Medical Related Issues in Sports Medicine
Original Editor - Your name will be added here if you created the original content for this page.
Top Contributors - Lucinda hampton, Kate Pribyl, Kellen Allen, James Teel, Josh Williams, Kim Jackson, 127.0.0.1, Evan Thomas, WikiSysop, Tony Lowe, Alyssa Juarez and Wanda van Niekerk
Introduction[edit | edit source]
This page brings to light some medical related issues in sports that it is important to be aware of, namely:
- Sudden Cardiac Arrest
- Asthma
- Mononucleosis aka Epstein-Barr Virus
- Sickle Cell Anemia
- Diabetes
- Hypertension
- Rhabdomyolysis
Sudden Cardiac Death in Sports[edit | edit source]
Sudden cardiac arrest is defined by the NIH as a condition in which the heart unexpectedly ceases beating [1]. While rare, sudden cardiac death is the leading cause of nontraumatic cause of death among young athletes.[2]
The below brief video gives an overview of the condition.
Causes include: Coronary artery disease; commoto cordis; hypertrophic, dilated and arrythmogenic right ventricular myopathy, marfan Syndrome and myocarditis[4]. In incidences where an abnormality cannot be identified post mortem, the cause hypothesised to be related to: inherited arrhythmic disorders; ion channel disorders; familial catecholamenergic polymorphic ventricular tachycardia.
Incidence of SCD in the high school athletic population is estimated at 1 out of every 100,000 to 200,000. Incidence in collegiate athletes is 1 out of every 65,000 to 69,000 [5]. There also seems to be a higher incidence in the African American population (1 out of every 1,700.)
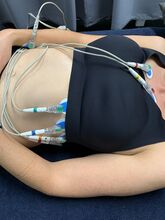
Clinical Presentation/Characteristics: Sports Medicine personnel should suspect sudden cardiac arrest (SCA) and impending death when an athlete collapses and is unresponsive. Immediately asses the patient’s airway, breathing, circulation, and rhythm if an AED is available. Look for seizure like activity or myoclonic jerking as both can be present following a SCA[6]. Some athlete may make complaints of dizziness, lightheadedness, or a racing pulse before collapsing. An hour before the incident, athletes may complain of chest pain, shortness of breath, nauseas and or vomiting [1]
Medical Exam/screening/testing: Typically a SCA is diagnosed after the fact by a cardiologist or a specialist known as a cardiac electrophysiologist. A barrier of tests are done to elicit the underlying cause for the arrest in those lucky enough to survive it. Tests and measures analyzed by these specialists include but are not limited to electrocardiograms, echocardiography, multiple gated acquisition testing, cardiac catheterization, electrophysiology study, and blood tests to ascertain levels of potassium, magnesium and other chemicals important in electrical signaling[1]. The American Heart Association has compiled a preparticipation screening known as the 12-Element Preparticipation Cardiovascular Screening for Competitive Athletes. It details important history questions to ask the athlete in their personal and family history as well as important physical examination techniques [6].
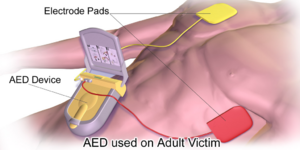
Treatment for the Arrested Athlete: Any athlete who is unresponsive after a collapse should be treated immediately and SCA is suspected first until ruled out. CPR protocols should be initiated if breathing and pulse are absent. Initiate EMS protocols. CPR should not be stopped until the AED has been retrieved and an analysis of the rhythm is initiated. Continue CPR and defibrillation as indicated until the appropriate emergency responders arrive[7].
The greatest factor that causes a SCA to advance to a SCD is the time from arrest to defibrillation [8]. Rates of survival are estimated to be 41% to 74% of a bystander performs CPR appropriately and defibrillation occurs within 3 to 5 minutes of the arrest. Remember that AEDs are safe to use in weather conditions such as rain or ice. However, if the athlete is lying in a puddle or on a wet surface he or she must be moved before defibrillation is safe. Likewise, move athletes who are on a metal surface to a nonmetal surface before defibrillation[6].
