Apraxia
Original Editor - Shreya Pavaskar
Top Contributors - Niha Mulla, Shreya Pavaskar and Lucinda hampton
Definition[edit | edit source]
Apraxia is a motor disorder caused by damage to the brain (specifically the posterior parietal cortex or corpus callosum.[1] Apraxia is inability to carry out learned purposeful movement despite the presence of a good motor, sensory, or coordination function. Both the desire and the capacity to move are present but the person simply cannot execute the act.
Relevant Anatomy[edit | edit source]
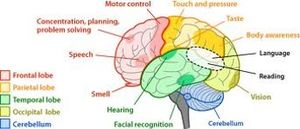
The frontal lobes are important for voluntary movement, expressive language and for managing higher level executive functions
The cerebellum has the ability to store and update motor information. There is a significant role played inaccurate learned movement. This is due to a modifiable synapse at the purkinje cell.
Refer- Brain, Frontal lobe
Causes[edit | edit source]
- Lesions of the premotor frontal cortex of either hemisphere, left inferior parietal lobe, and corpus callosum can produce apraxia. Apraxia is more evident with left hemisphere damage than right and is commonly seen with aphasia.[2]
- Any disease of these areas can cause apraxia, although stroke and dementia are the most common causes. Interestingly, callosal apraxia is rare after callosotomy and is much more common with anterior cerebral artery strokes or tumors
- Oculomotor apraxia is a dominant genetic trait.
- Tissue or cellular damage (lesions) to other specific parts of the brain (the premotor frontal cortex of either hemisphere, left inferior parietal lobe, and corpus callosum ), whether as a result of stroke or wounds, tumors, or dementias, may also cause apraxia.
- Individuals with degenerative dementia may also develop Apraxia.[3]
- Brain tumor[4]
Signs and symptoms[edit | edit source]
- Inability to perform movement in the absence of any physical paralysis.[5][6][7]
- Commands to move are understood, but cannot be executed.
- Movement is very clumsy, uncontrolled and inappropriate.
- Involuntary an unintentional movement is very common.
- Apraxia is sometimes accompanied by a person’s loss of ability to comprehend or use words (Aphasia)
Types of apraxia[edit | edit source]
There are two main types of apraxia:[2]-
1. Ideational apraxia
Ideational apraxia is often seen in patients with extensive left hemisphere damage, dementia, or delirium.[8]
It is an inability to perform a purposeful motor act, either automatically or on command, because the patient no longer understands the overall concept of the act, cannot retain the idea of the task, or cannot formulate the motor patterns required. Often the patient can perform isolated components of a task but cannot combine them into a complete act. Furthermore, the patient cannot verbally describe the process of performing an activity, describe the function of objects, or use them appropriately.
Cause - Ideational apraxia is thought to be in the dominant parietal lobe. This deficit also may be seen in conjunction with diffuse brain damage, such as cerebral arteriosclerosis.
Eg. When presented in the clinic with a toothbrush and toothpaste and told to brush the teeth, the patient may put the tube of toothpaste in the mouth, or try to put toothpaste on the toothbrush without removing the cap.
2. Ideomotor apraxia
In this type, the patient is unable to produce a movement on command but is able to move automatically. Thus, the patient can perform habitual tasks when not commanded to do so and often perseverates, repeating the activity over and over. It is an impaired performance of skilled motor acts despite intact sensory, motor, and language function.
Patients with ideomotor apraxia show temporal and spatial errors affecting timing, sequencing, amplitude, configuration, and limb position in space. They frequently use their limb as an object rather than demonstrating how to use the object. Patients are often able to perform the same acts without difficulty in their daily lives. This phenomenon has been called the “voluntary-automatic dissociation”
Performance may differ depending on gesture type: transitive (involving an object; eg, using a hammer) versus intransitive (eg, waving goodbye); meaningful (eg, mimicking a familiar gesture such as rubbing one’s chin) versus meaningless (eg, mimicking a novel gesture such as placing the dorsum of the hand against the contralateral cheek).[8]
Lesion area - Most frequently from lesions in the left, dominant hemisphere. here is evidence that both frontal lesions and posterior parietal lesions can result in apraxia.
