Nerve Injury Rehabilitation
Original Editor - Lucinda Hampton
Top Contributors - Lucinda hampton, Chrysolite Jyothi Kommu, Wendy Walker, Wajeeha Hassan, Rachael Lowe, Naomi O'Reilly, Kim Jackson and Vidya Acharya
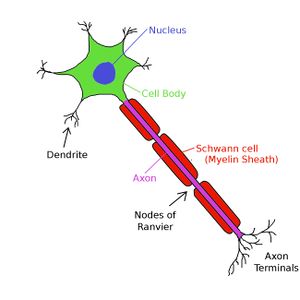
Clinically Relevant Anatomy[edit | edit source]
Nerve regrowth in the peripheral nervous system is dependent on the type of injury. Functional disability due to nerve lesions is intertwined with the severity of the lesion. Before reading this article it would be advised to have a good knowledge of the type of lesion and the denervation consequences[1]. Please read Classification of Peripheral Nerve Injury as an introduction to this page.
Pathological Process[edit | edit source]
Peripheral nerve injuries have numerous causes including traumatic injuries; infections; metabolic problems ( one of the most common causes is diabetes mellitus); inherited causes; exposure to toxins; tumors; iatrogenic causes.[2]
Watch the below to grasp the concepts of nerve damage and repair
Clinical Presentation[edit | edit source]
Clinical presentation varies according to the nerve affected i.e. sensory, motor, or combined.
Signs and symptoms may include[2]
- Gradual onset of numbness, prickling, or tingling in your feet or hands, which can spread upward into your legs and arms
- Sharp, jabbing, throbbing, freezing, or burning pain
- Extreme sensitivity to touch
- Lack of coordination and falling
- Muscle weakness or paralysis if motor nerves are affected
- Neuromatous or causalgia pain.[4]
Assessment[edit | edit source]
After a diagnosis of a peripheral nerve injury, a full subjective and objective examination is required to get a clear picture of the way the lesion is affecting the client. The examination should focus on
- Pain Assessment
- Sensation Deficit and Skin Condition
- Muscle Strength/Loss
- Functional Deficits
- Balance Deficits
- Joint Stiffness
- Emotional Stress
Outcome Measures[edit | edit source]
Depends on various criteria ( eg upper or lower limb) but could include:
- Oxford Scale
- Romberg or Berg Balance Scale
- Visual Analogue Scale
- Short form McGill Pain Questionnaire
- Nine-hole Peg Test
(see Outcome Measures Database)
Surgical Management[edit | edit source]
Nerve autografts are gold standard to repair delayed nerve injuries. They are useful in bridging the gap between nerves. [5]Now nerve allografts and conduits can also be used in place of autografts.[6][7]
In the table below are given donor nerve for associated nerve injures[8]
| Nerve injury | Donor nerve |
|---|---|
| Musculocutaneous/ upper trunk brachial plexus | Fascicle within ulnar nerve subserving Flexor carpi ulnaris |
| Axillary nerve/upper trunk brachial plexus | Motor branches of radial nerve to triceps (long or medial head) |
| Suprascapular nerve | Distal spinal accessory nerve |
| Posterior interosseous nerve | Branches of median nerve |
| Axillary nerve | Medial pectoral nerve |
| Long thoracic nerve/C5 6, 7 injuries | Thoracodorsal nerve |
| Avulsion of multiple cervical roots | Intercostal nerves |
| Peroneal nerve | Branches of the tibial nerve (eg, lateral gastrocnemius). May require a nerve graft to extend |
Physiotherapy Management[edit | edit source]
Management is directed towards:
Pain Management[edit | edit source]
Neuropathic pain affects the quality of life and is a common consequence of nerve damage. Pain control is of paramount importance[9]. Complete relief is rarely obtained and 40-60 % find means to obtain partial relief. A multidisciplinary approach is taken, with most input from the pharmacologist(s). Anticonvulsants and tricyclic anti-depressants are the medications most commonly used for neuropathic pain. A Physiotherapist can employ other modalities that show in various studies to be of benefit as complementary medicine for pain relief[1]. These include
- Massage eg aromatherapy massage, in studies, has shown to help manage neuropathic pain and improve QOL.[10] Many differing massage techniques have been employed showing benefits for pain management and QOL.[11]
- Transcutaneous Electrical Nerve Stimulation (TENS). Application of TENS has been found to be of benefit in pain reduction in neuropathic pain. It was found to be of benefit if used at 100hz in constant mode.[12]
- Low Level Laser Therapy (LLLT). Studies have found this to be of benefit in pain relief and acceleration of healing in treatment of neuropathic pain and neurological deficits as adjuvant therapy.[13]
- Relaxation Techniques
- Acupuncture
Muscle Weakness[edit | edit source]
A consequence of denervation is muscle atrophy and functional deficits. The healthy neuromuscular junction (NMJ) is critical for nervous control of muscles. TENS has been seen in numerous studies to have a positive effect on maintaining NMJ health and in prevention of muscle atrophy.[1]A 2018 study found the use of TENS was most beneficial if delayed to one-week post-trauma, the use of 100hz being most beneficial.[14]
Muscle care is of utmost importance to prevent damage to muscle units, in particular prevent: heat or cold trauma; over stretching by gravity or incorrect lifting/transfer techniques; contractures of muscles. The below video clips give a good guide to proper handling techniques involved in passive ROM.
