Anatomy of the Pelvic Girdle
Original Editor - Deborah Riczo, Wanda van Niekerk
Top Contributors - Wanda van Niekerk, Kim Jackson, Tarina van der Stockt, Lucinda hampton, Vidya Acharya and Olajumoke Ogunleye
Introduction[edit | edit source]
The term "pelvis" is used to identify the area between the abdomen and the lower extremities. It can be divided into the greater pelvis and the lesser pelvis.[1] The pelvis consists of the sacrum, the coccyx, the ischium, the ilium, and the pubis.[2][3] The structure of the pelvis supports the contents of the abdomen while also helping to transfer the weight from the spine to the lower limbs.[4] During gait, the joints within the pelvis work together to decrease the amount of force transferred from the ground and lower extremities to the spine and upper extremities.[4]
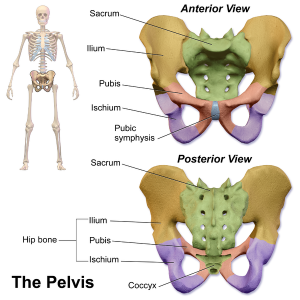
Osteology of the Pelvis[edit | edit source]
The pelvic bones are[1]:
- Sacrum
- Coccyx
- Two innominate bones, which consist of the:
- Ischium
- Ilium
- Pubis[2]
- The inlet to the pelvic canal is at the level of the sacral promontory and superior aspect of the pubic bones.
- The outlet is formed by the pubic arch, ischial spines, sacrotuberous ligaments, and the coccyx.
- The enclosed space between the inlet and outlet is called the true pelvis, with the plane of the inlet being at right angles to the plane of the outlet.
- The female true pelvis differs from the male in being shallower, having straighter sides, a wider angle between the pubic rami at the symphysis, and a proportionately larger pelvic outlet.
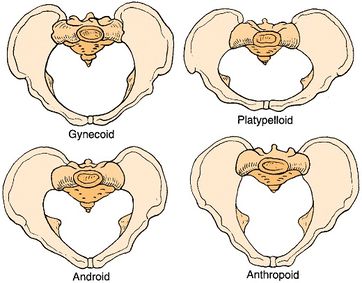
- The shape of the female bony pelvis can be classified into four broad categories: gynecoid, anthropoid, android, and platypelloid[3].
- Gynecoid/genuine pelvis
- the brim is round, wider, and both ischial spines are less prominent this allows easy baby delivery.
- Android pelvis
- like a heart-shaped brim with a narrow pelvic cavity than presented in gynecoid one, get narrower at the supra-pubic arch, and both ischial spines are prominent. During delivery, she needs to take an active role.
- Anthropoid pelvis
- oval brim, slightly narrower pelvic cavity than above with larger outlet diameter.
- Platypelloid pelvis
- shallow pelvic cavity, and decreased antero-posterior diameter, broad outlet, during labour there will be difficult for the baby to enter the pelvis at the beginning.
- Gynecoid/genuine pelvis
- In women, the pelvis houses the uterus, tubes, ovaries and vagina.
