Femoral Shaft Fractures
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
Fractures of the femoral shaft are a most common injury, often associated with polytrauma and can be life-threatening. They often result from high-energy mechanisms such as motor vehicle collisions with sequelae of limb shortening and deformities if not treated correctly.
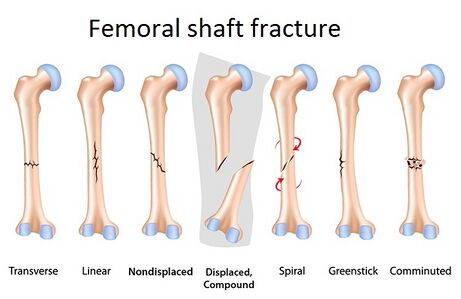
Femoral shaft fractures can be classified with the Winquist and Hansen classification, which is based on the amount of comminution.[1]
Epidemiology/Etiology[edit | edit source]
These fractures occur in a bimodal distribution: high-energy trauma in the young population; lower energy trauma in the elderly population.[1]
Fractures vary in degree and complexity, depending on the degree of force involved. They may be: transverse (horizontally across the shaft), oblique, spiral (due to a twisting force), comminuted (when there are three or more resulting bone pieces), open or closed.
Evaluation[edit | edit source]
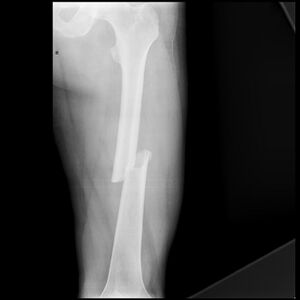
Femoral shaft fractures are readily identified injuries due to thigh deformity and instability; however, occasionally, these injuries are not evident, and further assessment and imaging are required, such as radiographs and CT scanning.
Treatment[edit | edit source]
Treatment of femoral shaft fractures can be operative or non-operative.
- Most femoral shaft fractures require surgery to heal. It is unusual for femoral shaft fractures to be treated without surgery in developed nations. Very young children are sometimes treated with a cast.[2]
- Operative fixation with intramedullary nailing is the gold standard of treatment in high-income countries. Other operative techniques include plate open reduction internal fixation (ORIF) techniques and external fixation. Most femur fractures are fixed within 24 to 48 hours. On occasion, fixation will be delayed until other life-threatening injuries or unstable medical conditions are stabilized.[2]
- Closed treatment with traction, splinting, and casting may be temporary treatment or definitive treatment in some third-world countries.[1]
Surgery:
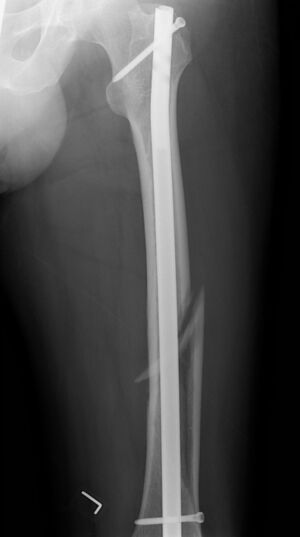
- Intramedullary nailing: During this procedure, a specially designed metal rod is inserted into the canal of the femur. The rod passes across the fracture to keep it in position.
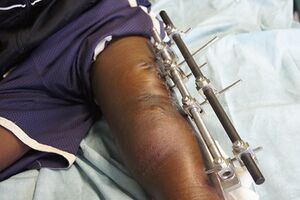
- External fixation (EF): Metal pins or screws are placed into the bone above and below the fracture site, with the pins and screws being attached to a bar outside the skin. This device is a stabilising frame that holds the femur in the proper position. EF is generally a short term treatment for femur fractures. As they are easily applied, EFs are commonly used put on when a patient has multiple injuries and is not yet ready for a longer surgery to fix the fracture. An EF is a temporary solution until the patient is healthy enough for the final surgery. Sometimes an EF is left on until the femur is fully healed, but not regularly.[2]
Complications[edit | edit source]
Most bone injuries heal normally. But some patients do experience complications during the healing process. See Fracture Complications
Recovery[edit | edit source]
Femoral shaft fractures take 3 to 6 months to completely heal. It may be longer if the fracture was open or broken into several pieces or if the patient is a smoker.[2]
Postoperative And rehabilitation Care[edit | edit source]
Postoperatively patients may experience local and systemic complications.
