Malnutrition
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Rucha Gadgil
Introduction[edit | edit source]
Malnutrition means ‘poor nutrition’ when there is a deficiency of energy and nutrients in the diet that causes a measurable clinical outcome or impact on body composition or function. As such, malnutrition can refer to people who are overweight but the term is more often used to apply to people who are underweight[1]ie:
- Undernutrition’—which includes stunting (low height for age), wasting (low weight for height), underweight (low weight for age) and micronutrient deficiencies or insufficiencies (a lack of important vitamins and minerals).
- Overweight, obesity and diet-related noncommunicable diseases (eg heart disease, stroke, diabetes, and cancer)[2].
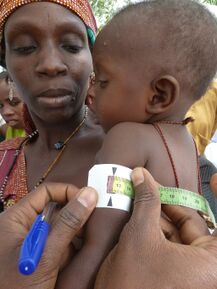
Image 1: A child is checked for signs of malnutrition in Katsina State, Nigeria,
Epidemiology[edit | edit source]
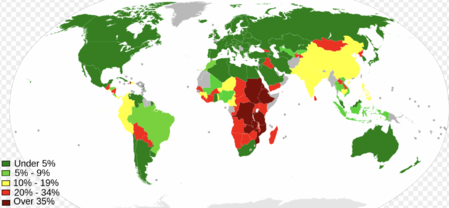
Malnutrition affects people in every country. Image 2: Global malnutrition map 2010-2012 .
- Around 1.9 billion adults worldwide are overweight, while 462 million are underweight.
- An estimated 41 million children under the age of 5 years are overweight or obese, while some 159 million are stunted and 50 million are wasted.
- Adding to this burden are the 528 million or 29% of women of reproductive age around the world affected by anaemia, for which approximately half would be amenable to iron supplementation[2].
- Malnutrition is common in Australia. Those most at risk are the elderly, half of older Australians living in aged care or at home are either at risk of malnutrition or are malnourished.
- People who have eating disorders, people with a poor appetite, and people with medical conditions such as cancer, HIV or kidney failure need more nutrients and hence are at risk of malnutrition[3].
Causes[edit | edit source]
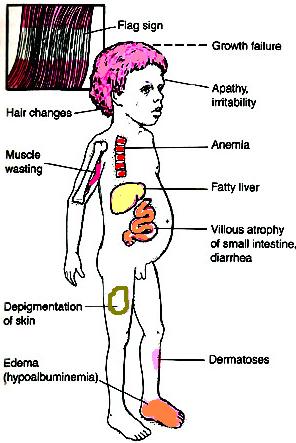
- The most-common form of malnutrition is protein-energy malnutrition. This occurs when a person gets too little protein, too few calories, or both. Kwashiorkor is a severe protein deficiency. It is common among young children in developing countries. Image 3: Kwashiorkor. Marasmus is another kind of malnutrition that results from not enough protein or calories. Children with marasmus do not grow properly, and their fat and muscles waste away. Other symptoms include dehydration and dry, loose skin. Marasmus occurs mostly among very young children, usually under famine conditions.
- People who do not receive vitamins and minerals for a long period of time can develop certain disorders. eg an iron deficiency causes anemia, lack of iodine causes goiter (enlargement of the thyroid gland), vitamin A deficiency can cause blindness or loss of vision, children who do not have enough vitamin D can lead to rickets. Vitamin C deficiency leads to scurvy. Vitamin B12 deficiency can cause blood disorders, affect the nervous system and also cause the intestine to function improperly. Too little thiamin in a diet can result in beriberi. Beriberi damages the nerves and heart.[4]
- Obesity is a form of malnutrition. It is when a body consumes more calories than it can use. This causes the body to have too much extra fat. Obesity can contribute to many health problems, including high blood pressure, heart disease, stroke, diabetes, and arthritis. Malnutrition can also be caused by eating disorders eg Anorexia nervosa[4].
The Hospital Setting[edit | edit source]
Malnutrition has been identified as a significant clinical problem in hospital settings both nationally and internationally. Malnutrition has been strongly associated with adverse clinical outcomes such as an increased length of stay and higher rates of medical complications.
Image 4: Essential nutrients are one of the main requirements of elderly care.
- An Australian study found the prevalence of malnutrition to be 53%.[5]
- A review of the publications on hospital malnutrition in Europe over the last 5 years shows that the incidence and prevalence of malnutrition are still very high: 21 and 37%, respectively.[6]
Malnutrition in low- and middle-income countries[edit | edit source]
More than one in three low- and middle-income countries (LMIC) face both extremes of malnutrition.
- The poorest low- and middle-income countries are seeing a rapid transformation in the way people eat, drink, and move at work, home, in transport and in leisure. The emerging malnutrition issues in these LMIC is being driven by factors beyond their control. This new nutrition reality is driven by changes to the food system, which have increased availability of ultra-processed foods that are linked to increased weight gain, while also adversely affecting infant and pre-schooler diets. These changes include disappearing fresh food markets, increasing supermarkets, and the control of the food chain by supermarkets, and global food, catering and agriculture companies in many countries.