Resources: Please refer to the National Institute of Health, the National Athletic Training Association, the American Heart Association, and local physicians for more information on the proper management and monitoring for athletes with SCD.
Clinical Bottom Line: AED implementation is crucial to the survivability of the athlete.
- Your goal as a sports medicine provider should be to provide the first shock before the 3-5 minute mark.
- Access to resources and proper planning before any incident takes place is a necessity.
- A preparticipation physical examination is essential to uncover episodes of exertional syncope, presyncope, chest pain, personal and/or family history of SCA, a family history of SCD, and exercise intolerance[6].
Asthma in Sports[edit | edit source]
Physical training has been shown to be beneficial for asthmatic adults and children in improving asthma control and asthma-related quality of life. Exercise training also reduces the risk of asthma exacerbations, improves exercise capacity, and decreases frequency and severity of exercise induced asthma (EIB). To minimize the risk of exercise induced bronchoconstriction [EIB], asthma must be well controlled, and specific pharmacological and nonpharmacological preventative measures can be taken ie athletes must have optimal asthma control and apply preventative measures against EIB, taking into account antidoping regulations for asthma medications.[9]
This video below highlights some of the issues
For more see Exercise Induced Asthma
Mononucleosis in Sports[edit | edit source]
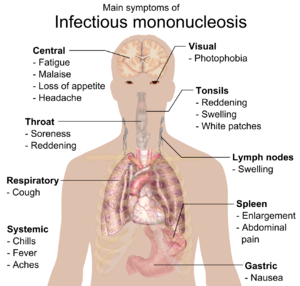
Mononucleosis commonly known as infectious mononucleosis is normally caused by the Epstein-Barr virus (EBV)[11]. Mononucleosis can affect several systems including lymph nodes, oral cavity, pharynx, lungs, spleen, liver, and possibly central nervous system (potential future complications).
Considerations for Sports Participation With the risk of splenic injury after contracting infectious mononucleosis, considerations must be taken when deciding to allow participation of sports. Recommendations for light, noncontact activity is participation may resume 3 weeks after initial onset of symptoms. Light, noncontact activity describes avoidance of chest or abdominal trauma and minimal exertion activities. Information provided for recommendations to return to contact activity is controversial, but literature suggests a minimal of 3 weeks and a gradual progression of participation.[12] Currently there are no set guidelines for the decision to allow players to return to their sport, and even with the 3 week time frame recommendation, each player needs individualized treatment given the course of the illness is variable.[13]
Clinical Bottom Line: Sports or activity participation should be limited to a minimum of 3 weeks to prevent splenic rupture with monitoring of symptoms and progression of activity.[12]
Sickle Cell Anemia in Sports[edit | edit source]
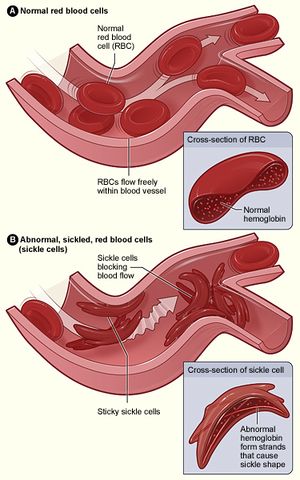
Sickle Cell Anemia (SCA) involves a distortion of red blood cells from their typical form. and are more likely to clog blood flow leading to infection, stroke and acute chest syndrome [14]. In the athletic world, sickle cell disease has been most prominently discussed in relation to football.[15], [16]
Clinical Presentation/Characteristics: Signs and symptoms will be different from person to person and are mostly related to disease complications. A sickle cell crisis can occur without warning with pain more severe than childbirth or postsurgical pain. The pain is often described as sharp, stabbing, knifelike, or throbbing [17]. The most common locations for pain exacerbation include the low back region, left arm, abdomen, and chest. Temperature changes, stress, illness, dehydration, and high altitudes often bring on these crises [6].
