Physiotherapy in Palliative Care
Top Contributors - Rachael McMillan, Allison Quigley, Sarah Verwoerd, Emma Mullen, Kim Jackson, Lucinda hampton, Shauna O' Connor, Admin, Lauren Lopez, Blessed Denzel Vudzijena, 127.0.0.1, Elaine Lonnemann, Evan Thomas, WikiSysop, Adam Vallely Farrell, Vidya Acharya, Shaimaa Eldib and Amrita Patro
Introduction[edit | edit source]
Palliative care is a practice discipline, which involves progressive and life-limiting illnesses such brain metastasis , chronic obstructive pulmonary disease, motor neuron disease [MND], and multiple sclerosis, each of which can benefit from the involvement of physiotherapy. Providing pain relief and management of distressing and debilitating symptoms, palliative care improves the quality of life (QoL) for patients with a life-limiting illness and their families.[1][2] Helping integrate the psychological, social, and spiritual aspects of holistic care, palliative care manages patients’ symptoms and pain levels, providing relief from distress and ultimately, facilitating improved function.[2][3]
All patients regardless of their diagnosis should be able to access palliative care appropriate to their current individual needs, to allow this to happen an integrated approach to palliative care is required.[4] The rise in the number of elderly people, especially those who have little home support, makes palliative care even more vital. People dying from stroke, dementia , or Multiple Organ Dysfunction Syndrome need to be guaranteed the same level of care as those that have a diagnosis of cancer.[5]
Palliative cares scope has recently broadened and the concept of ‘rehabilitation’ in palliative care is becoming more widespread.[6] Pain relief and the control of symptoms are employed where rehabilitation is not appropriate, depending on the stage of the illness.[4]
Physiotherapy in Palliative Care: The Need for Learning and Development in This Area[edit | edit source]
Allied health and rehabilitation in palliative care are well established.[7] Meeting patients’ physical, psychological, social, and spiritual needs, palliative care rehabilitation fits the adopted bio-psycho-social approach to health care, suggested by the World Health Organisation.[8]Involving symptom management and treatment effect minimization in patients with progressive and irreversible illness,[9]this essential service within health care must be utilized where appropriate, improving and maintaining patients’ and their families’ QoL. Physiotherapy aims to maximize movement and function when threatened by aging, injury, or disease, essential for optimal wellbeing.[10]
Existing evidence, though in its preliminary stages, advocates the role of physiotherapists and rehabilitation in palliative care.[7][11][9] Early referral to palliative care rehabilitation has been linked to higher-functioning patients,[9]therefore appropriate referral to palliative care physiotherapy is critical for optimal and patient-centered care.
Despite the potential benefits of palliative care physiotherapy, evidence suggests a lack of palliative care patients receiving physiotherapy treatment.[12]Research suggests the reluctance of referral, by other allied health professions, due to the misconceived perception of the inappropriateness of terminally ill patients to rehabilitation.[7]
Accessing Physiotherapy in Palliative Care[edit | edit source]
The ‘Quality Statement and Definition of Specialist Palliative Care’ provided by the National Institute for Health and Care Excellence (NICE) states, “Specialist Palliative Care encompasses hospice care as well as a range of other specialist advice, support, and a care such as that provided by hospital palliative care teams. Specialist palliative care should be available based on need and not diagnosis, offered in a timely way appropriate to their needs and preferences, at any time of day or night."[13]
General palliative care is an integral part of the routine care delivered by all health and social care professionals to patients living with life-limiting illnesses, whether at home, in a care home, or hospital.[14]
Specialist palliative care is based on general palliative care but can help patients with more complex palliative care needs. Specialist palliative care focuses on complex care needs. It is provided by a specially trained multi-disciplinary team (MDT) and can be accessed in any care setting.[15]
Palliative Care Settings[edit | edit source]
Everyone facing a life-limiting illness will need some degree of supportive care in addition to treatment for their condition.[15] Patients can receive palliative care physiotherapy at any time and at any stage of illness, whether it is terminal or not. It can be offered:
- In a hospice
- In the patient's home
- As a day patient in a hospice
