The Diabetic Foot
Original Editor - Tarina van der Stockt
Top Contributors - Tarina van der Stockt, Kim Jackson, Niha Mulla, Chelsea Mclene, Lauren Lopez, WikiSysop and Rachael Lowe
Introduction and description[edit | edit source]
Diabetes is a disease in which ones blood sugar levels are higher than normal range. Foot problems are very common in people with diabetes as high blood sugar damages the nerves and blood vessels in the feet.
The nerve damage is called diabetic neuropathy and it causes numbness, tingling and pain. As the neuropathy advances it leads to loss of sensation in feet.
Complications in the diabetic foot are mostly caused by a triad of ischemia, diabetic neuropathy, and infection. [1]
Statistics about the impact of diabetic foot complications:[1]
- Foot ulcer complications are the main reason why people with diabetes are hospitalized and have to undergo amputations.
- 20-40% of all the health care costs comprised for diabetes are for diabetic foot complications
- 7-10% of patients with diabetes and neuropathy will develop an ulcer; this increases up to 30% for patients with diabetes and other comorbidities.
- 5-8% of patients will undergo a major amputation 1 year after developing a diabetic ulcer.
- A foot ulcer preceded 85% of diabetes related amputations.
- “Diabetes increases the risk of amputation 8-fold in patients aged >45 years,8 12-fold in patients aged>65 years and 23-fold in those aged 65––74 years.”
More information on Diabetes is available from these Physiopedia pages: DM Type 2 and DM Type 1, Diabetes
Specific conditions and diabetic foot[edit | edit source]
Diabetic Neuropathy[edit | edit source]
Due to diabetic neuropathy patients do not have the protective sensation in their feet. Thus the patient will not feel any trauma, like stepping on something sharp or wearing tight shoes. This could lead to continuous tissue damage, ulceration, foot deformities, increased plantar pressure, and infection. [2]
Diabetic Neuropathy causes; numbness in the hands or feet, tingling or burning sensation in the feet, pain, distal- proximal or more focal weakness and dry or cracked skin.
Read more by clicking here; Diabetic Neuropathy
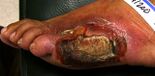
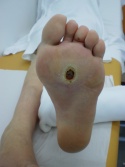
Diabetic Foot Ulcers and Delayed Wound Healing[edit | edit source]
- In the diabetic foot peripheral arterial disease (PAD) is seen as the primary cause for vascular impairment.[1]
- The risk of developing PAD is increased with diabetes. And ischemia is considered the biggest culprit delaying wound healing.[1]
- Diabetic neuropathy and ischemia combined is called neuroischemia and in these cases wound healing is affected by the severity of the ischemia.[1]
- Read more by clicking here; Diabetes Mellitus and Diabetic Ulcers
Diabetic Foot Infections[edit | edit source]
- The most common sign of diabetic foot infections is increased ulcer exudation rate.[1]
- Diabetic foot infections are mainly caused due to poor glycemic control. [1]
- There is a 50% delay in diagnosing deep foot infections in diabetic patients because the infection markers in the patients blood tests are found to be absent. [1]
- Infections in a diabetic foot can rapidly spread to the rest of the body and if not treated properly and in time, it could lead to a life-threatening general septic infection [1]
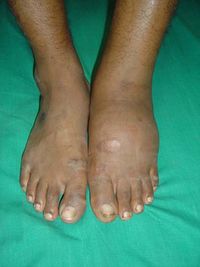
Charcot foot/joint[edit | edit source]
Charcot foot also known as Diabetic foot arthropathy. I is a complication of diabetes and can lead to amputation if left unmanaged. It affects the joint and bone structure of people with neuropathy. Although it is more common in diabetes to affect the foot it can also bee seen in the knee, hip and spine.[3]
Symptoms include: [3]
- Inflammation
- Redness
- Warm to touch feet or affected area
- Dislocation, caused by instability of the joints
- Muscle weakness in the feet, ankles, legs and hands
- Bony protrusions on the plantar aspect of the foot
- Awkward way of walking (gait)
- Deformation of the foot
- Numbness in the feet, arms and hands
Assessment[edit | edit source]
Clinical Examination according to Lep¨antalo et al. [1]
- History
- General (Medications, diseases, cardiovascular risk factors, work, hobbies, lifestyle, diabetes symptoms/complications
- Foot specific (risk factors and information about present ulcer – duration, treatment, aetiology)
- Inspection (at least once a year)
- Vascular
- Dorsalid Pedis Pulse
- Tibialis posterior pulse
- Venous refilling time - >5sec on dependency
- Foot appearance
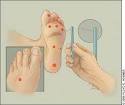
- Neurological
- 10-gram (5.07) Semmes––Weinstein monofilament
- Vibration(128 Hz-tuning fork)
- Pinprick discrimination and tactile sensation on the dorsum of the foot
- Achilles tendon reflexes
- Observe for foot deformities or bony prominences
- Ulcer – look for perfusion, extent and size, and infection
- Infection
- Local signs and symptoms of inflammation: purulent secretion, redness, warmth, swelling, pain, delayed healing, and or bad odor.
