Wound Debridement
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
The concept of preparing the wound bed to promote reepithelialization of chronic wounds has been applied to wound management for more than a decade. The 4 general steps to follow for better preparation are compassed in the acronym DIME.
- D: Debridement of nonviable tissue within the Wound.
- I: Management of Inflammation and Infection
- M: Moisture control
- E: Environmental and Epithelialization assessment[1]
The primary goal of debridement is:
- Remove all the devitalized tissue from the wound bed to promote wound healing
- Removal of biofilm and bioburden(ie the number of microorganisms with which an object is contaminated and will affect the healing rate of the wound[2]) ,along with senescent cells.
- It is suggested to be performed at each encounter[1]
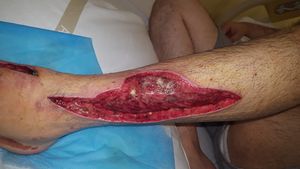
Image R:Aggressive debridement of Necrotizing fasciitis
Indications[edit | edit source]
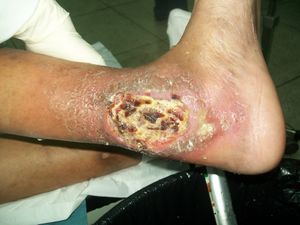
The indication for debridement is the removal of devitalized tissue such as necrotic tissue, slough, bioburden, biofilm, and apoptotic cells. Image R: diabetic ulcer prior to debridement.
Debridement is recognized as a major component of wound management to prepare the wound bed for reepithelialization.
Devitalized tissue:
- In general, and necrotic tissue, in particular, serve as the source of nutrients for bacteria.
- Acts as a physical barrier for reepithelialization (restoration of epithelium over a denuded area by natural growth or plastic surgery[3])preventing applied topical compounds to make direct contact with the wound bed to provide their beneficial properties.
- Necrotic tissue prevents angiogenesis, granulation tissue formation, epidermal resurfacing, and normal extracellular matrix (ECM) formation
- May prevent the clinician from making an accurate assessment of the extent and severity of the wound, even masking possible underlying infections[1]
Types of Debridement[edit | edit source]
Several types of the debridements exist. These include surgical debridement, biological debridement, enzymatic debridements, and autolytic debridement.
- Autolytic Debridement
- Most conservative type of debridement.
- Natural process by which endogenous phagocytic cells and proteolytic enzymes break down necrotic tissue.
- Highly selective process whereby only necrotic tissue will be affected in the debridement.
- It is indicated for noninfected wounds. It may also be used as adjunctive therapy in infected wounds. It can be used with other debridement techniques such as mechanical debridement in the case of infected wounds.
- It requires a moist environment and a functional immune system. The use of moisture retentive dressings can enhance it. This type of debridement induces softening of the necrotic tissue and eventual separation from the wound bed.
- The effectiveness of this type of debridement is mandated by the amount of devitalized tissue to be removed as well as the actual wound size.
- Autolytic debridement will take a few days. If a significant decrease in necrotic tissue is not seen in 1 or 2 days, a different method of debridement should be considered.
- Biological Debridement
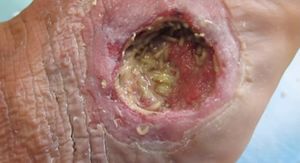
Biological debridement is the use of maggots, Lucilia sericata (green bottle fly), that are grown in a sterile environment and digest dead tissue and pathogens.- Sterile larvae of the Lucilia sericata species of the green bottle fly is an effective mode of debridement, particularly appropriate in large wounds where a painless removal of necrotic tissue is needed. The mechanism of action of mega therapy/debridement consists mainly of the release of proteolytic enzymes containing secretions and excretions that dissolve necrotic tissue from the wound bed.
- Maggots can be applied to the wound bed. They can be enclosed in a biological bag or are free range (Studies have shown that free-range maggots can debride a wound at least twice as fast as bag maggots)
- Contraindications to biological debridement are an abdominal wound contiguous with the intraperitoneal cavity, pyoderma gangrenosum in patients with immunosuppression therapy, and wounds in proximity to areas afflicted by septic arthritis.
- Enzymatic Debridement
This is a selective method for debridement of necrotic tissue using an exogenous proteolytic enzyme, collagenase, to debride Clostridium bacteria. Collagenase digests the collagen in the necrotic tissue allowing it to detach.- Performed by the application of a prescribed topical agent that chemically liquefies necrotic tissues with enzymes. These enzymes dissolve and engulf devitalized tissue within the wound matrix.
- Antimicrobial agents used in conjunction with collagenase can decrease the effectiveness of enzymatic debridement.