Joint Articulations[edit | edit source]
There are three articulations within the pelvis[7]:
- Inferiorly between the sacrum and the coccyx
- Posteriorly between the sacrum and each ilium (sacroiliac (SI) joint)
- Anteriorly between the pubic bodies (pubic symphysis)[3]
Other articulations:
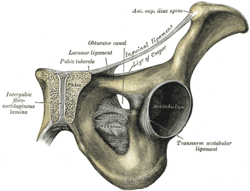
The pelvis and femur articulate via the acetabulum[2](hip joint)
Symphysis Pubis Joint[edit | edit source]
- non-synovial amphiarthrodial joint
- inter-pubic fibrocartilage disc
- less form closure than sacroiliac joint
Sacroiliac Joint[edit | edit source]
- diarthrodial joint[9][10]
- held together by fibrous capsule and synovial fluid[9]
- slightly moveable joint[9]
For more information on the sacroiliac joint, read this Physiopedia page: Sacroiliac Joint
Sacrococcygeal Joint[edit | edit source]
- at apex of sacrum and coccyx
- amphiarthrodial joint between the base of the coccyx (concave) and the sacral apex (convex)
- Synovium present occasionally
- sacrococcygeal disc present
- slightly moveable joint, but movement decreases with age
Ligaments of the Pelvis[edit | edit source]
Pubic Symphysis Ligaments[edit | edit source]
- Superior pubic ligament - runs between pubic tubercles[13]
- Inferior pubic ligament (aka arcuate pubic ligament) - runs between inferior pubic rami and blends with the fibrocartilaginous disc of the pubic symphysis[13]
- Anterior pubic ligament[13]
- Posterior pubic ligament - a membranous structure which blends with periosteum[13]
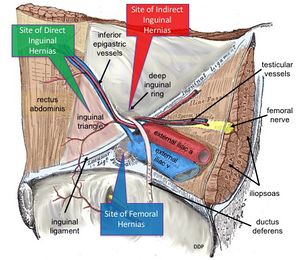
Inguinal Ligament[edit | edit source]
- runs from the ASIS to the pubic tubercle[14]
- formed by the aponeurosis of the external oblique
- continuous with fascia lata of the thigh
- Superficial inguinal ring:
- the exit of the inguinal canal
- inguinal nerve
- genitofemoral nerve
- spermatic cord (males)
- round ligament (females)
- palpable under normal conditions[15]
- dilated in athletic pubalgia
- inguinal hernia - abdominal contents may protrude through the ring
- the exit of the inguinal canal
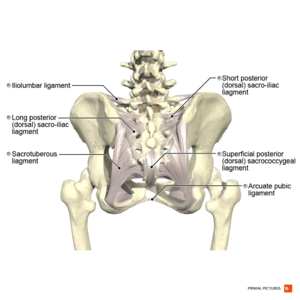
Ischio-sacral Ligaments[edit | edit source]
- Sacrotuberous Ligament
- from sacrum to tuberosity of the ischium[7]
- PSIS to the 4th and 5th transverse tubercle of the sacrum and the lateral inferior border of the sacrum and coccyx
- the free concave border is an attachment for obturator fascia
- directly continuous with the long head of biceps femoris
- the posterior surface of the ligament is also the origin of gluteus maximus
- Sacrospinous Ligament
Sacroiliac Ligaments[edit | edit source]
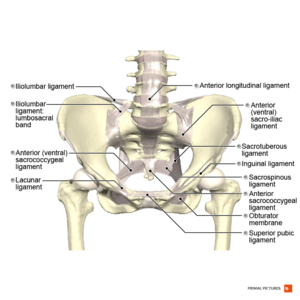
- Anterior/Ventral sacroiliac ligament[17]
- from the anterolateral aspect of the sacrum to the auricular surface of the ilium
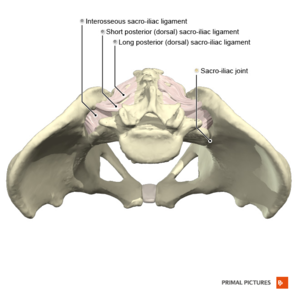
- Posterior/Dorsal sacroiliac ligament[17]
- The upper portion (short posterior sacroiliac ligament) - from 1st and 2nd transverse tubercles of the sacrum to the tuberosity of ilium
- The lower portion (long dorsal posterior sacroiliac ligament) - from 3rd transverse tubercle of the sacrum to the posterior superior iliac spine (PSIS)
- Interosseous sacroiliac ligament- lies deep to posterior SI ligament and runs between the tuberosities of the sacrum and ilium[17]
Iliolumbar Ligament[edit | edit source]
- from the tip of the transverse process of L5 to posterior aspect of the inner lip of iliac crest[7]
- 2 main bands attach to the pelvis
