Brain Metastasis
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
Brain metastases are a common complication of cancer and the most common type of brain tumor (10% to 26% of patients who die from their cancer will develop brain metastases). While few cancers that metastasize to the brain can be cured using conventional therapies, long-term survival and palliation are possible with minimal adverse effects to patients.[1]
- Brain metastasis are associated with poor survival outcomes and pose distinct clinical challenges[2].
- The term brain technically includes the cerebrum, the cerebellum and the brainstem. As the cerebrum corresponds to the majority of the brain volume and thus receives most of its blood supply, it is more common for metastatic lesions to appear in the cerebral parenchyma.[3]
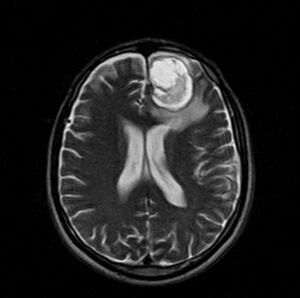
Image 1: Pancoast Tumour with cystic cerebral metastasis.
Etiology[edit | edit source]
The true incidence of brain metastases is unknown, but recent estimates are as high as 200,000 cases per year in the United States alone. Five primary tumours account for 80% of brain metastases:
- Lung cancer
- Renal cell carcinoma
- Breast cancer
- Melanoma
- Gastrointestinal tract adenocarcinomas (the majority colorectal carcinoma)
Other malignancies such as prostate and head and neck cancers rarely result in brain metastases. It can be difficult to predict which patients will develop brain metastases other than by using tumor type and subtype[1].
Parenchymal blood flow is an important determinant of the distribution of metastases: 80% of metastases localise to the cerebral hemispheres, 15% localise to the cerebellum, and 3% localise to the basal ganglia. [3]
Epidemiology[edit | edit source]
Brain metastases are the most common type of intracranial tumor. The incidence of brain metastases is increasingly likely as a result of several factors: patients with a systemic metastatic disease have a longer survival due to new systemic therapies (including immunotherapy); the use of sensitive magnetic resonance imaging (MRI) techniques with better detection of small asymptomatic brain metastases[1].
Brain metastasis continues to be a devastating complication of systemic malignancy, affecting approximately 20% of all patients suffering from cancer. Despite being a major source of morbidity and mortality for this patient population, a nationwide, systematic mechanism for reporting of brain metastases does not exist.[4]
Pathophysiology[edit | edit source]
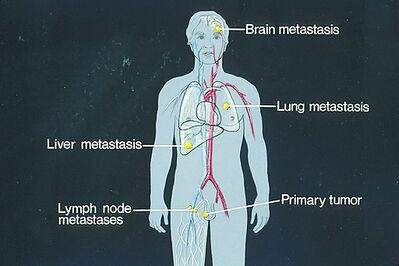
Metastatic cancer
- Passes through the bloodstream
- Enters the central nervous system through a breakdown of the blood-brain barrier.
- Clonal cells then proliferate, causing local invasion, displacement, inflammation, and edema.
Distribution throughout the central nervous system is more common in areas of high blood flow.[1]
Macroscopic appearance: Typically metastases are relatively well-demarcated from the surrounding parenchyma, and usually, there is a zone of peritumoural oedema out of proportion with the tumour size.[3]
Clinical presentation[edit | edit source]
The symptoms of brain metastases depend on where in the brain the tumor forms, the tumor’s size, and how fast the tumor spreads. Cancer treatment can also cause symptoms and side effects.
Patients commonly present with
- Physical symptoms. These can include headaches, seizures, mental status alterations, ataxia, nausea and vomiting, visual disturbances, muscle weakness and bowel and bladder problems.
- Cognitive symptoms. Can include personality changes, confusion, impaired judgment, memory loss, and socially inappropriate behavior.
- Emotional symptoms. Coping with a brain tumor or brain metastases can be very stressful, causing depression, anxiety, anger, and other emotional changes.[5]
In patients with known malignancies, the brain can sometimes act as a reservoir for metastatic disease (traditional chemotherapy regimes can have poor permeability through the blood-brain barrier) leading to presentation with cerebral metastases, even when in remission[3].
Treatment[edit | edit source]
Most of these patients are frail and have a reduced life expectancy, so the need for aggressive measures is not warranted. A team approach should discuss the best approach taking into account patient status, comorbidity, and life span. Many of these patients simply benefit from palliation and pain control[1]
Options to treat/relieve symptoms may include:
- Medications, such as corticosteroids (lower oedema in the brain), anti-seizure drugs, and pain medicine
- Assistive devices eg wheelchairs, canes, and walkers
- Emotional support, such as counseling
- Rehabilitation eg problem-solving therapy, speech and language therapy, and physical therapy
- Eating healthy[5]
Physiotherapy[edit | edit source]
There are a wide range of physical and psychological symptoms associated with brain metastases. Regardless of the stage of cancer, exercise has been found to improve quality of life for cancer patients including reducing and prevent future health complications and disability which can positively improve an individual’s body image and ability to return to work. Physiotherapists are experts in finding the best ways for cancer patients to be active; this may involve exercise programmes or advice on everyday activities.
