Some heart valve disease patients have abnormalities present from birth (congenital heart disease), others have disease that’s related to age, or is caused by another condition.
Heart valve disease caused by congenital heart disease may be due to:
- Bicuspid aortic valve
- Ebstein’s anomaly
- Pulmonary valve stenosis
Heart valve disease caused by damage to the heart valves may be due to:
- Heart failure or cardiomyopathy
- Damage to the heart muscle from a heart attack
- Heart valve infection (endocarditis)
- Scarring from rheumatic fever (rheumatic heart disease)
Heart valve disease caused by aging may be due to:
- Degenerative valve disease eg mitral valve prolapse, a condition that affects nearly 2% of Australians, may result in mitral valve regurgitation that needs treatment.
- Calcification due to ageing (calcium can accumulate on the heart's valves and lead to aortic stenosis).
- Mediastinal radiation therapy ie radiation to the chest, survivors of childhood cancer who had radiation therapy have an increased rate of heart valve disease later in life[1].
Although heart valve problems can potentially be severe and even life-threatening, these conditions can also be treatable.
Diagnosis[edit | edit source]
- Electrocardiogram (ECG)
- Echocardiogram (shows how the heart valves and chambers are functioning).
- Chest X-ray (show whether the heart is enlarged).
- Chest CT scan (shows the size and shape of your aorta)[1]
Treatment[edit | edit source]
Treatments for heart valve disorders depend on the severity of the disorder and symptoms. Conservative treatments include:
Medications that are usually prescribed are:
- beta-blockers and calcium channel blockers (help control heart rate and blood flow)
- diuretics to reduce fluid retention
- vasodilators
Surgery: If a heart valve starts to affect the heart’s ability to pump blood around the body, it may need repair or replacement. A doctor may perform the following procedures:
- Heart valve repair eg Valvuloplasty (using a balloon to widen a narrowed heart valve)
- Heart valve replacement (if the valve can’t be repaired). The damaged valve is removed and replaced with a mechanical valve or one made from cow, pig or human heart tissue (biological tissue valve). Transcatheter aortic valve implantation (TAVI) involves putting in a new valve without removing the old valve.
- The most effective treatment in patients with severe aortic stenosis has traditionally been surgical aortic valve replacement. Open surgery however often leaves people immobile during recovery and in particular sternum healing, requiring a significant period of rehabilitation and is also associated with higher risk of complications and mortality in elderly patients. Transcatheter aortic valve implantation (TAVI), which is minimally invasive, is usually preferred in elderly or frail patients, but nevertheless is still associated with a significant period of recovery.[2]
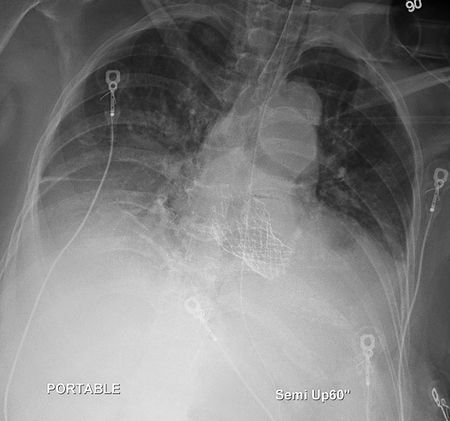
Image: AP portable radiograph demonstrates a transcather aortic valve replacement (TAVR).
Physiotherapy[edit | edit source]
Cardiac rehabilitation (CR) is defined as ‘the coordinated sum of activities necessary to provide patients with the best physical, social and mental circumstances, as well as make an impact on the underlying cause of cardiovascular disease. CR seeks to enable patients to maximise their function and halt or reverse disease progression through positive changes in healthier lifestyle behaviour. In addition to exercise training, comprehensive CR is recommended to include psychological and education-based interventions.
Valvular heart disease affects 1%-2% of young individuals. The management of exercising individuals with valvular heart disease requires a structured approach that incorporates several key factors including symptomatic status, functional capacity, type and nature of the valvular lesion, impact on ventricular structure and function and effect on pulmonary artery pressure.
- Asymptomatic individuals with minor valvular abnormalities may engage in all forms of competitive sport
- Those with lesions of moderate severity may exercise intensively if an exercise stress test tailored to the relevant physical activity reveals good functional capacity without myocardial ischaemia, haemodynamic disturbances or arrhythmia.
- Symptomatic athletes and those with severe valvular heart disease, impaired ventricular function, pulmonary hypertension and arrhythmias should refrain from most competitive sports.
- Athletes with a bicuspid aortic valve and aortic root diameter >40 mm should avoid sport with a strong isometric component even with minimal valvular dysfunction.
- There is an association between mitral valve prolapse and sudden cardiac death in the general population; however, there is limited evidence of increased risk with competitive sport.
- Athletes undergoing corrective surgery may return to exercise after 3 months if ventricular function and exercise capacity are preserved.
- Individuals anticoagulated for mechanical bioprosthetic valves should avoid contact or collision sport to minimise the risk of bleeding.[5]
See Cardiopulmonary Exercise Testing (CPET) In Adults: Cardiopulmonary exercise testing (CPET) is the study of responses of the cardiovascular and ventilatory systems to known exercise stress.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Heart Foundation Heart Valve disease Available:https://www.heartfoundation.org.au/conditions/heart-valve-disease (accessed 21.4.2021)
- ↑ 2.0 2.1 Anayo L, Rogers P, Long L, Dalby M, Taylor R. Exercise-based cardiac rehabilitation for patients following open surgical aortic valve replacement and transcatheter aortic valve implant: a systematic review and meta-analysis. Open heart. 2019 Apr 1;6(1):e000922.Available:https://openheart.bmj.com/content/6/1/e000922 (accessed 21.4.2021)
- ↑ 3.0 3.1 Oberman R, Bhardwaj A. Physiology, Cardiac. StatPearls [Internet]. 2020 Jul 21.Available: https://www.ncbi.nlm.nih.gov/books/NBK526089/(accessed 21.4.2021)
- ↑ Bandlamudi M, Ahmad M, Mungee S. Aortic Valvular Atresia. StatPearls [Internet]. 2020 May 13.Available: https://pubmed.ncbi.nlm.nih.gov/32491753/ (accessed 21.4.2021)
- ↑ Gati S, Malhotra A, Sharma S. Exercise recommendations in patients with valvular heart disease. Heart. 2019 Jan 1;105(2):106-10.Available: https://pubmed.ncbi.nlm.nih.gov/30262455/ (accessed 21.4.2021)