- Patients are evaluated for compartment syndrome, wound issues, and neurovascular compromise.
- Systemic complications include DVT, PE, and fat emboli syndrome.
Shortly after surgery, patients will start physical and occupational therapy in the hospital to regain mobility and function in daily activities with continuation in the outpatient setting.
Weight Bearing:
- Patients are typically allowed to bear weight as tolerated and return to full or near full capacity before radiographic healing, described as callus formation on three of the four sides of the bone on imaging.
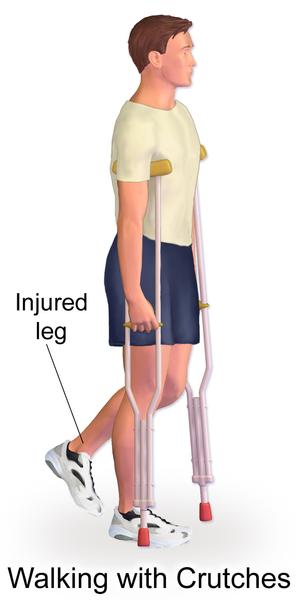
- When walking commences it is usually with crutches or a walker for support.
- Patients may return to driving a car when they can weight bear without assistance and can safely use the right leg to break.[1]
PT management[edit | edit source]
Physiotherapy aims to improve impairments after a femoral shaft fracture ie address weight bearing (WB) status, knee effusion, quadriceps control, and hip abduction strength. The program needs be dynamic, incorporating interventions designed to target these known impairments, helping to restore normal muscle strength, joint motion, and flexibility.[3]
Whilst in hospital, a therapist will teach the patient how to use a walking aid to allow them to mobilise, depending on their weight bearing status. Gait training results in increased bone formation. Even if gait training is completed using 30-50% of body weight support, an increase in bone formation could be found.[4]
Phases of Treatment:
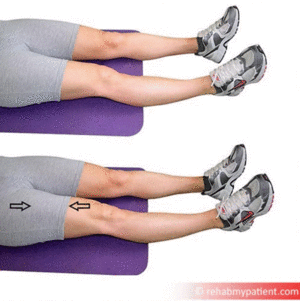
- Initial phase (week 0-2): Treatment includes gentle passive and active movements and gait training using assistive device. Also education to get in and out of bed, on and off the toilet and up and down the stairs . Soft tissue mobilisation may beused to help decrease pain levels and improve range of movement. The patient should be taught basic range of movement and strengthening exercises to maintain a degree of strength and reduce the risk of blood clots. Begin with a range of motion exercises for the hip, knee and ankle. During the immobilisation period, the therapists need to actively mobilise the foot, with or without weight. The use of isometric exercises are also important to train the muscles (quadriceps, hamstring & glutei) of the upper leg. Functional quadriceps exercises should be initiated as soon as possible after the surgery because the quadriceps help provides stability in the knee. Flexion exercises also need to start as soon as possible, provided the fracture is adequately supported (i.e. the selected fixation approach allows for weight bearing).
- Middle phase (week 2-6): Goal is to strengthen the quadriceps, hamstrings and gluteal muscles. The exercises are progressed as surgeon/physiotherapist see fit to ensure they are carried out safely and efficiently.
- Late phase (week 3-12): Aim to gradually return the patient to their function/sporting activity with exercises focusing on sport specific drills. Restoring ability with ADLs eg. walking to the shops, household cleaning and gardening[5].
- Hydrotherapy is an excellent good way to maximise mobility, strengthen muscle and stretch tight muscles (only appropriate when your wound has healed
- Development of exercises in order to continue strengthening muscles around you hip. Exercise will also improve balance, flexibility and endurance. Activities to increase your fitness levels may be included such as walking, hydrotherapy and gentle cycling.
