Physical Activity and Respiratory Conditions
Original Editor - Mariam Hashem
Top Contributors - Mariam Hashem, Kim Jackson, Wendy Walker, Admin, Rachael Lowe, Tony Lowe, Evan Thomas, Michelle Lee, Tarina van der Stockt, Adam Vallely Farrell, Vidya Acharya, Rucha Gadgil and Lucinda hampton
Introduction[edit | edit source]
Chronic respiratory diseases are a group of chronic diseases affecting the airways and the other structures of the lungs. Common chronic respiratory diseases are Asthma, Bronchiectasis, chronic obstructive pulmonary disease COPD, Chronic rhinosinusitis, Hypersensitivity pneumonitis,Lung cancer, cystic fibrosis, Adult Respiratory Distress syndrome[1]
Physical activity (PA) is defined as any bodily movement produced by skeletal muscles which results in energy expenditure. Physical activity in daily life can be categorised into occupational, sports, conditioning, household, or other activities. Exercise is a subset of physical activity that is planned, structured, and repetitive and has as a final or an intermediate objective the improvement or maintenance of physical fitness.[2]
Why Exercise?[edit | edit source]
Increased PA is associated with enhanced psychological functioning and quality of life, improved cardiorespiratory fitness, and decreased morbidity.[3]
Increasing physical fitness may be beneficial for children with asthma by increasing exercise tolerance and capacity and, as a consequence, the threshold for inducing a condition called exercise-induced bronchoconstriction.[3] A low level of regular physical activity, in turn, leads to chronic deconditioning. It is not surprising, therefore, that some studies have found that patients with asthma tend to have lower cardiorespiratory fitness than their healthy counterparts. [4][5][6]
Physical training programs in asthma have been designed to enhance aerobic power, neuromuscular coordination, and self-confidence.[7]Reduced activity levels observed in asthmatics may also increase the incidence of obesity, with negative consequences on self-esteem .[8][9]
Physical activity levels play a key role in the onset of muscle dysfunction and de-conditioning and have been associated with quality of life, hospital admission, co-morbidities, lung function decline and mortality.[10][11] Skeletal muscle dysfunction is now recognised as a major problem for COPD patients[12] , and, as such, the use of strength training as a modality to reverse the deleterious effects of the disease is now recommended[13] . A recent systematic review demonstrated strength training could improve skeletal muscle strength in COPD patients, and these improvements were associated with increased activities of daily living [14]
Gardiner et al. showed that a strength training program can decrease the atrophy and strength loss associated with steroid use. They also demonstrated that the extent of fast-twitch muscle atrophy resulting from chronic glucocorticoid treatment can be lessened by mild weight-lifting exercise. [15]
PA causes a reduction in mortality for patients with COPD[edit | edit source]
PA has been shown to be the strongest predictor of all-cause mortality in COPD patients, with PA showed the best discriminative properties for 4-year survival. The authors of a large study[16] concluded: "We found that objectively measured physical activity is the strongest predictor of all-cause mortality in patients with COPD".
PA and Lung Function[edit | edit source]
Despite all the positive effects of PA for people with respiratory conditions, there is no evidence of change in lung function.[17]
Key Evidence:[edit | edit source]
- A pilot 6 week excises intervention study measured exercise intensity, attendance rate, recorded respiratory fitness and health related quality of life (HRQoL) pre and post intervention.
- Asthmatic children, even with moderate to severe disease, had their aerobic capacity significantly improved after a 16-wk physical training program.
- Home-based pulmonary rehabilitation improves clinical features and systemic inflammation in chronic obstructive pulmonary disease patients
Barriers/Limitations to Physical Activities[edit | edit source]
There are many barriers that could limit the participation of a chronic respiratory condition patient in exercises.
Children and adolescents with asthma may experience frustration, embarrassment and low self-confidence because of their disease-related limitations.[18][19] They may also withdraw from PA because of their parents’ fear and protectiveness.[20] A prospective observational study suggests levels of physical activity in the elderly patients with pneumonia did not improve despite a gradual recovery in their condition. This could be because of patients falling, management of medical instruments, (for example, catheters and drips), a lack of staff and walking aids, and a lack of understanding about the importance of walking for the patients[21].
