Osteitis Pubis: Difference between revisions
No edit summary |
No edit summary |
||
| (5 intermediate revisions by the same user not shown) | |||
| Line 2: | Line 2: | ||
== Introduction == | == Introduction == | ||
[[File:Pelvis ant.jpeg|right|frameless]] | [[File:Pelvis ant.jpeg|right|frameless|292x292px]] | ||
Osteitis [[pubis]] is defined as non-infectious idiopathic, [[Inflammation Acute and Chronic|inflammatory]] condition of the pubic symphysis and surrounding structures, | Osteitis [[pubis]] is defined as non-infectious idiopathic, [[Inflammation Acute and Chronic|inflammatory]] condition of the pubic symphysis and surrounding structures with multiple causes, resulting in groin or lower abdominal pain.<ref name=":1" /> It is most likely related to overuse or trauma<ref>Up to date [https://www.uptodate.com/contents/osteitis-pubis#! Osteitis Pubis] Available:https://www.uptodate.com/contents/osteitis-pubis#! (accessed 8.11.2021)</ref>. Osteitis pubis was first described in patients who had undergone suprapubic [[Surgery and General Anaesthetic|surgery]], and it remains a well-known complication of invasive procedures about the [[pelvis]]. It may also occur as an inflammatory process in athletes<ref>Gomella P, Mufarrij P. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5737342/ Osteitis pubis: a rare cause of suprapubic pain]. Reviews in urology. 2017;19(3):156. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5737342/ (accessed 8.11.2021)</ref>. | ||
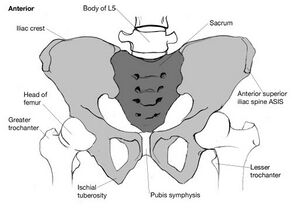
Image 1: anterior view of the pelvis. | Image 1: anterior view of the pelvis. | ||
| Line 16: | Line 16: | ||
== Clinical presentation == | == Clinical presentation == | ||
The most common symptom of Osteitis pubis is pain in the pelvis area. | The most common symptom of Osteitis pubis is pain in the pelvis area. The clinical presentation of osteitis pubis can vary from person to person, but common signs and symptoms may include: | ||
* Pain localized over the symphysis and radiating outward | * Pain localized over the symphysis and radiating outward | ||
* Patients with osteitis pubis often present with anterior and medial groin pain.<ref name=":0">Angoules AG. Osteitis pubis in elite athletes: Diagnostic and therapeutic approach. World Journal of Orthopedics. 2015;6(9):672.</ref> | |||
* Adductor pain or lower abdominal pain that then localizes to the pubic area | * Adductor pain or lower abdominal pain that then localizes to the pubic area | ||
* Pain is worsened by activities such as | * Pain is worsened by activities such as turning, walking, coughing, sneezing, lying on one side, and walking up or down stairs.<ref name=":0" /><ref>Gomella P, Mufarrij P. Osteitis pubis: A rare cause of suprapubic pain. Reviews in Urology [Internet]. 2017;19(3):156–63. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5737342/</ref> | ||
* In severe cases a waddling antalgic gait and crepitus may be present in individuals with osteitis pubis on examination or while doing daily activities.<ref name=":2">Hiti CJ, Stevens KJ, Jamati MK, Garza D, Matheson GO. Athletic osteitis pubis. Sport Med. 2011;41(5):361–76. </ref><ref name=":0" /> | |||
* Individuals suffering from osteitis pubis commonly experience tenderness around the pubic symphysis and pubic ramus, along with painful muscle spasms in the adductor region.<ref name=":0" /> | |||
* In severe cases a waddling | |||
The presentation is typical with varying degrees of pelvic and/or perineal pain, reproduced on hip adduction.<ref name=":4" /> | The presentation is typical with varying degrees of pelvic and/or perineal pain, reproduced on hip adduction.<ref name=":4" /> | ||
| Line 32: | Line 31: | ||
== Etiology == | == Etiology == | ||
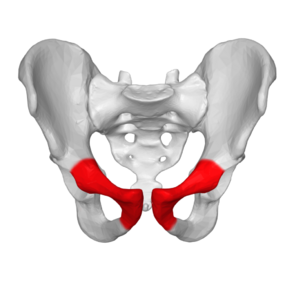
[[File:Pubic anterior view.png|right|frameless|294x294px|Image 2: Anterior view pelvis, pubis bone red.]] | |||
[[File:Pubic anterior view.png|right|frameless]] | Abnormal physical stresses at the pubic symphysis and parasymphyseal bone have been singled out as the likely cause of osteitis pubis. Although the aetiology is sometimes unknown, the most common causes are:<ref name=":2" /> | ||
