Respiratory Physiotherapy
Introduction[edit | edit source]
Respiratory physiotherapy is a core specialty within the physiotherapy profession and occupies a key role in the management and treatment of patients with respiratory diseases. It aims to unclog the patient’s airways and help them return to physical activity and exertion. The respiratory physiotherapist employs many diverse interventions, including pulmonary rehabilitation, early mobilisation, and airway clearance techniques, all having beneficial effects on the symptoms associated with respiratory diseases. For example improved sputum clearance and cough efficacy, reduced dyspnea, and improved physical fitness. The beneficial effects are demonstrated in improved functional ability and reduced intensive care and hospital stay, with savings in associated health-care costs. Physiotherapists specialising in respiratory care work in a variety of settings including Intensive Care Units (ICUs), hospital wards, and primary care settings[1]
As well as “chest physiotherapy”, which includes the management of clients with excessive airway secretions, maximising oxygenation, improving lung volume, preserving musculoskeletal function, and providing advice and education to patients and their carers – respiratory physiotherapists have an essential role in early mobilisation, exercising, and muscle retraining for clients across the spectrum of conditions[1]. Examples being: respiratory conditions (COPD, bronchiectasis, cystic fibrosis); neuromuscular diseases (muscular dystrophy, cerebral palsy, spinal cord injury), and during peri-operative care mainly in upper abdominal surgeries.[2][3]
Aims of Chest Physiotherapy[edit | edit source]
The purpose of chest physiotherapy are:
- To facilitate removal of retained or profuse airway secretions.
- To optimize lung compliance and the ventilation-perfusion ratio/ improve gas exchange.
- To decrease the work of breathing.
- Improve exercise tolerance
- Prevent secondary complications.[2][3]
The Physiological Mechanism of Airway Clearance[edit | edit source]
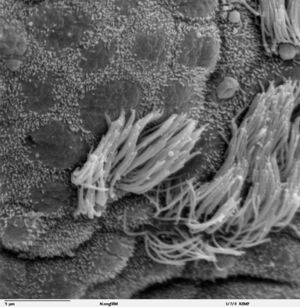
Normal Clearance: A normal clearance requires an open airway, a functional mucociliary escalator, and an effective cough. Airways normally are kept open by structural support mechanisms and kept clear by the proper function of their ciliated mucosa. The normal human bronchial tree is lined by a thin (5 micrometers) layer of mucus which is moved over the airway surface by the mucociliary escalator. The ciliated epithelium which lines the airways is responsible for the continuous flow of mucus over the airway surface to the upper respiratory tract. Mucus is moved via a coordinated movement of ciliary motion toward the trachea and larynx, where excess secretions can be swallowed or expectorated. [4]
The effective cough is a must for normal airway clearance.
Cough is one of the most important protective reflexes. By ridding the larger airways of excessive mucus and foreign matter, the cough assists the normal mucociliary clearance and helps ensure airway patency. There are four distinct phases to a normal cough: irritation, inspiration, compression, and expulsion.[4]
Abnormal Clearance: The flow of air through the tracheobronchial tree and its interaction with the mucus lining is complex because of the branching geometry of the airways, collapsible airway walls, constantly changing the velocity of airflow, and varying viscoelastic properties of mucus. This physiology of flow in liquid line airway is called a two-phase gas-liquid flow. In endobronchial diseases, the mucus layer may exceed 5 mm in thickness and ciliary clearance becomes ineffective. Two-phase flow now becomes an important mechanism of clearance, and at a particular combination of airflow, mucus viscosity, and thickness there is a very strong gas-liquid interaction which first exacerbates the pressure decrease then detaches liquid from the airway wall. this leads to the narrowing of the lumen of the tube causing a much greater resistance, thus affect airway clearance.
One of the mechanisms by which cough affects sputum clearance in endobronchial diseases is two phases gas-liquid flow: the transfer of momentum and energy from the high-speed flow of air to the mucus that lines the bronchi. The high transmural pressure produced during cough leads to dynamic compression of the airway inhibiting mucociliary clearances.[4] Thus, forced expiratory technique (FET) was introduced to solve this problem.