Identifying an Athlete in Crisis: The following are features of an exertional sickle cell collapse [18]:
1) Athletes will slump to the ground which differentiates the presentation from cardiac pathology (sudden fall) and heat cramps (hobbling).
2) Muscle strength will be abnormally weak comparative to the level of pain experienced by the athlete. The opposite presentation will occur in athletes with heat cramps.
3) Athletes will initially be able to communicate to the practitioner as opposed to an athlete who experiences a cardiac arrhythmia. Typically a cardiac arrhythmia leads to unconsciousness.
4) Muscles will look and feel normal upon palpation unlike someone undergoing heat cramps.
5) Rapid tachypnea will be present despite optimal air flow due to lactic acidosis
6) Temperatures usually are under 103 degrees Farenheit as opposed to over 106 degrees found in heat stroke.
Steps to take on the sideline when a Crisis is identified [18], [6]:
1) Treat as a medical emergency
2) Monitor Vital Signs
3) Give supplemental oxygen if available
4) Cool Athlete as needed
5) If no immediate improvement is made activate emergency response and prepare for cardiopulmonary resuscitation.
6) Tell physicians to expect explosive rhabdomyolysis
Medical Management/ Treatment: Pain related to an episode or crisis can be managed with OTC medications such as ibuprofen or aspirin. In the most severe crises, the patient will be admitted to the hospital and administered opioids such as morphine and other pain relieving medications. In severe crises where anemia, splenic sequestration, or acute chest syndrome occur, medicinal intervention includes blood transfusion, a spleenectomy, antibiotics to prevent infection, medicine to open airways, or administration of oxygen may be warranted. Interventions are considered on a case-by-case basis [19].
PT Management: The following are tips for preventing a sickling crisis.
1) The athlete should be allowed to set his/her own pace in conditioning exercises. They should be allowed to build training sessions slowly and have longer rest periods between bouts and repetitions.
2) Preseason strength and conditioning programs are encouraged to maintain the athlete’s preparedness for physical activity and should be sports specific.
3) Let athlete’s set their own workout pace, they typically do not have exacerbations into crisis.
4) Immediately stop activity with the onset of muscle cramps, inability to “catch breath,” pain, and swelling.
5) Remember that repetitive high level training leads to lactic acidosis and could cause a crisis. Therefore, training that leads to high levels of lactic acidosis must allow for extended recovery periods between repetitions in order to prevent a crisis.
6) Educate athletes on the importance of communication regarding the occurrence of sickle cell symptoms.
7) Finally, heat stress, dehydration, asthma, infection, and altitude can all predispose an athlete to a sickle cell crisis. Therefore, the athlete must hydrate, manage asthma effectively, modulate work load to fit the environmental stressors, not workout if ill, and modify workout load if new to a region with altitude[18], [6].
Multidisciplinary Teams: Critical to coordinate the athlete’s training, medical care, and engagement in team activities. To effectively accomplish this, the primary care physician, athlete and parental units, sports medicine personnel, coaching staff, and other support personnel must work to maintain optimal sports participation. Sports are not contraindicated for those with SCA, but the aforementioned persons must work to establish appropriate workout regimens, provide adequate access to emergency response intervention, and have open lines of communication.
Clinical Bottom Line: Physical activity and participation in sport are not prohibited for those with SCA. However the athlete should not be subjected to exercise conditioning tests, must be given elongated time to reach appropriate conditioning levels, must be cognizant of current health status, and be educated on the disease.
