Infection Control in Older Adults
Introduction[edit | edit source]
Infectious diseases account for one third of all deaths in people 65 years and older.[1]
Active infection is a challenge not only for older adults with infectious diseases, but also for health care providers[2]. It is therefore essential for clinicians, such as physiotherapists who manage older adults in different settings, to identify challenges in the control of infection in older adults and measures to stop the spread of infection.
Elderly and infections, key points
- Early detection is more difficult in the elderly because the typical signs and symptoms, eg fever and leukocytosis, are frequently absent.
- A change in mental status or decline in function may be the only presenting problem in an older patient with an infection.
- An estimated 90 percent of deaths resulting from pneumonia occur in people 65 years and older.
- Pneumonia, flu and other infectious diseases (including COVID-19) have resulted in high mortality rates among older adults (mortality resulting from influenza also occurs primarily in the elderly).
- Urinary tract infections are the most common cause of bacteremia in older adults. Asymptomatic bacteriuria occurs frequently in the elderly; however, antibiotic treatment does not appear to be efficacious.
There are also challenges with specific vaccines or anti-viral therapy for some infectious conditions, including the class of coronaviruses that include SARS, MERS, and COVID-19.
- Antibiotics are useless against viral infections. This is because viruses are so simple that they use their host cells to perform their activities for them. So antiviral drugs work differently to antibiotics, by interfering with the viral enzymes instead.
- It is possible to vaccinate against many serious viral infections eg measles, mumps, hepatitis A and hepatitis B. Some viruses eg those that cause the common cold, are capable of mutating from one person to the next. Vaccination for these kinds of viruses is difficult, because the viruses have already changed their format by the time vaccines are developed.
Infection Control Challenges in Older Adults[edit | edit source]
This section will focus on issues related to infection control in older adults, taking into account physiological changes and health care settings.
Physiological Changes[edit | edit source]
With aging, physiologic changes occur that affect the immune system as well as various organ systems. Aging itself is not a disease however, with time, the accumulation of such changes can sometimes lead to a clinical condition in older adults known as frailty.
Age related immune changes
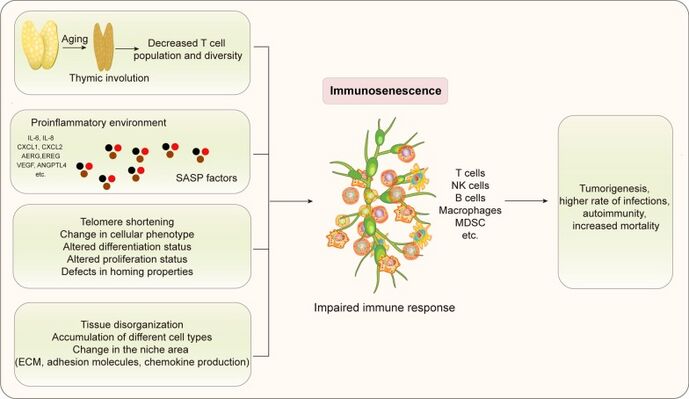
- Immunosenescence describes an age-related poor immune function that predisposes older adults to infectious diseases[3] and is attributed to a functional decline in the innate and adaptive immune system due to ageing.
- Innate immunity due in the older person is classically causes the upregulation of a number of pro-inflammatory cytokines, eg IL-6, C-reactive protein, and others[3]. Such a chronic pro-inflammatory state can lead to anorexia, nutritional impairment, muscle weakness, and weight loss, all of which can contribute to infections in older adults[4].
- Immunosenescence and inflammaging are gradual, relentless processes, with their clinical impact often not fully apparent until progression to frailty. Coupled with other factors such as multimorbidities and declining functional status, this frailty results in increased morbidity and mortality (including from infection).[1]
Age related organ-specific physiologic changes
- Aging causes physiologic changes that affect nearly every organ system, independently of existing co-morbidities and disease. This process is the result of lifelong accumulation of molecular and cellular damage caused by a number of mechanisms. These changes include structural transformations, altered anatomy, and decreased function in multiple physiologic systems, as well as loss of feedforward and feedback mechanisms between interacting systems, resulting in a constellation of physiologic changes causing progressive homeostatic dysregulation and contribute to vulnerability to infections[1].