- In a hospital
- In the community
Hospice[edit | edit source]
Most palliative care is received in a hospice (a specialist residential unit), run by an MDT comprising doctors, nurses, and therapists. They are smaller and quieter than hospitals and often feel more like home. Hospices can provide individual care more suited to the patient. Hospice care is palliative in nature, but the illness must have progressed to a point where curative treatment is no longer beneficial; the goal is no longer to cure but to promote comfort. Hospice care focuses on relieving symptoms and offering comfort from pain, shortness of breath, fatigue, nausea, anxiety, insomnia, and constipation.[2]
Care at Home[edit | edit source]
The patient can be cared for at home, by hospice staff. The patient’s general practitioner (GP) can arrange for community palliative care nurses to provide this level of care.[2]
Day Patient[edit | edit source]
Patients can remain at home but visit a hospice during the day, allowing them to receive the care and support that they require without the distress often associated with leaving their home.[2]
Hospital[edit | edit source]
Specialist palliative care teams are available in hospitals. Their role lies in providing education, training, and specialist advice on pain and symptom management to hospital staff with the ultimate aim of enhancing patient care. They also provide emotional support to the patients and families.[2]
Community[edit | edit source]
The community service provides specialist palliative care in the community, to avoid unplanned admission to the hospital for patients who have complex needs but prefer to care for at home.[16] It is an area in which large growth is proposed for the future.
The rationale for Physiotherapy in Palliative Care[edit | edit source]
Patient Needs and Our Role as a Physiotherapist[edit | edit source]
The physiotherapist must consider the patient’s needs and wishes, along with their physical needs [17]. Each individual will have different needs depending on how well they are handling their life-limiting illness. Robinson [18] claimed that patients’ needs and priorities must be addressed for treatment to be successful. Patients may need education on how to cope and handle the situation as best they can to lessen the fear and anxiety they have surrounding their condition. Worry and anxiety are two common psychological aspects associated with life-limiting illnesses. The entire MDT, including the physiotherapist, may be involved in the control of some of these symptoms, through education, maybe even just empathy towards the patient. Often when diagnosed with such illnesses patients can suffer from depression. This can regularly result in the individual becoming bedbound and inactive.
The needs of a patient in palliative care often include:
- To remain as independent as possible/maximize independence and daily function.
- To optimize and maintain quality of life (QoL) [19] – determined by physical functioning and psychological symptoms[20].
- Reduction/control of the consequences of the illness [21].
- Coping mechanisms and self-management[19] – to be in more control of their lives.
- To avoid secondary complications associated with life-limiting illnesses.
- Psychological support.[9]
Communication [edit | edit source]
Effective communication is paramount for interaction with patients and families in or being referred to palliative care.[22] Palliative care physiotherapy specialists demonstrate extensive knowledge and vast communication experience working with life-limiting illnesses, with competency in responding to rapidly changing situations.[9]
Appropriate communication follows the bio-psychosocial model and is a core priority for palliative care services concerned with the psychological and emotional well-being of the patient; including issues of self-esteem, insight into and adaptation to the illness and its consequences, communication, social functioning and relationships.[23]
In a study by McIlfatrick,[4] the needs identified by patients and their caregivers in palliative care included social support and the provision of practical care, respite care, psychological support, and information and choice. Therefore, knowledge of the patient’s diagnosis and any associated past treatments or conditions, to be able to plan the best physiotherapy treatment.[17]
Common symptoms and Physiotherapy Management[edit | edit source]
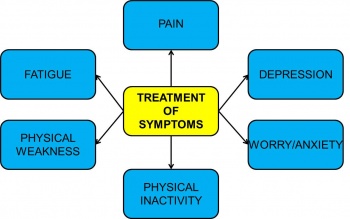
In patients with life-limiting illnesses, symptom control and maintenance of function become crucial aspects of treatment.[24] Palliative care aims to improve the QoL in patients faced with life-limiting illnesses. There is a role to be played in pain management and the reflief of other distressing symptoms, Figure 3.1.
