Respiratory Physiotherapy for ICU Patients
Original Editor - Merinda Rodseth
Top Contributors - Merinda Rodseth, Kim Jackson, Tarina van der Stockt, Uchechukwu Chukwuemeka, Lucinda hampton and Jess Bell
The Respiratory System[edit | edit source]
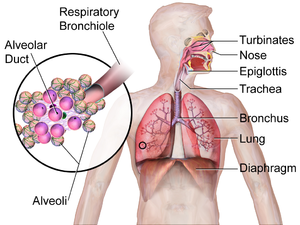
The respiratory system consists of the airways, lungs as well as musculoskeletal structures of the thoracic cage. A simple way of understanding the respiratory system is to split it into the musculoskeletal pump and the gas-exchanging organ.[1] The musculoskeletal pump consists of the surrounding bony structures (rib cage, cervical and thoracic spine, upper pelvic area) as well as the muscles of respiration. The gas-exchanging organ refers to the airways which allow the movement of air from outside the body to the alveoli, and the alveolar-capillary membrane, which is the specialised interface between the inspired air and the circulation.[1] Respiration involves the exchange of gas between the atmosphere and the lungs, lungs and the blood and the blood and body tissues. The function of this system is to maintain the supply of oxygen and the removal of carbon dioxide from the body.[1] Failure in any of the components of the respiratory system can result in the need for mechanical ventilation.[2]
Respiratory dysfunction is a common problem associated with the critically ill in the Intensive Care Unit (ICU).[2][3] Critically ill patients in ICU are often confined to their beds. This results in general deconditioning, which impacts many systems of the body, including the respiratory system.[1] Pulmonary complications, as the leading cause of hospital morbidity, is therefore of great concern in ICU patients.[1] Common complications following bed rest include reduced lung volumes and expiratory airflow rate, decreased respiratory muscle strength, reduced compliance of the lungs and chest wall as well as impaired gas exchange.[1] These factors all lead to an increase in the patient’s work of breathing and increases the risk for developing pneumonia and atelectasis. Weakness of the respiratory muscles together with the reduction in tidal volume can impair the cough mechanism which further increases the risk for pulmonary infections.[1] ICU patients are always at risk of developing complications such as secretion retention, atelectasis, ventilator-acquired pneumonia, decrease lung expansion, increased work of breathing, ventilation-perfusion mismatch, inspiratory muscle weakness and weaning failure.[1][3][4][5][6]
Aims of Physiotherapy[edit | edit source]
The aim of physiotherapy for respiratory dysfunction in the ICU is to maintain lung volume, improve oxygenation and ventilation, clear airway secretions, reduce the work of breathing, enhance inspiratory muscle function in order to prevent respiratory complications in both intubated and spontaneously breathing patients.[2][4][6][7][8][9] Other aims include maximizing musculoskeletal function, reducing the duration of mechanical ventilation, facilitating the return of independent function upon ICU discharge, improving long-term quality of life and reducing the length of stay in the ICU as well as the hospital in order to reduce the cost of care.[4][5][10] The goal of physiotherapy is targeted towards four key categories:[1][4][9][11][12]
- Airway secretion clearance
- Recruitment of lung volume or improvement of atelectasis
- Maintenance/improvement of oxygenation
- Maintenance/improvement inspiratory muscle strength
Physiotherapy Modalities for Respiratory Care[edit | edit source]
Physiotherapists, in an attempt to solve the respiratory challenges of ICU patients, utilise various modalities which will be discussed in brief. These modalities will be classified with respect to their uses.
Modalities for Airway Clearance[edit | edit source]
Airway clearance techniques refer to the manual or mechanical processes utilised to facilitate the mobilisation and removal of secretions (mucociliary clearance) from the airway.[4][13] The mucociliary clearance system is normally very efficient and effective, but following many respiratory diseases, pulmonary complications, anaesthesia and surgical procedures, excess sputum is often produced and the inherent mechanisms for secretion removal may become impaired.[4] Airway clearance techniques include:[1][3][4][5][8][11][12]
- Manual and Ventilator Hyperinflation (VHI)
- Positioning (Postural Drainage)
- Manual chest techniques (Percussion, Vibration, and Shaking)
- Airway Suctioning (open/closed)
- Insufflation and Exsufflation (positive pressure to negative pressure; device)
- Nebulisation
- Active Cycle of Breathing Technique (ACBT)
- Assisted Cough Techniques
- Forced expiratory maneuver (Coughing/Huffing)
- Positive Expiratory Pressure (PEP) Devices such as flutter, acapella
Modalities for Enhancing Lung Volume/Improvement of Atelectasis[edit | edit source]
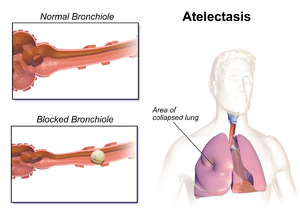
The following modalities can be used for enhancing lung volume or improve atelectasis (see figure 2):[1][4][8][11]
- Positioning (side-lying with affected side uppermost)
- Manual and Ventilator Hyperinflation
- Deep Breathing Exercises (Segmental and resisted breathing)
- Incentive Spirometry (IS)
- Positive End-Expiratory Pressure (PEEP)
- ACBT
- Breath Stacking
- Thoracic Expansion Exercises (TEE)
- Rib springing
- Manual Chest Wall Shaking and Vibrations
- Intermittent Positive Pressure Breathing (IPPB)
- Non-Invasive Ventilation (NIV) and CPAP
Modalities for Improvement of Oxygenation (Gas exchange)[edit | edit source]
- Positioning
- Non-Invasive Ventilation (Continuous Positive Airway Pressure (CPAP), Intermittent Positive Pressure Breathing (IPPB) devices, BiPAP, VPAP)
- Manual or ventilator hyperinflation
- Breath Stacking
- Deep Breathing Exercises
- TEE[1][4][8][11]
Modalities to Maintain or Improve Inspiratory Muscle Strength[edit | edit source]
- Breathing exercises
- Inspiratory Muscle Training Devices (spring-loaded Threshold® IMT or POWERbreathe® device)
- Incentive Spirometry
- Manual chest wall resistance [1][4][13]
Conclusion[edit | edit source]
Continuous evaluation is essential during the treatment of critically ill patients in the ICU. The findings of the evaluation are also what will guide the physiotherapist as to the most appropriate treatment. Constant changes in the physiological, motivational and emotional condition of the patient in ICU also necessitates that the plan of care is flexible.[1] Respiratory physiotherapy plays a big role in the ICU but it is important to remember that the role of the physiotherapist in the ICU is not limited only to respiratory management but also extends to mobilisation and rehabilitation which itself will have a direct impact on the respiratory system.