- Exposure to undernutrition early in life followed by becoming overweight from childhood onwards increases the risk of a range of non-communicable diseases. This is a key factor driving the emerging global epidemics of type 2 diabetes, high blood pressure, stroke, and cardiovascular disease. Negative effects can also pass across generations eg Maternal obesity increases the likelihood of the child having obesity and may be exacerbated if the mother was undernourished in early life[7].
- This double burden of malnutrition among women of reproductive age in 55 low- and middle-income countries continues as a major public health problem worldwide. Overall in LMIC underweight is declining but the dramatic increase of overweight will supersede this decline. None of the 55 LMICs is likely to eradicate malnutrition in women by 2030. Effective strategies and nutrition interventions need to be instituted to minimize the nutritional disparities across subpopulations[8].
Addressing the Problem[edit | edit source]
In April 2016, the United Nations General Assembly adopted a resolution proclaiming the UN Decade of Action on Nutrition from 2016 to 2025. The Decade aims to catalyse policy commitments that result in measurable action to address all forms of malnutrition. The aim is to ensure all people have access to healthier and more sustainable diets to eradicate all forms of malnutrition worldwide.[2]
Eating a healthy diet, along with getting enough physical activity and sleep, can help children grow up healthy and prevent overweight and obesity. In the United States, 19% of young people aged 2 to 19 years and 40% of adults have obesity, which can put them at risk for heart disease, type 2 diabetes, and some cancers. In addition, obesity costs the US health care system $147 billion a year[9].
Physiotherapy[edit | edit source]
In the various setting physiotherapists work in be aware of the signs of malnutrition eg in the older people; in pregnant women, in the immunocomprimised.
Poor nutritional status is associated with the onset of frailty. Screening and early diagnosis of malnutrition and frailty in elderly people will help to prevent the onset of disability. Effective treatment is based on correction of the macro- and micronutrient deficit and physical exercise[10]. Referral to appropriate health professionals when appropriate detected e dietician.
See also Child Health Conditions and Migration and Relevance of Nutrition in Physiotherapy
References[edit | edit source]
- ↑ Murphy J, Mayor A, Forde E. Identifying and treating older patients with malnutrition in primary care: the MUST screening tool. British Journal of General Practice. 2018 Jul 1;68(672):344-5.Available:https://bjgp.org/content/68/672/344 (accessed 30.8.2021)
- ↑ 2.0 2.1 2.2 WHO Malnutrition Available:https://www.who.int/news-room/q-a-detail/malnutrition (accessed 30.8.2021)
- ↑ Health Direct Malnutrition Available:https://www.healthdirect.gov.au/malnutrition (accessed 30.8.2021)
- ↑ 4.0 4.1 Kids Britannica Malnutrition Available:https://kids.britannica.com/kids/article/malnutrition/610143 (accessed 30.8.2021)
- ↑ Kellett J, Kyle G, Itsiopoulos C, Naunton M, Luff N. Malnutrition: the importance of identification, documentation, and coding in the acute care setting. Journal of nutrition and metabolism. 2016 Jan 1;2016. Available: https://www.hindawi.com/journals/jnme/2016/9026098/#discussion(Accessed 30.8.2021)
- ↑ Kondrup J, Sorensen JM. The magnitude of the problem of malnutrition in Europe. The Economic, Medical/Scientific and Regulatory Aspects of Clinical Nutrition Practice: What Impacts What?. 2009;12:1-4.Available:https://pubmed.ncbi.nlm.nih.gov/19858682/ (accessed 30.8.2021)
- ↑ WHO More than one in three low- and middle-income countries face both extremes of malnutrition Available:https://www.who.int/news/item/16-12-2019-more-than-one-in-three-low--and-middle-income-countries-face-both-extremes-of-malnutrition (accessed 31.8.2021)
- ↑ Naujokas MF, Anderson B, Ahsan H, Aposhian HV, Graziano JH, Thompson C, Suk WA. The broad scope of health effects from chronic arsenic exposure: update on a worldwide public health problem. Environmental health perspectives. 2013 Mar;121(3):295-302.Available: https://www.nature.com/articles/s41430-021-00945-y#Ack1(accessed 31.8.2021)
- ↑ CDC Malnutrition Available: https://www.cdc.gov/chronicdisease/resources/publications/factsheets/nutrition.htm(accessed 30.8.2021)
- ↑ Artaza-Artabe, I., Sáez-López, P., Sánchez-Hernández, N., Fernández-Gutierrez, N. and Malafarina, V., 2016. The relationship between nutrition and frailty: Effects of protein intake, nutritional supplementation, vitamin D and exercise on muscle metabolism in the elderly. A systematic review. Maturitas, 93, pp.89-99. Available: https://www.sciencedirect.com/science/article/abs/pii/S0378512216300810 (accessed 30.8.2021)