Although the aetiology is sometimes unknown, the most common causes are: | |||
* Pregnancy/childbirth | * Pregnancy/childbirth | ||
| Line 41: | Line 39: | ||
* Trauma | * Trauma | ||
* [[Psoriatic Arthritis|psoriatic arthritis]] | * [[Psoriatic Arthritis|psoriatic arthritis]] | ||
* [[Ankylosing Spondylitis|ankylosing spondylitis]]<ref name=":4">Radiopedia [https://radiopaedia.org/articles/osteitis-pubis Osteitis Pubis] Available: https://radiopaedia.org/articles/osteitis-pubis<nowiki/>(accessed 8.11.2021)</ref> | * [[Ankylosing Spondylitis|ankylosing spondylitis]]<ref name=":4">Radiopedia [https://radiopaedia.org/articles/osteitis-pubis Osteitis Pubis] Available: https://radiopaedia.org/articles/osteitis-pubis<nowiki/>(accessed 8.11.2021)</ref> Image 2: Anterior view pelvis, pubis bone red. | ||
== Pathophysiology == | == Pathophysiology == | ||
[[File:Pubic Symphysis.gif|alt=|right|frameless|399x399px]] | [[File:Pubic Symphysis.gif|alt=|right|frameless|399x399px]] | ||
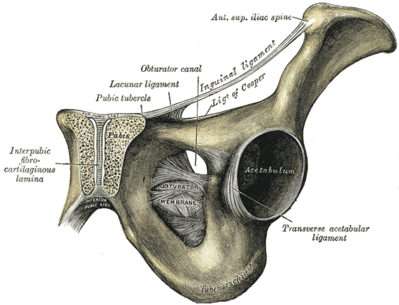
The pubic symphysis is a non-[[Synovial Joints|synovial]] amphiarthrodial [[Joint Classification|joint]] with an interposed fibrocartilaginous disc separating hyaline [[cartilage]]. The joint normally has minimal motion due to the static ligamentous complex. The pubic symphysis serves as the insertion point of the [[Rectus Abdominis|rectus abdominis]] and origin of the [[Adductor Magnus|adductor]] complex. The antagonistic nature of the rectus abdominis, which elevates the pubic symphysis while the adductors depress the joint, serves as a nidus for the development of osteitis pubis—the repetitive use of the anterior pelvic musculature results in chronic [[Tendinopathy|tendinosis]]. The chronic muscle imbalance results in abnormal forces across the pubic symphysis, causing symphyseal instability, pubic [[Bone Stress Injuries|bone stress reaction]], and eventually degeneration of the hyaline cartilage. Another emerging theory poses that osteitis pubis develops secondary to increased compensatory motion across the joint because of limited motion elsewhere in the [[Kinetic Chain|kinetic chain]], such as in [[Femoroacetabular Impingement|femoroacetabular impingement]].<ref name=":1">Dirkx M, Vitale C. [https://www.ncbi.nlm.nih.gov/books/NBK556168/ Osteitis Pubis]. StatPearls [Internet]. 2021 Jan 1.Available:https://www.ncbi.nlm.nih.gov/books/NBK556168/ (accessed 8.11.2021)</ref> | Osteitis pubis is thought to be a stress injury of the peri-symphyseal pubic bones secondary to increased strain on the anterior pelvis.<ref name=":2" /> The pubic symphysis is a non-[[Synovial Joints|synovial]] amphiarthrodial [[Joint Classification|joint]] with an interposed fibrocartilaginous disc separating hyaline [[cartilage]]. The joint normally has minimal motion due to the static ligamentous complex. The pubic symphysis serves as the insertion point of the [[Rectus Abdominis|rectus abdominis]] and origin of the [[Adductor Magnus|adductor]] complex. The antagonistic nature of the rectus abdominis, which elevates the pubic symphysis while the adductors depress the joint, serves as a nidus for the development of osteitis pubis—the repetitive use of the anterior pelvic musculature results in chronic [[Tendinopathy|tendinosis]]. The chronic muscle imbalance results in abnormal forces across the pubic symphysis, causing symphyseal instability, pubic [[Bone Stress Injuries|bone stress reaction]], and eventually degeneration of the hyaline cartilage. Another emerging theory poses that osteitis pubis develops secondary to increased compensatory motion across the joint because of limited motion elsewhere in the [[Kinetic Chain|kinetic chain]], such as in [[Femoroacetabular Impingement|femoroacetabular impingement]].<ref name=":1">Dirkx M, Vitale C. [https://www.ncbi.nlm.nih.gov/books/NBK556168/ Osteitis Pubis]. StatPearls [Internet]. 2021 Jan 1.Available:https://www.ncbi.nlm.nih.gov/books/NBK556168/ (accessed 8.11.2021)</ref> | ||
== Diagnosis == | == Diagnosis == | ||
| Line 52: | Line 50: | ||
