Synovial Fluid Analysis: Difference between revisions
No edit summary |
Kim Jackson (talk | contribs) m (Text replacement - "[[Medial meniscus" to "[[Medial Meniscus") |
||
| (20 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
<div class="editorbox"> '''Original Editor '''- [[User:Shwe Shwe U Marma|Shwe Shwe U Marma]] '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}}</div> | <div class="editorbox"> '''Original Editor '''- [[User:Shwe Shwe U Marma|Shwe Shwe U Marma]] '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}}<br> | ||
</div> | |||
== Introduction == | == Introduction == | ||
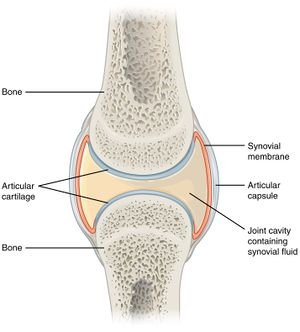
Synovial fluid or [[Joint Classification|joint]] fluid is physiologic collection of lubricant fluid within a joint space. It acts as source of nutrition for surrounding structures including [[cartilage]], [[Medial | [[Synovium & Synovial Fluid|Synovial fluid]] or [[Joint Classification|joint]] fluid is physiologic collection of lubricant fluid within a joint space. It acts as source of nutrition for surrounding structures including [[cartilage]], [[Medial Meniscus|meniscus]], [[Glenoid Labrum|labrum]] etc.<ref name=":0">Seidman AJ, Limaiem F. [https://europepmc.org/article/NBK/NBK537114 Synovial Fluid Analysis]. In: StatPearls. StatPearls Publishing, Treasure Island (FL); 2019.</ref>Synovial fluid is ultrafiltrate of blood [[Blood Physiology|plasma]] and is primarily composed of proteoglycans, lubricin, hyaluronan and phospholipids.<ref>Blewis ME, Nugent-Derfus GE, Schmidt TA, Schumacher BL, Sah RL. [https://pubmed.ncbi.nlm.nih.gov/17340555/ A model of synovial fluid lubricant composition in normal and injured joints]. Eur Cell Mater. 2007 Mar 6;13(1):26-39</ref>[[File:Synovial Joints.jpg|Synovial joint with synovial fluid|alt=|right|frameless]] | ||
== Purpose of Synovial Fluid Analysis == | == Purpose of Synovial Fluid Analysis == | ||
Physiologic changes in synovial fluid volume and content occur in response to trauma, inflammation, and bacterial, fungal, or viral penetrance. When patients present with acutely painful joints with suspicion of infection, inflammation or non-inflammatory causes of effusion, synovial fluid aspiration and analysis is imperative to aid in diagnosis and direct treatment modality.<ref name=":0" /> | Physiologic changes in synovial fluid volume and content occur in response to trauma, [[Inflammation Acute and Chronic|inflammation]], and [[Bacterial Infections|bacterial]], [[Fungal Diseases|fungal]], or [[Viral Infections|viral]] penetrance. When patients present with acutely painful joints with suspicion of infection, inflammation or non-inflammatory causes of effusion, synovial fluid aspiration and analysis is imperative to aid in diagnosis and direct treatment modality.<ref name=":0" /> | ||
One study guided by synovial fluid analysis found improvement in synovial fluid after isometric quadriceps exercise in patients with osteoarthritis.<ref>Miyaguchi M, Kobayashi A, Kadoya Y, Ohashi H, Yamano Y, Takaoka K. [https://www.sciencedirect.com/science/article/pii/S1063458402003722 Biochemical change in joint fluid after isometric quadriceps exercise for patients with osteoarthritis of the knee]. Osteoarthritis and cartilage. 2003 Apr 1;11(4):252-9.</ref>However, synovial fluid analysis is not done routinely but done to exclude other causes of inflammation such as infection.<ref>Ebnezer J. [https://www.amazon.com/Essentials-Orthopedics-Physiotherapists-John-Ebnezar/dp/9350251612 Essentials of Orthopaedics for Physiotherapists]. Delhi: Jaypee Brothers Medical Publishers (P) Ltd. 2003</ref> | |||
== Procedure == | == Procedure == | ||