Diabetes in Sports[edit | edit source]
Diabetes’ prevalence in the United States continues to rise exponentially largely owing to the obesity epidemic.[20]
PT management: The American Diabetes Association (ADA) has set guidelines that state all individuals with DM should be given the chance to experience the benefits of exercise.[21]Exercise has been associated with improved quality of life and metabolic control in the DM population.[22]With the appropriate adjustment of insulin dosage, glucose self-monitoring, dietary management, and properly timed exercise, children with DM should be able to participate.[21]When considering athletics for individuals with DM, glycemic control is crucial and should be addressed through diet, exercise, and medication.[22]Prior to initiating physical activity, glycemic index should be controlled to a reasonable level. The athlete should also consider being evaluated by their physician for coronary disease prior to the start of an exercise regime. When participating in physical activity, if glucose levels are above 250 prior to exercise and ketones are present then exercise must be postponed. If glucose are at or exceed 300, then exercise is inadvisable with or without ketones. Glucose levels at or below 200 are cleared for physical activity, but should be under close watch.[23]Also be sure to watch for insulin omission by those athletes aiming to lose weight in order to compete in athletics with specific weight categories such as wrestling, boxing, and weightlifting.[23]
CRITICAL: When participating in various sports, diabetic athletes should be advised to wear a MedicAlert-type bracelet and/or necklace that indicates their specific diagnosis of DM1 or DM2 and the appropriate pharmaceutical information.[20]
DM2: Physical activity has been noted as a key component to acutely lower blood glucose levels in DM2. Acute effects of physical activity in DM2 are abnormal insulin secretion and peripheral insulin resistance. These effects acutely, but favorably, change abnormal glucose levels and insulin resistance. Mild to moderate physical activity has been reported to decrease blood glucose levels in this population.[22], [24]The magnitude of these effects are directly correlated to exercise duration and intensity. Mild to moderate physical activity has also been shown to reduce insulin resistance by increasing peripheral and splanchnic insulin sensitivity.[22], [24]The acute effects of exercise are lost within a few days and the benefits of a single exercise session are short lived; therefore, regular exercise performed at moderate intensities are required to lessen insulin resistance.[22]
DM1: Those individuals with DM1 have been encouraged to participate in regular physical activity. These athletes are often young and more competitive than their DM2 counterparts. Athletes with DM1 meeting the activity guidelines set by the ADA have triglyceride levels lower than their inactive peers; however, continuous aerobic activity frequently causes hypoglycemia.[23]This can occur directly after exercise and up to 7-11 hours later.[24]If exercise is performed in the late afternoon, then hypoglycemia typically occurs during late-night sleep. High intensity exercises can cause elevations in blood glucose concentrations. These elevations may be sustained long into recovery but may be corrected with appropriate insulin dosing. DM1 athletes should work closely with their personal physicians while participating in physical activity to monitor their glucose levels before, during, and after exercise. Studies have reported that periods of continuous moderate-intensity exercise interspersed with bouts of high-intensity exertions my protect from exercise-induce hypoglycemia.[24]This type of intermittent exercise can be seen in recreational team or field sports like soccer, basketball, or football.[23]This form of exercise has been shown to cause low recovery glucose levels due to an increase in the need for muscle glycogen restoration. Some studies have reported that an increase in glycaemia in early recovery helped to prevent post exercise hypoglycemia in DM1 athletes while others reported an increase in nocturnal hypoglycemia in the same population.[24]
Exercise Recommendations: Athletes with DM should participate in aerobic exercise five or more days a week while incorporating a minimum of three days of resistance training.[22], [20]There is currently not a consensus on the ideal frequency, but these values are based on expert opinion. Intensity for those beginning an exercise program should be kept at 50%-70% of their maximum oxygen consumption; at intensities where they can still carry on conversation.[20]These parameters allow the athlete to participate for longer periods allowing for increase in aerobic capacity and caloric energy expenditure that will aid in weight loss/control.[23]Intensity can be further increased for those who frequently participate in physical activity. When considering the type or mode of exercise, medical recommendations have focused largely on aerobic activity; however, recent studies have shown similar improvements in insulin levels with resistance type exercise.[22], [20]The ADA recommends a combination of the two modes. Resistance training should target all major muscle groups consisting of six to eight separate exercises that should be progressed to include three sets of eight to ten repetitions per movement. Higher level DM athletes with well controlled blood glucose levels are able to participate in physical activity at the same level as their non-diabetic peers.
