Mindfulness Meditation in Chronic Pain Management
Original Editor - Merinda Rodseth based on the course by Shrey Vazir
Top Contributors - Merinda Rodseth, Kim Jackson, Tarina van der Stockt, Vidya Acharya, Jess Bell and Lucinda hampton
Introduction[edit | edit source]
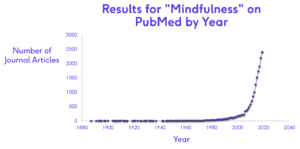
Evidence for the use of mindfulness has grown rapidly since its introduction to the Western world around 1979, with more than 2500 studies currently available on mindfulness (Figure 1).
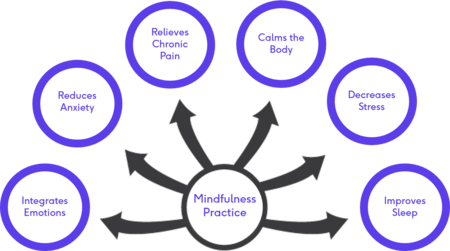
Mindfulness-Based Interventions (MBI) are showing promising results in supporting mental health needs even in the absence of psychological disorders and have become a more popular, cost-effective method to provide the support.[2][3] The benefits of MBI are well established and include:[3][4]
- Decreased anxiety and depression
- Relief of stress and psychological distress
- Increased coping abilities
- Alleviation of pain
- Decreased negative affect (decreased rumination)
- Enhanced cognitive control
- Emotion regulation
- Improved sleep
- Immune system support
Figure 2. Benefits of Mindfulness Practice[1]
Cognitive Changes Associated with Mindfulness[edit | edit source]
The greatest impact of mindfulness is its effect on the neural plasticity of the brain. Several changes in brain activation have been documented with mindfulness practice, allowing us to also “see” the benefits of MBI as is evident on functional Magnetic Resonance Imaging (fMRI).[5][6] However, the study designs vary greatly with the use of different MBI and therefore the locations of the reported effects are diverse and spread over multiple regions of the brain.[5] The brain regions most consistently altered with MBI are included in Table 1.[5][7][8][9]
Table 1: Neural changes associated with mindfulness practice
| Region of the brain | Effect with MBI | Function of the region |
| Insula and sensory cortices | Increased activation | Body awareness (interoception)
Emotional processing Self-awareness Interpersonal experience |
| Anterior cingulate cortex (ACC) | Increased activation | Higher order cognitive processes
Attention and attention regulation Self and emotional regulation Cognitive distancing - associated with non-judgemental acceptance |
| Prefrontal cortex | Increased activation | Higher order cognitive processes
Attention and attention regulation Emotion regulation Meta-awareness & reappraisal Reasoning and decision making Functional connectivity with the salience network Downregulation of amygdala responses |
| Hippocampus | Increased activation
Increased volume |
Memory processes |
| Amygdala | Decreased activation
Decrease in volume/size |
Fight-or-flight reaction
Fear response Stress response Adds emotional value to sensory input - emotional processing |
Greater stress is associated with greater amygdala activation. Down-regulation of the amygdala is what underscores the reduction in stress seen with Mindfulness-Based Stress Reduction (MBSR).[8] Mindfulness is therefore not simply about paying attention. The way in which we use this focus of the mind ultimately changes the function and the structure of the brain.[10] Just as we can train our muscles to grow, we can “train” our brains as is evident in the studies about mindfulness.