Resources[edit | edit source]
- Malone DJ, Bishop KL. Bed Rest, Deconditioning, Hospital-Acquired Neuromuscular Disorders, and Evidence-based Early Mobilisation. IN: Acute Care Physical Therapy : A Clinician’s Guide, Second Edition [Internet]. Thorofare, NJ: SLACK Incorporated; 2020. p.119-147.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Malone DJ, Bishop KL. Acute Care Physical Therapy : A Clinician’s Guide, Second Edition [Internet]. Vol. Second edition. Thorofare, NJ: SLACK Incorporated; 2020 [cited 2021 Mar 5].
- ↑ 2.0 2.1 2.2 Gosselink R, Roeseler J. Physiotherapy in critically ill patients. The ESC Textbook of Intensive and Acute Cardiovascular Care. 2015 Feb 26:284.
- ↑ 3.0 3.1 3.2 Connolly B, Barclay M, Blackwood B, Bradley J, Anand R, Borthwick M, et al. Airway clearance techniques and use of mucoactive agents for adult critically ill patients with acute respiratory failure: a qualitative study exploring UK physiotherapy practice. Physiotherapy. 2020;108:78-87. DOI:10.1016/j.physio.2020.06.003.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 4.9 Main E, Denehy L, editors. Cardiorespiratory Physiotherapy: Adults and Paediatrics E-Book: formerly Physiotherapy for Respiratory and Cardiac Problems. 5th ed. Elsevier Health Sciences; 2016 Jun 7.
- ↑ 5.0 5.1 5.2 Çakmak A, İnce Dİ, Sağlam M, Savcı S, Yağlı NV, Kütükcü EÇ, et al. Physiotherapy and Rehabilitation Implementation in Intensive Care Units: A Survey Study. Turkish thoracic journal. 2019;20(2):114. DOI:10.5152/TurkThoracJ.2018.18107
- ↑ 6.0 6.1 Spapen HD, De Regt J, Honoré PM. Chest physiotherapy in mechanically ventilated patients without pneumonia—a narrative review. Journal of thoracic disease. 2017;9(1): E44. DOI: 10.21037/jtd.2017.01.32
- ↑ Gosselink R, Clerckx B, Robbeets C, Vanhullebusch T, Vanpee G, Segers J. Physiotherapy in the intensive care unit. Neth J Crit Care. 2011;15(2):66-75.
- ↑ 8.0 8.1 8.2 8.3 Swaminathan N, Praveen R, Surendran P. The role of physiotherapy in intensive care units: a critical review. Physiotherapy Quarterly. 2019;27(4):1-5. DOI:10.5114/pq.2019.87739
- ↑ 9.0 9.1 Denehy L, Granger CL, El-Ansary D, Parry SM. Advances in cardiorespiratory physiotherapy and their clinical impact. Expert review of respiratory medicine. 2018;12(3):203-15. DOI:10.1080/17476348.2018.1433034
- ↑ Lipshutz AKM, Gropper MA. Early Ambulation in the ICU. In: Vincent JL, Abraham E, Kochanek P, Moore FA, Fink MP. editors Textbook of Critical Care. 7th ed. Philadelphia: Elsevier; 2017.
- ↑ 11.0 11.1 11.2 11.3 Troosters T, Bott J. Respiratory physiotherapy. In: Palange P, Rohde G. editors. ERS Handbook of Respiratory Medicine. 3rd ed. European Respiratory Society; 2019. p.232-238.
- ↑ 12.0 12.1 Gupta L, Gupta H. Physiotherapy for Respiratory Conditions. Advanced nursing & patient care international journal. 2018;1(1):180003.
- ↑ 13.0 13.1 Ahmad AM. Essentials of physiotherapy after thoracic surgery: What physiotherapists need to know. A narrative review. The Korean Journal of thoracic and cardiovascular surgery. 2018;51(5):293. DOI:10.5090/kjtcs.2018.51.5.293
- ↑ Cystic Fibrosis Foundation. Airway Clearance Techniques (ACTs). Published 19 May 2017. Available from: https://www.youtube.com/watch?v=1Ufj3oU_M2w [last accessed 30 April 2021]
- ↑ Nick Smith. CPAP and Non-Invasive Ventilation in 5 minutes. Publised 20 March 2015. Available from: https://www.youtube.com/watch?v=OHQK5PUTQ_0 [last accessed 30 April 2021].
- ↑ POWERbreatheUK. POWERbreathe - How it works. Published 10 Mar 2011. Available from: https://www.youtube.com/watch?v=nd5U7mDhFi4 [last accessed 30 April 2021].
- ↑ Dr. John Campbell. Respiratory System 8, Lung volumes and capacities. Published 25 March 2019. Available from: https://www.youtube.com/watch?v=KnNkqH3-1SU [last accessed 30 April 2021].