Functional Anatomy of the Cervical Spine: Difference between revisions
No edit summary |
mNo edit summary |
||
| Line 261: | Line 261: | ||
* [[Erector Spinae|<small>Erector spinae</small>]] | * [[Erector Spinae|<small>Erector spinae</small>]] | ||
* <small>[[Rectus Capitis Posterior|Rectus capitis posterior,]] [[Rectus Capitis Posterior Major|major]] and [[Rectus Capitis Posterior Minor|minor]] (head only)</small> | * <small>[[Rectus Capitis Posterior|Rectus capitis posterior,]] [[Rectus Capitis Posterior Major|major]] and [[Rectus Capitis Posterior Minor|minor]] (head only)</small> | ||
* Sternocleidomastoid | * <small>Sternocleidomastoid</small> | ||
* <small>longissimus capitis</small> | |||
* <small>spinalis capitis</small> | |||
| | | | ||
* <small>Scalene anterior, medius and posterior</small> | * <small>Scalene anterior, medius and posterior</small> | ||
| Line 269: | Line 271: | ||
* <small>Erector spinae</small> | * <small>Erector spinae</small> | ||
* <small>[[Rectus Capitis Lateralis|Rectus capitis lateralis]] (head only)</small> | * <small>[[Rectus Capitis Lateralis|Rectus capitis lateralis]] (head only)</small> | ||
* <small>spinalis capitis</small> | |||
| | | | ||
* [[Semispinalis Cervicis|<small>Semispinalis cervicis</small>]] | * [[Semispinalis Cervicis|<small>Semispinalis cervicis</small>]] | ||
| Line 277: | Line 280: | ||
* <small>Inferior oblique (head only)</small> | * <small>Inferior oblique (head only)</small> | ||
* <small>Rectus captitis posterior major (head only)</small> | * <small>Rectus captitis posterior major (head only)</small> | ||
* <small>longissius capitis</small> | |||
* <small>spinalis capitis</small> | |||
|} | |} | ||
<ref>Palastanga, N., & Soames, R. (2012). Anatomy and human movement (6th ed.). Edinburgh: Churchill Livingstone.</ref> | <ref>Palastanga, N., & Soames, R. (2012). Anatomy and human movement (6th ed.). Edinburgh: Churchill Livingstone.</ref> | ||
Revision as of 13:36, 26 July 2023
Top Contributors - Robin Tacchetti, Jess Bell, Kim Jackson, Tarina van der Stockt, Vidya Acharya and Ewa Jaraczewska
Introduction[edit | edit source]
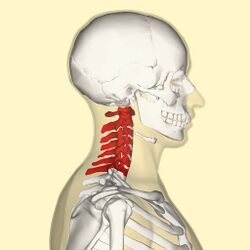
The cervical spine supports the weight of the head and enables head and neck movement.[1] [2] Intervertebral discs maintain the spaces between the vertebrae. These discs act like shock absorbers throughout the spinal column to cushion the bones as the body moves. Ligaments hold the vertebrae in place, and tendons attach the muscles to the spinal column. The cervical spine is subjected to a range of extrinsic factors such as repetitive movements, whole-body vibrations and static load.[3]
Key Terms[edit | edit source]
Axes: lines around which an object rotates. The rotation axis is a line that passes through the centre of mass. There are three axes of rotation: sagittal passing from posterior to anterior, frontal passing from left to right, and vertical passing from inferior to superior. The rotation axes of the foot joints are perpendicular to the cardinal planes. Therefore, motion at these joints results in rotations within three planes. Example: supination involves inversion, internal rotation, and plantarflexion.
Bursae: reduce friction between the moving parts of the body joints. A bursa is a fluid-filled sac. There are four types of bursae: adventitious, subcutaneous, synovial, and sub-muscular.
Capsule: one of the characteristics of the synovial joints. It is a fibrous connective tissue which forms a band that seals the joint space, provides passive and active stability and may even form articular surfaces for the joint. The capsular pattern is "the proportional motion restriction in range of motion during passive exercises due to tightness of the joint capsule."
Closed pack position: the position with the most congruency of the joint surfaces. In this position, joint stability increases. For example, the closed pack position for the interphalangeal joints is full extension.
Degrees of freedom: the direction of joint movement or rotation; there is a maximum of six degrees of freedom, including three translations and three rotations.
Ligament: fibrous connective tissue that holds the bones together.
Open (loose) pack position: position with the least joint congruency where joint stability is reduced.
Planes of movement: describe how the body moves. Up and down movements (flexion/extension) occur in the sagittal plane. Sideway movements (abduction/adduction) occur in the frontal plane. The transverse plane movements are rotational (internal and external rotation).