Mindfulness and Pain[edit | edit source]
Chronic pain poses a significant therapeutic challenge and has been declared a public health problem, placing burdens not only on those experiencing pain, but also society as a whole.[11][12] Chronic pain is estimated to affect more than 100 million adults at any given time in the United States, with chronic back pain being the most commonly reported chronic pain complaint.[4][11][12][13] Chronic pain is also one of the primary causes of disability and decreased quality of life, resulting in a cost of more than $600 billion dollars annually in the United States alone.[11][13] Opioid medication is frequently prescribed in order to manage pain and its potential consequences, which contributed to many other problems including the “opioid epidemic” of opioid misuse, addiction and opioid-related deaths due to patients overdosing.[12][13] Mindfulness, as a non-pharmacologic option, is receiving increased interest in the management of pain.[4][13][14]
Chronic pain is complex in nature, involving many physical and psychological factors.[12][15] It is associated with sleep disturbances, obesity and weight gain, chronic fatigue, limited physical functionality and decreased quality of life.[12] Individuals suffering from a variety of chronically painful conditions are also at an increased risk for anxiety, depression and other affective disorders.[11][13][16] The International Association for the Study of Pain (IASP) defines pain as “An unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.”[17] Treatment of pain should therefore also be multifaceted to address both the sensory component as well as the affective/emotional experience of pain. Treatments targeted at the negative affect associated with chronic pain are therefore hypothesised to not only positively influence the emotional distress but also influence the frequency and intensity of pain.[11] Mindfulness as a multifaceted intervention is therefore ideally placed to have a positive effect on pain and pain affect without the negative effects associated with pharmacological interventions such as opioids.[4][11][13][18]
MBSR is consistently showing positive improvements in pain management.[11][12][15] Several studies have looked at the effect of MBI on various chronic conditions and various chronically painful conditions including chronic low back pain (LBP).[19] Several of these studies can be found in Table 2.
Table 2. Studies on the effect of MBI
| Study | Year | Participants and design | Intervention | Results |
| Niazi[19] | 2011 | Systematic review
18 studies looking at chronic illness (cancer, hypertension, diabetes, HIV/AIDS, chronic pain, skin disorders) |
MBSR alone or with other treatments | Improvement in chronic conditions |
| Zeidan et al[20] | 2011 | 15 participants | 4days mindfulness meditation training | Reduction in pain intensity (40%)
Reduced pain unpleasantness (57%) |
| Zeidan et al[15] | 2015 | 75 participants | 4 groups: Mindfulness meditation, placebo, sham meditation and control | Mindfulness meditation group - significant reduction in pain intensity (27%)
Reduced pain unpleasantness (44%) |
| Morone et al[21] | 2016 | 282 participants with chronic LBP | MBSR and control group (8 weeks, 1.5 hrs once weekly) | Significant improvements in disability and quality of life |
| Cherkin et al[22] | 2016 | Randomised controlled trial
342 participants with chronic LBP |
Cognitive behavioural therapy (CBT)
MBSR 8 weekly 2-hour groups Control group (usual care) |
MBST and CBT equivalent in reducing pain and improving function showing greater improvements compared to usual care |
| Zgierska et al[23] | 2016 | 35 participants with chronic LBP | Meditation cognitive therapy and control (8 weeks, 2hrs/w)
Control/usual care group |
Significant decrease in pain intensity (short and long-term) |
| Anheyer et al[24] | 2017 | Systematic review & Meta-analysis
7 RCTs with patients with LBP |
MBSR associated with short-term improvements in pain intensity and physical functioning | |
| Banth & Ardebil[25] | 2018 | 88 patients with NSCLBP | MBSR (8 sessions) and control (usual care) | MBSR significant reduction in pain and improvement in physical and mental quality of life |
| Smith & Langen[12] | 2020 | Systematic review
12 studies in patients with chronic LBP |
Mindfulness-based interventions
Control groups |
Improvement in pain scores and quality of life after mindfulness interventions |
