Epstein-Barr Virus
Original Editors - Nicole Clark
Top Contributors - Nicole Clark, Lucinda hampton, Admin, Elaine Lonnemann, Kim Jackson, WikiSysop and Wendy WalkerIntroduction[edit | edit source]
Infectious mononucleosis is an acute infectious disease associated with Epstein-Barr virus that is characterized especially by fever, sore throat, swelling of lymph nodes, fatigue, and lymphocytosis and occurs primarily in adolescents and young adults.[1] It is usually a clinical diagnosis, with confirmation by serum testing, but may have suggestive findings on imaging
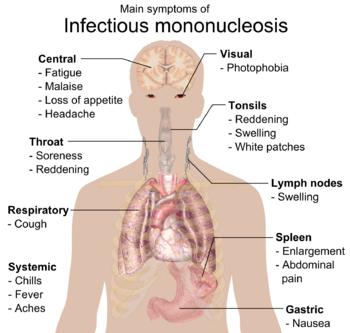
- Mononucleosis classically presents with fever, lymphadenopathy, and tonsillar pharyngitis. See image R
- It was originally called "mononucleosis" after abnormal mononuclear cells were found in patients with the clinical syndrome.[2]
- Later Epstein-Barr virus (EBV) was established as the cause of mononucleosis after an exposed healthcare worker developed a positive heterophile test (a rapid test which detects infectious mononucleosis that is caused by the Epstein Barr Virus)[3]
Etiology[edit | edit source]
The cause of mononucleosis is the Epstein-Barr virus (EBV), a type of herpesvirus spread by contact, typically with salivary secretions.
- Transmission is generally person-to-person, but EBV is not considered a highly contagious disease[3].
- It is thought to be spread primarily through a person-to-person route through salivary secretions. The EBV virus infects B-cells in the lymphoid tissue. Like other herpes viruses, it becomes a lifelong chronic infection with periodic shedding of virus[2].
- The duration of oral shedding is not entirely clear, but high levels of shedding can continue for a median of 6 months after illness onset.[3]
Epidemiolgy[edit | edit source]
It is estimated that up to 95% of adults in the world are eventually seropositive to EBV (widely disseminated in all population groups).
- Exposure to EBV, but often a subclinical infection, especially in children. Young adults (15-24) are more likely to be symptomatic[2].
- Mononucleosis is uncommon in adults: approximately 2% of all pharyngeal disease in adults is attributable to this disease.
- Adults are generally not susceptible to clinical illness because of previous exposure.
- In the United States, clinically evident infection occurs at rates estimated at 30 times higher in whites than in blacks (possibly because if acquired at a young (childhood) age, EBV is often subclinical ie earlier EBV exposures in blacks, and a higher frequency of asymptomatic infection as young children).
- After exposure, the EBV infects the epithelial cells of the salivary glands and the oropharynx. Lymphocytes residing in the tonsils get exposed to the virus and then enter the bloodstream. Lymphoid hyperplasia is common and may be seen as generalized lymphadenopathy, tonsillitis, and hepatosplenomegaly.
- The infection of the B-lymphocytes results in the production of immunoglobulins (heterophile antibodies)[3].
Characteristics/Clinical Presentation[edit | edit source]
- Fever
- Tonsillitis
- Lymphadenopathy and splenomegaly
- Occasionally hepatosplenomegaly
- Fatigue
- Occasionally: rash
Complications
- Splenic rupture: may be spontaneous
- Splenic infarction [2]
Associated Co-morbidities[edit | edit source]
While there are very few co-morbidities associated with mono, a select group of studies as shown a correlation between Chronic Fatigue Syndrome (CFS) and Mononucleosis. According to research the Epstein Barr Virus has many similar clinical features. It has yet to be determined whether or not the conditions are synonymous or just present with similar symptoms due to their viral nature of transmision. [4]
Medications[edit | edit source]
Symptomatic therapy is usually sufficient.
- Athletes are encouraged to discontinue sports during the acute phase (<3-4 weeks) to lower the risk of splenic rupture.[2]
- Antipyretics and anti-inflammatory medications help to treat fever, sore throat, and the general fatigue seen in this illness.
- Hydration, rest, and good nutritional intake should be encouraged.
- Corticosteroids are not generally recommended in the routine treatment of mononucleosis because of concerns with immunosuppression; however, in cases of airway obstruction, corticosteroids (and possible otolaryngology consultation) are indicated along with appropriate airway management[3].
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
The diagnostic test of choice for mononucleosis is the heterophile antibody (monospot) test (occasionally falsely negative in early disease and require repeat testing later in the course of the illness).
The most important entity to exclude from the differential diagnosis is primary HIV infection.
Splenic rupture is a rare complication in mononucleosis but can be potentially life-threatening if not diagnosed in a timely fashion[3].