Health Care Settings[edit | edit source]
Due to the unique needs of older adults, there are a variety of settings in which they may reside or seek care.
- Common places of residences include: family homes; senior apartments; older adult day care centers; long-term care facilities; acute care; rehabilitation centers; home care.
- Some of these selected settings be discussed with respect to infection control and challenges in older adults.
Acute Care Centres[edit | edit source]
Older adults often reside in acute care centres due to the presence of comorbidities.
Infection control challenges at this centre include
- Poor assessment of the infection status of older adults by physician prior to transfer to acute centres
- Poor record of comorbidity
- Drug resistance pathogens
- Atypical clinical findings of infection among this population. eg an older adult with pneumonia may be more likely to present with confusion and functional deterioration than shortness of breath or new cough, and that may result in delayed diagnosis, resulting in inappropriate intervention and ultimately a delay in effective interventions[5].
Nursing Homes[edit | edit source]
Residents of nursing homes are susceptible to infectious diseases due to the following factors: host factors, structural concerns and process factors[5][6].
Host factors that make older adults susceptible to infectious diseases include
- immunosensecence, multi-morbid conditions, impaired mental status, and incontinence.
- Some older adults may serve as hosts for antimicrobial-resistant pathogens.
Structural control (the ability of the facility to have sufficient resources to manage the infection in the nursing home).
- This involves preparing and implementing programs to monitor infections at nursing homes.
Process factors include a nursing home's ability to deliver effective health care delivery services.
- It includes having highly-educated personnel with knowledge of controlling infections among older adults.
- Process factors also include good diagnostic tools and effective infection monitors.
- In the case of affected older adults, unavailability of this equipment or problems in any of the above factors may result in delayed intervention or mismanagement of infection.
Home Healthcare and Rehabilitation Services[edit | edit source]
Home health services are becoming increasingly utilized for older adults, as they require a longer period of medical attention in the home setting.
- Atypical clinical presentation that may mask the presence of infection in this population present challenges to controlling infection in older adults.
- May further delay intervention in the affected individual as is deemed necessary.
- In rehabilitation services, older adults receiving treatment for hydrotherapy and functional rehabilitation should be considered for proper screening of infections because they may be asymptomatic[5].
Recommendations[edit | edit source]
- Control of infections in older adults is particularly challenging for clinicians and healthcare systems.
- Clinicians need to consider the multi-modal aspects of infection risk factors in older adults when conducting general assessments in order to prevent and reduce the spread of infection.
- During this pandemic of COVID-19, older people need to be familiar with the prevention of infection in order to prevent the contraction and spread of covid-19
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Mouton CP, Bazaldua OV, Pierce B, Espino DV. Common infections in older adults. American family physician. 2001 Jan 15;63(2):257.
- ↑ El Chakhtoura NG, Bonomo RA, Jump RL. Influence of aging and environment on presentation of infection in older adults. Infectious Disease Clinics. 2017 Dec 1;31(4):593-608.
- ↑ 3.0 3.1 Goronzy JJ, Weyand CM. Understanding immunosenescence to improve responses to vaccines. Nature immunology. 2013 May;14(5):428.
- ↑ Franceschi C, Campisi J. Chronic inflammation (inflammaging) and its potential contribution to age-associated diseases. Journals of Gerontology Series A: Biomedical Sciences and Medical Sciences. 2014 Jun 1;69(Suppl_1):S4-9.
- ↑ 5.0 5.1 5.2 Mody L. Infection control issues in older adults. Clinics in geriatric medicine. 2007 Aug 1;23(3):499-514.
- ↑ High KP, Juthani-Mehta M, Quagliarello VJ. Infectious diseases in the nursing home setting: challenges and opportunities for clinical investigation. Clinical infectious diseases. 2010 Oct 15;51(8):931-6.