SARS Severe Acute Respiratory Syndrome
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Rishika Babburu
Introduction[edit | edit source]
A new and rapidly progressive respiratory syndrome termed severe acute respiratory syndrome (SARS) was identified by the World Health Organization (WHO) in the Guangdong Province of China as a global threat in March of 2003.
SARS went on to spread globally over the following months to over 30 countries and became the 1st pandemic of the 21st century. Lessons learned from the SARS pandemic are currently used as a blueprint to fight the pandemic of COVID19.[1]
Severe acute respiratory syndrome (SARS)
- Following the discovery of SARS-CoV-2, the numeric digit 1 was suffixed to the name of the SARS-related coronavirus, creating SARS-CoV-1
- An airborne respiratory virus, spreads through small droplets of saliva in a similar way to the cold and influenza.
- Showed a clear capacity to spread along the routes of international air travel.
- Can also be spread indirectly via surfaces that have been touched by someone who is infected with the virus.
- Most patients identified with SARS were previously healthy adults aged 25–70 years[2].
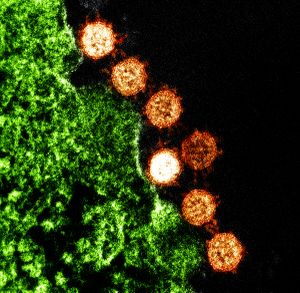
Image: Colorized transmission electron micrograph of Severe Acute Respiratory Syndrome (SARS) virus particles (orange) found near the periphery of an infected cell (green).
Etiology[edit | edit source]
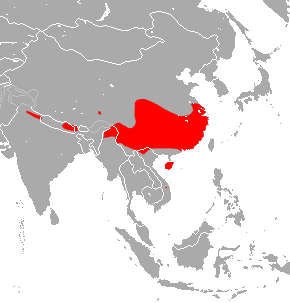
SARS-CoV is thought to have jumped from an animal reservoir in the horseshoe bat (see image) through an intermediate host in the palm civet and then to humans. All of these animals are sold in the live wild animal markets in China. The civet cats were thought to be the intermediaries who passed the SARS virus from bats to humans[3].
- Coronaviruses are named for their crown-like glycoprotein spikes on their surface.
- Coronaviruses are large single-stranded RNA viruses that have helical nucleocapsids.
- They are usually associated with humans with the common cold, though, and in animals, they’re linked with a highly virulent disease[1]
- The genome of SARS‐CoV has been sequenced and it is not related to any of the previously known human or animal coronaviruses. It is probable that SARS‐CoV was an animal virus that adapted to human‐human transmission in the recent past.[4]
Epidemiology[edit | edit source]
Early cases of SARS appeared to have originated in southern China (Guangdong province) as an unusual epidemic of severe pneumonia in November 2002. In 2003, an international outbreak developed involving 29 countries with 8098 cases of probable SARS and 774 (9.6%) deaths.
- The countries with the greatest number of reported cases included China, Hong Kong, Taiwan, Singapore, and Canada.
- In the US there were 27 cases (13 female and 14 male, with a median age of 36 years), 8 of which had laboratory evidence of SARS coronavirus (CoV) infection.
- There are no known cases of SARS transmission in any part of the world. The last known case in North America was identified on June 22, 2003, in Toronto, and globally on July 15, 2003, in Taiwan.
- Since then, 7 additional sporadic cases in humans have been reported: 2 laboratory-acquired in Singapore and Taiwan in 2003, and a cluster of 5 confirmed cases in China in April 2004[5].
- Image: Chinese Rufous Horseshoe Bat area
Pathologenisis[edit | edit source]
Seven coronaviruses have been found to be responsible for human diseases, two more are zoonoses, COVID-19 and Middle East respiratory syndrome coronavirus (MERS-CoV), both of which may sometimes be fatal. The remaining four viruses are ubiquitous in human societies worldwide and cause mild coryzal illnesses[3].