Figure 3.1 Common symptoms experienced by palliative care patients and physiotherapy treatment of these symptoms.
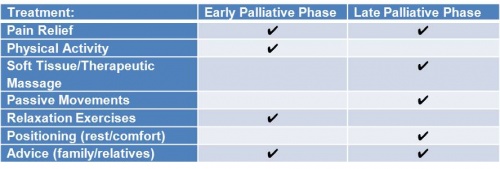
Physiotherapists primarily address the physical components of rehabilitation. With life-limiting illnesses, cancer, for example, there is also a psychological aspect, which we as physiotherapists may need to also address. The whole needs of the individual must be addressed.[19]There are many forms of treatment that physiotherapists can employ in the management of patients in palliative care. The decision as to what option best suits each patient is quite personal and depends on the stage of the disease process and goals set. Goals are largely dependent on the stage the patient is at. Life prolongation can be a goal in the early stage of illness but as the illness progresses the goal can shift to optimizing QoL as opposed to prolonging it.[17] Different treatments are suitable for the various phases of illnesses. These different forms of treatment provided by physiotherapists and their suitable phases are displayed in Table 3.1 below.
Table 3.1 Physiotherapy treatment and suitable phase during palliation.[17]
- Pain relief – TENS, heat, massage, lymphedema treatment, and acupuncture are common forms of pain relief.[19][9] Pain relief is often employed where rehabilitation is not appropriate.[9]
- Passive movements – These are often used, in-bound patients.[24]
- Physical exercise – This may positively affect depression and is currently emerging as a major aspect of the treatment of patients in palliative care.[25][26]
- Soft tissue massage and/or therapeutic massage are used to relieve muscle tension and can often aid in easing the symptoms of anxiety.
Physiotherapist's Role in Family and Carer Education[edit | edit source]
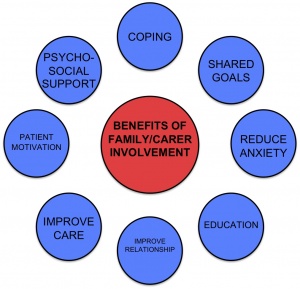
Family/carer involvement is beneficial as it provides an opportunity for education on the delivery of treatments when the physiotherapist is absent. It enables the family/carer to assist in treatments such as transcutaneous electrical nerve stimulation (TENS) to reduce pain. They can also be educated in methods to assist patient during transfers.[17] Inclusion of the family and/or carer into physiotherapy interventions will help to motivate the patient to participate in therapy and the patient may find it more comforting and enjoyable as a familiar face will be involved.[27] A range of inter-connected benefits are associated with family and/or carer involvement in physiotherapy treatment, see Figure 3.2.
Physiotherapists have a role in providing advice or education to patient and family/carers, enabling them to adjust and adapt to the consequences of the illness.[19][17] Adequate education and counselling to patients and their families is an integral part of palliative care rehabilitation.[3]
Figure 3.2 Benefits of family and/or carer involvement in physiotherapy treatment.
Physiotherapy Goals[edit | edit source]
The primary goal of physiotherapy in palliative care is to achieve the best possible QoL for both the patient and their families.
Other common goals of physiotherapy in the treatment of a cancer patient in palliative care are:
- Minimize symptoms
- Optimize functioning ability[28]
- Maintain or regain physical independence[28]
- Preserve the patients autonomy[17]
As stated previously goals and treatment are highly dependent on the stage of the disease. For example, the focus and goal of ‘traditional’ cancer rehabilitation are different from those of a terminally ill patient where there is a focus on maintaining a balance between optimal functioning levels and comfort.[24]
Physical Activity and Exercise[edit | edit source]
Fatigue and the reduction in physical functioning in life-limiting illnesses are significant factors in the reduced QoL often seen in these patient groups.[26] Rehabilitation in palliative care is gaining more and more attention in the literature today. However, it can be difficult to predict which patients will benefit from this ‘rehabilitation’ and how long these benefits will be sustained.[28]
In cancer patients, physical activity has been shown to address a decline in physical functioning and cancer-related fatigue (CRF). Most studies to date have researched physical activity and palliative care in the early phases of illnesses such as cancer. Limited studies have focused on the ‘end-of-life’ phase.[26] A review of the current literature by Lowe et al.[26] examined physical activity as a supportive care intervention in palliative cancer patients. Encouraging results have been found regarding physical activity interventions and palliative care and the ability of patients to tolerate this physical activity.
