Carers Guide to Dementia
Original Editor - Aileen Lambe, Aisling Kavanagh, Carla Ellis, Claire Hagan as part of the Queen Margaret University's Current and Emerging Roles in Physiotherapy Practice Project
Top Contributors - Carla Ellis, Aisling Kavanagh, Scott Buxton, Claire Hagan, Aileen Lambe, Kim Jackson, Lucinda hampton, Shaimaa Eldib, Admin, Gillian Condy, 127.0.0.1, Eugenie Lamprecht, Tony Lowe, Vidya Acharya and Lauren Lopez
Introduction[edit | edit source]
Currently, Dementia, a neurodegenerative disease, has no known cure and is not part of the normal ageing process. It is characterised by changes in reasoning, memory, comprehension, problem-solving, and/or attention[1].
- Currently more than 55 million people live with dementia worldwide, and there are nearly 10 million new cases every year.
- Dementia results from a variety of diseases and injuries that primarily or secondarily affect the brain. Alzheimer's disease is the most common form of dementia and may contribute to 60-70% of cases.
- Dementia is currently the seventh leading cause of death among all diseases.
- Dementia has physical, psychological, social and economic impacts, not only for people living with dementia, but also for their carers, families and society at large.[2]
Types of Dementia[edit | edit source]
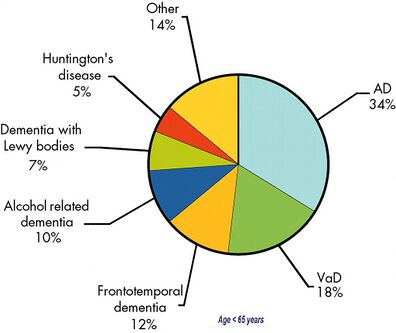
There are many types of dementia. Types of dementia include:
- Alzheimer's disease: most common type It accounts for 60-70% of cases of dementia
- Vascular dementia: second most common type (following cerebrovascular accident). See also Subcortical Vascular Dementia: Case Study
- Fronto-temporal lobar degeneration dementia
- Huntington's disease
- Alcohol related dementia (Korsakoff's syndrome)
- Motor Neurone Disease.
- Multiple Sclerosis (MS)..
- Parkinson's (2%).
- HIV related cognitive impairment.
- Creutzfeldt-Jakobs Disease (CJD), degenerative brain disorder that leads to dementia and it belongs to prion diseases.[3]
Normal Ageing Vs Early Signs of Dementia [edit | edit source]
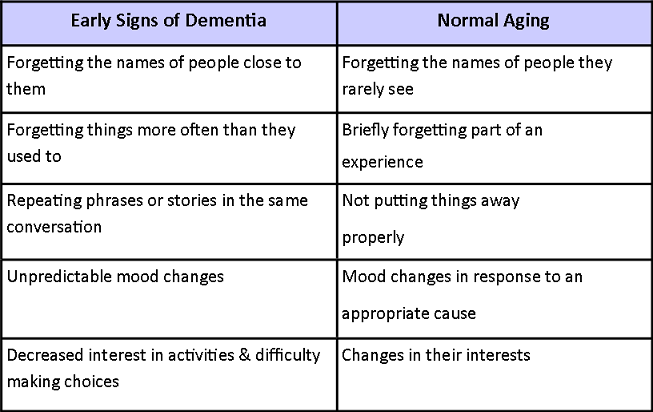
It is sometimes difficult to tell the difference between what is normal ageing and what is the early onset of dementia (see Perceptions about Ageing and Ageism). You may be concerned that an elderly relative or friend is developing dementia. So, how will you know? You can use this table to compare the signs of early-onset dementia and normal ageing.[4]
The 3 Stages of Dementia[edit | edit source]
This table shows the 3 generalised 'main stages' of the different types of dementia.
Some symptoms may appear earlier or later than indicated on this table and the stages may overlap. Progression through the stages varies from person to person and depends on many factors including:
- The type of dementia
- Age of onset
- The presence of other illnesses
- The level of support and care available
What else to expect?[edit | edit source]
- Depression: People with dementia may suffer from depression and/or behavioural problems. They may often become easily irritated/ frustrated or act aggressively towards a family member or friend. Behaviour management is one strategy that is used to decrease depression in individuals with dementia and can be carried out by carers. For example, reducing the repetition of words, managing aggression and the eating behaviours in people with dementia has a positive effect on their behaviour and overall well-being [8].
- Mood: Mood is also commonly affected in individuals with dementia. Individuals can often become flustered and distressed and in some cases can become aggressive and depressed. Regular movement will balance their mood, help to reduce depression and keep them calm. Physical activities can help improve sleep pattern which can often be disturbed by dementia. Regular routines can include household activities, exercise classes, resistance training and stretching [9].
What Can Physiotherapy Offer?[edit | edit source]
Physiotherapists use movement of the body to help bring about physical, psychological and social well-being. Physiotherapy has an important role in promoting and maintaining mobility in people with dementia as well as improving their quality of life and reducing the burden of care.
Fall prevention: Poor balance is known to increase the risk of falls. Physiotherapy can lower an individual's risk of falling by providing exercises specifically for improving balance. Fall prevention programmes can also address their fear of falling to ensure they maintain independence and safety with ADLs. For more information see here Falls and Dementia
Benefits of Exercise: Exercise has been shown to:
- Reduce the risk of coronary heart disease, stroke, certain types of cancers and diabetes.
