Fever
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Nupur Smit Shah
Introduction[edit | edit source]
Fever is the elevation of an individual's core body temperature above a 'set-point' that is normally regulated by the body's thermoregulatory center in the hypothalamus. This increase in the body's 'set point' temperature is often secondary to a pathological process that involves the release of immunological mediators (eg cytokines) to trigger the thermoregulatory center of the hypothalamus to elevate the body's core temperature.
The normal temperature of the human body is considered to be 37 degrees C and varies by about 0.5 degrees C through the course of the day. This minor variation of the core temperature is the result of many normal physiological processes of the human body, including sleep/wake cycles, metabolic changes, hormone variability, and activity levels. In fever, however, the increase in the core body temperature is often greater than 0.5 degrees C and attributed to a fever-inducing substance (pyrogen)[1].
Etiology[edit | edit source]
Many disorders can cause fever. They are broadly categorized as
- Infectious (most common)
- Neoplastic
- Inflammatory (including rheumatic, nonrheumatic, and drug-related)
The cause of an acute (ie, duration ≤ 4 days) fever in adults is highly likely to be infectious. When patients present with fever due to a noninfectious cause, the fever is almost always chronic or recurrent. Also, an isolated, acute febrile event in patients with a known inflammatory or neoplastic disorder is still most likely to be infectious. In healthy people, an acute febrile event is unlikely to be the initial manifestation of a chronic illness.[2]
Virtually all infectious illnesses can cause fever. But overall, the most likely causes are
- Upper and lower respiratory tract infections
- Gastrointestinal infections
- Urinary tract infections
- Skin infections
Most acute respiratory tract and gastrointestinal infections are viral.
Pathophysiology[edit | edit source]
Body temperature is determined by the balance between heat production by tissues, particularly the liver and muscles, and heat loss from the periphery. Normally, the hypothalamic thermoregulatory centre maintains the internal temperature between 37° and 38° C. Fever results when something raises the hypothalamic set point, triggering vasoconstriction and shunting of blood from the periphery to decrease heat loss; sometimes shivering, which increases heat production, is induced. These processes continue until the temperature of the blood bathing the hypothalamus reaches the new set point.
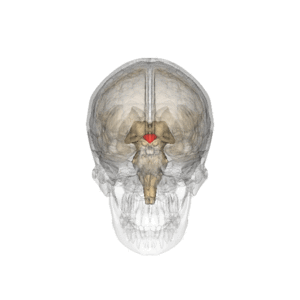
The hypothalamus (see gif R), which sits at the base of the brain, acts as the body's thermostat. It is triggered by pyrogens, which flow from sites where the immune system has identified potential trouble to the hypothalamus via the bloodstream. Some pyrogens are produced by body tissue (cytokines); many pathogens also produce pyrogens. When the hypothalamus detects them, it tells the body to generate and retain more heat, thus producing a fever. Children typically get higher and quicker fevers, reflecting the effects of the pyrogens upon an inexperienced immune system.[3]
- Pyrogens are substances that cause fever. Exogenous pyrogens are usually microbes or their products. Fever is the result of exogenous pyrogens produced by pathogen that induce release of endogenous pyrogens,eg interleukin-1 (IL-1), tumor necrosis factor-alpha (TNF-alpha), and IL-6 and other cytokines, which then trigger cytokine receptors, or exogenous pyrogens that directly trigger Toll-like receptors[2].
Complications[edit | edit source]
Although many patients worry that fever itself can cause harm, the modest transient core temperature elevations (ie, 38 to 40° C) caused by most acute infections are well tolerated by healthy adults[2].
Human beings live in a very narrow survival zone. Significant deviations from average in this tightly controlled physiological variable can quickly become life-threatening.[4] eg. Internal body temperatures in excess of 105 degrees F expose proteins and body fats to direct temperature stressors. This form of heat distress can threaten the integrity and function of proteins accustomed to the body's usual temperature variations and the occasional less excessive fevers. Cellular stress, infarctions, necrosis, seizures and delirium are among the potential consequences of prolonged, severe fevers. The receptor environment at the hypothalamus maintains limitations on high fevers. In the rare instances in which the hypothalamus itself malfunctions, the result is typically low body temperature, not elevated body temperature[3].
Post Operative Fever[edit | edit source]
Postoperative fever is a common occurrence of all surgery. Because there are so many causes of fever, the problem is usually managed by an interprofessional team of healthcare professionals. The nurse is probably the first person who monitors the patient and discovers the fever. In order to know the cause:
- First check the wound site, auscultate the lungs, and assess for deep vein thrombosis.
