Myopathies
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson, Shreya Pavaskar, Vidya Acharya and Rucha Gadgil
Introduction[edit | edit source]
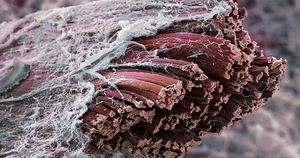
Myopathies are diseases of skeletal muscle which are not caused by nerve disorders. These diseases cause the skeletal or voluntary muscles to become weak or wasted. [Image: Muscle fibres surrounded by fascia]
There are many different types of myopathies, most common types include
- Genetic Myopathies
- Inflammatory Myopathies
- Endocrine Myopathies.
Myopathies are rare and not usually fatal. Typically, effects are mild, largely causing muscle weakness and movement problems, and many are transitory. Only rarely will patients become dependent on a wheelchair[1].
Cause
- Myopathies are usually degenerative, but they are sometimes caused by drug side effects, chemical poisoning, or a chronic disorder of the immune system[1].
Hereditary Myopathies[edit | edit source]
Hereditary myopathies are inherited disorders primarily affecting the skeletal muscle tissue. These are caused by mutations in different genes-encoding proteins that play important roles in muscle structure and function. Skeletal muscle weakness and hypotonia are typical clinical manifestations in most of hereditary myopathies. Histological features such as fibre type disproportion, myofibrillar disorganization, and structural abnormalities are usually observed in muscle biopsies of non-dystrophic myopathies, while fibrosis, fibre regeneration, wasting, and atrophy are characteristic of dystrophic myopathies.[2]Examples are given below:
- Mitochondrial Myopathies: eg Mitochondrial encephalopathy; lactic acidosis; and strokelike syndrome (MELAS)
- Congenital Myopathies: eg Core myopathies; Centronuclear myopathies
- Metabolic Myopathies: eg Lipid myopathies; Glycogen storage disease myopathy (caused by enzyme deficiencies)
- Channelopathies: eg Periodic paralysis (Hypokalemic, hyperkalemic)
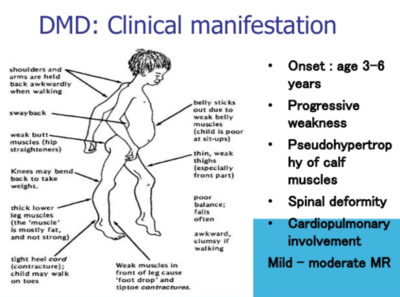
- Muscular Dystrophies: eg Duchenne muscular dystrophy; Becker muscular dystrophy, Symptoms are almost identical to Duchenne but condition is milder and progresses more slowly; survival into middle age; Limb-Girdle, Symptoms include weakness and wasting, affecting shoulder girdle and pelvic girdle first; progression is slow; death is usually due to cardiopulmonary complications. A study demonstrates the use of a holistic approach in the initial stage while reaching a diagnosis of Limb girdle muscular dystrophy is important. The biopsychosocial model, myotome testing, creatine kinase testing and MRI (results showed paraspinal atrophy) highlighted the Limb girdle muscular dystrophy diagnosis which was missed on normal physiotherapy assessment. The case report suggests the need of appropriate testing to rule out differential diagnose[3]; Myotonic Dystrophy, Symptoms include weakness of all muscle groups accompanied by delayed relaxation of muscles after contraction; affects face, feet, hands, and neck first; progression is slow, sometimes spanning 50 to 60 years; Spinal Muscular Atrophy (most common type of muscular atrophies).[4]
Inflammatory Myopathies[edit | edit source]
Some myopathies are inflammatory, leading to inflamed, weakened muscles. Inflammation is a protective response of injured tissues characterized by redness, increased heat, swelling, and/or pain in the affected area. Eg polymyositis, dermatomyositis, and myositis ossificans.[1]
Endocrine Myopathies[edit | edit source]
Endocrine disorders represent a large group of highly varied clinical disorders, many of which can be diagnosed largely based on the patient's history and physical examination with a little help from modern technology. The interactions between the force generating and metabolic functions of skeletal muscle serve as the source of muscle disorders associated with endocrine abnormalities. These myopathies are usually reversible with correction of the underlying disturbance.
Major categories of endocrine myopathy include those associated with: adrenal dysfunction (as steroid myopathy); thyroid dysfunction (as in myxedema coma or thyrotoxic myopathy); parathyroid dysfunction (as in multiple endocrine neoplasia); pituitary dysfunction; and islands of Langerhans dysfunction (as in diabetic myopathy from ischemic infarction of the femoral muscles).