- Systemic signs: fever, and poor general condition
- Increased exudation in the ulcer
- X-rays to determine the presence of foreign bodies, gas, osteomyelitis, osteolysis, or joint effusion
- MRI, bone scan or CT scan to determine the extent of the infection
- Non-invasive vascular studies
- Ankle pressure
- Ankle-brachial systolic pressure index (ABI) (<0.6indicates significant ischemia in respect to wound healing)
- Toe pressures (<30 mmHg indicates severely impaired healing)
- Vascular imaging
- Sub-talar ROM (any reduction may increase plantar pressures during walking) [2]
Diabetic foot/stump assessment form
Management / Interventions[edit | edit source]
Physical Therapy[edit | edit source]
- Physical Therapists are involved in both the prevention and management of diabetic foot complications. [5] This is done by gait, posture, and foot off-loading education and training.[5]
- Diabetes Medical and Physical Therapy Management
- Ankle and foot arthropathies Medical Management
- Physical Activity in Diabetes
- Diabetic foot Management
- Diabetic Neuropathy Management/Intervention
- The Physical Therapist is also involved in the rehabilitation process after an amputation.
Patient education[edit | edit source]
Diabetic Foot Care[edit | edit source]
- Inspect your feet daily. Check for cuts, blisters, redness, swelling or nail problems and inform doctor if you notice any changes.[6]
- Bathe feet in lukewarm water.
- Wash feet using a soft washcloth or sponge. Dry by blotting or patting and carefully dry between the toes.
- Moisturize your feet but not between toes as it can cause fungal infections.
- Cut nails carefully.[7]
- Never treat corns or calluses yourself.
- Wear clean, dry socks and change them daily.
- Wear socks to bed.
- Shake out your shoes and feel the inside before wearing to check for any foreign bodies.
- Keep your feet warm and dry. Consider using an antiperspirant on soles.
- Never walk barefoot.
- Keep blood sugar levels under control.
- Do not smoke.
- Get periodic foot exams.[8]
- Diabetes Complication and Amputation Prevention.
- Shoes and Orthotics for Diabetics
- In a 2009 evidence-based literature review, the authors found that TENS might be effective for pain treatment in diabetic neuropathy.[9]
- The authors of a 2008 control study of 30 neuropathic diabetic patients concluded that as part of the multidisciplinary approach physical therapy plays an important role in the treatment of diabetic neuropathic patients. [2]
They used the following adjunct on the treatment group every day for twelve weeks:- Low level laser irradiation for 10-15 minutes/session on the ulcer
- Laser biostimulation on the peroneal nerve trunk (at the fibula head) at 1000 Hz for 15 minutes
- Specific dorsiflexion and ankle ROM exercises
- Education on foot care and home exercises
Medical Management[edit | edit source]
- Diabetic Wound Care Management.