There is however, a need for more feasible studies to be produced to further advance this emerging research in palliative care. Further definition is required as to what patients are able and willing to participate in physical activity and those who are not.[26] Assessment of the needs, interests, and preferences of patients before developing physical activity interventions is of major importance.
Referrals to Physiotherapy in Palliative Care[edit | edit source]
Current referrals to palliative care physiotherapy are made largely by nursing staff, with referrals commonly increased by the presence of a physiotherapist.[9] Existing negative beliefs about rehabilitation in palliative care, amongst nursing staff, persist as definite barriers against referral to physiotherapy.[11] Professional and public attitudes about physical therapy goals are also reported to limit referral to physiotherapy in palliative care.[29] With increasing evidence base advocating referral to rehabilitation services in palliative care, there is a clear need for relevant educational tools, and, an exploration of these negative beliefs.[11][9]
Referral Process[edit | edit source]
Referral pathways need to be viewed as a continuum and considered from the point of view of the person, not the condition. They need to be well ‘signposted’ so that they are easy to navigate for patients, families, and staff.[30] Good quality pathways ensure a timely, smooth and coordinated journey across the whole system and a better experience for all. They support care that is safer, more efficient and effective making it easier for us to do the right thing.[30] Early referral to physiotherapy is advisable to ensure early implementation of rehabilitation goals, especially those that are preventative or restorative.[31] Referral can be made for a patient who has any life limiting illness and is in or is entering the palliative phase of their illness if they have:
- Complex end of life care needs
- Uncontrolled pain or other symptoms
- Complex physical, psychological, spiritual, or family needs that cannot be met by the staff in that care setting.[32]
Physiotherapy objectives within each of the palliative care settings differ depending on what stage the patient is at. Some may be actively dying; the physiotherapy input here is based on positioning and respiratory care. Longer-term patients’ physiotherapy looks at maximizing quality of life and maintaining mobility and independence.[31]
It is not possible to predict the timescale of individual prognosis accurately so evidence-informed clinical reasoning is used to identify people who may benefit from supportive and palliative care. Clinical indicators can help identify patients who are candidates for assessment to see if they have unmet needs (Supportive and Palliative Care Indicators Tool- SPICT).[33] A patient can be discharged from the hospice once they no longer require palliative care but can return at any time if their condition changes.[16]
There appears to be a lack of consensus within the available literature regarding standardized referral processes for palliative care physiotherapy. The points of transition from long-term condition management to palliative care and end of life are poorly defined and recognized. There is a risk that patients may not receive appropriate care.eg Continuity of palliative care over 24 hours needs to improve; Quality of care is variable
Future Direction for Physiotherapy in Palliative Care[edit | edit source]
The future direction of palliative care is set to extend to accommodate the changing demographics of the population. With more elderly patients, the burden of existing co-morbid conditions will increase, therefore rehabilitation will require to be more invasive and last longer. In conjunction with this, the length of in-patient or home care attachment may increase. This will put an extra burden on a setting that is currently low on resources. In addition to the decreasing morbidity associated with cancer, it is expected that fewer patients will die from cancer but more patients will be involved with palliative care for other conditions.[34]
References[edit | edit source]
- ↑ World Health Organization. Planning and implementing palliative care services: a guide for programme managers. 2016. Full version: https://iris.who.int/bitstream/handle/10665/250584/9789241565417-eng.pdf (accessed 21 September 2023).