Understanding the pathogenesis of SARS is difficult as most available autopsy tissues are from patients dying later in the illness, at a time when the initial viral pathology is obscured by secondary infections or changes due to ventilator therapy, steroids and other immune modulators. Despite these limitations on autopsy material, it has been possible to determine that there are two phases of SARS pneumonia.
- Within the first 10 days the histological picture is that of acute phase diffuse alveolar damage (DAD) with a mixture of inflammatory infiltrate, oedema and hyaline membrane formation. Desquamation of pneumocytes is prominent and consistent.
- After 10 days of illness the picture changes to one of organizing DAD with increased fibrosis, squamous metaplasia and multinucleated giant cells.
- The role of cytokines in the pathogenesis of SARS is still unclear.[4]
- In 10–20% of cases, the respiratory illness is severe enough to require intubation and mechanical ventilation. Chest radiographs may be normal throughout the course of illness, though not for all patients. The white blood cell count is often decreased early in the disease, and many people have low platelet counts at the peak of the disease.[2]
Clinical Signs and Symptoms[edit | edit source]
Patients with SARS present with flu-like symptoms that will either show clinical improvement after the first week (30% of patients) or require intensive care treatment (20-30% of patients). A history of SARS-CoV-1 contact is often found. Initial symptoms include:
Complications include: acute respiratory distress syndrome (ARDS); acute cardiac injury; hypotension; tachycardia; acute renal failure; encephalitis.
Treatment/Prognosis[edit | edit source]
- No specific treatment exists for severe acute respiratory syndrome.
- Patients are given broad-spectrum antibiotics as well as antivirals, steroids, and supportive therapy.
- Vaccines for MERS-CoV and SARS-CoV-2 are under development[3]
Controlling future outbreaks rely on containment measures including:
- prompt detection of cases through good surveillance networks and including an early warning system;
- isolation of suspected of probably cases;
- tracing to identify both the source of the infection and contacts of those who are sick and may be at risk of contracting the virus;
- quarantine of suspected contacts for 10 days;
- exit screening for outgoing passengers from areas with recent local transmission by asking questions and temperature measurement; and
- disinfection of aircraft and cruise vessels having SARS cases on board using WHO guidelines.
Personal preventive measures to prevent spread of the virus include frequent hand hygeine and use of PPE[2].
Physiotherapy[edit | edit source]
See Role of the Physiotherapist in COVID-19 as many lessons learnt here apply to SARS COV 1
What is the public health response?[edit | edit source]
Doctors, hospitals and laboratories must report suspected cases of SARS to the local public health unit. The public health unit staff can help ensure appropriate diagnostic tests are done at a reference laboratory.
The suspected patient must be isolated and contacts identified, counselled, and isolated themselves from others if symptoms begin and seek urgent medical assessment.
A single confirmed case of SARS would constitute a public health emergency of international concern[2].
References[edit | edit source]
- ↑ 1.0 1.1 Hodgens A, Gupta V. Severe Acute Respiratory Syndrome. [Updated 2020 Oct 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-..Available from:https://www.ncbi.nlm.nih.gov/books/NBK558977/#article-28937.s2 (accessed 29.11.2020)
- ↑ 2.0 2.1 2.2 2.3 WHO SARS Available from:https://www.who.int/health-topics/severe-acute-respiratory-syndrome#tab=tab_1 (last accessed 30.11.2020)
- ↑ 3.0 3.1 3.2 3.3 Radiopedia SARS Available from:https://radiopaedia.org/articles/severe-acute-respiratory-syndrome-1?lang=us (last accessed 29.11.2020)
- ↑ 4.0 4.1 Nicholls J, DONG XP, Jiang G, Peiris M. SARS: clinical virology and pathogenesis. Respirology. 2003 Nov;8:S6-8.Available:https://onlinelibrary.wiley.com/doi/full/10.1046/j.1440-1843.2003.00517.x( accessed 29.11.2020)
- ↑ BMJ SARS Available from:https://bestpractice.bmj.com/topics/en-us/904/epidemiology (accessed 29.11.2020)