Cervical Spine Structure[edit | edit source]
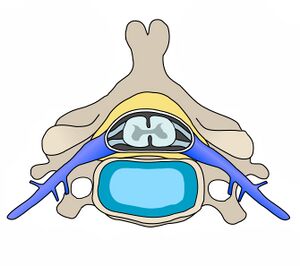
Cervical Vertebrae[edit | edit source]
There are seven cervical vertebrae, which are known as C1-C7. Their role is to support the head and neck and to promote head movement. The cervical spine is only exposed to small weight-bearing loads. Therefore, the cervical vertebral bodies do not need to be large and "an increased range of motion takes priority over vertebral size and rigidity".[2] However, because of this increased range of motion at the cervical spine, there is a heightened injury risk for the spinal cord and the associated neurovascular structures.[2]
The seven vertebral bodies have unique characteristics:[2][4]
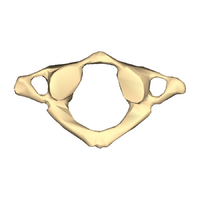
Atlas (C1)
- no vertebral body
- no spinous process
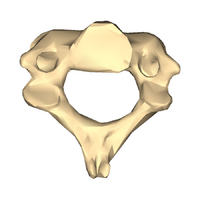
Axis (C2)
- odontoid process (dens) extends superiorly from the anterior portion of the vertebra
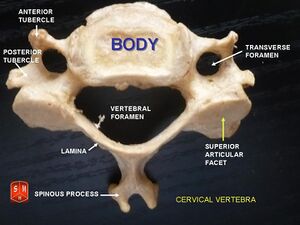
C3-C6
- triangular vertebral foramen
- bifid spinous process
- transverse foramina (space for nerves and vasculature)
C7
- singular spinous process
- larger spinous process
**In supine, it may be difficult to palpate the spinous process of C3-C6 in individuals with normal cervical lordosis.
Intervertebral Discs (IVD)[edit | edit source]
The intervertebral discs make up 25% of the height of the entire spine. However, in the cervical region, they make up 40% of the height. This increased height relative to vertebral body height provides a mobility advantage.[5]
The nucleus pulposus of the cervical discs is gelatinous in children and young people. However, it dries out by the age of 30 years and becomes a firm, fibrocartilaginous plate.[6]
The following are characteristics of the cervical spine intervertebral discs:
- thicker anteriorly than posteriorly
- concave superior surface
- convex inferior surface
- movement limited by the uncinate process
- anteroposterior translation does occur
** Due to the location of the uncinate process, posterolateral disc herniations are less frequent.
Cervical Lordosis[edit | edit source]
Typically, the cervical spine has a lordotic curvature. A lordotic posture can resist large compressive loads. It also helps to decrease stress on vertebral end plates. Compressive loads are distributed differently in the cervical spine than in the thoracic and lumbar spine. In the cervical spine, the anterior column absorbs 36% of the load, and the posterior facet (zygapophyseal) joints absorb 64%.[7]
Kinematics and Joints of the Cervical Spine[edit | edit source]
Kinematics[edit | edit source]
The cervical spine is the most mobile part of the vertebral column.
Flexion range of motion is usually around 40 degrees, and extension is around 50 degrees. The largest contributors to flexion/extension are:
- C4/C5 and C5/C6 in sitting
- C6/C7 in supine
C7/T1 contributes the least to flexion/extension.
Lateral flexion range of motion is normally close to 30 degrees. C3/C4 and C6/C7 allow for the most movement in this plane of motion.
Cervical rotation range of motion is usually close to 70 degrees. Flexibility in this plane is mainly achieved through the C1/C2 segment.[8]
| Joint | Location/Articulations | Function | Orientation/Composition |
|---|---|---|---|
| Intervertebral Disc Joint |
|
|
|
| Facet (Zygapophyseal) Joints |
|
|
|
| Uncovertebral Joint |
|
|
|
| Atlanto-Axial Joint |
|
|
|
| Atlanto-Occipital Joint |
|
|
|
Spinal Ligaments[edit | edit source]
Ligaments present throughout the entire vertebral column:
- Anterior longitudinal ligament: anterior surface of the vertebral bodies; limits extension of the spine
- Posterior longitudinal ligament: posterior surface of the vertebral bodies; limits flexion of the spine
- Ligamentum flavum: connects the laminae of each vertebrae; series of short ligaments
- Intertransverse ligament: a series of short ligaments that connect the laminae of each vertebrae; preserves upright posture and prevents hyperflexion of the spine[10]
| Ligament | Origin | Insertion | Role/Function |
|---|---|---|---|
| Nuchal ligament | Occiput | Tips of the spinous process from C1-C7 | Limits hyperflexion |
| Transverse ligament | Attaches to lateral masses of atlas | Anchors dens in place | |
| Apical ligament | Dens of the axis | Foramen magnum | Connects the dens of the axis to the foramen magnum
Stabilises the skull on the spine |
| Alar ligament | Dens of the axis | Occiput | Connects the dens of the axis to the occiput
Limits atlanto-axial rotation |
| Cruciform or cruciate ligament
1. Superior longitudinal band 2. Inferior longitudinal band 3. Transverse band |
|
|
Holds dens in place |
** ligaments in spinal column
Muscles of the Cervical Spine[edit | edit source]
The muscles of the cervical spine can be divided by location or by function.