- Lower band - attaches to the base of sacrum, contiguous with anterior sacroiliac ligament
- Upper band - attaches to iliac crest anterior to the sacro-iliac articulation, contiguous with lumbodorsal fascia
- Supports the lumbosacral joint
- Anterior relationship with psoas major
- Posterior relationship with muscles in vertebral groove such a multifidus and erector spinae
- Superior relationship with quadratus lumborum
Lateral Lumbosacral Ligament[edit | edit source]
- partially continuous with the lower border of the iliolumbar ligament
- from the lower border of L5 transverse process to the ala of the sacrum[7]
- intermingles with anterior sacroiliac ligament
- consists of bundles of fibres of varying strength
Sacrococcygeal Ligaments[edit | edit source]
- Ventral/Anterior sacrococcygeal ligament[7]
- from the anterior surface of sacrum to the front of the coccyx; continuation of the anterior longitudinal ligament of the spine
- Dorsal sacrococcygeal ligament[7]
- Deep portion - from the inside sacral canal at the 5th sacral segment to the dorsal surface of the coccyx; continuation of the posterior longitudinal ligament of the spine
- Superficial portion - from free margin of sacral hiatus to dorsal surface of the coccyx; corresponds with the ligamentum flavum of the spine
- Lateral sacrococcygeal ligament
- from the inferior lateral angle of the sacrum to the transverse process of the 1st coccygeal vertebra
Muscles of the Pelvis[edit | edit source]
There are 36 muscles that attach to the sacrum or innominates. The purpose of these muscles is primarily to provide stability to the joint not to produce movement.[18]
Muscles that attach to the sacrum or innominates are:
Muscles of the Hip[edit | edit source]
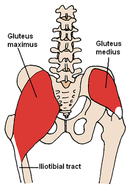
- Gluteus maximus
- the primary stabilising muscle of the sacroiliac joint[19]
- often inhibited in people with low back pain, pelvic girdle pain or sacroiliac joint dysfunction[19][20]
- Gluteus medius
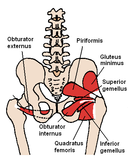
- Gluteus minimus
- Piriformis
- Superior gemellus
- Obturator Internus
- Inferior gemellus
- Quadratus femoris
- Iliopsoas
- composed of psoas major and iliacus[21]
- primarily hip flexor[21]
- may assist in anterior pelvic tilt[21]
- also functions as an external rotator of the hip[21]
- acts as a pelvic and hip stabiliser, especially during single-leg stance[21]
- important to consider iliopsoas during any pelvic rehabilitation[21]
Muscles of the Back[edit | edit source]
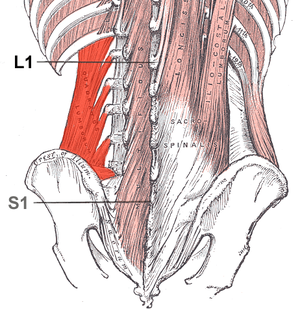
- Quadratus Lumborum - may play a role in functional scoliosis as a result of its attachments
- Multifidus
Muscles of the Abdomen and Groin[edit | edit source]
- Rectus Abdominis
- External and Internal Obliques
- Transverse Abdominis
- Relationship between abdominal muscles and adductor longus:
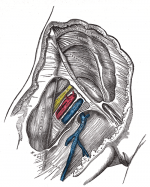
- Femoral Triangle
Muscles of the Abdominal Canister[edit | edit source]
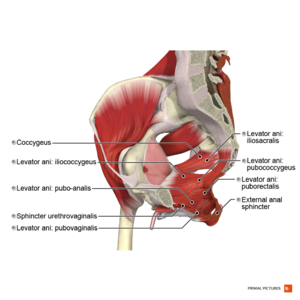
Pelvic Floor Myology[edit | edit source]
Layer One - Urogenital Triangle[27]
- Bulbocavernosus
- Ischiocavernosus
- Superficial transverse perineal
- External anal sphincter
Layer Two - Urogenital Diaphragm[27]
The urogenital diaphragm, also called the triangular ligament, is a strong, muscular membrane that occupies the area between the symphysis pubis and ischial tuberosities and stretches across the triangular anterior portion of the pelvic outlet. The urogenital diaphragm is external and inferior to the pelvic diaphragm.