* In chronic osteitis pubis, the pubic symphysis demonstrates lytic changes, sclerosis, sub-chondral resorption, bony margin irregularities and widening. | * In chronic osteitis pubis, the pubic symphysis demonstrates lytic changes, sclerosis, sub-chondral resorption, bony margin irregularities and widening. | ||
* Dynamic instability of the pubic symphysis can be observed on the flamingo view (obtained by double- and single-legged stance positions bilaterally on a pelvic anterior-posterior radiograph). Greater than 2 mm of subluxation is considered a positive finding for symphyseal instability. | * Dynamic instability of the pubic symphysis can be observed on the flamingo view (obtained by double- and single-legged stance positions bilaterally on a pelvic anterior-posterior radiograph). Greater than 2 mm of subluxation is considered a positive finding for symphyseal instability. | ||
* MRI has become the imaging modality of choice. MRI has a high sensitivity for distinguishing between chronic and acute cases.<ref name=":4" /> | * MRI has become the imaging modality of choice. MRI has a high sensitivity for distinguishing between chronic and acute cases.<ref name=":4" /> | ||
== Treatment == | == Treatment == | ||
The management of osteitis pubis includes both | The management of osteitis pubis includes both non-surgical and surgical approaches, with the initial preference being non-surgical (conservative) methods. | ||
The first option remains conservative treatment. | The first option remains conservative treatment. | ||
* Conservative management | * Conservative management involves a combination of rest, non-steroidal anti-inflammatory drugs (NSAIDs) and a progressive course of physical therapy (see [[Pubalgia]]). There is no standard conservative treatment protocol resulting in a variety of outcomes. The conservative treatment of osteitis pubis can be protracted. It may take some athletes six months or more to return to the preinjury level, but more commonly, most return by 3 months. | ||
* Albeit protracted, conservative management remains the mainstay of treatment. Only approximately 5% to 10% of athletes require surgical treatment. | * Albeit protracted, conservative management remains the mainstay of treatment. Only approximately 5% to 10% of athletes require surgical treatment. | ||
| Line 69: | Line 66: | ||
== Differential Diagnosis == | == Differential Diagnosis == | ||
* Athletic [[ | * Athletic [[Pubalgia]] | ||
* [[Osteomyelitis]] | * [[Osteomyelitis]] | ||
* [[Adductor Tendinopathy|Adductor strain]] | * [[Adductor Tendinopathy|Adductor strain]] | ||
* Rectus Abdominus strain | * Rectus Abdominus strain | ||
* Sacroiliac joint dysfunction | * Sacroiliac joint dysfunction | ||
* Genitourinary disease | |||
* Genitourinary disease | |||
== Viewing == | == Viewing == | ||
The short video below is of Physiotherapy techniques used for osteitis pubis{{#ev:youtube|7U5GLjR92Dk}}<ref>Pelvic pain Rehab Video-Osteitis Pubis. Available from: https://www.youtube.com/watch?v=7U5GLjR92Dk </ref> | The short video below is of Physiotherapy techniques used for osteitis pubis{{#ev:youtube|7U5GLjR92Dk}}<ref>Pelvic pain Rehab Video-Osteitis Pubis. Available from: https://www.youtube.com/watch?v=7U5GLjR92Dk </ref> | ||
== Complications == | |||
Surgical treatment of individuals with osteitis pubis can result in: | |||
* Chronic pain | |||
* Infection | |||
* Nonunion of fusion | |||
* Recurrence | |||
* Scrotal or labial swelling | |||
== Prognosis == | |||
The prognosis of individuals with osteitis pubis is very good. Those who undergo conservative treatment typically recover and can resume sports activities in about three months, with a low likelihood of experiencing a recurrence. A small number of patients with osteitis pubis, around 5% to 10% , need surgical intervention. However, those who undergo surgery generally experience highly positive outcomes, with the majority returning to their sports activities within approximately 3 to 4 months<ref name=":1" /> | |||
== References == | == References == | ||
<references />. | <references />. | ||
[[Category:Sports Injuries]] | [[Category:Sports Injuries]] | ||
Latest revision as of 14:18, 1 September 2023
Introduction[edit | edit source]