Techniques employed by physiotherapist to achieve the above goals are massage, US, hydrotherapy, splints, passive ROM stretches and correct transfer skill education.
When muscle strengthening exercises can commence it is important not to damage the healing nervous tissue: if pins and needles, numbness or increased pain occurs the exercise is too hard and can have a negative effect on healing.
Muscle strengthening exercises are employed as appropriate, eg isometric, graded weight progression, open-close chain, and Use of support slings may be employed to assist the movement and take the weight of the limb. In addition, splinting techniques, frequently have a place in management of peripheral nerve injuries, including postoperative splinting and casting, as well as splints to prevent deformities developing, or even to overcome established contractures and improve function, and in this way aid the patient's recovery[17]. Static and dynamic splints can help to rest paralyzed muscles in optimum positioning to avoid overstretching and or contractures. They also assist in allowing unaffected muscles to operate from correct positions. See video clip below for examples
A recent study found that exercise can enhance axonal growth via a neurotrophin-dependent mechanism affecting adult dorsal root ganglion neurons.[19] Aerobic activity should also be encouraged ( aiming for 30 minutes 4 times a week) for its’ known health benefits.
Functional deficits and sensory deficit[edit | edit source]
In the relearning of functional tasks, the brain is utilized to regain visio-tactile and audio-tactile interaction. In the upper limb, the focus is on fine motor skill learning. In the lower limb balance and coordination are areas of focus.
Sensory reeducation aids in the recovery of sensibility[17]. In sensory stimulation pinching and tapping, brushing and icing are regularly used.
Proprioception deficits can be improved using eg exercise balls, balance pads for WB activities, juggling balls for upper limbs, yoga, Tai-chi.[20]
Balance Deficits[edit | edit source]
see Otago Balance Program as an example of a good balanced program.
Joint Stiffness[edit | edit source]
The soft tissues of the region and adjacent regions supplied by the damaged nerve are at risk of contractures if left in shortened positions. PROM exercises on a daily basis are useful to prevent these problems, and protective removable static splints can also be useful in contracture prevention. For joints that have become stiff ultrasound and laser therapies have been found to provide benefit.[1]
Emotional Stress[edit | edit source]
Chronic neuropathic pain has a life-debilitating effect causing emotional stress and reduced QOL. To properly treat a client with neuropathic pain this must be respected. The ultimate goal is not simply to reduce pain but to achieve better QOL. This can only be achieved if the depression, anxiety, and sleep disorders are also addressed.[21]
Related Pages[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Reza Salman Roghani and Seyed Mansoor Rayegani (2012). Basics of Peripheral Nerve Injury Rehabilitation, Basic Principles of Peripheral Nerve Disorders, Dr. Seyed Mansoor Rayegani (Ed.), ISBN: 978-953-51-0407-0, InTech, Available from: http://www.intechopen.com/books/basic-principles-of-peripheral-nervedisorders/basics-of-peripheral-nerve-injury-rehabilitation (last accessed 24.3.2019)
- ↑ 2.0 2.1 Mayo clinic. Peripheral neuropathy. Available from: https://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/symptoms-causes/syc-20352061 (last accessed 24.3.2019)
- ↑ Dr. Simon Freilich. Nerve damage and repair. Available from: https://www.youtube.com/watch?v=OlNyp0RfiBg&feature=youtu.be (last accessed 24.3.2019)
- ↑ Medscape. Peripheral nerve injuries clinical presentation. Available from: https://emedicine.medscape.com/article/1270360-clinical (last accessed 24.3.2019)
- ↑ Lundborg G. A 25-year perspective of peripheral nerve surgery: evolving neuroscientific concepts and clinical significance. The Journal of hand surgery. 2000 May 1;25(3):391-414. https://pubmed.ncbi.nlm.nih.gov/10811744/
- ↑ Pabari A, Lloyd-Hughes H, Seifalian AM, Mosahebi A. Nerve conduits for peripheral nerve surgery. Plastic and reconstructive surgery. 2014 Jun 1;133(6):1420-30. https://pubmed.ncbi.nlm.nih.gov/24867724/
- ↑ Brooks, D.N., Weber, R.V., Chao, J.D., Rinker, B.D., Zoldos, J., Robichaux, M.R., Ruggeri, S.B., Anderson, K.A., Bonatz, E.E., Wisotsky, S.M. and Cho, M.S., 2012. Processed nerve allografts for peripheral nerve reconstruction: a multicenter study of utilization and outcomes in sensory, mixed, and motor nerve reconstructions. Microsurgery, 32(1), pp.1-14. https://pubmed.ncbi.nlm.nih.gov/22121093/
- ↑ Korus L, Ross DC, Doherty CD, Miller TA. Nerve transfers and neurotization in peripheral nerve injury, from surgery to rehabilitation. Journal of Neurology, Neurosurgery & Psychiatry. 2016 Feb 1;87(2):188-97. https://jnnp.bmj.com/content/87/2/188.short
- ↑ Michael D Robinson, Steven Shannon.Rehabilitation of peripheral nerve injuries.PMID: 11878078.DOI: 10.1016/s1047-9651(03)00074-3.PubMed.gov. National Library of Medicine. National Centre for Biotechnology Information.