Eg. The patient may fail to walk if requested to in a traditional manner. However, if a cup of coffee is placed on a table at the other end of the room and the patient is told, “Please have coffee,” the patient is likely to traverse the room to get it
3. Buccofacial apraxia
It is actually a type of ideomotor apraxia and is characterized by difficulties with performing the purposeful movements that involve facial muscles related to the mouth. It involves difficulty in responding to the commands like “pretend to blow out a candle,” or producing an orderly sequence of phonemes to produce speech.[2]
Difficulties with buccofacial apraxia seem associated with lesions in the frontal and central opercula, anterior insula, and a small area of the first temporal gyrus (adjacent to the frontal and central opercula). Although buccofacial apraxia often coexists with broca's aphasia, the two may be seen independently.
4. Conceptual apraxia
Patients with conceptual apraxia show impairment of object or action knowledge. They may misuse objects, have difficulty matching objects and actions, be unaware of the mechanical advantage afforded by tools, or be unable to judge whether a gesture is well- or ill-formed. It can be seen in patients with dementia and have been associated with lesions of posterior regions of the left hemisphere.[8]
5. Orofacial apraxia
Orofacial apraxia is characterized by an impairment of skilled movements involving the face, mouth, tongue, larynx, and pharynx (eg, blowing a kiss). Orofacial apraxia has been associated with inferior frontal, deep frontal white matter, insula, and basal ganglia lesions. Moreover, orofacial apraxia frequently coexists with limb apraxia. Based on these observations, orofacial apraxia has been considered a subtype of ideomotor apraxia. However, orofacial and limb apraxia can be dissociated, suggesting that the neural systems underlying these disorders are at least partially separable [8]
6. Limb kinetic apraxia
The term limb-kinetic apraxia has been used to describe inaccurate or clumsy distal limb movements. It is often seen in the limb contralateral to the affected hemisphere, regardless of side.. The nature of limb-kinetic apraxia has been controversial. This disorder has been associated with frontal lesions and can be difficult to differentiate from concurrent limb weakness. Limb-kinetic apraxia has also been observed in patients with neurodegenerative conditions such as CBD, progressive supranuclear palsy, and Parkinson’s disease. Limb-kinetic apraxia tends to be independent of modality (eg, verbal command versus imitation), and there is typically no voluntary-automatic dissociation.[8]
7. Verbal apraxia
It is a selective disturbance of the articulation of words and is often confused with orofacial apraxia
Other types of apraxia include:
- Constructional apraxia: Difficulty in drawing and constructing objects. Impairment in the combinatory or organizing activity in which details and relationship among the component parts of the entity must be clearly perceived.
- Developmental dyspraxia: Disorders affecting the initiation, organization and performance of actions in children.
- Modality-specific apraxias: Localized within one sensory system.
- Pantomime agnosia: Normal performance in gesture production tests both on imitation and on verbal command, but poor performance in gesture discrimination and comprehension. Patients with pantomime agnosia can imitate pantomimes they cannot recognize.
- Conduction apraxia: Superior performance on pantomime to verbal command than on pantomime imitation.
- Visuo-imitative apraxia: Normal performance on verbal command with selectively impaired imitation of gestures. Also used to designate the defective imitation of meaningless gestures combined with preserved imitation of meaningful gestures.
- Optical (or visuomotor) apraxia: Disruptions to actions calling upon underlying visual support.
- Tactile apraxia: Disturbance of transitive hand movements for use of, recognition and interaction with an object, in the presence of preserved intransitive movements.
- Effector-specific apraxias: Upper/lower face apraxia - Impairment in performing actions with parts of the face. Oral apraxia Inability to perform skilled movements with the lips, cheeks and tongue.
- Lid apraxia: Difficulty with opening the eyelids.
- Ocular apraxia: Impairment in performing saccadic eye movements on command.
- Trunk (or axial) apraxia: Difficulty with generating body postures
- Leg apraxia: Difficulty with performing intentional movements with the lower limbs.
- Task-specific apraxias - Gait apraxia: Impaired ability to execute the highly practised, co-ordinated movements of the lower legs required for walking.
- Gaze apraxia: Difficulty in directing gaze.
- Apraxic agraphia: A condition in which motor writing is impaired but limb praxis and non-motor writing (typing, anagram letters) are preserved.
- Dressing apraxia: Inability to perform the relatively complex task of dressing.
- Dyssynchronous apraxia: Failure to combine simultaneous preprogrammed movements.
- Orienting apraxia: Difficulty in orienting one’s body with reference to other objects.
- Mirror apraxia: A deficit in reaching to objects presented in a mirror.
- Lesion-specific apraxias: Callosal apraxia - Apraxia caused by damage to the anterior corpus callosum that usually affects the left limb.
- Sympathetic apraxia Apraxia - of the left limb due to damage to the anterior left hemisphere (the right hand being partially or fully paralyzed).