Osteitis pubis is defined as non-infectious idiopathic, inflammatory condition of the pubic symphysis and surrounding structures with multiple causes, resulting in groin or lower abdominal pain.[1] It is most likely related to overuse or trauma[2]. Osteitis pubis was first described in patients who had undergone suprapubic surgery, and it remains a well-known complication of invasive procedures about the pelvis. It may also occur as an inflammatory process in athletes[3].
Image 1: anterior view of the pelvis.
Quick Facts[edit | edit source]
- Osteitis pubis is a rare cause of groin pain but is more common in athletic patients, specifically soccer players, runners, and rugby players.
- Patients often present with groin pain made worse with activity.
- Plain radiographs and MRIs may aid with the diagnosis.
- The condition is usually treated with NSAIDs, activity restriction, and physical therapy.
- In rare cases, surgical intervention may be required[1].
Clinical presentation[edit | edit source]
The most common symptom of Osteitis pubis is pain in the pelvis area. The clinical presentation of osteitis pubis can vary from person to person, but common signs and symptoms may include:
- Pain localized over the symphysis and radiating outward
- Patients with osteitis pubis often present with anterior and medial groin pain.[4]
- Adductor pain or lower abdominal pain that then localizes to the pubic area
- Pain is worsened by activities such as turning, walking, coughing, sneezing, lying on one side, and walking up or down stairs.[4][5]
- In severe cases a waddling antalgic gait and crepitus may be present in individuals with osteitis pubis on examination or while doing daily activities.[6][4]
- Individuals suffering from osteitis pubis commonly experience tenderness around the pubic symphysis and pubic ramus, along with painful muscle spasms in the adductor region.[4]
The presentation is typical with varying degrees of pelvic and/or perineal pain, reproduced on hip adduction.[7]
Epidemiology[edit | edit source]
To date, there has been no epidemiological study to determine the true incidence of osteitis pubis. The incidence in athletes has been reported as 0.5% to 8%, with a higher incidence in distance runners and athletes in kicking sports, in particular, male soccer players who account for 10% to 18% of injuries per year.[1]
Etiology[edit | edit source]
Abnormal physical stresses at the pubic symphysis and parasymphyseal bone have been singled out as the likely cause of osteitis pubis. Although the aetiology is sometimes unknown, the most common causes are:[6]
- Pregnancy/childbirth
- High-level of athletic activity: see athletic pubalgia
- Urological or gynaecological surgery
- Trauma
- psoriatic arthritis
- ankylosing spondylitis[7] Image 2: Anterior view pelvis, pubis bone red.
Pathophysiology[edit | edit source]
Osteitis pubis is thought to be a stress injury of the peri-symphyseal pubic bones secondary to increased strain on the anterior pelvis.[6] The pubic symphysis is a non-synovial amphiarthrodial joint with an interposed fibrocartilaginous disc separating hyaline cartilage. The joint normally has minimal motion due to the static ligamentous complex. The pubic symphysis serves as the insertion point of the rectus abdominis and origin of the adductor complex. The antagonistic nature of the rectus abdominis, which elevates the pubic symphysis while the adductors depress the joint, serves as a nidus for the development of osteitis pubis—the repetitive use of the anterior pelvic musculature results in chronic tendinosis. The chronic muscle imbalance results in abnormal forces across the pubic symphysis, causing symphyseal instability, pubic bone stress reaction, and eventually degeneration of the hyaline cartilage. Another emerging theory poses that osteitis pubis develops secondary to increased compensatory motion across the joint because of limited motion elsewhere in the kinetic chain, such as in femoroacetabular impingement.[1]
Diagnosis[edit | edit source]
Both radiographs and MRI aid in the diagnosis of osteitis pubis. In the early stage, plain radiographs might appear normal.