Physical Therapy Management[edit | edit source]
Infectious Mononucleosis: PREFERRED PRACTICE PATTERNS 6B:
- Impaired Aerobic Capacity/Endurance Associated with Deconditioning
- Infectious mononucleosis is probably contagious before symptoms develop until the fever subsides and the oral and pharyngeal lesions disappear. Although infectious mononucleosis appears to be only mildly contagious, adherence to standard precautions, especially good handwashing and avoidance of shared dishware or food items with other people.
- The person with infectious mononucleosis should be cautioned against engaging in excessive activity, especially contact sports, which could result in splenic rupture or lowered resistance to infection. Usually this guideline is appropriate for a period of at least 1 month.
- Any sign of splenic rupture (e.g., abdominal or upper quadrant pain, Kehr's sign, sudden left shoulder pain, or shock) requires immediate medical evaluation.
- Any soft tissue mobilization or myofascial techniques necessary in the left upper quadrant, especially up and under the rib cage, must take into consideration the enlarged liver and/or spleen; indirect techniques away from the spleen are indicated.
- In rare cases mononucleosis impairs the CNS. Any change in neurologic status must be evaluated and reported to the physician.
- Changes in respiration or signs and symptoms of airway obstruction may require emergency intervention.[5]
See also relevant section in Medical Related Issues in Sports Medicine
Differential Diagnosis[edit | edit source]
Many other viral and some rickettsial illnesses have characteristics similar to EBV.
- The differential includes:
- cytomegalovirus
- human immunodeficiency virus (HIV)
- human herpes virus type 6
- EBV hepatitis - this is an uncommon diagnosis and causes a self‐limiting hepatitis[6]
- hepatitis B
- tick-borne illnesses such as Lyme disease.
- Primary HIV may present with mucocutaneous ulcerations; furthermore, skin rash is frequently seen in primary HIV and is far less common in mononucleosis.[3]
Case Reports/ Case Studies[edit | edit source]
- Cosmopoulos K, Pegtel M, Hawkins J, Moffett H, Novina C, Middledorp J, Thorly-Lawson DA. Comprehensive profiling of Epstein-Barr virus microRNAs in nasopharyngeal carcinoma. J Virol. 2009 Mar;83(5):2357-67. Epub 2008 Dec 17.
- Candy B, Chalder T, Cleare AJ, Wessely S, White PD, Hotopf M. Recovery from infectious mononucleosis: a case for more than symptomatic therapy? A systematic review. Department of Psychological Medicine, Guy's, King's and St. Thomas' School of Medicine, London. Br J Gen Pract. 2002 October; 52(483): 844–851
- Candy B, Chalder T, Cleare AJ, Peakman A, Skowera A, Wessely S, Weinman J, Zuckerman M, Hotopf M. Predictors of fatigue following the onset of infectious mononucleosis. Department of Psychological Medicine, Public Health Laboratory and Medical Microbiology, Guy's, King's and St Thomas' School of Medicine and Institute of Psychiatry, London. Psychol Med. 2003 Jul;33(5):847-55.
- Katz BZ, Shiraishi Y, Mears CJ, Binns HJ, Taylor R. Chronic fatigue syndrome after infectious mononucleosis in adolescents. Department of Pediatrics, Division of Infectious Diseases, Northwestern University Feinberg School of Medicine and Children's Memorial Hospital, Chicago, Illinois 60614, USA. [email protected] Pediatrics. 2009 Jul;124(1):189-93.
- Buchwald DS, Rea TD, Katon WJ, Russo JE, Ashley RL. Acute infectious mononucleosis: characteristics of patients who report failure to recover. Department of Medicine, University of Washington, Seattle, Washington, USA. Am J Med. 2000 Nov;109(7):531-7.
Resources[edit | edit source]
References[edit | edit source]
- ↑ Merriam Webster infectious mononucleosis Available from: https://www.merriam-webster.com/dictionary/infectious%20mononucleosis ( last ccessed 5.8.2020)
- ↑ 2.0 2.1 2.2 2.3 2.4 Radiopedia Mononucleosis Available from:https://radiopaedia.org/articles/infectious-mononucleosis-1?lang=us (last accessed 3.8.2020)
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Mohseni M, Boniface MP, Graham C. Mononucleosis. April 27 2020 Available from:https://www.ncbi.nlm.nih.gov/books/NBK470387/ (last accessed 3.8.2020)
- ↑ Straus, S., The Chronic Mononucleosis Syndrome. The Journal of Infectious Diseases, Vol. 157, No. 3 (Mar., 1988) pp. 405-412. Oxford University Press. http://www.jstor.org/stable/30136640
- ↑ Goodman C, Fuller K. Pathology. Implications for the Physical Therapist. St. Louis, MO: Saunders Elseveir: 2009
- ↑ Vine LJ, Shepherd K, Hunter JG, Madden R, Thornton C, Ellis V, Bendall RP, Dalton HR. Characteristics of Epstein–Barr virus hepatitis among patients with jaundice or acute hepatitis. Alimentary pharmacology & therapeutics. 2012 Jul;36(1):16-21.