- The urethral sphincter (sphincter urethrae)
- Compressor urethrae
- Sphincter urethral vaginalis
- Deep transverse perineal
- Perineal membrane
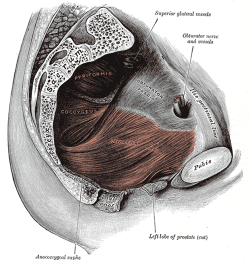
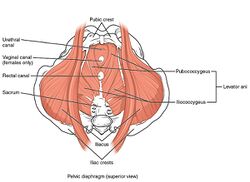
Layer Three - Pelvic Diaphragm[27]
The pelvic diaphragm is a wide but thin muscular layer of tissue that forms the inferior border of the abdominopelvic cavity. Composed of a broad, funnel-shaped sling of fascia and muscle, it extends from the symphysis pubis to the coccyx and from one lateral sidewall to the other.
- Levator Ani Muscle (pubococcygeus aka pubovisceral, pubovaginalis, puboanalis, puborectalis, iliococcygeus)
- Coccygeus
- Piriformis
- Obturator internus
- Arcus tendinous of the levator ani
- Arcus tendinous fasciae pelvis
Perineal Body[27] - a fibromuscular structure located between the vagina/testicles and the anus, attaching to the sides of the ischiopubis rami by the deep transverse perineal muscle. It is known as the central tendon of the pelvis because many pelvic floor structures intersect with the perineum at this structure.
For more information read this Physiopedia page on Pelvic Floor Anatomy
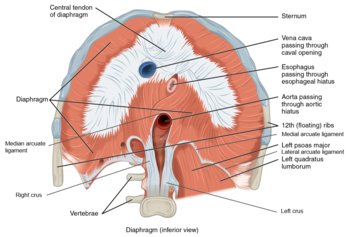
Diaphragm[edit | edit source]
- Contributes to the health of the pelvic girdle by "pistoning" motion in produces in abdominal "canister"
- Peripherally
- Attaches to 11th & 12th ribs and the costal cartilages 7 to 10, xiphoid process and lumbar vertebrae
- Centrally via R and L crura of the central tendon
- L1-3 intervertebral discs
- Physiological sphincter of the oesophagus
- The inferior surface of the pericardium
References[edit | edit source]
- ↑ 1.0 1.1 Madsen C, Gordon DA. Anatomy, Neuroanatomy, and Biomechanics of the Pelvis. InPelvic Floor Dysfunction and Pelvic Surgery in the Elderly 2017 (pp. 3-26). Springer, New York, NY.
- ↑ 2.0 2.1 2.2 White TD, Black MT, Folkens PA. Human osteology. Academic press; 2011.
- ↑ 3.0 3.1 3.2 Lewis CL, Laudicina NM, Khuu A, Loverro KL. The human pelvis: Variation in structure and function during gait. The Anatomical Record 2017;300(4):633-42.
- ↑ 4.0 4.1 Magee DJ. Orthopedic physical assessment. Elsevier Health Sciences; 2013.
- ↑ Anatomy Zone. Bones of the Pelvis. Available from: https://youtu.be/3v5AsAESg1Q [last accessed 07/11/2020]
- ↑ Kenhub Learn Human Anatomy. Bones of the Pelvis. Available from https://www.youtube.com/watch?v=yK-8ZwLFarc [last accessed 07/11/2020]
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 Chaudhry SR, Hulaibi FA, Nahian A, Chaudhry K. Anatomy, Abdomen and Pelvis, Pelvis. StatPearls [Internet]. 2020 May 24.
- ↑ 3D Anatomy Lyon. Arthrology of the pelvis the symphysis pubis. Available from https://www.youtube.com/watch?v=Jkw-X6zOLVI&list=PL5uEMr5n9RPGx9IX9mKc-aMe-KwJCndSj&index=8. (last accessed 14 November 2020)
- ↑ 9.0 9.1 9.2 Kiapour A, Joukar A, Elgafy H, Erbulut DU, Agarwal AK, Goel VK. Biomechanics of the sacroiliac joint: anatomy, function, biomechanics, sexual dimorphism, and causes of pain. International journal of spine surgery. 2020 Feb 1;14(s1):S3-13.