- ↑ Gok Metin, Zehra & Arikan Dönmez, Ayşe & Izgu, Nur & Ozdemir, Leyla & Emre Arslan, Ismail. (2017). Aromatherapy Massage for Neuropathic Pain and Quality of Life in Diabetic Patients. Journal of nursing scholarship : an official publication of Sigma Theta Tau International Honor Society of Nursing. 49. 10.1111/jnu.12300. (last accessed 25.3.2019)
- ↑ The foundation for peripheral neuropathy. Massage for neuropathy. Available from: https://www.foundationforpn.org/living-well/integrative-therapies/massage/ (last accessed 25.3.2019)
- ↑ Yameen F, Shahbaz NN, Hasan Y, Fauz R, Abdullah M. Efficacy of transcutaneous electrical nerve stimulation and its different modes in patients with trigeminal neuralgia. JPMA-Journal of the Pakistan Medical Association. 2011 May 1;61(5):437. (last accessed 25.3.2019)
- ↑ Cotler HB, Chow RT, Hamblin MR, Carroll J. The use of low level laser therapy (LLLT) for musculoskeletal pain. MOJ orthopedics & rheumatology. 2015;2(5). Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4743666/ (last accessed 26.3.2019)
- ↑ Su HL, Chiang CY, Lu ZH, Cheng FC, Chen CJ, Sheu ML, Sheehan J, Pan HC. Late administration of high-frequency electrical stimulation increases nerve regeneration without aggravating neuropathic pain in a nerve crush injury. BMC neuroscience. 2018 Dec;19(1):37.(last accessed 25.3.2019)
- ↑ Kellog community college. PROM upper extremity. Available from:https://www.youtube.com/watch?v=J-YE4lAVEmo&t=30s (last accessed 27.3.2019)
- ↑ Kelloge community college. PROM lower extremity. Available from: https://www.youtube.com/watch?v=CK6Uq7JGy0g&t=6s (last accessed 27.3.2019)
- ↑ 17.0 17.1 G K Frykman, J Waylett. Rehabilitation of Peripheral nerve injuries.PubMed.gov.National Library of Medicine.National Centre for Biotechnology Information.Orthop Clin North Am. 1981 Apr;12(2):361-79.
- ↑ HomeCEU Dynamic splinting. Available from: https://www.youtube.com/watch?v=XT68ZcEXG5A (last accessed 25.3.2019)
- ↑ Voluntary exercise increases axonal regeneration from sensory neurons Raffaella Molteni, Jun-Qi Zheng, Zhe Ying, Fernando Gómez-Pinilla, Jeffery L. Twiss Proceedings of the National Academy of Sciences Jun 2004, 101 (22) 8473- Available from: https://www.pnas.org/content/101/22/84738478; DOI:10.1073/pnas.0401443101 (last accessed 26.3.2019)
- ↑ Dr Ben Kim. Simlpe ways to improve balance and proprioception. Available from: https://www.youtube.com/watch?v=KDvJpp6-ID0 (last accessed 27.3.2019)
- ↑ Torta R, Ieraci V, Zizzi F. A Review of the Emotional Aspects of Neuropathic Pain: From Comorbidity to Co-Pathogenesis. Pain and therapy. 2017 Dec 1;6(1):11-7. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5701895/ (last accessed 27.3.2019)