Corticosteroid myopathy is the most common endocrine myopathy. Endocrine myopathies have been underreported in neurological practice (with only few studies on endocrine myopathy from India)[5].
Epidemiology[edit | edit source]
Most common type of myopathy:
- Inflammatory and endocrine myopathies (usually in middle-aged women> men).
- Prevalence varies between 2.4 to 33.8 per 100,000 population.
The most common inherited myopathies are the dystrophinopathies
- More common in male patients and affect every race and ethnicity equally.
- Duchenne's and Becker's muscular dystrophy are the most prevalent which varied between 19.8 and 25.1 per 100,000 person-years.
- Mitochondrial myopathies affect 1 in 4300 people.
- Other forms of inherited myopathies are rare[4]
Presentation[edit | edit source]
- Myopathies typically involve motor impairment without no sensory symptoms (primary symptom is muscle weakness from dysfunction of muscle fiber)
- Presents as proximal muscle weakness, mainly in the pelvic girdle or the shoulder girdle muscle groups.
- Pelvic muscle group is more common and more severe.
- Patients may complain of difficulty raising up from sitting position, climbing stairs or difficulty brushing their hair, or practicing any above head activities.
- Other symptoms of myopathy can include include muscle cramps, stiffness, and spasm.
- Some other myopathies will present in different muscle groups like thighs, back muscles, or fingers, and could be possibly associated with other symptoms like myalgia, rashes, fatigue, or cramps.
- Muscle disease could also present with dark urine as a sign of renal damage in the case of rhabdomyolysis, particularly after vigorous exercises like running marathons[4].
Diagnosis[edit | edit source]
Early diagnosis of myopathy is important so that the best possible care can be provided as soon as possible. Diagnosis is based on evaluating a person's medical history and performing a thorough physical exam. Diagnostic tests can help differentiate between the different types of myopathy, as well as between myopathy and other neuromuscular disorders. If a genetic myopathy is suspected, a thorough family history will also be taken.
Diagnostic tests the doctor may order include:
- Measurements of potassium in the blood
- Muscle biopsy
- Electromyogram (EMG)[1].
Treatment[edit | edit source]
Treatments for the myopathies depend on the disease or condition and specific causes. Supportive and symptomatic treatment may be the only treatment available or necessary for some disorders. Treatment for other disorders may include drug therapy, such as immunosuppressives, physical therapy, bracing to support weakened muscles, and surgery.
Physiotherapy[edit | edit source]
Physiotherapy can help control symptoms and help client maintain a good quality of life.
Treatment may include:
- Increasing muscle strength
- Improving balance
- Increasing flexibility
- Reducing risk of falls
- Preventing development of muscular and joint contractures
- Providing equipment for mobility eg walking aids, orthoses, callipers and wheelchairs
- Advising on moving and handling techniques and equipment
- Referral to other appropriate medical health professionals
- Anticipating and minimising other secondary complications of myopathies[6]
See also Physiotherapy under links to specific myopathies.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 The free dictionary Myopathies Available from:https://medical-dictionary.thefreedictionary.com/Myopathies (last accessed 21.11.2020)
- ↑ González-Jamett AM, Bevilacqua JA, Díaz AM. Hereditary Myopathies. Muscle Cell and Tissue-Current Status of Research Field. 2018 Apr 12.Available from:https://www.intechopen.com/books/muscle-cell-and-tissue-current-status-of-research-field/hereditary-myopathies (last accesssed 22.11.2020)
- ↑ Arch Physiother. 2019 Nov 14;9:13. doi: 10.1186/s40945-019-0066-3. eCollection 2019. Limb girdle muscular dystrophy: a case report initially presenting to an outpatient musculoskeletal physiotherapy clinic with spinal pain and functional weakness.
- ↑ 4.0 4.1 4.2 Nagy H, Veerapaneni KD. Myopathy. StatPearls [Internet]. 2020 Sep 1.Available from:https://www.ncbi.nlm.nih.gov/books/NBK562290/ (accessed 21.11.2020)
- ↑ Sharma V, Borah P, Basumatary LJ, Das M, Goswami M, Kayal AK. Myopathies of endocrine disorders: a prospective clinical and biochemical study. Annals of Indian Academy of Neurology. 2014 Jul;17(3):298.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4162016/ (last accessed 22.11.2020)
- ↑ Manchester Physio Myopathies Available from:https://www.manchesterneurophysio.co.uk/adults/conditions-we-treat/orthopaedic-msk-conditions/myopathy/physiotherapy-treatment-for-myopathies.php (last accessed 22.11.2020)