| Qaseem et al [26] | 2017 | Systematic review to establish practice guidelines | MBSR recommended for patients with chronic LBP |
MBIs are suggested to have greater effects on pain-related catastrophising, especially in the presence of high levels of pain intensity, compared to traditional cognitive behavioural therapy (CBT) approaches.[11][18] In general, participants practising mindfulness (especially MBSR) for chronic pain, displayed significantly improved outcomes of pain measures as well as quality of life and mental health measures compared to matched control groups.[12] Patients with chronic pain who engaged in mindfulness practice were generally found to be able to find new ways of living with and accepting pain, resulting in a less negative impact on their daily lives.[12] The need for methodologically sound studies on MBI for patients with chronic pain is however reiterated in many studies.[16]
Mechanism of Pain Reduction through Mindfulness Practice[edit | edit source]
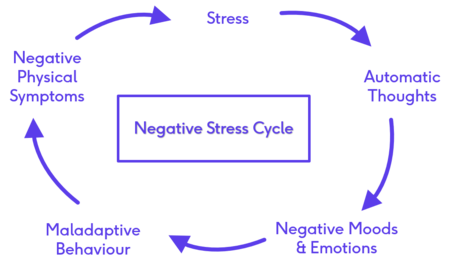
Exploring the mechanisms by which mindfulness influences stress and pain, necessitate an explanation of the negative stress cycle that develops as a result of the long-term and unrelenting presence of stress and pain.[1] The negative stress cycle is set off by the occurrence of a stressful event which is often not relenting. The patient enters into a cycle of automatic thoughts about this event (the stress/pain) which leads to negative moods and emotions, ultimately resulting in maladaptive behaviours which often end up sustaining this cycle by worsening their symptoms (Figure 3).[11][1]
Figure 3. The Negative Stress Cycle [1]
The practice of mindfulness is able to break this cycle by interrupting the “automatic thoughts” stage achieved through turning off the autopilot mode of living and guiding the awareness back to the present moment with an attitude of non-judgement and non-reactance.[12][1] MBSR proposes that mindfulness practice “will allow for the “uncoupling” of the bottom-up, afferent, sensory-driven components of pain from the top-down, psychological, cortically-driven components of pain”.[12] This suggests that awareness can result in a dissociation between the physical sensation of pain from the emotions and thoughts previously attached to pain.[12][25] The goal of mindfulness, therefore, is not to eliminate the stress or pain, but to teach the patient self-awareness and alternate responses to stress and pain by embracing the pain, accepting the moment for what it is.[12][1] By making peace with the pain, the patient is able to better manage the pain with fewer negative coping responses (including fear and anxiety).[12][25][1]
Pain reduction through mindfulness meditation also utilises different neural mechanisms as compared to placebo analgesia.[15] Besides its proposed influence on pain affect, mindfulness-based pain relief also engages brain mechanisms involved in mediating the cognitive modulation of pain, which include:[4][13][15][20]
- Decreased activity in neural regions associated with low-level nociceptive processing (eg thalamus)
- Increased activity in neural regions associated with interoceptive awareness (eg right anterior insula)
- Top-down executive control (eg ACC)
- Cognitive reappraisal of sensory information (eg orbitofrontal cortex)
The ultimate strength of mindfulness lies in the neural changes it causes. Keeping in mind that “nerves that fire together, wire together”, repetitive practise of mindfulness meditation leads to changes in neural pathways resulting in a more calm, accepting disposition towards life.[1]
Several studies have found that long-term meditation practice can lead to increased pain threshold values and lower pain sensitivity even while the practitioners are not engaged in mindfulness practice.[4] Grant et al[27] studied Zen meditators using fMRI and found that long-term meditators had distinct neural pathways which predicted their low pain sensitivity. These neural pathways suggest a reduction in cognitive-emotional and evaluative processing during aversive stimulation which relates to reduced connectivity (greater “decoupling”) between the cognitive and evaluative areas of pain processing and the sensory component of pain processing.[4][1][27] These Zen meditators still preserved the capacity to feel the pain on a sensory level, but displayed reduced affective appraisal, or less activation in the evaluative and emotional areas of the brain, related to the painful event.[4][27] These pathways also correspond well to the psychological construct (present moment, non-judgmental awareness) of mindfulness which resulted in the meditators possessing quieter and less reactive brains.[27]