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 NHS Choices. Accessing palliative care. 2012. Full version: http://www.nhs.uk/CarersDirect/guide/bereavement/Pages/Accessingpalliativecare.aspx (accessed 30 Oct 2013).
- ↑ 3.0 3.1 Prevost V, GRACH MC. Nutritional support and quality of life in cancer patients undergoing palliative care. European journal of cancer care. 2012 Sep;21(5):581-90.Available: https://pubmed.ncbi.nlm.nih.gov/22574646/(last accessed 25.8.2023)
- ↑ 4.0 4.1 4.2 Mcilfatrick S. Assessing palliative care needs: views of patients, informal carers and healthcare professionals. Journal of Advanced Nursing 2007; 57(1) 77-86.Available:https://pubmed.ncbi.nlm.nih.gov/17184376/ (accessed 25.8.2023)
- ↑ Higginson I, Wade A, McCarthy M. Palliative care: views of patients and their families. British Medical Journal 1990; August 301(6746): 277-281 Full version: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1663479/ (accessed 10 Oct 2013).
- ↑ Scialla S, Cole R, Scialla T, Bednarz L, Scheerer J. Rehabilitation for elderly patients with cancer asthenia: making a transition to palliative care. Palliative medicine 2000:14:(2):121-127.Available:https://pubmed.ncbi.nlm.nih.gov/10829146/ (accessed 25.8.2023)
- ↑ 7.0 7.1 7.2 Horne-Thompson A, Bramley R. The benefits of interdisciplinary practice in a palliative care setting: a music therapy and physiotherapy pilot project. Progress in Palliative Care 2011; 19(6): 304-308.Available:https://www.tandfonline.com/doi/abs/10.1179/1743291X11Y.0000000017?journalCode=yppc20 (accessed 25.8.2023)
- ↑ World Health Organization.International Classification of Functioning, Disability and Health (ICF). 2002. Full version:https://resources.relabhs.org/resource/international-classification-of-functioning-disability-and-health-icf-beginners-guide/ (Accessed 21 September 20230
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 9.8 Cobbe S, Nugent K, Real S, Slattery S, Lynch M. A profile of hospice-at-home physiotherapy for community-dwelling palliative care patients. International Journal of Palliative Nursing 2013; 19(1): 39-45.
- ↑ Kumar SP, Jim A. Physical Therapy in Palliative Care: From Symptom Control to Quality of Life: A Critical Review. Indian Journal of Palliative Care 2010; 16(3): 138-146.
- ↑ 11.0 11.1 11.2 Nelson LA, Hasson F, Kernohan WG. Exploring district nurses' reluctance to refer palliative care patients for physiotherapy. International Journal of Palliative Nursing 2012; 18(4):163-170.
- ↑ Parliament UK.Appendix 29: Memorandum by the Chartered Society of Physiotherapy (PC 37)2004. Full version: http://www.publications.parliament.uk/pa/cm200304/cmselect/cmhealth/454/454we34.htm (accessed 29 Oct 2013).
- ↑ National Institute for Healthand Care Excellence. Specialist Palliative Care. Updated 2021. Full version: https://www.nice.org.uk/guidance/qs13 (accessed 21 September 2023).
- ↑ Chartered Society of Physiotherapy.A flowering vocation.2012. http://www.csp.org.uk/frontline/article/flowering-vocation (accessed 16 Oct 2013).
- ↑ 15.0 15.1 The National Council for Palliative Care. Palliative Care explained. 2012. Full version: http://www.ncpc.org.uk/palliative-care-explained (accessed 16 Oct 2013).
- ↑ 16.0 16.1 Marie Curie Cancer Care. Marie Curie Hospices.2013. Full version: http://www.mariecurie.org.uk/en-gb/Commissioners-and-referrers/Referring-patients/Marie-Curie-Hospices/ (accessed 16 Oct 2013).