- Antibiotic treatment is indicated in all infected wounds in combination with wound care, until the infection is cleared up.[1]
- Hospitilisation, immobilisation, and IV antibiotics are indicated for limb threatening or uncontrolled infections.[1]
- Urgent surgery is indicated if the infection is "accompanied by a deep abscess, extensive bone or joint involvement, crepitus,
substantial necrosis or gangrene, or necrotising fasciitis."[1] Lepäntaloa et al. recommend that "surgical intervention for moderate or severe infections is likely to decrease the risk of major amputation."[1]
Resources[edit | edit source]
These articles are recommended for further in depth reading on the subject:
- Lepäntaloa M, Apelqvistc J, Setaccie C, Riccof JB, de Donatoe G, Beckerg F, Robert-Ebadig H, Caoh P, Ecksteini HH, De Rangok P, Diehml N. Chapter V: Diabetic Foot. European Journal of Vascular and Endovascular Surgery. 2011;42(S2):S60-74
- Pedrosa HC, Leme LA, Novaes C, Saigg M, Sena F, Gomes EB, Coutinho A, Borges Carvalho WJ, Boulton A. The diabetic foot in South America: progress with the Brazilian Save the diabetic foot project. International Diabetes Monitor. 2004;16(4):17-23.
- Turan Y, Ertugrul BM, Lipsky BA, Bayraktar K. Does physical therapy and rehabilitation improve outcomes for diabetic foot ulcers?. World journal of experimental medicine. 2015 May 20;5(2):130.
Case Studies[edit | edit source]
- Amputation secondary to Diabetes Mellitus: Amputee Case Study
- A 35 year old diabetic Aboriginal women, who underwent a right transtibial amputation for diabetic foot ulcer and completed prosthetic rehabilitation: Amputee Case Study
- Diabetic patient amputation: Amputee Case Study
- Diabetic complications leading to amputation: Amputee Case Report
- Diabetic Patient with Bilateral Amputations : Amputee Case Study
- The Young, Diabetic Amputee: Amputee Case Study
- Bilateral Below Knee Amputation due to Diabetic Complications: Amputee Case Study
- Lower Limb Amputation: Diabetic Case Presentation: Amputee Case Study
- Older Diabetic Amputee with slow healing: Amputee Case Study
Follow this link to read more case studies.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Lepäntaloa M, Apelqvistc J, Setaccie C, Riccof JB, de Donatoe G, Beckerg F, Robert-Ebadig H, Caoh P, Ecksteini HH, De Rangok P, Diehml N. Chapter V: Diabetic Foot. European Journal of Vascular and Endovascular Surgery. 2011;42(S2):S60-74.
- ↑ 2.0 2.1 2.2 Zakaria HM, Adel SM, Tantawy SA. The Role of Physical Therapy Intervention in the Management of Diabetic Neuropathic Foot Ulcers. Bull. Fac. Ph. Th. Cairo Univ. 2008 Jul;13(2).
- ↑ 3.0 3.1 Dardari D. An overview of Charcot’s neuroarthropathy. Journal of Clinical & Translational Endocrinology. 2020 Dec;22.
- ↑ Youtube Video: The Diabetic Foot Exam https://youtu.be/aVz-Ja9Grvg
- ↑ 5.0 5.1 Kalra S, Kalra B, Kumar N. Prevention and management of diabetes: the role of the physiotherapist. Diabetes Voice. 2007;52 (3)
- ↑ Reiber GE. Diabetic foot care. Financial implications and practice guidelines. Diabetes care. 1992 Mar 1;15:29-31.
- ↑ Bakker K, Apelqvist J, Schaper NC, International Working Group on the Diabetic Foot Editorial Board. Practical guidelines on the management and prevention of the diabetic foot 2011. Diabetes/metabolism research and reviews. 2012 Feb;28:225-31.
- ↑ Pinzur MS, Slovenkai MP, Trepman E, Shields NN. Guidelines for diabetic foot care: recommendations endorsed by the Diabetes Committee of the American Orthopaedic Foot and Ankle Society.
- ↑ Dubinsky RM, Miyasaki J. Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review) Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology. 2010 Jan 12;74(2):173-6.