- In chronic osteitis pubis, the pubic symphysis demonstrates lytic changes, sclerosis, sub-chondral resorption, bony margin irregularities and widening.
- Dynamic instability of the pubic symphysis can be observed on the flamingo view (obtained by double- and single-legged stance positions bilaterally on a pelvic anterior-posterior radiograph). Greater than 2 mm of subluxation is considered a positive finding for symphyseal instability.
- MRI has become the imaging modality of choice. MRI has a high sensitivity for distinguishing between chronic and acute cases.[7]
Treatment[edit | edit source]
The management of osteitis pubis includes both non-surgical and surgical approaches, with the initial preference being non-surgical (conservative) methods.
The first option remains conservative treatment.
- Conservative management involves a combination of rest, non-steroidal anti-inflammatory drugs (NSAIDs) and a progressive course of physical therapy (see Pubalgia). There is no standard conservative treatment protocol resulting in a variety of outcomes. The conservative treatment of osteitis pubis can be protracted. It may take some athletes six months or more to return to the preinjury level, but more commonly, most return by 3 months.
- Albeit protracted, conservative management remains the mainstay of treatment. Only approximately 5% to 10% of athletes require surgical treatment.
Steroid injections have been demonstrated as a useful adjunctive therapy
If conservative management does fail, surgical intervention may be required. The timeframe of when to consider conservative treatment as a failure ranges and no set timetable has been established. Commonly, a minimum of six months of conservative treatment is attempted before surgical options are discussed[1].
Differential Diagnosis[edit | edit source]
- Athletic Pubalgia
- Osteomyelitis
- Adductor strain
- Rectus Abdominus strain
- Sacroiliac joint dysfunction
- Genitourinary disease
Viewing[edit | edit source]
The short video below is of Physiotherapy techniques used for osteitis pubis
Complications[edit | edit source]
Surgical treatment of individuals with osteitis pubis can result in:
- Chronic pain
- Infection
- Nonunion of fusion
- Recurrence
- Scrotal or labial swelling
Prognosis[edit | edit source]
The prognosis of individuals with osteitis pubis is very good. Those who undergo conservative treatment typically recover and can resume sports activities in about three months, with a low likelihood of experiencing a recurrence. A small number of patients with osteitis pubis, around 5% to 10% , need surgical intervention. However, those who undergo surgery generally experience highly positive outcomes, with the majority returning to their sports activities within approximately 3 to 4 months[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Dirkx M, Vitale C. Osteitis Pubis. StatPearls [Internet]. 2021 Jan 1.Available:https://www.ncbi.nlm.nih.gov/books/NBK556168/ (accessed 8.11.2021)
- ↑ Up to date Osteitis Pubis Available:https://www.uptodate.com/contents/osteitis-pubis#! (accessed 8.11.2021)
- ↑ Gomella P, Mufarrij P. Osteitis pubis: a rare cause of suprapubic pain. Reviews in urology. 2017;19(3):156. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5737342/ (accessed 8.11.2021)
- ↑ 4.0 4.1 4.2 4.3 Angoules AG. Osteitis pubis in elite athletes: Diagnostic and therapeutic approach. World Journal of Orthopedics. 2015;6(9):672.
- ↑ Gomella P, Mufarrij P. Osteitis pubis: A rare cause of suprapubic pain. Reviews in Urology [Internet]. 2017;19(3):156–63. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5737342/
- ↑ 6.0 6.1 6.2 Hiti CJ, Stevens KJ, Jamati MK, Garza D, Matheson GO. Athletic osteitis pubis. Sport Med. 2011;41(5):361–76.
- ↑ 7.0 7.1 7.2 Radiopedia Osteitis Pubis Available: https://radiopaedia.org/articles/osteitis-pubis(accessed 8.11.2021)
- ↑ Pelvic pain Rehab Video-Osteitis Pubis. Available from: https://www.youtube.com/watch?v=7U5GLjR92Dk
.