Multidisciplinary Teams: The management of athletes with DM is very much a multidisciplinary team approach. The top tier includes both the athlete’s endocrinologist and primary care physician who both aid in the medical/pharmaceutical management of the condition. The next tier includes various other health professionals including nutritionists and physical/recreational therapists. These parties focus on the best nutritional regime while incorporating the most appropriate exercise schedule to ensure the best outcome while avoiding medical hazards like hypo- and hyperglycemia.[22]Coaches and athletic trainers also play a very large role in the management of this athletic population.[23], [25]Athletic trainers are equipped with the tools and skills needed to manage athletes with DM. These include diabetic care plans; supplies for athletic training kits; pre-participation physical examinations; the ability to recognize, treat, and prevent hypoglycemia and hyperglycemia; the skill to administer insulin; the knowledge of appropriate travel recommendations; and how to manage athletic injury in the DM population.[25]The athletic trainers often get more time than anyone else with these athletes, and so their proficiency in these skills is crucial to the safety and well-being of the DM athlete.
Clinical Bottom Line: Physical activity has been shown to reduce several of the complications induced by DM. Athletes with DM are on a case-by-case basis so their participation in physical activity and insulin regime will have to be modified according to the athlete’s individual needs.[20]However, mild to moderate exercise has been shown to have the best effects on athletes with DM while producing the least risk.[22]Blood glucose control for these athletes may take several bouts of trial-and-error in order to develop the best practice. Hyper/hypoglycemia are the primary concerns for these athletes, but both can be controlled through insulin dosage modification and increase/decrease of carb consumption both before and after exercise.[22], [20]
Hypertension in Sports[edit | edit source]
Athletes and physically active individuals are often (and inaccurately) thought to be free of hypertension and cardiovascular disease. Although athletic individuals are 52% less likely to develop hypertension than the general population, it can occur. African americans, the elderly, people who are obese, and individuals with a history of renal disease, diabetes, or familial hypertension are at a greater risk of developing hypertension themselves. Additionally, wheelchair athletes who sustained a spinal cord injury are more likely to have hypertension due to abnormal autonomic control[26].
Athletes that are known to have hypertension should monitor their blood pressure prior to physical activity, and should not resume or initiate sports participation until their blood pressure is controlled. Dynamic and isometric exercise have an especially significant effect on blood pressure. The following recommendations have been made for exercise restrictions of hypertensive athletes:[26]
| High-normal blood pressure | No restrictions |
| Controlled mild to moderate hypertension (<140/90 mm Hg) | No restrictions on dynamic exercise; possible limit on isometric training or sports in some patients |
| Uncontrolled hypertension (>140/90 mm Hg) | Limited to low-intensity dynamic exercise; avoid isometric sports |
| Controlled hypertension with end-organ damage | Limited to low-intensity dynamic exercise; avoid isometric sports |
| Severe hypertension with no end-organ involvement | Limited to low-intensity dynamic exercise, with participation only if blood pressure is under adequate control |
| Secondary hypertension of renal origin | Limited to low-intensity dynamic exercise; avoid “collision” sports that could lead to kidney damage |
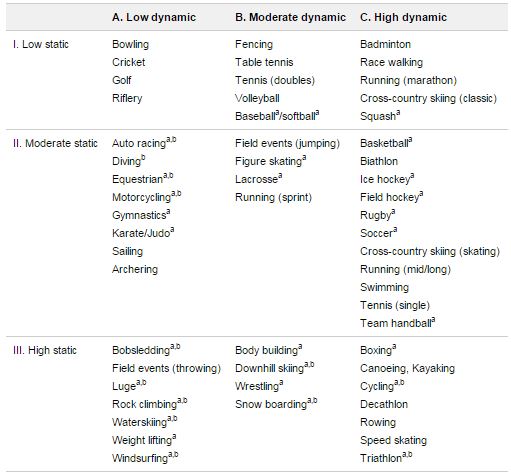
Below is a chart that describes sports in terms of their dynamic and static properties:[27]
ALL potential athletes should go be screened and evaluated for cardiovascular disease, and is discussed in further detail in the following section.