Key messages[edit | edit source]
- Mindfulness and neuroscience research has exploded in recent years
- Mindfulness has many benefits, especially for stress-reduction
- Through the wonder of neuroplasticity, mindfulness has shown to have a direct effect on our physiology and our psychology
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Shrey Vazir. Mindful Meditation in Chronic Pain Management. Plus Course. 2021
- ↑ Nunes A, Castro SL, Limpo T. A review of mindfulness-based apps for children. Mindfulness. 2020 Sep;11(9):2089-101. DOI:10.1007/s12671-020-01410-w
- ↑ 3.0 3.1 Creswell JD. Mindfulness interventions. Annual review of psychology. 2017 Jan 3;68:491-516. DOI: 10.1146/annurev-psych-042716-051139
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 Zeidan F, Baumgartner JN, Coghill RC. The neural mechanisms of mindfulness-based pain relief: a functional magnetic resonance imaging-based review and primer. Pain reports. 2019 Jul;4(4). DOI:10.1097/PR9.0000000000000759
- ↑ 5.0 5.1 5.2 Tang YY, Hölzel BK, Posner MI. The neuroscience of mindfulness meditation. Nature Reviews Neuroscience. 2015 Apr;16(4):213-25. DOI:10.1038/nrn3916
- ↑ Bauer CC, Caballero C, Scherer E, West MR, Mrazek MD, Phillips DT, Whitfield-Gabrieli S, Gabrieli JD. Mindfulness training reduces stress and amygdala reactivity to fearful faces in middle-school children. Behavioural Neuroscience. 2019 Dec;133(6):569. DOI:10.1037/bne0000337
- ↑ Young KS, van der Velden AM, Craske MG, Pallesen KJ, Fjorback L, Roepstorff A, Parsons CE. The impact of mindfulness-based interventions on brain activity: A systematic review of functional magnetic resonance imaging studies. Neuroscience & Biobehavioral Reviews. 2018 Jan 1;84:424-33. DOI: 10.1016/j.neubiorev.2017.08.003
- ↑ 8.0 8.1 Gotink RA, Meijboom R, Vernooij MW, Smits M, Hunink MM. 8-week mindfulness based stress reduction induces brain changes similar to traditional long-term meditation practice–a systematic review. Brain and cognition. 2016 Oct 1;108:32-41. DOI:10.1016/j.bandc.2016.07.001
- ↑ Zimmerman B, Finnegan M, Paul S, Schmidt S, Tai Y, Roth K, Chen Y, Husain FT. Functional brain changes during mindfulness-based cognitive therapy associated with tinnitus severity. Frontiers in neuroscience. 2019 Jul 24;13:747. DOI:10.3389/fnins.2019.00747
- ↑ Siegel DJ. Mindfulness training and neural integration: Differentiation of distinct streams of awareness and the cultivation of well-being. Social cognitive and affective neuroscience. 2007 Dec 1;2(4):259-63. DOI:10.1093/scan/nsm034
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 Edwards RR, Dworkin RH, Sullivan MD, Turk DC, Wasan AD. The role of psychosocial processes in the development and maintenance of chronic pain. The Journal of Pain. 2016 Sep 1;17(9): T70-92. DOI:10.1016/j.jpain.2016.01.001
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 12.11 12.12 12.13 Smith SL, Langen WH. A systematic review of mindfulness practices for improving outcomes in chronic low back pain. International Journal of Yoga. 2020 Sep;13(3):177. DOI:10.4103/ijoy.IJOY_4_20
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 McClintock AS, McCarrick SM, Garland EL, Zeidan F, Zgierska AE. Brief mindfulness-based interventions for acute and chronic pain: A systematic review. The Journal of Alternative and Complementary Medicine. 2019 Mar 1;25(3):265-78. DOI:10.1089/acm.2018.0351
- ↑ Ngamkham S, Holden JE, Smith EL. A systematic review: mindfulness intervention for cancer-related pain. Asia-Pacific journal of oncology nursing. 2019 Apr;6(2):161. DOI:10.4103/apjon.apjon_67_18
- ↑ 15.0 15.1 15.2 15.3 15.4 Zeidan F, Emerson NM, Farris SR, Ray JN, Jung Y, McHaffie JG, Coghill RC. Mindfulness meditation-based pain relief employs different neural mechanisms than placebo and sham mindfulness meditation-induced analgesia. Journal of Neuroscience. 2015 Nov 18;35(46):15307-25. DOI:10.1523/JNEUROLSCI.2542-15.2015
- ↑ 16.0 16.1 Hilton L, Hempel S, Ewing BA, Apaydin E, Xenakis L, Newberry S, Colaiaco B, Maher AR, Shanman RM, Sorbero ME, Maglione MA. Mindfulness meditation for chronic pain: systematic review and meta-analysis. Annals of Behavioral Medicine. 2017 Apr 1;51(2):199-213. DOI:10.1007/s12160-016-9844-2
- ↑ International Association for the Study of Pain. IASP Terminology. Last Updated: December 14, 2017. [Accessed 29 March 2021].
