Rehabilitation Phases
Original Editors - Naomi O Reilly, Khloud Shreif and ReLAB-HS
Top Contributors - Naomi O'Reilly, Shaimaa Eldib, Kim Jackson, Lucinda hampton, Tarina van der Stockt, Tony Lowe, Oyemi Sillo, Jess Bell, Ashmita Patrao and Aminat Abolade
Introduction[edit | edit source]
There is a growing need for rehabilitation within health systems as the worldwide population is increasing. According to the World Health Organisation (WHO) 1 in 3 people need to access rehabilitation.[1][2], yet there are more than 50% of people who need rehabilitation in low and middle-income countries that do not receive access to rehabilitation. The type of care and rehabilitation needs will vary hugely dependant on a number of factors that are influenced specifically by both the acuity of the condition and the complexity of the condition. The type of care will vary to cover the individual's needs, ranging from acute care in acute illness/injury or exacerbation of a current condition that requires the need for rapid intervention, through to sub-acute care and long term care when the individual's condition is more stable.
Acute Care[edit | edit source]
A reasonable working definition of acute care should include the most time-sensitive, individually-oriented diagnostic and curative actions whose primary purpose is to improve health and as such, the proposed definition includes the health system components, or care delivery platforms, used to treat sudden, often unexpected, urgent or emergent episodes of injury and illness, regardless of their ultimate cause, that can lead to death or disability without rapid intervention. Acute care plays a vital role in the prevention of death and disability and the integration of acute care with preventive and primary care completes a healthcare system paradigm that fully encompasses all essential aspects of health care delivery.
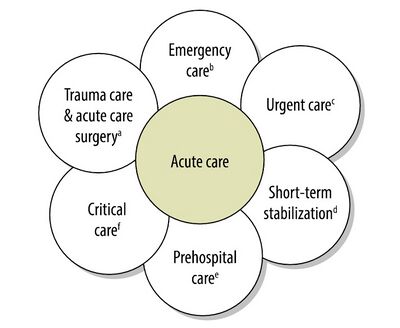
Acute care encompasses a range of clinical health-care functions, including urgent care, pre-hospital emergency care, emergency or trauma care, acute care surgery, critical care and short-term inpatient stabilization. It may require a visit or stay in an urgent care centre, hospital emergency department, or other short-term stay facilities, along with the assistance of diagnostic services, surgery, or follow-up outpatient care in the community. Hospital-based acute inpatient care typically has the goal of discharging patients as soon as they are deemed healthy and stable. Many simple, effective and inexpensive acute care interventions can be life-saving, often within the first 24 hours. Among them are those that are provided at basic surgery wards in district hospitals offering treatment for trauma, high-risk pregnancy and other common surgical conditions[3]
Acute care settings include the emergency department, intensive care, coronary care, cardiology, neonatal intensive care, and many general areas where the patient could become acutely unwell and require stabilization prior to transfer to another higher dependency unit for further treatment. [4][3]
Where Acute Care Occurs[edit | edit source]
a. Trauma Care & Acute Care Surgery[edit | edit source]
Treatment of individuals with acute surgical needs, such as life-threatening injuries, acute appendicitis or strangulated hernias or intestinal obstruction (the most common cause of hospital admission). [3][5]
b. Emergency Care[edit | edit source]
Treatment of individuals with acute life- or limb-threatening medical and potentially surgical needs, such as acute myocardial infarctions or acute cerebrovascular accidents, or evaluation of patients with abdominal pain. [3] May be carried out by General Practitioners (GPs,) to prevent irreversible complications but frequently occurs at an emergency department in a hospital: where they can assess the airway, breathing, circulatory, and treat critically ill people to stabilize their condition. Depending on the degree of severity, some cases can be managed exclusively within the emergency department while others will be referred onward to receive specialist care.
c. Urgent Care[edit | edit source]
Walk-in care in a facility delivering medical care outside a hospital emergency department, usually on an unscheduled, walk-in basis such as within a minor injury unit, for example, treatment of minor injury (sprain, strain, fracture), seasonal illness, fever, or following an exacerbation of a chronic disease.[3][6]
d. Short Term Stabilisation[edit | edit source]
As the name suggests short term stabilisation focuses on stabilising the individual to minimise or control the symptoms of their condition until they can receive delivery of definitive treatment. Examples include administering intravenous fluids to a critically injured patient before transfer to an operating room.
