Wound Assessment
Original Editor - Lucinda Hampton
Top Contributors - Lucinda hampton, Abbey Wright and Kim Jackson
Introduction[edit | edit source]
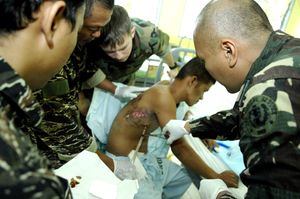
A wound is damaged or disruption to the skin. Before treatment, the exact cause, location, and type of wound must be assessed to provide appropriate treatment.[1]
Wound healing is a complex physiological process occurring after an injury in the cells and tissues of our bodies to restore function of the tissue.
The healing process is affected by:
- Severity of the wound
- Location,
- Extent of injury
- External and internal factors that will either inhibit or promote wound healing.
A health care provider must understand how to assess a wound, assess external and internal factors, and determine treatment to optimize the healing process[2].
Why Assess?[edit | edit source]
Wound assessment is performed to determine the appropriate treatment for an extremely diverse grouping of disease processes. Each of the underlying etiologies of the given wound must be identified and treated as if it were its own disease (not a blanket classification of "wound").
It is important for healthcare professionals to all assess wounds as it provides better care for the patient, however, specific training courses may be beneficial to provide the same standard of care[3].
While there are many excellent biologics, skin grafts, and other options available, without the appropriate understanding of the nature of the wound the chances of healing decline significantly.[1]
Areas Of Concern[edit | edit source]
While some wounds are simple, the majority of wounds we encounter are caused by, or complicated by, some other issues:
- Chronicity: chronic wounds will have a different makeup than that of an acute wound, requiring conversion for healing.
- Infection: an underlying infection will prevent wound healing even if the infection is subacute.
- Blood supply: damaged or constricted arterial supply will prevent appropriate blood flow to the wound. Equally damaged venous supply will cause venous stasis.
- Compression: Physical pressure on chronic ulceration will cause repeated damage and prevent healing[1].
Types of Wounds[edit | edit source]
Wounds are initially classified as:
- Acute: healing occurs in a short time frame without complications. Such as a surgical incision or a traumatic wound (stab or gunshot are common examples).
- Chronic: healing occurs over weeks to years, and treatment is usually complex. Such as venous and arterial ulcers, diabetic ulcers, and pressure ulcers.
Wounds can further be categorised by type or cause.
The table below lists the six main types of wounds:
| Surgical | Purposeful incision, done in sterile conditions. Healing occurs by primary, secondary, or tertiary intention. | ||
| Traumatic | Non-purposeful incisions, not done in sterile conditions. E.g. gunshot wounds, stab wounds, accidental cuts. These wounds may be start off as acute but could become chronic if not treated. | ||
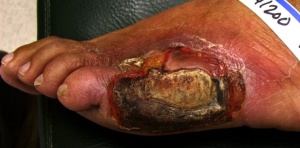
| Diabetic/neuropathic ulcer | These wounds generally occur as a result of damage to the autonomic, sensory, or motor nerves and have an arterial perfusion deficit. They are usually located in the lower extremity on the foot. Diabetic/neuropathic ulcers are often small with a calloused edge. Pain may be absent or severe depending on the neuropathy. | ||
| Arterial ulcer | Arterial ulcers occur when tissue ischemia occurs due to arterial insufficiency from the narrowing of an artery by an obstruction (atherosclerosis). They are located on the distal aspects of the arterial circulation, and can be anywhere on the legs, including feet or toes. Wound margins are well defined with a pale wound bed with little or no granulation. Necrotic tissue is often present. There is minimal to no exudate present. Pedal pulses are usually absent or diminished. Pain occurs in limb at rest, at night, or when limb is elevated.
Account for 5% to 20% of all leg ulcers. Perfusion must be assessed prior to initiating treatment. | ||
| Venous ulcer | Lower extremity wound. Tissue ischemia occurs due to the failure of the venous valve function to return blood from the lower extremities to the heart. It is usually located in the ankle to mid-calf region, usually medial or lateral, and can be circumferential. Drainage can be moderate to heavy. A venous ulcer can be irregularly shaped, large, and shallow with generalized edema to lower limbs. Pulse may be difficult to palpate.
Account for 70% to 90% of all leg ulcers. Perfusion must be assessed prior to initiating treatment. | ||
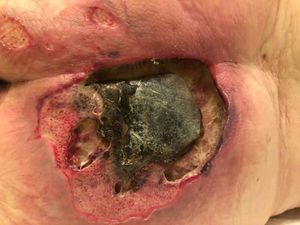
| Pressure ulcer | Localized area of tissue damage that results from compression of soft tissue between a hard surface and a bony prominence (coccyx, ankle, shoulder blade, or hip). As blood supply decreases to the area of compression, tissue anoxia occurs, which can lead to eventual tissue death. Wounds are usually circular and may have viable or necrotic tissue, and exudate can vary from none to heavy. Pressure ulcers are classified depending on the level of tissue damage (stages 1 to 4). Treatment is based on stage, exudate, type of available dressing, and frequency of dressing changes. |
Wound Assessment[edit | edit source]
A holistic assessment of the patient is essential to identify the causative or contributory factors and to highlight issues that could delay wound healing. The following factors must be considered when choosing an appropriate plan of care.
