Sleep: Theory, Function and Physiology
Original Editor - Wanda van Niekerk
Top Contributors - Wanda van Niekerk, Lucinda hampton, Kim Jackson, Admin and Tarina van der Stockt
Introduction[edit | edit source]
Sleep is an important part of our daily routine. It is estimated that we spend about a third of our time sleeping.
- Quality sleep is just as important for good health as proper nutrition and physical activity.
- Sleep is important to many brain functions, we need sleep to learn effectively and it has been shown that a lack of sleep affects our concentration levels negatively.
- Evidence also shows that sleep affects almost every type of tissue and system in the body and that a chronic lack of sleep can increase the risk for non-communicable diseases such as hypertension, diabetes, cardiovascular disease and obesity.
Sleep is vital to good health!
What is Sleep?[edit | edit source]
Sleep can be defined as “an active state of unconsciousness produced by the body where the brain is in a relative state of rest and is reactive primarily to internal stimulus."[2] Sleep is characterised by:
- low physical activity levels
- reduced sensory awareness
Sleep is also regulated by the circadian rhythm and homeostatic mechanisms. Furthermore, certain brain activity patterns, as well as the different phases of sleep can be visualised using electroencephalography(EEG).
Multiple areas in the brain work together to control sleep-wake cycles. Some of these areas include the:
- Thalamus
- Hypothalamus - contains the Suprachiasmatic nucleus (SCN) - the body's biological clock, and in conjunction with the thalamus it regulates slow-wave sleep[3]
- Pons - important in the regulation of rapid eye movement(REM) sleep
During sleep, several endocrine glands secrete and regulate hormones such as:
- Melatonin - involved in the regulation of biological rhythms and the immune system[4]
- Follicle-stimulating hormone (FSH) -secreted by the pituitary gland and key in regulating the reproductive system[5]
- Luteinising hormone (LH) - secreted by the pituitary gland and key in regulating the reproductive system[5]
- Growth hormone - secreted by the pituitary gland and has a role in physical growth and maturation[6]
History of Sleep Science[edit | edit source]
The science of sleep has come a long way and has changed significantly over the years. Initially, sleep was considered as a near-death experience.
- Aristotle investigated the concept of sleep and wrote about it in “On sleep and sleepiness." Aristotle was of the view that falling asleep involved the digestion of food particles. These food particles then created vapours which rose from the stomach and accumulated in the brain. These vapours then led to the onset of sleep.
- Other schools of thought in the 18th and 19th century were that sleep was the result of a lack of blood supply to the brain or the total opposite and that sleep was caused by an excess of blood in the brain.[8]
Sleep was also initially considered to be a passive state, but with the creation of the Electroencephalogram (EEG) by Hans Berger in the late 1920s proved otherwise.[9]
- The EEG allows for the objective measurement of brain activity during sleep and showed that there are different patterns of brain activity during periods of sleep and wakefulness.[10]
- The notion of sleep as a passive state was therefore disregarded.
- The EEG also clearly shows that the mind remains active during sleep and during certain phases of sleep there are increased levels of activity.
Concepts around Sleep[edit | edit source]
Sleepiness - “inclined to sleep, having difficulty in keeping awake, drowsy, somnolent” or “ drowsiness, sleep propensity and decreased alertness”[11]
- Subjective feelings of sleep may include:
- difficulty keeping eyes open
- the tendency to stay at rest
- to be slower
Fatigue – “overwhelming sense of tiredness, lack of energy and a feeling of exhaustion, associated with impaired physical and/or cognitive functioning.”
- Fatigue is associated with physical and mental exertion and the inability to continue performing a task.[11]
Physical fatigue is a physiological phenomenon, characterised by “time on task” (i.e the time spent performing a specific task at home or at work).
- Physical fatigue is also associated with a decrement in performance of a specific task and this fatigue is often relieved through changing the task.[8]
Mental fatigue is closely linked to getting sufficient rest – this includes sleep, but not just sleep, it may be just getting some rest or a break from a specific task.[8]
- Cognitive load theory refers to the amount of information that working memory can hold at one time. Working memory has a limited capacity. Cognitive load theory is thus the idea that you are not working over your cognitive working load capacity and that you are therefor working within a capacity that is stimulating enough not to bore you.[12]
Tiredness – refers to a lack of energy and initiative and may be improved by rest and proper nutritional intake for example.[8]
Sleep Regulation[edit | edit source]
Sleep is regulated by two systems, the circadian rhythm and sleep/wake homeostasis.
- The circadian rhythm synchronises biological rhythms, including sleep, over a cycle of 24 hours.