e. Pre-Hospital Care[edit | edit source]
Care is provided in the community until the patient arrives at a formal healthcare facility capable of giving definitive care. Examples include delivery of care by ambulance personnel or evaluation of acute health problems by local healthcare providers and can include;
- First Responder Care
- Basic Prehospital Care
- Advanced Prehospital Care
f. Critical Care[edit | edit source]
Critical care is the specialized care of patients whose conditions are life-threatening and who require comprehensive care and constant monitoring, usually in intensive care units. Examples are patients with severe respiratory problems requiring endotracheal intubation and patients with seizures caused by cerebral malaria.[4][3]
Services Provided at Acute Care[edit | edit source]
Acute care is a branch of health care where a patient receives active but short-term treatment for a severe injury or episode of illness, an urgent medical condition, or during recovery from surgery that is generally delivered by teams of health care professionals from a range of medical and surgical specialties and may receive a combination of rehabilitative care (physical, occupational, respiratory, and speech therapy as needed) based on the individual; need to ensure a return to optimal function.
Acute care helps patients to improve their quality of life and help them to improve till transferred to the next phase of care appropriate for their needs, whichever that is. The transfer of care from acute care to the next rehabilitation phase is an important decision that may have a significant impact on the quality of care provided to the patient and their life.
Sub-acute Care[edit | edit source]
Sub-acute care is care provided for individuals who generally have a more stable condition and no longer meet the criteria for acute care but may require ongoing medical support to manage a new or changing health condition. It supports the individual to regain or adapt their ability to carry out activities of daily life.[7] The model of sub-acute care being conducted in the American focuses on the extension of acute medical services beyond the period of acute instability by a non-acute care unit within or close to the hospital in order to shorten the length of acute inpatient care.
Often seen as a step down from acute care, subacute care usually takes place in a skilled facility where an individual will receive a limited amount of treatment. Examples include rehab centres where physical, occupational and/or speech therapy are delivered. Other types of subacute care include wound care, IV antibiotic therapy, pain management, dialysis, and physician-mandated treatment for cardiac, pulmonary and other conditions such as diabetes or hypertension. Subacute care also can include short-term, post-surgical care with the individual remaining as an inpatient in the facility vs. visiting it for treatment.
Where it Occurs[edit | edit source]
Sub-acute care is generally carried out at hospitals, homes, health care centres, or specialist rehabilitation centres.[7]
Services Provided at Sub-acute Care[edit | edit source]
Generally, interventions provided within sub-acute care are goal orientated which combine a range of services such as physical, occupational and speech therapy.[7]
Benefits of Sub-acute Care[edit | edit source]
- Decreases the time of hospitalization (if in hospital);
- Provide support to a develop optimal function;
- Support adaptation and help manage changes as a result of their health condition and manage their everyday tasks. [7]
Post Acute Care[edit | edit source]
While post-acute care also provides continued medical treatment after a hospital stay, it maintains an emphasis on recuperation, rehabilitation, and symptom management. Individuals in recovery from cardiac or pulmonary disease, stroke or neurological disorders, or orthopaedic surgery often require rehabilitative therapies to help bridge the gap between hospital and home.
The post-acute care model is designed to assist patients to transition from illness to recovery while avoiding the need for a long-term care facility for individuals who could receive care at home, that relies on a series of care services to help individuals return home successfully after hospital discharge to aid the transition from recovery to functional autonomy.
The chief goals of post-acute care extend beyond medical aspects to encompass the provision of appropriate transitional integrated care to patients with the potential for functional recovery, thereby facilitating their return to their place of residence and maximise wellness and independence so they can get back to the business of living their best lives.