Classification[edit | edit source]
There are various physiotherapy treatments incorporated within chest physiotherapy. Chest physiotherapy techniques can be classified as conventional, modern, or instrumental techniques based on evolving research.[2]
Conventional Techniques[edit | edit source]
Conventional chest physiotherapy is also known as traditional chest physiotherapy. It was advocated first in 1915. It involves manual handling techniques to facilitate mucociliary clearance. Postural drainage along with percussion and vibration ( PDPV) was previously widely named as Chest Physiotherapy. Later, coughing exercises and forced expiratory techniques (huffing) were incorporated within it. PDPV with huffing has shown an effective outcome. It can be self-administered or performed with the assistance of another person (a physiotherapist, parent, or caregiver). PDPV works better if applied with bronchodilator therapy.
Postural drainage[edit | edit source]
Postural drainage (see link) involves positioning a person with the assistance of gravity to aid the normal airway clearance mechanism. Postural drainage positioning varies based on specific segments of the lungs with a large amount of secretions. Postural drainage is the drainage of secretions, by the effect of gravity, from one or more lung segments to the central airways (where they can be removed by a cough or mechanical aspiration). Each position consists of placing the target lung segment(s) superior to the carina. Positions should generally be held for 3 to 15 minutes (longer in special situations). Standard positions are modified as the patient's condition and tolerance warrant. Before determining the postural drainage position, it is very important to auscultate the lungs and identify the lung segments where added sound (Crepitus, Ronchi) is heard. Postural drainage can be facilitated with percussion and vibration in the postural drainage position.[6][2]
Percussion[edit | edit source]
Percussion is also referred to as cupping, clapping, and tapotement. The purpose of percussion is to intermittently apply kinetic energy to the chest wall and lungs. This is accomplished by rhythmically striking the thorax with a cupped hand or mechanical device directly over the lung segment(s) being drained. [6]
Vibration[edit | edit source]
Vibration involves the application of a fine tremorous action (manually performed by pressing in the direction that the ribs and soft tissue of the chest move during expiration) over the draining area. In this technique, a rapid vibratory impulse is transmitted through the chest wall from the flattened hands of the therapist by isometric alternate contraction of forearm flexor and extensor muscles, to loosen and dislodge the airway secretions.[6]
Coughing[edit | edit source]
Coughing includes directed coughing and various assisted coughing techniques.
Forced Expiratory Technique (FET)[edit | edit source]
Forced expiratory techniques involve diaphragmatic inspiration, relaxing the scapulohumeral region, and expiring forcefully from mid to low lung volumes whilst maintaining an open glottis ("huffing" exercises).[6] It is more effective than coughing.
Indication of Conventional techniques[edit | edit source]
Postural drainage positioning
- Inability or reluctance of the patient to change body position. (eg, mechanical ventilation, neuromuscular disease, drug-induced paralysis).
- Poor oxygenation associated with the position (eg, unilateral lung disease).
- Potential for or presence of atelectasis.
- Presence of artificial airway[6].
PDPV
- Difficulty clearing secretions with expectorated sputum production greater than 25-30 mL/day (adult).
- Evidence or suggestion of retained secretions in the presence of an artificial airway.
- Presence of atelectasis caused by or suspected of being caused by mucus plugging.
- Diagnosis of diseases such as cystic fibrosis, bronchiectasis, or cavitating lung disease
- Presence of foreign body in the airway.
- Patient with copious sputum or with central consolidation.[6]
Frequency[edit | edit source]
Positioning: Ventilated and critically ill patients: as necessary with the goal of once each hour or every other hour as tolerated, around the clock. Less acute patients should be turned every 2 hours as tolerated.
PDPV
- In critical care patients, including those on mechanical ventilation, PDT should be performed every 4 to every 6 hours as indicated. PDT order should be re-evaluated at least every 48 hours based on assessments from individual treatments.
- In spontaneously breathing patients, frequency should be determined by assessing patient response to therapy.
- Acute care patient orders should be re-evaluated based on patient response to therapy at least every 72 hours or with a change of patient status.
- Domiciliary patients should be re-evaluated every 3 months and with a change of status.[6]
Modern techniques[edit | edit source]
Over the years, several additional noninvasive clearance methods have been developed to augment this traditional approach. Modern techniques use a variation of flow through breath control to mobilize secretions. It includes an active cycle of breathing and autogenic drainage.
Active cycle of breathing technique[edit | edit source]
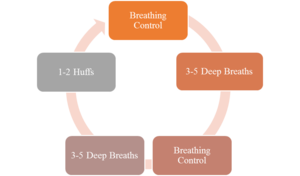
Active cycle of breathing technique (ACBT) is an active breathing technique performed by the patient, and can be used to mobilize and clear excess pulmonary secretions and to generally improve lung function. It has a series of three main phases: Breathing control, Thoracic expansion, and Forced expiratory technique.