For analysis, synovial fluid is collected by Arthrocentesis, the procedure to collect synovial fluid from joint by using a needle.<ref>Mackie JW. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2218651/ Joint aspiration: arthrocentesis]. Canadian Family Physician. 1987 Sep;33:2057.</ref> | |||
For analysis, synovial fluid is collected by Arthrocentesis, the procedure to collect synovial fluid from joint by using a needle.<ref>Mackie JW. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2218651/ Joint aspiration: arthrocentesis. Canadian Family Physician | |||
== Indications == | == Indications == | ||
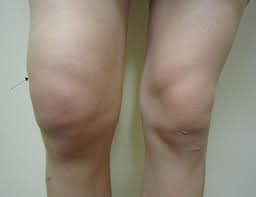
[[File:Joint swelling.jpg|Swollen right knee, an indication for synovial fluid analysis|thumb]] | [[File:Joint swelling.jpg|Swollen right knee, an indication for synovial fluid analysis|thumb]] | ||
| Line 20: | Line 18: | ||
* Acute trauma with painful effusion | * Acute trauma with painful effusion | ||
* A definitive diagnosis of [[gout]] or pseudogout | * A definitive diagnosis of [[gout]] or pseudogout | ||
* Effusions of unknown etiology | * Effusions of unknown etiology | ||
* | * Removing excess fluid can help relieve pain in the affected joint<ref name=":0" /> | ||
* | * Monitor known joint disorders.<ref>Courtney P, Doherty M. [https://www.sciencedirect.com/science/article/abs/pii/S1521694209000047 Joint aspiration and injection and synovial fluid analysis]. Best Practice & Research Clinical Rheumatology. 2009 Apr 1;23(2):161-92.</ref> | ||
== Potential Diagnosis == | == Potential Diagnosis == | ||
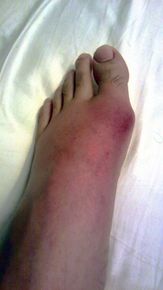
[[File:Gout | * '''Inflammatory arthritis including''' [[File:Gout.1st.MTP.Left.jpg|Swollen and erythemic left 1st metatarsophalangeal (MTP) joint due to gout|thumb|291x291px]] | ||
** Gout | ** Gout | ||
** Pseudogout, | ** Pseudogout, | ||
| Line 42: | Line 38: | ||
== Expected Values per Category == | == Expected Values per Category == | ||
{| class="wikitable" | {| class="wikitable" | ||
! | !Synovial fluid | ||
!Normal | !Normal | ||
!Non-inflammatory | !Non-inflammatory | ||
!Inflammatory | !Inflammatory | ||
! | !Septic | ||
|- | |- | ||
|'''Color''' | |'''Color''' | ||
|Clear | |Clear | ||
|Yellow | |Yellow | ||
|Yellow | |Yellow, opalescent | ||
|Yellow-green | |Yellow-green | ||
|- | |- | ||
| Line 57: | Line 53: | ||
|Transparent | |Transparent | ||
|Transparent | |Transparent | ||
| | |Translucent-opaque | ||
| | |Opaque | ||
|- | |- | ||
|'''Viscosity''' | |'''Viscosity''' | ||
|High | |High | ||
|High | |High | ||
|Low | |Low | ||
|Variable | |||
|- | |- | ||
|'''WBCs/ | |'''WBCs/mm<sup>3</sup>''' | ||
|<200 | |<200 | ||
| | |200-2000 | ||
| | |2000-10,000 | ||
|> | |>50,000 | ||
|- | |- | ||
|''' | |'''Polymorphonuclear leucocytes (PMNs)''' | ||
|<25% | |<25% | ||
|~25% | |||
|>50% | |>50% | ||
|>75% | |>75% | ||
|- | |- | ||
|''' | |'''Culture''' | ||
|Negative | |Negative | ||
|Negative | |Negative | ||
|Negative | |Negative | ||
| | |Often positive | ||
|- | |- | ||
|''' | |'''Glucose (mg/dL)''' | ||
| | |Nearly = to plasma | ||
| | |Nearly = to plasma | ||
| | |~25, lower than plasma | ||
| | |<25, even lower than plasma | ||
|} | |} | ||
<ref> | <ref>García-De La Torre I. [https://www.researchgate.net/publication/6680287_Advances_in_the_Management_of_Septic_Arthritis Advances in the management of septic arthritis]. Infectious Disease Clinics. 2006 Dec 1;20(4):773-88.</ref> | ||
== Differential Diagnosis == | == Differential Diagnosis == | ||
| Line 102: | Line 92: | ||
!Non-inflammatory | !Non-inflammatory | ||
!Inflammatory | !Inflammatory | ||
! | !Septic | ||
|- | |- | ||
|Osteoarthritis | |Osteoarthritis | ||
| Line 139: | Line 129: | ||