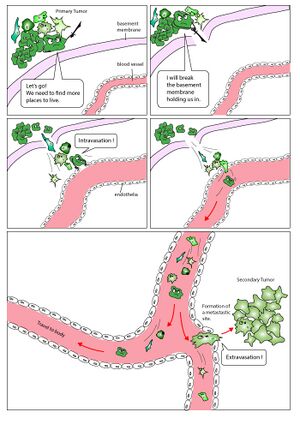
Recent findings: Physical activity regulates the levels of metastatic factors in each of the five steps of the process.
- Moderate intensity exercise appears to prevent tumor spread around the body, among others, by normalizing angiogenesis, destroying circulating tumor cells, and decreasing endothelial cells permeability.
- Contrarily, high-intensity exercise seems to favor cancer dissemination, likely through excessive stress, which can be somewhat counteracted by an appropriate warm-up.[6]
- It is appropriate to promote those with brain cancer to be as physically active as possible. The need or ability of those with brain cancer to meet current PA guidelines promoted to all people with cancer remains unclear.[7]
Other techniques include: breathing exercises, massage, meditation, acupuncture, tai chi
For more guidance see below links
New Directions[edit | edit source]
Brain metastases used to be regarded as the terminal stage of cancer and left life expectancy to only 1 month. The application of whole brain radiotherapy for patients with brain metastases increased the life expectancy to 4–6 months in the 1980s.
- With the development of stereotactic radiosurgery, stereotactic radiosurgery plus whole brain radiotherapy provides an alternative modality, with superior mental functioning outcomes, at the cost of overall survival.
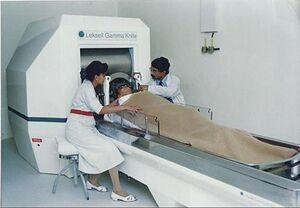
- Stereotactic radiosurgery combined with whole brain radiotherapy may offer a promising modality for patients with numerous multiple brain metastases who are not eligible for surgical resection. Image 8: Dr. B. K. Misra performing Stereotactic Gamma Knife Radiosurgery
- With the advancing understanding of molecular pathway and biological behavior of oncogenesis and tumor metastasis, novel targeted therapy including tyrosine-kinase inhibitors and immunotherapy are applied to brain metastases. Clinical trials have revealed the efficacy of targeted therapy[8].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Mark J. Amsbaugh; Catherine S. Kim. June 30, 2020. Brain Metastasis Available: https://www.ncbi.nlm.nih.gov/books/NBK470246/ (accessed 23.6.2021)
- ↑ Boire A, Brastianos PK, Garzia L, Valiente M. Brain metastasis. Nat Rev Cancer. 2020 Jan;20(1):4-11. doi: 10.1038/s41568-019-0220-y. Available:https://pubmed.ncbi.nlm.nih.gov/31780784/ (accessed 23.6.2021)
- ↑ 3.0 3.1 3.2 3.3 Radiopedia Brain metastases Available: https://radiopaedia.org/articles/brain-metastases (accessed 23.6.2021)
- ↑ Sacks P, Rahman M. Epidemiology of Brain Metastases. Neurosurg Clin N Am. 2020 Oct;31(4):481-488. Available:https://pubmed.ncbi.nlm.nih.gov/32921345/ (accessed 23.6.2021)
- ↑ 5.0 5.1 Cancer net Caring for a person with brain mets Available from: https://www.cancer.net/coping-with-cancer/caring-loved-one/caring-person-with-brain-tumor-or-metastatic-brain-cancer(accessed 24.6.2021)
- ↑ van Doorslaer de Ten Ryen S, Deldicque L. The regulation of the metastatic cascade by physical activity: A narrative review. Cancers. 2020 Jan;12(1):153.Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7017263/ (accessed 24.6.2021)
- ↑ Sandler CX, Matsuyama M, Jones TL, Bashford J, Langbecker D, Hayes SC. Physical activity and exercise in adults diagnosed with primary brain cancer: a systematic review. Journal of neuro-oncology. 2021 Apr 28:1-4.Available: https://link.springer.com/article/10.1007/s11060-021-03745-3(accessed 24.6.2021)
- ↑ Liu Q, Tong X, Wang J. Management of brain metastases: history and the present. Chinese Neurosurgical Journal. 2019 Dec;5(1):1-8. Available: https://cnjournal.biomedcentral.com/articles/10.1186/s41016-018-0149-0#Abs1(accessed 24.6.2021)