PT Management: Measurement of vital signs is an important aspect of a thorough systems review, which physical therapists should be conducting with every single patient. Physical therapists that work with athletic and physically active populations should known how to accurately measure blood pressure and monitor response to exercise. In order to fully understand how an athlete responds to various levels of exercise, the physical therapist should use blood pressure measurements to gain information on the athletes baseline cardiovascular status, their response to exercise and physical activity, and how those measurements impact clinical decision making.[28]
Physical therapists should also be able to serve as a fitness and wellness coach to individuals with hypertension and guide them to making the best diet and exercise decisions.
Rhabdomyolysis[edit | edit source]
Physical therapists may play an essential role in preventing rhabdomyolysis, identifying athletes who demonstrate signs and symptoms of rhabdomyolysis, and making return to sport decisions following rhabdomyolysis.
Watch this 8 minute video about the condition
Prevention[30]
- Acclimatization - gradually increase physical activity, intensity, duration, and frequency
- Monitor environmental factors - high heat and humidity are risk factors to developing rhabdomyolysis
- Hydrate - make sure athletes are drinking plenty of water before, during, and after physical activity
- Replenish electrolytes
- Maintain good sodium and potassium intake
- Wear light clothing that easily allows for heat dissipation
Treatment[30]
- Provide medical treatment for any complications (renal failure, hyperkalemia, hypocalcemia)
- Hydrate
- Increase carbohydrates to replenish glycogen stores
- Avoid drugs and alcohol, as well as any medications that can lead to rhabdomyolysis
- Allow proper time for the body to heal before returning to physical activity
Return to Sport: In mild cases, athletes are usually able to return within 2-4 weeks. The best way to determine return to sport is to monitor CK levels, but that is rarely possible because baseline measures are not often available. The first step in making return to sport decisions is to classify the athlete as either high or low risk for reoccurance.
High Risk for Reoccurrance:[30]
- When activities have been restricted, it still takes more than one week for the athlete to recover from activity.
- Persistent elevation of blood CK levels(greater than five times the upper limit of the normal range), even when they have had strict rest from physical activity for longer than two weeks.
- Their rhabdomyolysis experience was complicated by a kidney injury of any sort.
- They have a personal history or a family history of rhabdomyolysis
- Personal or family history of recurrent muscle cramps or severe muscle pain that interferes with activities of daily living or sports performance.
- Personal or family history of malignant hyperthermia or family history of unexplained complications or death following general anesthesia.
- Personal or family history of sickle cell disease.
- Muscle injuries after low to moderate physical activity.
- Personal injury of significant heat stroke.
- Their original CK blood value was over 100,000.
Low Risk for Reoccurrance[31]: To be considered low risk, the athlete must not have any of the high risk conditions and must display at least one of the following:
- Rapid clinical recovery and CK normalization after exercise restrictions
- Sufficiently fit or well trained athlete with a history of very intense training/exercise bout
- No personal or family history of rhabdomyolysis orprevious reporting of debilitating exercise-induced muscle
pain, cramps, or heat injury - No existence of other group or team-related cases of exertional rhabdomyolysis during the same exercise sessions
- Not suspected or documented concomitant viral illness or infectious disease
- Not taking a drug or dietary supplement that could contribute to the development of ER
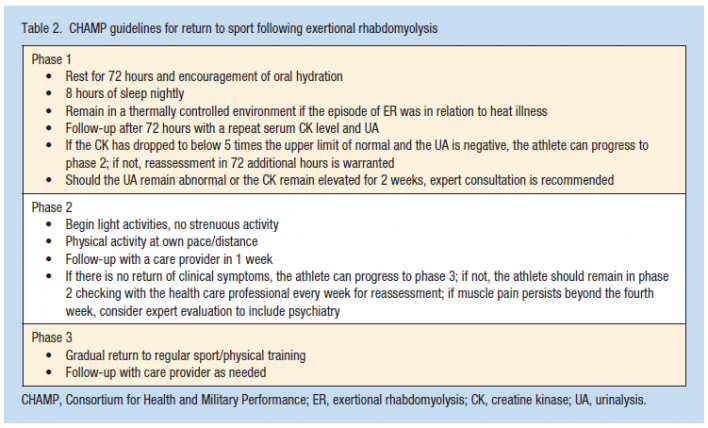
Return to sport decisions should be individualized, and should take into account whether or not the athlete is at a low or high risk for reoccurrance. Although there is no evidence-based protocol for RTS, the military came up with their own guidelines for return to activity following an episode of rhabdomyolysis, and is pictured below.
