Immunotherapy
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Vidya Acharya and Kim Jackson
Introduction[edit | edit source]
Immunotherapy is a relatively new form of treatment whereby the immune system is modulated to control diseases, for example autoimmune disease, allergies, or cancer. Therapies include immunosuppressants, biologicals (e.g. cytokines, monoclonal antibodies), vitamins and minerals (e.g., zinc, vitamin C, and vitamin B6), transplantation (e.g., bone marrow) and oncolytic viruses and cancer vaccines.[1][2][3]
Uses[edit | edit source]
Immunotherapy is used to treat certain types of cancer. It is also used to treat inflammatory diseases eg.:
- Rheumatoid Arthritis
- Inflammatory Bowel Diseases, including ulcerative colitis and Crohn's disease
- Multiple Sclerosis (MS)
- Psoriasis[3]
Immunotherapy can be used to suppress the immune system. This is particularly helpful in autoimmune disorders when it wrongly attacks normal tissues.
Inflammation (useful for fighting infection) is overproductive in autoimmune diseases and it damages normal tissues. Biological therapies can cool off this harmful inflammation (see DMARDs and BDMARDs).
The video below (9 minutes) is a useful watch.
Types of Cancer Immunotherapy[edit | edit source]
NB: Not exhaustive list
Monoclonal antibodies (MABs)[edit | edit source]
- Monoclonal antibodies are made in a laboratory to boost the body’s natural antibodies or act as antibodies themselves.
- Monoclonal antibodies can help fight cancer in different ways. eg can be used to block the activity of abnormal proteins in cancer cells (known as a targeted therapy), or cancer treatment that targets a cancer’s specific genes, proteins, or the tissue environment that helps the tumor grow and survive[5].
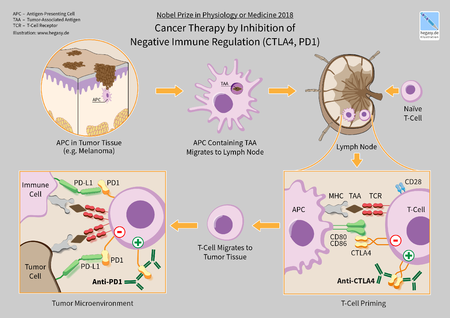
Checkpoint Inhibitors[edit | edit source]
- Cancer cells can find ways to hide from the immune system by activating these checkpoints. These drugs basically take the ‘brakes’ off the immune system, which helps it recognize and attack cancer cells[6]. Common checkpoints that these inhibitors affect are the PD-1/PD-L1 and CTLA-4 pathways. Examples of immune checkpoint inhibitors are: Ipilimumab (Yervoy); Nivolumab (Opdivo)[5].
- Checkpoint inhibitors are used to treat cancers such as melanoma skin cancer and lung cancer. Researchers are also looking at them in clinical trials for other types of cancer.
Cytokines[edit | edit source]
- This treatment uses cytokines (small proteins that carry messages between cells) to stimulate the immune cells to attack cancer.[6]
- Cytokines are a group of proteins that are found naturally in the body.
- They help to boost the immune system.
- Man made versions of these proteins have been developed as a treatment for cancer.
Donor lymphocyte therapy (DLI)[edit | edit source]
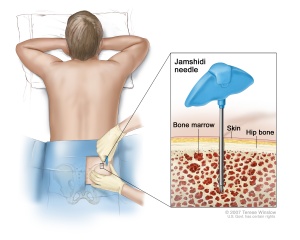
DLI involves the infusion of lymphocytes from a donor to a patient who has already had an allogenic bone marrow transplant from the same donor. The donor lymphocytes may assist in identifying targets for immune system attack. This can induce remission or potentially prevent relapse in patients who are at high risk for relapse after bone marrow transplant. DLI can also cause graft versus host disease (GVHD), a potentially serious side effect in which the recipient’s cells/tissues are attacked by the donor immune cells[7].
Radioimmunotherapy[edit | edit source]
This is a combination of a monoclonal antibody and a radiation source. This results in radiation being delivered directly to the specific tumor cells, but often in lower doses and over a longer period of time. An example is ibritumomab tiuxetan (Zevalin®)[7].
Vaccines to treat cancer[edit | edit source]
- Vaccines are substances put into the body to start an immune response against certain diseases. We usually think of them as being given to healthy people to help prevent infections[6].
- Some vaccines can help prevent or treat cancer.
- The HPV and hepatitis B vaccines are preventive vaccines. They work by preventing an infection that might lead to cancer. Viruses, however, do not cause most cancers. The challenge for researchers is to use the model of the immune response to viral infection of cells to develop vaccines for cancers not caused by viruses. ie a therapeutic cancer vaccine that would be used to treat cancer after it has already appeared. There are two main types of such therapeutic vaccines: autologous vaccines and allogenic vaccines[8].