These factors above will either delay or promote the wound healing process. Successful wound healing is dependent on the patient’s ability to heal, not the dressing used.[4]
Should include a comprehensive:
| General Information | Subjective History | Past medical History | Objective Assessment |
|---|---|---|---|
| Age | Patient history of the wound | History of previous wounds | Identify the location of the wound |
| Medication and allergies | Determine the cause of the wound | Other diseases such as
|
Condition of the wound bed and peri wound area |
| Pain[1] | Obesity | Amount, colour, and consistency of exudate as well as signs of infection. | |
| Nutritional status and fluid intake | Determine the stage of the wound
| ||
| Smoking/alcohol | Evaluate and measure the depth, length, and width of the wound | ||
| Mobility level | Measure the amount of undermining and tunnelling | ||
| Pressure sore risk | Evaluate the wound bed | ||
| Skin sensitivity and integrity[4] | Assess for presents, type, and amount of exudate:
| ||
| Continence | Evaluate for signs and symptoms of infection (warm, pain, odour, delayed healing) | ||
| Oxygen deficit/anaemia |
Most chronic wounds are complex and best managed by an interprofessional team that includes a wound care nurse, general and vascular surgeon, hyperbaric specialist, infectious disease consultant, dietitian, and physical therapist. The key is to first find out the cause of wound breakdown. Without resolving the primary cause, wounds cannot heal.[1]
Physiotherapy considerations[edit | edit source]
When considering patients with any type of wound, from chronic to acute, it is important for physiotherapists to consider the impact the wound may have on the patient's mobility, pain and range of movement of the area where the wound is.
In acute wounds such as TKR or THR these are elective and will most likely heal quickly, however, pain can be generated from the wound especially in the first few days post-op. In a small cohort of patients these wounds can become infected, which can lead to longer term mobility issues and feeling generally unwell which could also lead to more bed rest, and overall increase the risk of post-op complications[5]. With this in mind some steps to improve healing can be done which can lead to reduced risk of infection and better functional outcomes post op such as compression bandages[6].
In chronic wounds such as venous leg ulceration, mobility is likely to be reduced, therefore we need to consider additional care for them such as walking aids, more intense physiotherapy and MDT wound management[7]. This cohort of patients are also more likely to have additional past medical history issues, so this should be considered when assessing them.
Conclusion[edit | edit source]
Accurate wound assessment is vital to give a successful resolution and uncomplicated wound healing. It provides valuable information to enable informed decisions about a patient and their wound.[4]In relation to physiotherapy it is necessary to understand the impact wounds can have on the patient in regards to pain, mobility and movement of the affected joints, along with the phycological impact wounds can have on motivation and self-image.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Nagle SM, Waheed A, Wilbraham SC. Wound Assessment InStatPearls [Internet] 2020 Apr 28. StatPearls Publishing.Available from:https://www.ncbi.nlm.nih.gov/books/NBK482198/ (last accessed 9.10.2020)
- ↑ 2.0 2.1 BC campus CLINICAL PROCEDURES FOR SAFER PATIENT CARE Available from:https://opentextbc.ca/clinicalskills/chapter/introduction-3/ (last accessed 9.10.2020)
- ↑ Iyun AO, Ademola SA, Michael A, Olawoye O, Oluwatosin O. Perception of healthcare professionals in University College Hospital, Ibadan toward wound care. Nigerian Journal of Plastic Surgery. 2016 Jul 1;12(2):47. BibTeXEndNoteRefManRefWorks
- ↑ 4.0 4.1 4.2 Activheal academy Wound Assessment Available from:http://academy.activheal.com/lessons/sf-wound-assessment-simplified/ (last accessed 9.10.2020)
- ↑ Khan J. Risk Factors of Infection in Total Knee Arthroplasty. Journal of Rawalpindi Medical College. 2017 Sep 30;21(3):253-6.
- ↑ Cheung A, Lykostratis H, Holloway I. Compression bandaging improves mobility following total knee replacement in an enhanced recovery setting. Journal of perioperative practice. 2014 Apr;24(4):84-6.
- ↑ Roaldsen KS, Rollman O, Torebjörk E, Olsson E, Stanghelle JK. Functional ability in female leg ulcer patients—a challenge for physiotherapy. Physiotherapy Research International. 2006 Dec;11(4):191-203.