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 Frymark U, Hallgren L, Reisberg A. Physiotherapy in palliative care–a clinical handbook. Dostopno na: (Datum dostopa: 5. 10. 2011). 2010. (Accessed 21 September 2023)
- ↑ Robinson S. The learning needs of cancer patients. European Journal of Cancer Care 1992; 1(3): 18-20.
- ↑ 19.0 19.1 19.2 19.3 19.4 Bancroft MI. Physiotherapy in cancer rehabilitation: a theoretical approach. Physiotherapy 2003; 89(12):729-733.
- ↑ Martlew B. What do you let the patient tell you? Physiotherapy 1996;82(10): 558-565.
- ↑ Association of Chartered Physiotherapists in Oncology and Palliative Care. The role of physiotherapy in oncology and palliative care. 2009. Full version: http://www.acpopc.org.uk/acpopc/Young%20A5%20leaflet_Jun09%20b%20ref.pdf (accessed 16 October 2013).
- ↑ Pitman S. Evaluating a self-directed palliative care learning package for rural aged care workers: a pilot study.International Journal of Palliative Nursing 2013; 19(6): 290-294.
- ↑ Bradley SE, Frizelle D, Johnson M. Coping with Terminal Illness: The Experience of Attending Specialist Palliative Day Care. Journal of palliative medicine 2010;13(10):1211-1218.
- ↑ 24.0 24.1 24.2 Santiago‐Palma J, Payne R. Palliative care and rehabilitation. Cancer 2001; 92(Suppl 4): 1049-1052.
- ↑ Oldervoll LM, Loge JH, Paltiel H, Asp MB, Vidvei U, Wiken AN, Hjermstad MJ, Kaasa S. The Effect of a Physical Exercise Program in Palliative Care: A Phase II Study. Journal of Pain and Symptom Management 2006; 31 (5): 421-430.
- ↑ 26.0 26.1 26.2 26.3 26.4 Lowe SS, Watanabe SM, Baracos VE, Courneya KS. Associations between physical activity and quality of life in cancer patients receiving palliative care: A Pilot Survey. Journal of Pain and Symptom Management 2009; 38(5):785-796.
- ↑ Pollak KI, Childers JW, Arnold RM. Applying Motivational Interviewing Techniques to Palliative Care Communication.Journal of Palliative Medicine 2011; May 14(5): 587–592. Full version: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3089740/ (accessed 25 Oct 2013).
- ↑ 28.0 28.1 28.2 Montagnini M, Lodhi M, Born W. The utilization of physical therapy in a palliative care unit. Journal of Palliative Medicine 2003; 6(1): 11-17.
- ↑ Kumar SP, Jim A. Physical Therapy in Palliative Care: From Symptom Control to Quality of Life: A Critical Review. Indian Journal of Palliative Care 2010; 16(3): 138-146.
- ↑ 30.0 30.1 The Scottish Government Health Delivery Directorate Improvementand Support Team. Long term conditions collaborative: Improving care pathways. 2010.Edinburgh: Scottish Government. Full version: http://www.scotland.gov.uk/Resource/Doc/309257/0097421.pdf (accessed 17 Oct 2013).
- ↑ 31.0 31.1 Chartered Society of Physiotherapy.The remains of the day. 2008. http://www.csp.org.uk/frontline/article/remains-day (accessed 16 Oct 2013).
- ↑ Scottish Palliative Care Guidelines. Online versionhttps://www.palliativecareguidelines.scot.nhs.uk/ (accessed 21 September 2023).
- ↑ NHS Lothian. Supportive and Palliative Care Indicators Tool (SPICTTM). 2012. Full version: http://www.palliativecareguidelines.scot.nhs.uk/documents/SPICT_Sept2012.pdffckLR(accessed 27 October 2013).
- ↑ The Scottish Government.Cancer scenarios: An aid to planning cancer services in Scotland in the next decade- Implications for palliative care.2001; 330-335. Full version: http://www.sehd.scot.nhs.uk/publications/csatp/csatp.pdf (accessed 17 Oct 2013).
Role of Physical Therapy Intervention in Patients With Life-Threatening Illnesses.