The fear of breathlessness (Dyspnoea) due to cardiovascular disease, peripheral vascular disease, lung cancer, diabetes, dyslipidemia, hypertension, osteoporosis, and psychological disorders inhibits many patients from taking part in PA.[22][23] Corticosteroid use, overuse of bronchodilators, and interactions with other medications can further complicate management of PA programs in these patients. Other concerns during both rest and exercise include pulmonary hypertension, gas-trapping, dynamic hyperinflation, poor gas exchange, and increased respiratory pressure associated with destruction of lung parenchyma and increased airway resistance.[24]
To facilitate engagement in exercise programs many approaches should be addressed, such as managing acute dyspnoea[25], Psychosocial and behavioural interventions through educational sessions focusing on specific problems such as stress management, instructions in relaxation exercises, panic control, and smoking cessation[26]. Nutritional interventions should be considered[27], as well as social support, the option to participate in group activities, and the availability of professional support are frequently reported as enablers of physical activity.[28]
Exercise prescription[edit | edit source]
Individualised exercise training prescriptions should be based on patient characteristics, such as baseline pulmonary function, exercise capacity, habitual physical activity levels, inflammation and infection status to establish favourable exercise-training induced effects.[29]
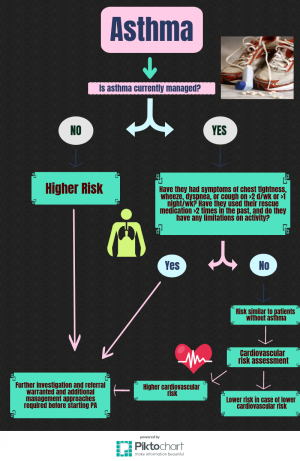
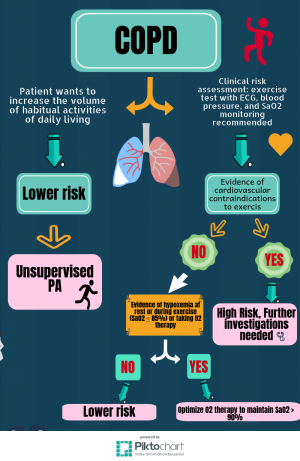
Burr, Davidson, Shephard and Eves Developed two clinical decision trees for assessing the risk of adverse events during PA in patients with COPD ad Asthma. These decision trees can be used to categorise a patient as higher or lower risk, informing the requirements of PA prescription and the monitoring of exercise programs. The info-graphs below illustrate the clinical decision trees:
Interval training[edit | edit source]
In patients with advanced COPD, interval exercise consisting of repeated bouts (30–60 s) of high- or even maximal-intensity work (80–100% peak) separated by periods (30–60 s) of lower intensity work intervals, has been shown to be associated with a small increase in arterial lactate concentration, lower ventilation and degrees of dynamic hyperinflation and lower symptoms of dyspnoea and leg discomfort, thus allowing the total amount of work performed to be significantly greater than that of constant-load exercise.[30]
Implementation of high-intensity interval training in patients with COPD has proven to be effective in terms of improvements in muscle fibre oxidative capacity, thus enhancing the utilisation of oxygen by the exercising muscles. [31]
Aerobic Exercises[edit | edit source]
Moderate aerobic exercises is defined as exercise, which noticeably accelerates heart rate and requires 3.0 to 6.0 metabolic equivalents (METs) (e.g. slow cycling, brisk walking or swimming), whereas vigorous aerobic exercise requires more than 6.0 METs and causes rapid breathing and a substantial increase in heart rate (e.g. running fast, swimming laps, singles tennis)[32]
A large body of evidence demonstrates important health benefits from aerobic exercise, including decreases in dynamic hyperinflation and exertional dyspnea; improved exercise tolerance; and enhanced quality of life, with fewer disease exacerbations and reported sick days.[33]
Strength training[edit | edit source]
To optimise the benefits gleaned from a strength training program, the exercise prescription variables of intensity, volume and frequency should be tailored to the needs of each patient.[34]
Strength training exercises be performed at an intensity of approximately 60% of the muscle’s maximum force-generating capacity to increase strength. To determine the amount of weight of the appropriate stimulus, the common approach is based on a 1 repetition maximum, (1-RM) or the ability to lift or perform a movement only once before fatigue prevents a subsequent contraction. If the weight employed is below 60% of the 1-RM, there may be only modest improvements of 5% to 10% in strength.
The volume of the strength training exercise is a function of the number of repetitions and sets of an exercise completed. For frail patients, the ACSM recommends that at least one set of each exercise be performed. As patients increase the intensity of their exercise prescription, the number of sets of an exercise may also increase. Once the patient can complete the pre-determined number of repetitions for all the prescribed sets, the resistance should be increased. Specific exercises should target strength improvements for the major muscle groups which include the chest, shoulders, arms, upper and lower back, abdomen, hips and legs. One or more exercises can be prescribed for each of these muscle groups depending upon the patient’s specific needs.