Conclusion[edit | edit source]
Hopefully this page will bring to life some important issues to be aware of in the sporting populace and have help with your knowledge on this topic. The links all add further depth to the read.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 National Institutes of Health, National Heart, Lung, and Blood Institute. Sudden cardiac arrest. http://www.nhlbi.nih.gov/health/health-topics/topics/scda/ (accessed 7 Nov 2015).
- ↑ Yow AG, Rajasurya V, Sharma S. Sudden cardiac death. InStatPearls [Internet] 2021 May 7. StatPearls Publishing. Available:https://www.ncbi.nlm.nih.gov/books/NBK507854/ (accessed 1.6.2022)
- ↑ Sudden Cardiac Arrest | Cincinnati Children's Available from: https://www.youtube.com/watch?v=iptEygAuDRI&app=desktop (last accessed 18.12.2019)
- ↑ Maron BJ. Sudden death in young athletes. N Engl J Med. 2003;349(11):1064–1075.
- ↑ Drezner JA, Rogers KJ, Zimmer RR, Sennett BJ. Use of automated external defibrillators at NCAA Division I universities. Med Sci Sports Exerc.fckLR2005;37(9):1487–1492.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 National Athletic Trainers' Association. National athletic trainers' association position statement:preventing sudden cardiac arrest. Journal of Athletic Training 2012;47:96-118.
- ↑ Emergency Care Committee, Subcommittees and Task Forces of the American Heart Association. 2005 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care, part 3: overview of CPR. Circulation. 2005;112(suppl 24):IV12–fckLRIV18.
- ↑ Drezner JA, Courson RW, Roberts WO, Mosesso VN Jr, Link MS, Maron BJ. Inter-association Task Force recommendations on emergency preparedness and management of sudden cardiac arrest in high school and college athletic programs: a consensus statement. J Athl Train. 2007; 42(1):143–158.
- ↑ Côté A, Turmel J, Boulet LP. Exercise and asthma. InSeminars in respiratory and critical care medicine 2018 Feb (Vol. 39, No. 01, pp. 019-028). Thieme Medical Publishers. Available from: https://www.thieme-connect.com/products/ejournals/abstract/10.1055/s-0037-1606215 (last accessed 18.12.2019)
- ↑ childrens hospgh exercise and asthma Available from: https://www.youtube.com/watch?v=P-i2TK1ol2g&feature=youtu.be (last accessed 18.12.2019)
- ↑ Lennon, P., Crotty, M., & Fenton, J. E. (2015). Infectious mononucleosis. BMJ, 350, 1-7. doi: http://dx.doi.org/10.1136/bmj.h1825
- ↑ 12.0 12.1 Putukian, M., O’Connor, F. G., Striker, P., McGrew, C., Hosey, R. G., Gordon, S., . . . Landry, G. ( 2008). Mononucleosis and athletic partipation: An evidence-based subject review. Clinical Journal of Sports Medicine, 18(4), 309-315. doi: 10.1097/JSM.0b013e31817e34f8
- ↑ Becker, J. A. & Smith, J. A. (2014). Return to play after infectious mononucleosis. Sports Health, 6(3), 232-238. doi: 10.1177/1941738114521984
- ↑ Tripette J, Loko G, Samb A, et al. Effects of hydration and dehydration on blood rheology in sickle cell trait carriers during exercise. Am J Physiol Heart Circ Physiol 2010;299:H908–14.
- ↑ Van Camp SP, Bloor CM, Mueller FO, Cantu RC, Olson HG. Nontraumatic sports death in high school and college athletes. Med Sci SportsfckLRExerc 1995;27:641-647.