Autogenic drainage[edit | edit source]
Autogenic drainage is a diaphragmatic breathing pattern used by patients with respiratory illnesses (e.g., cystic fibrosis, bronchiectasis) to clear the lungs of mucus and other secretions. Various techniques are used, all of which combine positive reinforcement of deep breathing and voluntary cough suppression for as long as possible before evacuating the airways of mucus. See Link. [2]
Instrumental techniques[edit | edit source]
Instrumental techniques such as non‐invasive ventilation have been considered useful as an adjunct therapy to airway clearance and to provide respiratory support. Common instrumental techniques are:
- Positive expiratory pressure (PEP): There are various positive expiratory pressure devices that provide resistance to expiration through a mouthpiece or facemask, followed by forced expirations. The inhalation is at tidal volume, and the expiration is slightly active against devices. These devices help to remove secretions by increasing functional residual capacity and thus enhancing collateral ventilation and removing secretions from collapse airways. Some of the devices are Flutter, Acapella, lung flute, etc.
- Continuous Positive Airway Pressure: generated by exhalation against a constant opening pressure, this produces positive end‐expiratory pressure (PEEP). Continuous positive airway pressure can also be delivered by commercially available pressure drivers. These generally require tightly fitting nasal prongs or a CPAP face mask. Bubble CPAP can be used in a low resource environment and in the pediatric population. It consists of an interface (nasal cannula), inspiratory tubing, and expiratory tubing immersed in an underwater bottle system.[2]
- High-Frequency Chest Wall Oscillation (HFCWO): an airway clearance technique in which external chest wall oscillations are applied to the chest using an inflatable vest that wraps around the chest. These machines produce vibrations at variable frequencies and intensities, helping to loosen and thin mucus and separate it from airway walls.
- HFCWO involves an inflatable jacket that is attached to a pulse generator by hoses that mechanically enable the equipment to perform at variable frequencies (5–25 Hz). The generator sends air through the hose, which causes the vest to inflate and deflate rapidly. The vibrations not only separate mucus from the airway walls but also help move it up into the large airways. Typically, it is paused during the 20- to 30-minute HFCWO treatment every 5 minutes to cough out loosened mucus that has moved into the large airways.[8]
- [9]
- Intrapulmonary Percussive Ventilation (IPV): designed to promote mobilisation of bronchial secretions and improve efficiency and distribution of ventilation, providing intrathoracic percussion and vibration and an alternative system for the delivery of the positive pressure to the lungs.[10] Each IPV session lasted fifteen minutes and was performed twice a day (morning and afternoon).[10] Intrapulmonary percussive ventilation uses a pneumatic device to deliver a series of pressurised gas minibursts at rates of 100 to 225 cycles per minute to the respiratory tract, by a mouthpiece. The duration of each percussive cycle is manually controlled by a thumb button. During the cycle, constant PAP is maintained at the airway. It also incorporates nebulizer for the delivery of the aerosol.
Assessment of need and outcome[edit | edit source]
The following should be assessed together to establish a need for chest physiotherapy:
- Excessive sputum production.
- Effectiveness of cough.
- History of pulmonary problems treated successfully with PDT (eg, bronchiectasis, cystic fibrosis, lung abscess).
- Decreased breath sounds or crackles or rhonchi suggesting secretions in the airway.
- Change in vital signs.
- Abnormal chest x-ray consistent with atelectasis, mucus plugging, or infiltrates.
- Deterioration in arterial blood gas values or oxygen saturation[6].
The following can be used as an outcome tool to determine the effectiveness of treatment:
- Change in sputum production.
- Change in breath sounds of lung fields.
- Patient subjective response to therapy.
- Change in vital signs.
- Change in chest x-ray.
- Change in arterial blood gas values or oxygen saturation.
- Change in ventilator variables.[6]
- Change in Modified borg scale- dyspnea level.
- Change in Peak Expiratory Flow Rate.