Post-acute care services range from intensive short-term rehab to longer-term restorative care. Some patients will achieve full recovery, while others learn to manage the symptoms of a chronic illness or learn to compensate for functional loss as a result of their impairment.[7]
Where it Occurs[edit | edit source]
Depending on the patient’s needs, post-acute-care may include a stay in a facility, such as a skilled nursing facility, inpatient or outpatient rehabilitation facility, or long-term care hospital, or care in the home via a home health agency, or in schools and workplaces as the individual returns to education or employment.[7]
Services Provided at Post-acute Care[edit | edit source]
There is some crossover here with subacute care, in that post-acute care can also include rehabilitation and other services after an acute-care episode. Post-acute care, however, also covers palliative services for patients who are nearing the end of life, and these along with other post-acute services can be delivered in a facility or via outpatient treatment in the patient’s home. Due to a growing ageing population, there is significant growth in the post-acute care area.[7]
Long Term Care[edit | edit source]
Long-term care is an integral part of health and social systems and incorporates activities undertaken for people requiring care by informal caregivers (family, friends, and neighbours), or by formal caregivers, including professionals and auxiliaries (health, social, and other workers). The need for long-term care is influenced by changing physical, mental, and/or cognitive functional capacities that are in turn, over the course of an individual’s life, influenced by the environment.
Long-term care enables people, who experience significant declines in capacity, to receive the care and support that allow them to live a life consistent with their basic rights, fundamental freedoms and human dignity. The goal of long-term care is to ensure that an individual who is not fully capable of long-term self-care can maintain the best possible quality of life, with the greatest possible degree of independence, autonomy, participation, personal fulfilment, and human dignity and should include respect for that individual’s values, preferences, and needs;
Long-term care services include traditional health services such as management of chronic conditions, rehabilitation, palliation, promotion and preventative services and can also include assistive care services such as caregiving and social support that should be integrated and provided in a continuum with the underlying core principles of person-centred care. The importance of ensuring continuity of care and of maximizing the opportunities for providing an optimal balance of care makes a strong case for the integration of long-term care into the general health services and when effectively integrated long term care can help reduce the inappropriate use of acute healthcare services.
Long-term care may be institutional or home-based, formal or informal.
- Institutional or residential long-term care is defined as the provision of such care to three or more unrelated people in the same place. Care communities provide a broad range of health care, personal care, and supportive services for adults who have limited self-care capabilities. In USA about 2.1 million reside in long-term care facilities[2].
- Home-based care may be provided exclusively in the home or combined with care in the community (such as in day centres, or under arrangements made for respite care) and may also be considered to include care provided to people whose “home” falls outside conventional definitions (e.g. travelling families, people living in slums). People who require home-based long-term care may also need other services, such as acute physical or mental health care and rehabilitation, together with financial, social, and legal support.
- Formal care may be publicly financed and organized, but the services may be provided by governmental organizations, by NGOs (local, national, or international), or by the private sector. It is usually provided by professionals (doctors, nurses, social workers) and auxiliaries, such as personal care workers (who help with bathing, dressing, etc.). In some communities, traditional healers may be an important additional source of care.
- Informal care includes that provided by members of nuclear and extended families, neighbours, friends, and individual volunteers, as well as assistance organized through voluntary organizations such as religious bodies.
References [edit | edit source]
- ↑ World Health Organisation. Health Topic - Rehabilitation. Available from: https://www.who.int/health-topics/rehabilitation#tab=tab_1 (accessed 30 June 2021)
- ↑ 2.0 2.1 World Health Organisation. Rehabilitation Key Facts. Available from: https://www.who.int/news-room/fact-sheets/detail/rehabilitation (accessed 2 May 2021).
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Hirshon JM, Risko N, Calvello EJ, Ramirez SS, Narayan M, Theodosis C, O'Neill J. Health systems and services: the role of acute care. Bulletin of the World Health Organization. 2013;91:386-8.
- ↑ 4.0 4.1 World Health Organization. Integrated management of adolescent and adult illness: interim guidelines for first-level facility health workers. World Health Organization; 2004.
- ↑ Ball CG, Hameed SM, Brenneman FD. Acute care surgery: a new strategy for the general surgery patients left behind. Canadian journal of surgery. 2010 Apr;53(2):84.
- ↑ Ramanayake RP, Sudeshika Ranasingha SL. Management of emergencies in general practice: role of general practitioners. Journal of family medicine and primary care. 2014 Oct;3(4):305.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 HealthyWA. Subacute Care. Available from: https://www.healthywa.wa.gov.au/Articles/S_T/Subacute-care (accessed on 30 June 2021)