- Sleep/wake homeostasis describes the body’s internal neurophysiologic drive toward either sleep or waking.[13]
Homeostasis refers to principles of equilibrium or balance and the body is driven towards a balance between sleep and wakefulness i.e. a neurophysiological drive to sleep is evident after long periods of wakefulness and there is a neurophysiological drive to wakefulness after long periods of sleep.
Function of Sleep[edit | edit source]
Several theories have been proposed to explain the function of sleep and why it is necessary. These theories include the restorative theory of sleep, the cognitive theory of sleep; the energy conservation theory of sleep and the adaptive theory of sleep.
Restorative Theory[edit | edit source]
This theory supports the notion that sleep is necessary to revitalise and restore the physiological processes that help in rejuvenating the body and mind. With this theory, it is postulated that NREM sleep is important for restoring physiological functions and REM sleep is important in the restoration of mental functions.[15]
Findings of many biological functions occurring primarily during sleep support the restorative theory of sleep. Some of these functions include:
- Muscle repair
- Cell repair
- Tissue growth
- Protein synthesis
- Release of many of the important hormones for growth
Sleep therefore allows for the body to repair and replete several cellular components that are needed for physiological functions and that become depleted during the day. This supports the concept of allowing our patients to get sufficient rest after surgeries in order to promote efficient recovery processes.
Cognitive Function Theory[edit | edit source]
Sleep is important for cognitive function and memory formation. Studies on sleep deprivation show disruption in cognition and also indicate memory deficits.[16] These disruptions lead to[16]:
- Impairment in the attention-maintaining ability
- Impairments in decision making
- Difficulty recalling long-term memories
These types of disruptions are also positively correlated to the amount of sleep deprivation, the impairments become more severe as the sleep deprivation time increases.[16]
It has also been shown that slow-wave sleep (NREM N3) after learning a new task has the ability to improve resultant performance on that task. Stickgold (2005) also showed that slow-wave sleep is vital for effective memory formation.[17] It is therefore not the best idea to stay up all night studying for a test, as it may not be effective and may even be counterproductive.
Energy Conservation Theory[edit | edit source]
Sleep has been implicated as a means of energy conservation. The energy conservation theory suggests that the main function of sleep is to reduce energy demand during a part of the day and night. The fact that the body has a decreased metabolism of up to 10% during the sleep, supports this theory. Body temperature and calorie demand drop during sleep and increase when we are awake, again supporting the hypothesis that sleep plays an important role in helping to conserve energy resources.[19]
Adaptive Theory[edit | edit source]
The adaptive theory is also referred to as the evolutionary theory of sleep or the inactivity theory. It is one of the earliest theories that explain the function of sleep. This theory suggests that sleep is a behaviour which enhances our overall survival. It has been suggested that human beings evolved at a faster rate compared to other species due to our focus on getting rest.
- This theory suggests that all species have adapted to sleep during periods of time when wakefulness will put them more at risk of danger eg that sleep is an adaptive behavior to keep us away from night and darkness when predator species enjoy advantage in vision and stealth.[15]
- Similar to hunger and thirst, sleepiness may represent an underlying physiological need which is only satisfied by sleeping and it’s integral to survive of individuals.[8]
Physiology of Sleep[edit | edit source]
Assessment of Sleep[edit | edit source]
Medical Assistance Methods[edit | edit source]
Different studies can be used in sleep laboratories to assess sleep. The advantages of these methods include:
- The use of advanced technology (cannot be used at home)
- Precise and discrete methods – can distinguish between different sleep phases
- Gold standard for sleep evaluation
The disadvantages are:
- Expensive methods
- Time-consuming methods
- Require professional assistance
- Can only be done over a short period of time (one or two days)
- Another important functional disadvantage is that the assessment in a sleep laboratory is not done in the usual seep context of the patient at home, therefore it does not really measure a normal sleep situation.