Contraindication of Conventional Techniques[edit | edit source]
Positioning[edit | edit source]
All positions are contraindicated for:
- Intracranial pressure (ICP) > 20 mm Hg
- Head and neck injury until stabilized (Absolute)
- Active hemorrhage with hemodynamic instability (Absolute)
- Recent spinal surgery (eg, laminectomy) or acute spinal injury
- Acute spinal injury or active hemoptysis
- Empyema
- Bronchopleural fistula
- Pulmonary edema associated with congestive heart failure
- Large pleural effusions
- Pulmonary embolism
- Aged, confused, or anxious patients who do not tolerate position changes
- Rib fracture, with or without flail chest
- Surgical wound or healing tissue
Trendelenburg position is contraindicated for
- Intracranial pressure (ICP) > 20 mm Hg
- Patients in whom increased intracranial pressure is to be avoided (eg, neurosurgery, aneurysms, eye surgery)
- Uncontrolled hypertension
- Distended abdomen
- Oesophageal surgery
- Recent gross hemoptysis related to recent lung carcinoma treated surgically or with radiation therapy.
- Uncontrolled airway at risk for aspiration (tube feeding or recent meal)
Reverse Trendelenburg is contraindicated in the presence of hypotension or vasoactive medication.
External Manipulation of the Thorax[edit | edit source]
In addition to contraindications previously listed
- Subcutaneous emphysema.
- Recent epidural spinal infusion or spinal anesthesia.
- Recent skin grafts, or flaps, on the thorax.
- Burns, open wounds, and skin infections of the thorax.
- Recently placed transvenous pacemaker or subcutaneous pacemaker (particularly if mechanical devices are to be used).
- Suspected pulmonary tuberculosis.
- Lung contusion.
- Bronchospasm.
- Osteomyelitis of the ribs.
- Osteoporosis.
- Coagulopathy.
- Complaint of chest-wall pain.
Complications[edit | edit source]
- Hypoxemia
- Bronchospasm
- Increased Intracranial Pressure
- Acute Hypotension during Procedure
- Pulmonary Hemorrhage
- Pain or Injury to Muscles, Ribs, or Spine
- Vomiting and Aspiration
- Bronchospasm
- Dysrhythmias
Resources[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 Al Mohammedali Z, O’Dwyer TK, Broderick JM. The emerging role of respiratory physiotherapy: A profile of the attitudes of nurses and physicians in Saudi Arabia. Annals of thoracic medicine. 2016 Oct;11(4):243.Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5070432/(accessed 21.10.2022)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Chaves GS, Freitas DA, Santino TA, Nogueira PA, Fregonezi GA, Mendonça KM. Chest physiotherapy for pneumonia in children. Cochrane Database of Systematic Reviews. 2019(1).
- ↑ 3.0 3.1 D. SELSBY AND J. G. JONES.SOME PHYSIOLOGICAL AND CLINICAL ASPECTS OF CHEST PHYSIOTHERAPY. British Journal of Anaesthesia 1990; 64: 621-631
- ↑ 4.0 4.1 4.2 Selsby DS. Chest physiotherapy. BMJ: British Medical Journal. 1989 Mar 4;298(6673):541.
- ↑ Armando Hasudungan. Physiology of coughing. Available from: https://www.youtube.com/watch?v=fn1XjzXQrwY. [last accessed 19/7/2020]
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 American Association for Respiratory Care. AARC Clinical Practice Guideline: postural drainage therapy. Respir care. 1991;36(12):1418-26.
- ↑ Tan Tock Seng Hospital. HVRSS 7. Chest Physiotherapy – Postural Drainage. Available from: https://www.youtube.com/watch?v=LJU_zVMnF3o
- ↑ High Frequency Chest Wall Oscillation (HFCWO). Bronchiectasis News Today. Available from: https://bronchiectasisnewstoday.com/high-frequency-chest-wall-oscillation-hfcwo/. [Last visited: 19th July, 2020]
- ↑ Pediatric Home Service. Giving a vest therapy. Available from: https://www.youtube.com/watch?v=mKiix67dd90. [last accessed 19/7/2020]
- ↑ 10.0 10.1 Nicolini A, Grecchi B, Ferrari-Bravo M, Barlascini C. Safety and effectiveness of the high-frequency chest wall oscillation vs intrapulmonary percussive ventilation in patients with severe COPD. International journal of chronic obstructive pulmonary disease. 2018;13:617.
- ↑ Percussionaire Corporation. Percussionaire High Frequency Ventilation. Available from: https://www.youtube.com/watch?v=K3d-ZmKgtQc [last accessed 12/05/2021]