- ↑ Wong M, Kiel J. Anatomy, Abdomen and Pelvis, Sacroiliac Joint. InStatPearls [Internet] 2019 Feb 6. StatPearls Publishing.
- ↑ 3D Anatomy Lyon. Arthrology of the pelvis the sacroiliac joint. Available from https://www.youtube.com/watch?v=FTYnuXy0y1s&list=PL5uEMr5n9RPGx9IX9mKc-aMe-KwJCndSj&index=7 (last accessed 14 November 2020)
- ↑ 3D Anatomy Lyon. Arthrology of the pelvis The sacrococcygeal joint. (last accessed 14 November 2020)
- ↑ 13.0 13.1 13.2 13.3 Mahadevan V. Anatomy of the pelvis. Surgery (Oxford). 2018 Jul 1;36(7):333-8.
- ↑ Miller HJ. Inguinal hernia: mastering the anatomy. Surgical Clinics. 2018 Jun 1;98(3):607-21.
- ↑ Myers T. Fascial Palpation. Palpation and Assessment in Manual Therapy. 2017.
- ↑ Health and Medicine. Pelvis Anatomy Tutorial (Ligaments). Available from https://www.youtube.com/watch?v=pskEkYof95w&t=293s. (last accessed 14 November 2020)
- ↑ 17.0 17.1 17.2 Poilliot AJ, Zwirner J, Doyle T, Hammer N. A Systematic Review of the Normal Sacroiliac Joint Anatomy and Adjacent Tissues for Pain Physicians. Pain physician. 2019 Jul;22(4):E247-74.
- ↑ Calvillo O, Skaribas I, Turnipseed J. Anatomy and pathophysiology of the sacroiliac joint. Current review of pain 2000;4(5):356-61.
- ↑ 19.0 19.1 Buckthorpe M, Stride M, Della Villa F. Assessing and treating gluteus maximus weakness–a clinical commentary. International journal of sports physical therapy. 2019 Jul;14(4):655.
- ↑ Klahsen O. Sacroiliac joint pain: Where are we now?. SURG Journal. 2019 Jun 20;11.
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 Lifshitz L, Sela SB, Gal N, Martin R, Klar MF. Iliopsoas the Hidden Muscle: Anatomy, Diagnosis, and Treatment. Current Sports Medicine Reports. 2020 Jun 1;19(6):235-43.
- ↑ Animated Anatomy. Hip Muscles - Lateral Rotator Group & Gluteus Muscles. Available from https://www.youtube.com/watch?v=YohBVpLMZ6g. (last accessed 14 November 2020)
- ↑ KenHub Learn Human Anatomy. Iliopsoas Muscle: Action / Function, Anatomy & Innervation - Human Anatomy | Kenhub. Available from https://www.youtube.com/watch?v=cHWjpQ06-cE (last accessed 14 November 2o20)
- ↑ Poor AE, Roedl JB, Zoga AC, Meyers WC. Core muscle injuries in athletes. Current sports medicine reports. 2018 Feb 1;17(2):54-8.
- ↑ Riff AJ, Movassaghi K, Beck EC, Neal WH, Inoue N, Coleman SH, Nho SJ. Surface mapping of the musculotendinous attachments at the pubic symphysis in cadaveric specimens: implications for the treatment of core muscle injury. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2019 Aug 1;35(8):2358-64.
- ↑ 26.0 26.1 Moore KL, Dalley AF, Agur AMR. Clinial oriented anatomy. Philadelphia: Wolters Kluwer, 2010.
- ↑ 27.0 27.1 27.2 27.3 Eickmeyer SM. Anatomy and physiology of the pelvic floor. Physical Medicine and Rehabilitation Clinics. 2017 Aug 1;28(3):455-60.
- ↑ Mandy RoscherUnderstanding the Layers of the Pelvic Floor MusclesAvailable fromhttps://www.youtube.com/watch?v=G48NE8LdkSY&t=104sAccessed on 16/6/21