- ↑ Eichner ER. Sickle cell trait in sports. Curr Sports Med Rep. 2010;9 (6):347–351.
- ↑ National Institute of Health, Genetic home reference. Sickle cell disease. http://ghr.nlm.nih.gov/condition/sickle-cell-disease (accessed 7 Nov 2015).
- ↑ 18.0 18.1 18.2 Eichner ER. Sickle cell consideration in athletes. Clin Sports Med. 2011;30:537–549.
- ↑ National Heart, Lung and Blood Institute. Evidence-based management of sickle cell disease: expert panel report, 2014. http://www.nhlbi.nih.gov/health-pro/guidelines/sickle-cell-disease-guidelines/(accessed 8 Nov 2015).
- ↑ 20.0 20.1 20.2 20.3 20.4 20.5 20.6 Shugart, C., Jackson, J., & Fields, K. (2010). Diabetes in Sports. Sports Health, 2(1), 29-38. doi:10.1177/1941738109347974
- ↑ 21.0 21.1 Valerio, G., Spagnuolo, M., Lombardi, F., Spadaro, R., Siano, M., & Franzese, A. (2005). Physical activity and sports participation in children and adolescents with type 1 diabetes mellitus. Nutrition, Metabolism and Cardiovascular Diseases, 17, 376-382. doi:10.1016/j.numecd.2005.10.012
- ↑ 22.0 22.1 22.2 22.3 22.4 22.5 22.6 22.7 22.8 22.9 Albright, A., Franz, M., Hornsby, G., Kriska, A., Marrero, D., Ullrich, I., & Verity, L. (n.d.). Exercise and Type 2 Diabetes. Medicine & Science in Sports & Exercise, 1345-1360.
- ↑ 23.0 23.1 23.2 23.3 23.4 23.5 Hornsby, W., & Chetlin, R. (2005). Management of Competitive Athletes With Diabetes. Diabetes Spectrum, 18(2), 102-107.
- ↑ 24.0 24.1 24.2 24.3 24.4 Iscoe, K., & Riddell, M. (2011). Continuous moderate-intensity exercise with or without intermittent high-intensity work: Effects on acute and late glycaemia in athletes with Type 1 diabetes mellitus. Diabetic Medicine, 824-832. doi:10.1111/j.1464-5491.2011.03274.x
- ↑ 25.0 25.1 Jimenez, C., Corcoran, M., Crawley, J., Hornsby, G., Peer, K., Philbin, R., & Riddell, M. (2007). National Athletic Trainers’ Association Position Statement: Management of the Athlete With Type 1 Diabetes Mellitus. Journal of Athletic Training, 42(4), 536-545.
- ↑ 26.0 26.1 Niedfeldt M. Managing hypertension in athletes and physically active patients. American Family Physician 2002;66(3):445-453. www.aafp.org/afp/2002/0801/p445.html (accessed 19 November 2015).
- ↑ European Society of Cardiology. Recommendations for participation in leisure-time physical activities and competitive sports for patients with hypertension. http://cpr.sagepub.com/content/12/4/326.short (accessed 19 November 2015).
- ↑ Frese E, Fick A, Sadowsky H. Blood pressure measurement guidelines for physical therapists. www.ncbi.nlm.nih.gov/pmc/articles/PMC3104931/ (accessed 19 November 2015).
- ↑ Mayo Clinic Rhabdomylosis Available from:https://www.youtube.com/watch?v=M8luZTZRRc8&app=desktop (last accessed 18.12.19)
- ↑ 30.0 30.1 30.2 Shaffer M. Rhabdomyolysis prevention and treatment in athletes. http://yourlivingbody.com/preventing-treating-rhabdomyolysis-athletes/ (accessed 19 November 2015).
- ↑ O'Connor F, Brennan F, Campbell W, Heled Y, Deuster P. Return to physical activity after exertionalfckLRrhabdomyolysis. http://missyleone.com/wp-content/uploads/2011/08/Return-Physical-Activity-after-Exertional-Rhabdomyolysis.pdf (accessed 19 November 2015).