- Researchers must carefully evaluate which cancers are most suitable for a therapeutic vaccine approach. Generally, the cancers that are the best candidates are those whose treatments are associated with high costs and therapies that are less effective, or therapies that involve the risk of serious side effects for the patient. Cancers such as lung cancer, pancreatic cancer, and breast cancer are such candidates for vaccine therapy.
- Much study, insight, and skill will be needed to develop these vaccines[8].
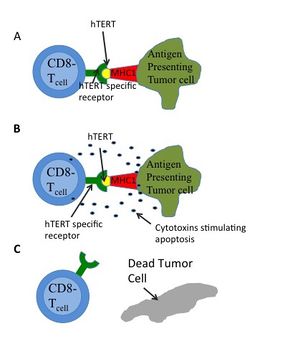
CAR (chimeric antigen receptor) T-cell therapy[edit | edit source]
- This therapy takes some T-cells from a patient's blood, mixes them with a special virus that makes the T-cells learn how to attach to tumor cells, and then gives the cells back to the patient so they can find, attach to, and kill the cancer.
- This type of immunotherapy is still quite new and researchers are looking into how well it works as a treatment for cancer.
Oncolytic viruses[edit | edit source]
- This treatment uses viruses that have been modified in a lab to infect and kill certain tumor cells[6].
Benefits[edit | edit source]
- Only a tiny minority of patients expected to die from cancer will benefit from immunotherapy.
- Immunotherapies have been used for a hundred years eg the deliberate injection of bacteria into the body to stimulate the immune system,
- 2011 marked the approval of the first immunotherapy for cancer, a checkpoint inhibitor named ipilimumab (Yervoy). This class of drugs unleashes the body’s immune system against cancer, and is the subject of much enthusiasm.
- When immunotherapy works the results are terrific.
- Patients with otherwise life-threatening cancers live far longer than expected and some may even be cured by immunotherapy however today few patients can expect to be among the lucky ones.
- Several common cancers, like colon and breast cancer, these drugs work poorly for[9].
- The ability to manipulate components of the immune system with drugs and to manipulate and activate an individual patient’s cells in the laboratory are the areas with great interest and activity now,” said Clifford A. Hudis, MD, the chief of breast cancer medicine service at Memorial Sloan Kettering Cancer Center in New York City, although he warned that clinicians should avoid creating unreasonable expectations among patients.
- The key point physicians have to convey to lay audiences is the power of the immune system and the fact that manipulating it can cause significant toxicities that require expert management. It is not as simple as stimulating the immune system, a misleading phrase that many patients find attractive,[10]
References[edit | edit source]
- ↑ Radiopedia Immunotherapy Available:https://radiopaedia.org/articles/immunotherapy?lang=us (accessed 20.1.2023)
- ↑ Justiz AV, Zito PM. Immunotherapy.22.6.2020 Available from: https://www.ncbi.nlm.nih.gov/books/NBK519046/(last accessed 4.9.2020)
- ↑ 3.0 3.1 Drugs.com Immunotherapy Available from:https://www.drugs.com/health-guide/immunotherapy.html (last accessed 4.9.2020)
- ↑ Society for immunotherapy of cancer Immunotherapy Available fromhttps://www.youtube.com/watch?v=UbFjiWOBErA&app=desktop (last accessed 5.9.2020)
- ↑ 5.0 5.1 Cancer net Immunotherapy Available from:https://www.cancer.net/navigating-cancer-care/how-cancer-treated/immunotherapy-and-vaccines/understanding-immunotherapy (last accessed 4.9.2020)
- ↑ 6.0 6.1 6.2 6.3 ACS Immunotherapy Available from:https://www.cancer.org/treatment/treatments-and-side-effects/treatment-types/immunotherapy/what-is-immunotherapy.html (last accessed 4.9.2020)
- ↑ 7.0 7.1 Oncolink Immunotherapy Available from:https://www.oncolink.org/cancer-treatment/immunotherapy/all-about-immunotherapy (last accessed 5.9.2020)
- ↑ 8.0 8.1 Dermime S, Armstrong A, Hawkins RE, Stern PL. Cancer vaccines and immunotherapy. British medical bulletin. 2002 Jul 1;62(1):149-62.Available from:https://www.historyofvaccines.org/content/articles/cancer-vaccines-and-immunotherapy (last accessed 4.9.2020)
- ↑ Gay N, Prasad V. Few people actually benefit from ‘breakthrough’cancer immunotherapy. STAT. 2017 Mar 8.Available from:https://www.statnews.com/2017/03/08/immunotherapy-cancer-breakthrough/(last accessed 4.9.2020)
- ↑ Targeted Ongology A Brief History of Immunotherapy Available from:https://www.targetedonc.com/view/a-brief-history-of-immunotherapy (last accessed 4.9.2020)