| | | | ||
|} | |} | ||
<ref>Faryna A, Goldenberg K. [https://www.ncbi.nlm.nih.gov/books/NBK274/ Joint fluid] | <ref>Faryna A, Goldenberg K. [https://www.ncbi.nlm.nih.gov/books/NBK274/ Joint Fluid]. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. Boston: Butterworths; 1990. p773-76.</ref> | ||
{{#ev:youtube|whpB4VkpxM0}} <ref>Medicosis Perfectionalis. Rheumatology...Joint fluid analysis (Pathology). Available from: https://www.youtube.com/watch?v=whpB4VkpxM0 [last accessed 18 September 2020]</ref> | |||
== Interfering Factors == | == Interfering Factors == | ||
| Line 155: | Line 146: | ||
* Skin reaction to antiseptics or soft bandage adhesive | * Skin reaction to antiseptics or soft bandage adhesive | ||
* Reaccumulation of the joint effusion<ref name=":0" /> | * Reaccumulation of the joint effusion<ref name=":0" /> | ||
== Conclusion == | == Conclusion == | ||
Synovial fluid analysis is an important diagnostic test to confirm several diseases of joints. It can be done to know existing condition of a joint so that appropriate physiotherapy management can be delivered. | Synovial fluid analysis is an important diagnostic test to confirm several diseases of joints. It can be done to know existing condition of a joint so that appropriate physiotherapy management can be delivered. | ||
<div class="row"> | <div class="row"> | ||
== References == | == References == | ||
| Line 170: | Line 154: | ||
<references /> | <references /> | ||
[[Category:Joints]] | [[Category:Joints]] | ||
[[Category:Physiology]] | |||
[[Category:Anatomy]] | |||
Latest revision as of 11:04, 22 January 2024
Introduction[edit | edit source]
Synovial fluid or joint fluid is physiologic collection of lubricant fluid within a joint space. It acts as source of nutrition for surrounding structures including cartilage, meniscus, labrum etc.[1]Synovial fluid is ultrafiltrate of blood plasma and is primarily composed of proteoglycans, lubricin, hyaluronan and phospholipids.[2]
Purpose of Synovial Fluid Analysis[edit | edit source]
Physiologic changes in synovial fluid volume and content occur in response to trauma, inflammation, and bacterial, fungal, or viral penetrance. When patients present with acutely painful joints with suspicion of infection, inflammation or non-inflammatory causes of effusion, synovial fluid aspiration and analysis is imperative to aid in diagnosis and direct treatment modality.[1]
One study guided by synovial fluid analysis found improvement in synovial fluid after isometric quadriceps exercise in patients with osteoarthritis.[3]However, synovial fluid analysis is not done routinely but done to exclude other causes of inflammation such as infection.[4]
Procedure[edit | edit source]
For analysis, synovial fluid is collected by Arthrocentesis, the procedure to collect synovial fluid from joint by using a needle.[5]
Indications[edit | edit source]
- Presentation of acute painful joint with surrounding warmth/erythema
- Suspicion of septic arthritis
- Suspicion for subacute or chronic periprosthetic joint infection
- Acute exacerbation of chronic knee pain from osteoarthritis or non-inflammatory arthritis, or
- Acute trauma with painful effusion
- A definitive diagnosis of gout or pseudogout
- Effusions of unknown etiology
- Removing excess fluid can help relieve pain in the affected joint[1]
- Monitor known joint disorders.[6]
Potential Diagnosis[edit | edit source]
- Inflammatory arthritis including
- Gout
- Pseudogout,
- Infection
- Spondyloarthritis
- Non-inflammatory arthritis which can include effusion from osteoarthritis or meniscal tears
- Septic arthropathy
- Acute septic arthropathy
- Subacute or chronic septic arthropathy