- Physiotherapy should be continued until an acceptable functional range has been achieved or until a static position has been reached. It is necessary to record the range of movements in the knee with accuracy; first, this should be done at weekly and then at monthly intervals. Strengthening exercises based on the surgeon's orders typically begin at six weeks post-op.
- Balance and proprioceptive rehab important as these abilities are quickly lost with inactivity.[6]
- After the consolidation therapists need to focus on: the revalidation of the gait cycle; more intense mobilisation, strength-training therapy to reverse the muscle atrophy that occurred during the immobilisation period and condition training to increase the loss of endurance during the immobilisation period.
Viewing[edit | edit source]
Watch this video titled "Femoral shaft fracture physiotherapy management in acute phase". 4 minutes.
This video is a personal journey from week 1 to 10, (less than 3 minutes)
Physical Exercise[edit | edit source]
Physical exercises are not only crucial for rehabilitation after fracture but for ongoing reinforcing of the mineral bone density, especially in vulnerable populations like elder fragile patients, osteoporotic post-menopausal women or people suffering from osteoporosis or osteopenia. Long-term odd-impact exercise-loading, is associated, similar to high-impact exercise-loading, with a 20% thicker cortex around the femoral neck . In aerobic fitness, these type of movements are most frequently used .[9][10]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Denisiuk M, Afsari A. Femoral shaft fractures. InStatPearls [Internet] 2022 Feb 4. StatPearls Publishing. Available:https://www.statpearls.com/articlelibrary/viewarticle/81253/ (accessed 10.12.2022)
- ↑ 2.0 2.1 2.2 2.3 Orthoinfo Femur Shaft Fractures (Broken Thighbone) Available:https://orthoinfo.aaos.org/en/diseases--conditions/femur-shaft-fractures-broken-thighbone (accessed 11.12.2022)
- ↑ Paterno MV, Archdeacon MT. Is there a standard rehabilitation protocol after femoral intramedullary nailing?. Journal of orthopaedic trauma. 2009 May 1;23:S39-46. Available:https://journals.lww.com/jorthotrauma/Fulltext/2009/05005/Is_There_a_Standard_Rehabilitation_Protocol_After.9.aspx (accessed 11.12.2022)
- ↑ Carvalho DC, Garlipp CR, Bottini PV, Afaz SH, Moda MA, Cliquet Jr A. Effect of treadmill gait on bone markers and bone mineral density of quadriplegic subjects. Brazilian journal of medical and biological research. 2006;39:1357-63.
- ↑ Physio uk Fractured Shaft of Femur Available:https://www.physio.co.uk/what-we-treat/surgery/hip/fractured-shaft-of-femur.php (accessed 11.12.2022)
- ↑ MCarneiro B, Alves DP, Mercadante MT. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013;21:175-8
- ↑ Christine Ng. Femoral Femoral Shaft Fracture Physiotherapy Management in Acute Phase. Available from: https://www.youtube.com/watch?v=x0BheysnRVg [last accessed 11.12.2022]
- ↑ Hugh Van. Broken Femur Recovery - 10 Weeks - Part 1. Available from: https://www.youtube.com/watch?v=ufAoBqtOWmk [last accessed 11.12.2022]
- ↑ Nikander R, Kannus P, Dastidar P, Hannula M, Harrison L, Cervinka T, Narra NG, Aktour R, Arola T, Eskola H, Soimakallio S. Targeted exercises against hip fragility. Osteoporosis International. 2009 Aug;20(8):1321-8.Available:https://pubmed.ncbi.nlm.nih.gov/19002370/ (accessed 11.12.2022)
- ↑ Yang SD, Ning SH, Zhang LH, Zhang YZ, Ding WY, Yang DL. The effect of lower limb rehabilitation gymnastics on postoperative rehabilitation in elderly patients with femoral shaft fracture: a retrospective case-control study. Medicine. 2016 Aug;95(33).Available: https://pubmed.ncbi.nlm.nih.gov/27537579/ (accessed 11.12.2022)