The final component of the exercise prescription that needs to be considered is frequency or the number of times the exercise should be performed per week. Outpatient recommendations stipulate that individuals exercise 2 to 3 times per week and to allow 48 hours of recovery between exercise bouts.[35]
Precautions[edit | edit source]
Exercises should be discouraged during periods of active infection in patients with Cystic Fibrosis.[29]
patients with substantial hypoxaemia (SpO2 < 90%) at rest or during exertion, uncontrolled asthma, or the presence of pulmonary hypertension should be optimally medically managed before starting exercise[33]
Persons with COPD who wish to become more physically active should be evaluated using a graded exercise test including ECG monitoring and pulse oximetry. Remarkable test results and evidence of serious cardiovascular conditions (ie, angina, ischaemia, complex ectopy, high-degree AV block, uncontrolled blood pressure) should be seen by the appropriate specialist before commencing PA[33]
Supervising exercise professionals should have specific training with and monitor for potential pulmonary related complications as well as complications related to the common sequelae and co-morbidities of COPD[33]
To reduce the risk of exercise-related adverse events, those with asthma should make sure that their disease is properly controlled before becoming more physically active. Those with poor or partial control of their asthma should see their physicians before becoming more active[33]
For individuals who develop EIB or asthma like symptoms with exercise, a rapid-acting β2-agonist should be taken before exercise. Individuals with asthma should also incorporate a progressive warm-up and should try to avoid exercising in the excessive cold or environments with known asthma triggers[33]
Resources[edit | edit source]
The Motivate2Move website, created by Wales Deanery, has a useful section on physical activity and respiratory disease.
References[edit | edit source]
- ↑ Diseases, C. R. (n.d.). CHRONIC RESPIRATORY, 12–36.
- ↑ Caspersen CJ, Powell KE, Christenson GM. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep 1985; 100: 126–131.
- ↑ 3.0 3.1 Berntsen S, Carlsen KC, Anderssen SA, et al. Norwegian adolescents with asthma are physical active and fit. Allergy 2009;64:421–6.
- ↑ CLARK, C. J., and L. M. COCHRANE. Assessment of work performance in asthma for determination of cardiorespiratory fitness and training capacity. Thorax 43:745–749, 1988
- ↑ GARFINKEL, S. K., K. R. KESTEN, and A. S. CHAPMAN REBUCK. Physiologic and nonphysiologic determinants of aerobic fitness in mild to moderate asthma. Am. Rev. Respir. Dis. 145:741–745, 1992
- ↑ NEDER, J. A., L. E. NERY, A. C. SILVA, A. L. B. CABRAL, and A. L. G. FERNANDES. Short term effects of aerobic training in the clinical management of moderate to severe asthma in children. Thorax 54:202–206, 1999.
- ↑ ORESTEIN, D. M. Asthma and sports. In: The Child and The Adolescent Athlete, O. Bar-Or (Ed.). London, UK: Blackwell, 1996, pp. 433–454.
- ↑ GIBSON, P. G., G. V. HENRY, and J. H. VIMPANI. Asthma knowledge, attitudes, and quality of life in adolescents. Arch. Dis. Child 73: 321–326, 1995.
- ↑ NIXON, P. A. Role of exercise in the evaluation and management of pulmonary disease in children and youth. Med. Sci. Sports Exerc. 28:414–420, 1996.
- ↑ Schols AM, Ferreira IM, Franssen FM, et al. Nutritional assessment and therapy in COPD: a European Respiratory Society statement. Eur Respir J 2014; 44: 1504–1520.