- Periprosthetic joint infection
- Hemorrhagic
- Traumatic, often seen with tendon, meniscal or ligament injury[1]
Expected Values per Category[edit | edit source]
| Synovial fluid | Normal | Non-inflammatory | Inflammatory | Septic |
|---|---|---|---|---|
| Color | Clear | Yellow | Yellow, opalescent | Yellow-green |
| Clarity | Transparent | Transparent | Translucent-opaque | Opaque |
| Viscosity | High | High | Low | Variable |
| WBCs/mm3 | <200 | 200-2000 | 2000-10,000 | >50,000 |
| Polymorphonuclear leucocytes (PMNs) | <25% | ~25% | >50% | >75% |
| Culture | Negative | Negative | Negative | Often positive |
| Glucose (mg/dL) | Nearly = to plasma | Nearly = to plasma | ~25, lower than plasma | <25, even lower than plasma |
Differential Diagnosis[edit | edit source]
| Non-inflammatory | Inflammatory | Septic |
|---|---|---|
| Osteoarthritis | Rheumatoid arthritis | Bacterial infection |
| Trauma | Crystal synovitis | Rheumatoid arthritis |
| Avascular necrosis | Spondyloarthropathy | Crystal synovitis |
| Systemic lupus | Reactive arthritis | |
| Acute rheumatic fever | Connective tissue disorders | |
| Endocrine arthropathy | Acute rheumatic fever
Viral infection Fungal infection Bacterial infection |
Interfering Factors[edit | edit source]
Several factors can interfere with aspiration and therefore analysis of synovial fluid.
- Unsuccessful aspiration is common as synovium can clog the needle and interfere with sample collection
- Non-sterile technique can contaminate the collected fluid.
- It is important to remember that multiple etiologies can co-exist, i.e., the presence of gout does not rule out the presence of concomitant infection.[1]
Complications[edit | edit source]
Potential complications include:
- Seeding a cutaneous infection within the joint
- Cartilage damage from needle insertion (rare)
- Pain at arthrocentesis site or local ecchymosis
- Bleeding and iatrogenic hemarthrosis
- Skin reaction to antiseptics or soft bandage adhesive
- Reaccumulation of the joint effusion[1]
Conclusion[edit | edit source]
Synovial fluid analysis is an important diagnostic test to confirm several diseases of joints. It can be done to know existing condition of a joint so that appropriate physiotherapy management can be delivered.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Seidman AJ, Limaiem F. Synovial Fluid Analysis. In: StatPearls. StatPearls Publishing, Treasure Island (FL); 2019.
- ↑ Blewis ME, Nugent-Derfus GE, Schmidt TA, Schumacher BL, Sah RL. A model of synovial fluid lubricant composition in normal and injured joints. Eur Cell Mater. 2007 Mar 6;13(1):26-39
- ↑ Miyaguchi M, Kobayashi A, Kadoya Y, Ohashi H, Yamano Y, Takaoka K. Biochemical change in joint fluid after isometric quadriceps exercise for patients with osteoarthritis of the knee. Osteoarthritis and cartilage. 2003 Apr 1;11(4):252-9.
- ↑ Ebnezer J. Essentials of Orthopaedics for Physiotherapists. Delhi: Jaypee Brothers Medical Publishers (P) Ltd. 2003
- ↑ Mackie JW. Joint aspiration: arthrocentesis. Canadian Family Physician. 1987 Sep;33:2057.
- ↑ Courtney P, Doherty M. Joint aspiration and injection and synovial fluid analysis. Best Practice & Research Clinical Rheumatology. 2009 Apr 1;23(2):161-92.
- ↑ García-De La Torre I. Advances in the management of septic arthritis. Infectious Disease Clinics. 2006 Dec 1;20(4):773-88.
- ↑ Faryna A, Goldenberg K. Joint Fluid. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. Boston: Butterworths; 1990. p773-76.
- ↑ Medicosis Perfectionalis. Rheumatology...Joint fluid analysis (Pathology). Available from: https://www.youtube.com/watch?v=whpB4VkpxM0 [last accessed 18 September 2020]