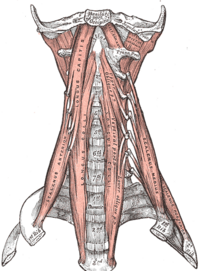
Anterior (Prevertebral) Vertebral Muscles[edit | edit source]
- Rectus capitis anterior
- Rectus capitis lateralis
- Longus capitis
- Longus colli/ Longus cervicis (3 portions: superior oblique, inferior oblique, vertical)
These muscles are also known as the deep cervical (neck) flexors.
Lateral Vertebral Muscles[edit | edit source]
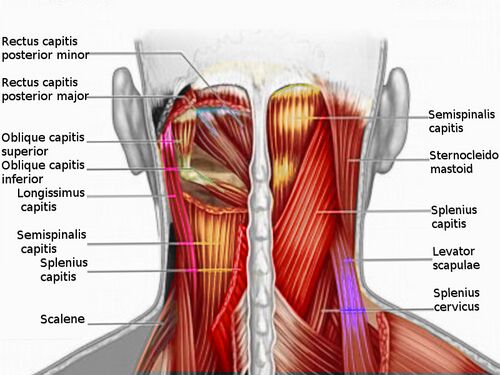
Posterior Vertebral Muscles[edit | edit source]
These can be further divided into intrinsic and extrinsic muscles.
Extrinsic muscles[edit | edit source]
Intrinsic muscles[edit | edit source]
- Superficial muscles :
- Deep muscles:
- suboccipital group
- transversospinalis muscles
- semispinalis capitis
- semispinalis cervicis
- rotatores cervicis
- multifidus (these are also known as deep neck extensors)
- interspinales and intertransversarii
Movement[edit | edit source]
| Motion | Flexion | Extension | Lateral Flexion | Rotation |
|---|---|---|---|---|
| Muscles |
|
|
|
The following tables identify the origin, insertion, innervation and action of key cervical muscles. Muscles with multiple functions are repeated in the relevant tables.
Cervical Spine Flexors[edit | edit source]
| Muscle | Origin | Insertion | Innervation | Action |
|---|---|---|---|---|
| Rectus capitis anterior | Lateral mass and transverse process of atlas (C1) | Basilar part of occipital bone | Anterior rami of 1st and 2nd cervical spinal nerves (C1, C2) |
|
| Longus colli | Transverse processes of C3-C5 and the vertebral bodies of C5-T3 | Anterior tubercle of C1, the vertebral bodies of C2-C4, and the transverse processes of C5 and C6. | Anterior rami of the 2nd to 6th cervical spinal nerves (C2-C6) |
|
| Longus capitis | Transverse processes of C3-C6 | Occipital bone | Anterior rami of 1st to 3rd cervical spinal nerves (C1-C3) |
|
| Anterior scalene | Transverse processes of C3-C6 | First rib | Anterior rami of 4th to 6th cervical spinal nerves (C4-C6) |
|
| Sternocleidomastoid | Manubrium and the medial portion of the clavicle | Mastoid process of the temporal bone | Accessory nerve (CN XI), branches of cervical plexus (C2-C3) |
|
| Rectus capitis lateralis | Transverse process of atlas (C1) | Jugular process of occipital bone | Anterior rami of 1st and 2nd cervical spinal nerves (C1-C2) |
|
Cervical Spine Extensors[edit | edit source]
| Muscle | Origin | Insertion | Innervation | Action |
|---|---|---|---|---|
| Obliquus capitis superior | Transverse process of the atlas | Occipital bone | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Obliquus capitis inferior | Spinous process of the axis | Tansverse process of atlas | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Rectus capitis posterior major | Spinous process of C2 | Occipital bone | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Rectus capitis posterior minor | Posterior tubercle of the atlas | Occipital bone | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Iliocostal cervicis | Ribs 3-6 | Transverse process of C4-C6 | Dorsal rami of the upper thoracic and lower cervical spinal nerves |
|
| Trapezius | Occipital bone, nuchal ligament and spinous process C7-T12 | Lateral third of the clavicle, acromian and spine of the scapula | Spinal root of accessory nerve (CN XI) (motor)
Cervical nerves (C3 and C4) (pain and proprioception) |
|
| Splenius cervicis | Spinous process of T3-T6 | Transverse process of C1-C3 | Dorsal rami of cervical spinal nerves (C5-C8) |
|
| Splenius capitis | Spinous process of C7-T3 and nuchal ligament | Occipital bone | Posterior rami of the 2nd and 3rd cervical spinal nerves |
|
** The transversospinal muscles (rotatores, multifidus, semispinalis) are the deep muscle of the spine. They attach between the transverse and spinous process of the vertebrae. They stabilise and extend the spine. The rotatores also provide rotation.