- Prevent post-menopausal osteoporosis and therefore reduce the risk of osteoporotic fractures.
- Reduce the complications of immobility
- Reduce the risk of accidental falls
- Improve mental/cognitive function, reduces stress/anxiety and improve self- confidence
Physiotherapy & Exercise[edit | edit source]
Physiotherapy can provide;
- Strengthening exercises: to increase bone strength and decrease the risk of osteoporosis.
- Balance: to prevent falls and increase confidence in everyday tasks.
- Flexibility & stretching: to prevent muscle tightening and make movement easier.
- Maintenance of independence: to stay as involved as possible for as long as possible in everyday life.
- Postural management: Regular change in body position is essential for comfort and prevention of poor posture which may lead to muscle tightness and spasms, decreased movement of joints and pressure sores [10].
- Help and advice on aids for the house: Equipment and adaptations at home will help make life easier for your loved one with dementia and keep them independent for as long as possible
It is also assessed everyday activities such as walking, going up and downstairs, getting out of a chair and getting in and out of bed. If someone is struggling to do any of these activities appropriate exercises should be incorporated into the treatment plan.
Physiotherapy and Pain[edit | edit source]
Physiotherapy can help manage pain. Pain affects mental function, motivation and will affect how the person with dementia responds to any rehabilitation programme. People living with dementia who have difficulty speaking will not be able to easily report pain. These people are at risk of receiving inadequate medication and treatment of pain. It is important that pain is addressed before and during therapy to allow for better rehabilitation [8].
Education[edit | edit source]
By teaching carers about the disease, they will know what to expect and be better able to handle the challenges associated with dementia. Some suggestions are:
- Create a daily routine with small rituals - Predictability can be calming. This may help to relax the person.
- Allow the individual do as much as they can independently
- Give the individual a role/task; doing the washing up, peeling the vegetables, pairing socks.
- Do less for them while encouraging them to do more for themselves.
- If motivation is an issue, make the tasks functional: walk to the kitchen to get a drink instead of carrying it to them.
- If the person is wandering around or restless, then think about why this might be happening. Some people walk because they are bored, have excess energy or it may be a reaction to an hallucination.
- By doing as much as possible by themselves, they will be more likely to retain their self esteem.
- Plan activities that you can both enjoy
- If it is realistic to do so, encourage them to take the person for a walk each day. It will burn off energy and the fresh air will do them both good.
- Encourage other activities such as gardening, baking, listening to music, singing, dancing or playing cards. What is important is that the person is participating in an activity that makes him/her feel useful.
- Assess the home - The home can be full of potential hazards contributing to falls. Make sure there is nothing around the house that the person could trip on. For example carpets, rugs, doorway thresholds.
See also Preventing Dementia and Cognitive Decline
Improve Communication[edit | edit source]
- Keep commands simple- one request at a time.
- Allow extra time for a response to your question before repeating it.
- If the individual doesn't appear to understand your request, try rephrasing it.
- Don't chat whilst the person is trying to perform a task, this will likely be a distraction.
- Make sure communication problems are not due to problems with the individual's sight or hearing. Check that glasses and hearing aids are in good working order.
- Use names and explain phrases where possible, such as "Your son, John."
Other forms of communication that may be useful [edit | edit source]
Touch :can be used to help movement during walking by placing a hand on their shoulder or by taking their hand.
Sounds :can provide extra stimulation to encourage normal movement or to trigger a response to an instruction. Walking can improve by providing rhythm, for example counting aloud or by playing music with a rhythm the person can walk to.
Visual communication: can be used to show tasks or give instructions. When performing exercises it is betting o show the exercise than to say the instructions [8].
References[edit | edit source]
- ↑ NHS Choices 2012. www.nhs.uk/conditions/dementia/pages/introduction/apsx (accessed 21/10/2012)
- ↑ WHO Dementia Available:https://www.who.int/news-room/fact-sheets/detail/dementia (accessed 13.9.22)
- ↑ Gubbels S, Bacci S, Laursen H, Høgenhaven H, Cowan S, Mølbak K, Christiansen M. Description and analysis of 12 years of surveillance for Creutzfeldt–Jakob disease in Denmark, 1997 to 2008. Eurosurveillance. 2012 Apr 12;17(15):20142.
- ↑ Alzheimers UK (2012) Available online at: http://www.alzheimers.org.uk/site/scripts/documents_info.php?documentID=120 Accessed on 12/11/2012
- ↑ http://www.onmemory.ca/en/signs_symptoms/aging_vs_alzheimers/ (accessed on 21/10/2012)
- ↑ http://www.psychiatry24x7.com/bgdisplay.jhtml?itemname=dementia_memoryloss
- ↑ Psychiatry 24 7 (2012) Available online at:http://www.psychiatry24x7.com/bgdisplay.jhtml?itemname=dementia_symptoms#stages Accessed 12/11/2012)
- ↑ 8.0 8.1 8.2 Marshall, M. 2005. Perspectives on Rehabilitation and Dementia. [Online book] London: Jessica Kingsley. Available at: http://books.google.co.uk/books/about/Perspectives_On_Rehabilitation_And_Demen.html?id=KqhaW28SZ8oC [Accessed November 05 2012]
- ↑ Dementia Physiotherapist (2012) Available online at: http://www.healthcentre.org.uk/physiotherapists/physiotherapist-dementia.html Accessed 12/11/2012)
- ↑ NHS Postural Management Survey 2012