- ↑ 18.0 18.1 Elvery N, Jensen MP, Ehde DM, Day MA. Pain catastrophizing, mindfulness, and pain acceptance. The Clinical journal of pain. 2017 Jun 1;33(6):485-95. DOI:10.1097/AJP.0000000000000430
- ↑ 19.0 19.1 Niazi AK, Niazi SK. Mindfulness-based stress reduction: a non-pharmacological approach for chronic illnesses. North American journal of medical sciences. 2011 Jan;3(1):20. DOI:10.4297/najms.2011.320
- ↑ 20.0 20.1 Zeidan F, Martucci KT, Kraft RA, Gordon NS, McHaffie JG, Coghill RC. Brain mechanisms supporting the modulation of pain by mindfulness meditation. J Neurosci. 2011 Apr 6;31(14):5540-8. DOI:10.1523/JNEUROSCI.5791-10.2011.
- ↑ Morone NE, Greco CM, Moore CG, Rollman BL, Lane B, Morrow LA, Glynn NW, Weiner DK. A mind-body program for older adults with chronic low back pain: a randomized clinical trial. JAMA internal medicine. 2016 Mar 1;176(3):329-37. DOI:10.1001/jamainternmed.2015.8033
- ↑ Cherkin, D.C., Sherman, K.J., Balderson, B.H., Cook, A.J., Anderson, M.L., Hawkes, R.J., Hansen, K.E. and Turner, J.A., 2016. Effect of mindfulness-based stress reduction vs cognitive behavioural therapy or usual care on back pain and functional limitations in adults with chronic low back pain: a randomized clinical trial. Jama, 315(12), pp.1240-1249. DOI:10.1001/jama.2016.2323.
- ↑ Zgierska AE, Burzinski CA, Cox J, Kloke J, Stegner A, Cook DB, Singles J, Mirgain S, Coe CL, Bačkonja M. Mindfulness meditation and cognitive behavioral therapy intervention reduces pain severity and sensitivity in opioid-treated chronic low back pain: pilot findings from a randomized controlled trial. Pain Medicine. 2016 Oct 1;17(10):1865-81. DOI: 10.1093/pm/pnw006
- ↑ Anheyer D, Haller H, Barth J, Lauche R, Dobos G, Cramer H. Mindfulness-based stress reduction for treating low back pain: a systematic review and meta-analysis. Annals of internal medicine. 2017 Jun 6;166(11):799-807. DOI: 10.7326/m16-1997
- ↑ 25.0 25.1 25.2 Banth S, Ardebil MD. Effectiveness of mindfulness meditation on pain and quality of life of patients with chronic low back pain. International journal of yoga. 2015 Jul;8(2):128. DOI:10.4103/0973-6131.158476
- ↑ Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Annals of internal medicine. 2017 Apr 4;166(7):514-30. DOI: 10.7326/M16-2367.
- ↑ 27.0 27.1 27.2 27.3 Grant JA, Courtemanche J, Rainville P. A non-elaborative mental stance and decoupling of executive and pain-related cortices predicts low pain sensitivity in Zen meditators. PAIN®. 2011 Jan 1;152(1):150-6. DOI:10.1016/j.pain.2010.10.006