Cervical Spine Lateral Flexors[edit | edit source]
| Muscle | Origin | Insertion | Innervation | Action |
|---|---|---|---|---|
| Splenius cervicis | Spinous process of T3-T6 | Transverse process C1-C3 | Dorsal rami of cervical spinal nerves (C5-C8) |
|
| Splenius capitis | Spinous process of C7-T3 and nuchal ligament | Occipital bone | Posterior rami of the 2nd and 3rd cervical spinal nerves |
|
| Sternocleidomastoid | Manubrium and the medial portion of the clavicle | Mastoid process of the temporal bone | Accessory nerve (CN XI), branches of cervical plexus (C2-C3) |
|
| Anterior scalene | Transverse processes of C3-C6 | First rib | Anterior rami of 4th to 6th cervical spinal nerves (C4-C6) |
|
| Middle scalene | Posterior tubercles of the transverse processes of C1-C7 | Scalene tubercle of the first rib | Anterior rami of C3-C8 |
|
| Posterior scalene | Posterior tubercles of the transverse processes of C4-C6 | 2nd rib | Anterior rami of C6-C8 |
|
| Trapezius | Occipital bone, nuchal ligament and spinous process C7-T12 | Lateral third of the clavicle, the acromian and the spine of s scapula | Spinal root of accessory nerve (CN XI) (motor)
Cervical nerves (C3 and C4) (pain and proprioception) |
|
| Rectus capitis lateralis | Superior surface of the transverse process of atlas | Inferior surface of the jugular process of the occipital bone | Anterior rami of C1-C2 spinal nerves |
|
Cervical Spine Rotators[edit | edit source]
| Muscle | Origin | Insertion | Innervation | Action |
|---|---|---|---|---|
| Rectus capitis posterior major | Spinous process of C2 | Occipital bone | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Rectus capitis posterior major | Spinous process of C2 | Occipital bone | Suboccipital nerve (posterior ramus of 1st cervical spinal nerve (C1)) |
|
| Sternocleidomastoid | Manubrium and the medial portion of the clavicle | Mastoid process of the temporal bone | Accessory nerve (CN XI), branches of cervical plexus (C2-C3) |
|
| Splenius capitis | Spinous process ofC7-T3 and nuchal ligament | Occipital bone | Posterior rami of the 2nd and 3rd cervical spinal nerves |
|
| Splenius cervicis | Spinous process T3-T6 | Transverse process C1-C3 | Dorsal rami of cervical spinal nerves (C5-C8) |
|
Innervation of the Cervical Spine[edit | edit source]
Nerves originating from the cervical plexus innervate the muscles of the neck. Each nerve root in the cervical spine exits above its corresponding nerve root. There are eight pairs of cervical nerves despite there being seven cervical vertebrae. The C8 nerve root exits below the seventh cervical vertebra. The accessory nerve, which is cranial nerve XI innervates sternocleidomastoid and trapezius.[2]
| Nerve | Motor | Sensory |
|---|---|---|
| C1 | Flexion of the head and neck
Rectus capitus anterior and lateralis, longus capitis |
|
| C2 | Flexion of the head and neck
Rectus capitus anterior and lateralis, longus capitus, prevertebral muscles and sternocleidomastoid |
Lateral occiput and submandibular area |
| C3 | Head and neck flexion and rotation
Longus capitus, longus colli, prevertebral muscles and sternocleidomastoid, diaphragm, levator scapulae, trapezius and scalenus medius |
Lateral occiput and lateral neck, overlapping C2 |
| C4 | Head and neck flexion and rotation
Longus capitus, longus colli, levator scapulae, scaleni, trapezius, diaphragm |
Lower lateral neck and medial shoulder area |
| C5 | Deltoid, biceps, bicep tendon reflex | Clavicle level and lateral arm |
| C6 | Biceps, wrist extensors (brachioradialis tendon reflex) | Lateral forearm, thumb, index and half of 2nd finger |
| C7 | Wrist flexors, triceps (triceps tendon reflex) | Second finger |
| C8 | Finger flexors, interossei | Medial forearm, ring and little finger |
| T1 | Interossei | Medial arm |
Vascular Supply of the Cervical Spine[edit | edit source]
Vertebral arteries, veins and nerves pass through the transverse foramina of the cervical vertebrae except for in C7, where the vertebral artery passes around the vertebra instead of through the transverse foramen.[4] The neural components sit posterior to the vertebral artery.[12]
The cervical spine vascular supply is primarily provided by the vertebral arteries on each side of the spine. These arteries arise from the subclavian arteries, which originate directly from the arch of the aorta on the right and the brachiocephalic trunk on the left.