Polysomnogram (PSG): Medical procedure composed of several concurrent but independent tests that monitor different body functions during sleep and that are recorded for their later study using different channels[20]
Tests and information gathered in a PSG can include[20]:
- Electroencephalogram (EEG) – measures and records brainwave activity – used to identify sleep stages and detect seizure activity
- Electrooculogram (EOG) – records eye movements. Important for identifying the different sleep stages, especially the REM stage
- Electromyogram (EMG) – records muscle activity such as teeth grinding and face twitches and limb movements. Chin EMG is needed to differentiate REM from wakefulness and limb EMG identifies periodic limb movements during sleep (PLMS)
- Electrocardiogram (EKG) – heart rate and rhythm
- Pulse oximetry – oxygen saturation (SaO2)
- Respiratory monitor – respiratory effort
- Capnography – measures and displays inhaled and exhaled CO2 concentrations at the airway opening
- Transcutaneous monitors – O2 and CO2 diffusion through the skin
- Microphone – records snoring volume and kind
- Video camera – good to identify body motion and position
- Thermometer – core body temperature and changes
- Light Intensity Tolerance Test – investigates the influence of light intensity on sleep
- Esophageal tests
- Nasal and oral airflow sensor – records airflow and breathing rate
- Blood pressure monitor – measures blood pressure and changes in it
The above list is an exhaustive list of tests that can be used, generally, only some specific tests are selected for each specific case. The EEG, EOG and EMG, however, are the key outcome measures.
Other Medical Assistance tests include[20]:
- Multiple Sleep Latency Test (MLST)
- Maintenance of wakefulness test (MWT)
- CPAP titration test (CTT)
- Home Sleep Test (HTS)
Self-Assessment Methods[edit | edit source]
- Sleep questionnaires[20]
- Sleep diaries
- Hardware devices such as sleep detection apps
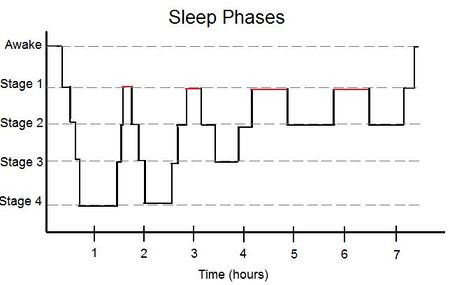
Sleep Stages[edit | edit source]
Sleep can be divided into two sleep states or types and there is a sequential rotation between these two sleep states several times (5 to 6 times) during a night. These rotations are generally between 90 to 100 minutes per cycle. These two major phases of sleep are:
- Rapid eye movement (REM) sleep
- Non- rapid eye movement (NREM) sleep.
The increasingly longer and deeper REM stages generally occur during the latter part of the sleep cycle.
- There is no sleep stage division of REM
- NREM sleep consists out of three or four main subdivisions.
- Rechtschaffen and Kales published standardised criteria for the staging of sleep in 1968.[21]
- The American Academy of Sleep medicine revised these criteria and published the revised version in 2007.[22]
- Main change: combining of stage three and four into a single-stage – defined now as slow-wave sleep or deep sleep (for the purpose of this page, reference will be made to the American Academy of Sleep classification).
Polysomnography is used to identify and categorise the different sleep states.[23]
- Non-rapid eye movement (NREM) sleep is subdivided into three stages (N1, N2 and N3) of increasing sleep depth.[2][24]
NREM Sleep Stage 1 (N1)[edit | edit source]
- Transitional phase between wakefulness and sleep (the period during which we drift off to sleep)
- Shallow stage of sleep
- Reduced respiration rate
- Reduced heartbeat
- Brain wave activity (EEG)[23]
- Associated with alpha and theta waves
- Earlier in N1 – alpha waves, low frequency (8-13 Hz), high amplitude patterns of electrical activity (waves) that become synchronised
- This brain wave activity pattern is like someone who is very relaxed, but awake
- Further on in stage N1 – increase theta wave activity
- Theta waves – lower frequency (4 -7 Hz), higher amplitude brain waves
- Easy to wake someone from stage 1
- Lasts around 5 -10 minutes
NREM Sleep Stage 2 (N2)[edit | edit source]
- the body goes into a deep relaxation state
- the onset of sleep
- drop in body temperature
- heart rate slows down
- the brain produces sleep spindles
- people are less aware of their surroundings
- lasts around 20 minutes
- Brain wave activity[23]
- Theta waves still dominant, but interrupted by sleep spindles (rapid burst of higher frequency brain waves – these may be important for learning and memory)
- K-complexes also during this stage (very high amplitude pattern of brain activity that may occur in response to environmental stimuli – may serve as a bridge to higher levels of arousal in response to what is going on in our environments)
- Sleep spindles and K-complexes help to distinguish between NREM N1 and N2
NREM Sleep Stage 3 (N3)[edit | edit source]
Revised combination of previous stage 3 and 4 according to Rechtschaffen and Kales[22] Also known as slow-wave sleep (SWS)
- Muscles relax
- Blood pressure drops
- Breathing rate drops
- Deepest sleep occurs
- People are less responsive
- Noises and activity in the surrounding environment may fail to generate a response
- Transitional period between light sleep and very deep sleep
- Lasts about 20 to 40 minutes[26].