- Crossed apraxia: The unexpected pattern of apraxia of the right limb following damage to the right hemisphere[9].
Diagnosis[edit | edit source]
- Many patients with apraxia present with aphasia and it may be sometimes difficult to distinguish.
- Various bedside tasks are used to evaluate apraxia which may include ADLs and physical performances.
- Hand gestures, finger gestures, and pantomime are used to diagnose apraxia.
- Electroencephalogram (EEG) is performed to map brain activity.
- Spinal tap may be done to check for inflammation or an infection that affects the brain
Outcome measures[edit | edit source]
- For Ideomotor and Ideational Apraxia - Goodglass and Kaplan test for apraxia is composed of universally known movements, such as blowing, brushing teeth, hammering, shaving, and so forth. It is based on what the authors consider a hierarchy of difficulty for patients with apraxia Additional apraxia tests may be found in Butler and the work of van Heugten et al,171 who have adapted the Arnadottir OT-ADL Neurobehavioural Evaluation (A-ONE) as an observational method of testing for apraxia.[2]
- For Upper Limb Apraxia -Apraxia screen of TULIA (AST), Cologne apraxia screening (CAS)
Differential Diagnosis[edit | edit source]
- Agnosia
- Aphasia
- Hemiparesis
- Movement disorders such as Parkinson disease and dystonia
- Alzheimer disease
- Progressive supranuclear palsy
Treatment[edit | edit source]
Medical management
Medicines are not known to be effective for the treatment of ideomotor apraxia.
Physiotherapy management
- Remedial approach: In the remediation of apraxias, it is advised that the therapist speak slowly and use the shortest possible sentences. One command should be given at a time, and the second command should not be given until the first task is completed. When teaching a new task, it should be broken down into its smaller parts. One component is taught at a time, physically guiding the patient through the task if necessary. It should be completed in precisely the same manner each time. When all the individual units are mastered, an attempt to combine them should be made. A great deal of repetition may be necessary. Family members must be advised to use the exact approach found to be successful in the clinic. Performing activities in as normal an environment as possible is also helpful. Butler provides a case example of a young woman relearning how to drink from a cup using this technique. Using the sensorimotor approach, multiple sensory inputs are used on the affected body parts to enhance the production of appropriate motor responses.[2]
- Compensatory approach: Strategy training involves teaching the patient compensatory techniques to overcome the apraxia such as use of pictures in the correct sequence to support ADL skills. his approach has been developed further and is now widely used to help patients overcome apraxia
- Activities to improve coordination and balance can be incorporated.
- Strategy training for daily activities (i.e. teaching specific strategies to overcome the difficulties to patient experiences)
- Gesture training (i.e. relearning gestures)
- Direct ADL training (i.e. relearning – or learning new ways to perform – daily tasks)
References[edit | edit source]
- ↑ Zeidman LA. Brain science under the swastika: ethical violations, resistance, and victimization of neuroscientists in Nazi Europe. Oxford University Press; 2020 May 25.
- ↑ 2.0 2.1 2.2 2.3 2.4 O'Sullivan SB, Schmitz TJ, Fulk G. Physical rehabilitation. FA Davis; 2019 Jan 25.
- ↑ Parker H. Apraxia: Symptoms, causes, tests, treatments. WebMD. WebMD; 2021 June 7 Available from: https://www.webmd.com/brain/apraxia-symptoms-causes-tests-treatments
- ↑ 4.0 4.1 Apraxia: Medlineplus medical encyclopedia. MedlinePlus. U.S. National Library of Medicine. Available from: https://medlineplus.gov/ency/article/007472.htm
- ↑ De Renzi E, Faglioni P. Apraxia. InHandbook of clinical and experimental neuropsychology 2020 Mar 6 (pp. 421-440). Psychology press.
- ↑ Denny-Brown D. The nature of apraxia. Journal of Nervous and Mental Disease. 1958.
- ↑ Apraxia. NORD (National Organization for Rare Disorders). Available from: https://rarediseases.org/rare-diseases/apraxia/#:~:text=Apraxia%20is%20a%20neurological%20disorder,simply%20cannot%20execute%20the%20act.
- ↑ 8.0 8.1 8.2 8.3 8.4 Gross RG, Grossman M. Update on apraxia. Current neurology and neuroscience reports. 2008 Nov;8(6):490-6.
- ↑ Petreska B, Adriani M, Blanke O, Billard AG. Apraxia: a review. Progress in brain research. 2007 Jan 1;164:61-83.