** The common carotid artery bifurcates into the internal and external carotid arteries at the C3 segmental level. Only the external carotid artery provides any blood supply to the neck.
Clinical Relevance[edit | edit source]
- Atlanto-axial instability (AAI) can have serious neurological consequences:
- conditions with the potential for AAI include:
- rheumatoid arthritis
- Down syndrome:
- laxity in the transverse ligament is present in 14-22% of individuals with Down syndrome.
- conditions with the potential for AAI include:
- A tight sternocleidomastoid muscle can cause torticollis.
- Disc herniation:
- disc herniations in the cervical spine are a lot less common than in the lumbar spine
- typical locations:
- C5-C6
- C6-C7
- Because the prevertebral cervical muscles stabilise the neck, dysfunction in these muscles can cause cervicogenic pain
- Trigger points that develop in the suboccipital muscles can refer pain to the head, causing cervicogenic headaches[10]
Resources[edit | edit source]
- Functional Anatomy of the Thoracic Spine and Rib Cage
- Functional Anatomy of the Lumbar Spine and Abdominal Wall
- Cervical Deep Neck Extensors
- Cervical Deep Neck Flexors
References[edit | edit source]
- ↑ Frost BA, Camarero-Espinosa S, Foster EJ. Materials for the spine: anatomy, problems, and solutions. Materials. 2019 Jan;12(2):253
- ↑ 2.0 2.1 2.2 2.3 2.4 Kaiser JT, Reddy V, Lugo-Pico JG. Anatomy, Head and Neck: Cervical Vertebrae. [Updated 2022 Oct 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK539734/
- ↑ Petersen JA, Brauer C, Thygesen LC, Flachs EM, Lund CB, Thomsen JF. Prospective, population-based study of occupational movements and postures of the neck as risk factors for cervical disc herniation. BMJ open. 2022 Feb 1;12(2):e053999.
- ↑ 4.0 4.1 Teach me anatomy The cervical Spine Available from:https://teachmeanatomy.info/neck/bones/cervical-spine/
- ↑ 5.0 5.1 Learn muscles . Cervical spine joints. Available from: https://learnmuscles.com/blog/2017/08/01/cervical-spinal-joints/ (last accessed 29.1.2020)
- ↑ Peng B, Bogduk N. Cervical discs as a source of neck pain. An analysis of the evidence. Pain Medicine. 2019 Mar 1;20(3):446-55.
- ↑ Guo GM, Li J, Diao QX, Zhu TH, Song ZX, Guo YY, Gao YZ. Cervical lordosis in asymptomatic individuals: a meta-analysis. Journal of orthopaedic surgery and research. 2018 Dec;13(1):1-7.
- ↑ Lindenmann S, Tsagkaris C, Farshad M, Widmer J. Kinematics of the Cervical Spine Under Healthy and Degenerative Conditions: A Systematic Review. Annals of Biomedical Engineering. 2022 Dec 10:1-29.
- ↑ RSNA Joints of Luschka Available from: https://pubs.rsna.org/doi/10.1148/66.2.181 (last accessed 28.1.2020)
- ↑ 10.0 10.1 Xuan D. Exploring Cervical Spine Anatomy Course. Plus, 2023.
- ↑ Palastanga, N., & Soames, R. (2012). Anatomy and human movement (6th ed.). Edinburgh: Churchill Livingstone.
- ↑ Joshi N, Klinger N, Halalmeh DR, Tubbs RS, Moisi MD. The Neural Sulcus of the Cervical Vertebrae: A Review of Its Anatomy and Surgical Perspectives. Cureus. 2020 Jan 18;12(1)