- Brainwaves [23] - low frequency (up to 4Hz), high amplitude delta waves
REM Sleep[edit | edit source]
- Eyes move rapidly under closed eyelids
- Brain becomes more active
- Low amplitude, mixed frequency EEG (similar to an awake pattern)
- Desynchronized EEG activity
- Body becomes relaxed and immobilised
- Muscle atonia or paralysis
- Dreams occur
- Also referred to as paradoxical sleep because while the brain and other body systems become more active, muscles become more relaxed[27].
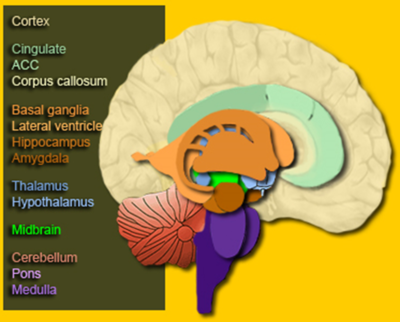
Anatomy of Sleep[edit | edit source]
Structures of the brain that are involved with sleep include[28][24]:
- Hypothalamus
- small structure deep inside the brain
- Contains groups of nerve cells that act as control centres for sleep and arousal
- Suprachiasmatic nucleus
- Lies within the hypothalamus
- Clusters of thousands of cells that receive information about light exposure from the eyes
- Brain Stem
- At the base of the brain
- Communicates with the hypothalamus to control the transition between wakefulness and sleep
- Includes the pons, medulla and midbrain
- Contains sleep-promoting cells (also within the hypothalamus) – these cells produce GABA (a brain chemical) which acts to reduce the activity of arousal centres in the hypothalamus and the brain stem
- The pons and medulla play a key role in REM sleep by sending signals to relax the muscles that are needed for posture and limb movements – this is to ensure that we don’t act out our dreams.
- Thalamus
- acts as a relay for sensory information to the cerebral cortex (part of the brain that interprets and processes information from short- to long-term memory)
- Quiet through most stages of sleep in order to tune out the external world
- Active during REM
- sends images, sounds and other sensations that fill our dreams to the cerebral cortex
- Pineal gland
- located within the brain’s two hemispheres
- Receives signals from SCN and increases melatonin production which helps put a person to sleep once the lights go down
- Basal forebrain
- near front and bottom of the brain
- promotes sleep and wakefulness
- cells in the basal forebrain release adenosine which supports sleep drive
- Midbrain
- Acts as an arousal system
- Amygdala and Hippocampus
- Structures of the limbic system
- Involved in the processing of emotions
- Increasingly active during REM sleep
- Lateral prefrontal cortex
- Involved in thought and judgement thus logical reasoning
- Deactivates during REM (this might be why we have bizarre, illogical dreams and struggle to comprehend why we have them).
- Anterior cingulate gyrus
- Governs attention and motivation
- More active during REM sleep
- May be part of the reason that we have such vivid and changeable images in our dreams
Resources[edit | edit source]
References[edit | edit source]
- ↑ The Economist. What happens when we sleep. Published 30 January 2019. Available from https://www.youtube.com/watch?v=eTgNgGO_bLs (last accessed 17 July 2020)
- ↑ 2.0 2.1 Brinkman JE, Sharma S. Physiology, sleep. InStatPearls [Internet] 2019 Mar 16. StatPearls Publishing.
- ↑ Luppi PH, Fort P. Sleep–wake physiology. In Handbook of Clinical Neurology 2019 Jan 1 (Vol. 160, pp. 359-370). Elsevier.
- ↑ Hardeland R, Pandi-Perumal SR, Cardinali DP. Melatonin. The international journal of biochemistry & cell biology. 2006 Mar 1;38(3):313-6.
- ↑ 5.0 5.1 Christensen AS, Clark A, Salo P, Nymann P, Lange P, Prescott E, Rod NH. Symptoms of sleep disordered breathing and risk of cancer: a prospective cohort study. Sleep. 2013 Oct 1;36(10):1429-35.
- ↑ Smiley A, Wolter S, Nissan D. Mechanisms of Association of Sleep and Metabolic Syndrome. J Med-Clin Res & Rev. 2019;3(3):1-9.
- ↑ Neuro Transmissions. What is sleep? Published on 23 February 2015. Available from https://www.youtube.com/watch?v=mjTFFtCvOqc (last accessed 17 July 2020)
- ↑ 8.0 8.1 8.2 8.3 8.4 Whelehan, D. The theory, function and physiology of sleep. Course, Plus 2020.