- This method can be used in conjunction with surgical and sharp debridement.
- This method can be expensive. [4]
- Enzymatic debridement is commonly used in the long-term care setting because there is less pain and nurses can apply it daily[1].
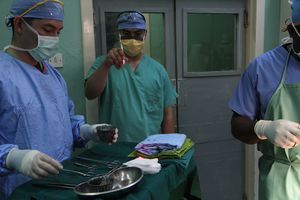
- Surgical Debridement with Sharp Instruments
This is a type of debridement where devitalized tissue in the presence of underlying infection is removed using sharp instruments such as a scalpel, Metzenbaum, curettes, among others.[1]- Promotes wound healing by removing biofilm and devitalized tissue.
- The level of debridement is determined by the level of devitalized tissue removal.
- The most aggressive type of debridement and is performed in a surgical operating room.
- Sharp and conservative debridement can be performed in a clinic or at the bedside with sterile instruments[4].
- Mechanical Debridement
Mechanical debridement is a nonselective type of debridement, meaning that it will remove both devitalized tissue and debris as well as viable tissue. It is usually carried using mechanical force: wet-to-dry, pulsatile lavage, or wound irrigation.- It is indicated for both acute and chronic wounds with moderate to large amounts of necrotic tissue, regardless of the presence of an active infection.
- Used to remove drainage and dead tissue from wounds.
- Wound Irrigation: a steady, gentle stream is used; pressure should be sufficient to reach the desired area, but not enough to force the fluid beyond the area to be irrigated. Pressure may be applied manually, such as with a bulb syringe or mechanical device, or by gravity[5].
- Pulsatile lavage is the delivery of an irrigating solution (or irrigant) under pressure that is produced by an electrically powered device. Irrigation under pressure may be delivered concurrently with suction, removing the irrigating solution from the target area.[6]
- A wet-to-moist dressing is another option accepted in long-term care (involves a primary dressing that directly touches the wound bed, and a secondary dressing covering it[7]). This type of dressing is used to promote moist wound healing and is used to remove drainage and dead tissue from wounds. They provide a moist healing environment, but they can require several dressing changes each day to maintain that moisture. These frequent dressing changes come with personal cost to the patient, financial cost in terms of nursing time and supplies, risk of infection associated with frequent dressing changes, and potential damage to the wound bed if the dressing is allowed to dry out.[7]
- Deep wounds with undermining and tunneling need to be packed loosely. Without packing, the space may close off to form a pocket and not heal leading to infection or abscess. This type of dressing is to be changed daily, compared with the wet-to-dry dressing, which is changed every 4 to 6 hours.[4][1].
Conclusion[edit | edit source]
- To promote healing, reduce risks of infection, and improve patients' outcomes an array of debridement methods should be included in the patient's wound management plan of care.
- Utilizing more than one debridement method will provide consistency in wound bed preparation toward healing.
- As a wound advances through the cascade of healing, the transition to wound closure can be timely..
- The complexity of a chronic wound may be frustrating and utilisation of the most appropriate method(s) of advanced wound care helps improve healing outcomes[4].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Manna B, Morrison CA. Wound debridement. StatPearls [Internet]. 2020 Feb 14.Available from:https://www.ncbi.nlm.nih.gov/books/NBK507882/ (last accessed 10.10.2020)
- ↑ Salcido R. What is Bioburden?: The Link to Chronic Wounds.Available from;https://journals.lww.com/aswcjournal/Fulltext/2007/07000/What_is_Bioburden___The_Link_to_Chronic_Wounds.1.aspx (last accessed 10.10.2020)
- ↑ Merriam webster Reepitheliazition Available from:https://www.merriam-webster.com/medical/reepithelialization (last accessed 10.10.2020)
- ↑ 4.0 4.1 4.2 4.3 Wound Source Wound Debridement Available from:https://www.woundsource.com/blog/wound-debridement-options-5-major-methods (last accessed 11.10.2020)
- ↑ Free Dictionary Available from: https://medical-dictionary.thefreedictionary.com/wound+irrigation (last accessed 11.10.2020)
- ↑ Luedtke-Hoffmann KA, Schafer DS. Pulsed lavage in wound cleansing. Physical Therapy. 2000 Mar 1;80(3):292-300.Available from:https://academic.oup.com/ptj/article/80/3/292/2842509 (last accessed 11.10.2020)
- ↑ 7.0 7.1 BC campus Wound Care Available from:https://pressbooks.bccampus.ca/clinicalproceduresforsaferpatientcaretrubscn/chapter/4-6-advanced-wound-care-wet-to-moist-dressing-and-wound-irrigation-and-packing/ (last accessed 11.10.2020)