- ↑ Vaes AW, Garcia-Aymerich J, Marott JL, et al. Changes in physical activity and all-cause mortality in COPD. Eur Respir J 2014; 44: 1199–1209
- ↑ American Thoracic Society European Respiratory Society. Skeletal muscle dysfunction in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 1999; 159:S1–S40. [PubMed: 10194189]
- ↑ Newman AB, Kupelian V, Visser M, Simonsick E, Goodpaster B, Nevitt M, Kritchevsky SB, Tylavsky FA, Rubin SM, Harris TB. Sarcopenia: alternative definitions and associations with lower extremity function. J Am Geriatr Soc. 2003; 51:1602–1609. [PubMed: 14687390]
- ↑ O'Shea SD, Taylor NF, Paratz J. Peripheral muscle strength training in COPD: a systematic review. Chest. 2004; 126:903–914. [PubMed: 15364773
- ↑ Gardiner PF, Hibl B, Simpson DR, Roy R, Edgerton VR. Effects of a mild weight-lifting program on the progress of glucocorticoid-induced atrophy in rat hindlimb muscles. Pflugers Arch. 1980; 385:147–153. [PubMed: 7190273
- ↑ Waschki B, Kirsten A, Holz O, et al. (2011) Physical activity is the strongest predictor of all-cause mortality in patients with COPD: a prospective cohort study. Chest. 140 (2):331-42
- ↑ Hill, N.S. (2006). Proceedings of the American Thoracic Society. Pulmonary Rehabilitation; 3:66-74.
- ↑ Stewart M, Masuda JR, Letourneau N, et al. “I want to meet other kids like me”: Support needs of children with asthma and allergies. Issues Compr Pediatr Nurs 2011;34:62–78.
- ↑ Grover C, Armour C, Van Asperen PP, et al. Medication use in Australian children with Asthma: user’s perspective. J Asthma 2013;50:231–41
- ↑ Williams B, Hoskins G, Pow J, et al. Low exercise among children with asthma: a culture of over protection? A qualitative study of experiences and beliefs. Br J Gen Pract 2010;60:319–26.
- ↑ KAWAMURA K, KATO T, SAKAI H, SETAKA Y, HIROSE Y, OOZONE K, AITA I, TOMITA K. Investigation into the mobility of elderly patients with pneumonia using triaxial accelerometer data. Physical Therapy Research. 2019 Dec 20;22(2):73-80.
- ↑ . Briggs DD Jr. Chronic obstructive pulmonary disease overview: prevalence, pathogenesis, and treatment. J Manag Care Pharm 2004;10(4 Suppl):S3-10.
- ↑ CROFT, D., and B. LLOYD. Asthma spoils sport for too many children. Practitioner 233:969–971, 1989.
- ↑ Chatila WM, Thomashow BM, Minai OA, Criner GJ, Make BJ. Comorbidities in chronic obstructive pulmonary disease. Proc Am Thorac Soc 2008;5(4):549-55.
- ↑ Hill K, Vogiatzis I, Burtin C. The importance of components of pulmonary rehabilitation, other than exercise training, in COPD. Eur Respir Rev 2013; 22: 405–413.
- ↑ Spruit MA, Singh SJ, Garvey C, et al. An official American Thoracic Society/European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med 2013; 188: e13–e64.
- ↑ . Schols AM, Ferreira IM, Franssen FM, et al. Nutritional assessment and therapy in COPD: a European Respiratory Society statement. Eur Respir J 2014; 44: 1504–1520.
- ↑ Thorpe O, Johnston K, Kumar S. Barriers and enablers to physical activity participation in patients with COPD: a systematic review. J Cardiopulm Rehabil Prev 2012; 32: 359–369
- ↑ 29.0 29.1 Most, D. (n.d.). COPD and exercise : does it make a difference ?, 12(2), 38–49.
- ↑ Vogiatzis I, Nanas S, Kastanakis E, et al. Dynamic hyperinflation and tolerance to interval exercise in patients with advanced COPD. Eur Respir J 2004; 24: 385–390.
- ↑ Vogiatzis I, Terzis G, Nanas S, et al. Skeletal muscle adaptations to interval training in patients with advanced COPD. Chest 2005; 128: 3838–3845
- ↑ 2. Ries AL, Bauldoff GS, Carlin BW, et al. Pulmonary rehabilitation: Joint ACCP/AACVPR Evidence-Based Clinical Practice Guidelines. Chest 2007; 131: 4S–42S
- ↑ 33.0 33.1 33.2 33.3 33.4 33.5 Burr, J. F., Davidson, W., Shephard, R. J., & Eves, N. (2012). Assessing risks for physical activity clearance and prescription, 58, 761–764.
- ↑ . Garber CE, Blissmer B, Deschenes MR, Franklin BA, Lamonte MJ, Lee IM, Nieman DC, Swain DP. American College of Sports Medicine position stand Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exerc. 2011; 43:1334–1359. [PubMed: 21694556
- ↑ Manuscript, A., & Patients, R. F. (2014). NIH Public Access, 41(4), 208–215. https://doi.org/10.1097/JES.0b013e3182a4e67c.Early