- ↑ Mecarelli O. Past, Present and Future of the EEG. InClinical Electroencephalography 2019 (pp. 3-8). Springer, Cham.
- ↑ Yao D, Qin Y, Hu S, Dong L, Vega ML, Sosa PA. Which reference should we use for EEG and ERP practice?. Brain topography. 2019 Jul 1:1-20.
- ↑ 11.0 11.1 Greenberg S, Aislinn P, Kirsten D. Development and validation of the fatigue state questionnaire: Preliminary findings. The Open Psychology Journal. 2016 Jun 30;9(1).
- ↑ Mindtools. Cognitive Load Theory. Helping People Learn Effectively. Available from https://www.mindtools.com/pages/article/cognitive-load-theory.htm (last accessed 16 July 2020)
- ↑ Bathory E, Tomopoulos S. Sleep regulation, physiology and development, sleep duration and patterns, and sleep hygiene in infants, toddlers, and preschool-age children. Current problems in pediatric and adolescent health care. 2017 Feb 1;47(2):29-42.
- ↑ All Health TV. Functions of Sleep. Published on 21 November 2018. Available from https://www.youtube.com/watch?v=taz17X8oCog (last accessed 17 July 2020)
- ↑ 15.0 15.1 Ezenwanne EB. Current concepts in the neurophysiologic basis of sleep; a review. Annals of medical and health sciences research. 2011;1(2):173-80.
- ↑ 16.0 16.1 16.2 Hudson AN, Van Dongen HP, Honn KA. Sleep deprivation, vigilant attention, and brain function: a review. Neuropsychopharmacology. 2020 Jan;45(1):21-30.
- ↑ Stickgold R. Sleep-dependent memory consolidation. Nature. 2005 Oct;437(7063):1272-8.
- ↑ TED-Ed. What would happen if you didn't sleep? - Claudia Aquirre. Published on 12 November 2015. Available from https://www.youtube.com/watch?v=dqONk48l5vY&t=172s (last accessed 17 July 2020)
- ↑ Northeast RC, Vyazovskiy VV, Bechtold DA. Eat, sleep, repeat: The role of the circadian system in balancing sleep-wake control with metabolic need. Current Opinion in Physiology. 2020 Feb 28.
- ↑ 20.0 20.1 20.2 20.3 Ibáñez V, Silva J, Cauli O. A survey on sleep assessment methods. PeerJ. 2018 May 25;6:e4849.
- ↑ Moser D, Anderer P, Gruber G, Parapatics S, Loretz E, Boeck M, Kloesch G, Heller E, Schmidt A, Danker-Hopfe H, Saletu B. Sleep classification according to AASM and Rechtschaffen & Kales: effects on sleep scoring parameters. Sleep. 2009 Feb 1;32(2):139-49.
- ↑ 22.0 22.1 Iber C, Ancoli-Israel S, Chesson AL, Quan SF. The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. Westchester, IL: American academy of sleep medicine; 2007 Jan.
- ↑ 23.0 23.1 23.2 23.3 Armon, C. Polysomnography. Available from https://emedicine.medscape.com/article/1188764-overview#a4 Updated 29 April 2020. (last accessed 17 July 2020)
- ↑ 24.0 24.1 National Institute of Neurological Disorders and Stroke. Brain Basics: Understanding Sleep. Available from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Understanding-Sleep (last accessed 17 July 2020)
- ↑ Neuroscientifically Challenged. 2-Minute Neuroscience: Stages of Sleep. Published on 18 August 2018. Available from https://www.youtube.com/watch?v=iWo90uxkNM0 (last accessed 17 July 2020)
- ↑ UHMS Stages of sleep Available from:https://www.uofmhealth.org/health-library/hw48331 (last accessed 4.10.2020)
- ↑ Siegel JM. REM sleep: a biological and psychological paradox. Sleep Med Rev. 2011;15(3):139-42. doi:10.1016/j.smrv.2011.01.001
- ↑ Izac MS. Basic anatomy and physiology of sleep. American journal of electroneurodiagnostic technology. 2006 Mar 1;46(1):18-38.
- ↑ NEI Psychopharm. Sleep/Wake Cycles. Published on 15 March 2019. Available from https://www.youtube.com/watch?v=llS2sPKHwGU&t=124s (last accessed 17 July 2020)
- ↑ TED. Matt Walker. Sleep is your Superpower. Published 3 June 2019. Available from https://www.youtube.com/watch?v=5MuIMqhT8DM (last accessed 17 July 2020)