- Other causes of postoperative fever may be a urinary tract infection, an intravenous line (thrombophlebitis), or sepsis.
- Once the fever has been noted, the health care provider should be notified, and the workup depends on patient presentation and the day of the fever.
- If atelectasis is suspected, a chest x-ray may be ordered, blood and urine culture for sepsis, and a urinary tract infection and duplex ultrasound if a deep vein thrombus is suspected.
- The key is to examine the patient as it may provide a clue to the cause.[5]
Older Person Fever[edit | edit source]
In frail older adults, infection is less likely to cause fever, and if elevated by infection, temperature often it is lower than the standard definition of fever. Also inflammatory symptoms, such as focal pain, may be less prominent. Frequently, alteration of mental status or decline in daily functioning may be the only other initial manifestations of eg pneumonia or urinary tract infection.
- In spite of their less severe manifestations of illness, the febrile older adults are significantly more likely to have a serious bacterial illness than are febrile younger adults.
- As in younger adults, the cause is commonly a respiratory infection or urinary tract infection, but in older adults, skin and soft-tissue infections are among the top causes.
- Older adults with respiratory virus infections such as influenza and COVID-19 are also more likely to have serious manifestations.
- Focal findings are evaluated as for younger patients. But unlike younger patients, older patients probably require urinalysis, urine culture, and chest x-ray. Blood cultures should be done to exclude bacteremia; if bacteremia is suspected or vital signs are abnormal, patients should be admitted to the hospital[2].
Head Injury Fever[edit | edit source]
Fever management should take into consideration the protection of the brain from secondary insults as well as the capacity to fight against infections. Fever should most likely be treated aggressively in the first days of TBI, SAH, or stroke.
- Therapeutic hypothermia has yielded promising results in animal models of TBI, SAH, or stroke, but its usefulness in clinical practice is still debated. In severe TBI, therapeutic hypothermia permits control of intracranial pressure elevation, but its effects on outcome and mortality have not been conclusively demonstrated.
- The benefit of hypothermia in reducing infarct size in humans after ischemic stroke is not clear.[6]
Measuring Fever[edit | edit source]
A temperature reading will differ depending where on the body you measure it; some of the common sites include in the mouth, in the ear, under the armpit, on the forehead, or rectally.
- Oral or rectal measurement, taken closer to the sites of more energy use will produce more heat, resulting in higher temperature readings
- Measurements taken at sites close to the body’s surface eg ear or skin, are influenced by the surrounding environment and will tend to be lower (ie skin temperature might not be a foolproof screening tool for eg COVID-19). Someone who’s been in a cool environment may falsely screen negative for fever, while someone who’s been rushing outside in the sun may falsely screen positive[4].
Sleep and Fever[edit | edit source]
A fever is an attempt to create an environment that is not conducive to viral replication, while the increase in sleep allows the body to devote most of its energy on fighting the virus instead of focusing its energy on wakeful tasks. The hypothalamus induces a need for sleep during a fever.
During sleep, the flow of cerebrospinal fluid in the brain increases dramatically, washing away harmful waste proteins that build up between brain cells during waking hours[7], This process is even more crucial as the body fights an infection and is dealing with a surplus of proteins that need to be removed from the spaces between neurons. Essentially, all of this debris can act to obstruct or slow normal metabolic function and can attribute to the “foggy headed” feeling.
Sleep deprivation is a no-no when it comes fighting the flu. Sleeping lets the body focus its energy on fighting the virus, allowing the body to wash away the waste products lodged in between the brain cells.
Fever of Unknown Origin[edit | edit source]
Fever of unknown origin (FUO) was first described in 1961. The current definition proposed by Durack and Street in 1991 divided cases into four distinct subclasses: classic FUO, nosocomial FUO, neutropenic FUO, and HIV-related FUO[8]
Common causes of fever in the different subclasses are discussed below:
- Classic FUO: Endocarditis, complicated urinary tract infections, abscesses, and tuberculosis (TB) are consistently reported in patients with classic FUO. In patients over the age of 65, connective tissue diseases are determined to be the cause of fever more frequently. Fever in travelers is more likely to be secondary to infections such as malaria, typhoid fever, and acute HIV.
- Nosocomial FUO: Healthcare-associated fevers can be due to drug fever, complications post-operatively, venous thromboembolic disease, malignancy, transfusion-related reactions, or Clostridium difficile infection. Risk factors such as surgical procedures, instrumentation, intravascular devices, immobilization, and medications can help determine diagnostic testing necessary to obtain a diagnosis.
- Neutropenic FUO: Fevers are common in this subclass and are frequently due to infection.
- HIV-related FUO: Fevers can be present during acute illness, but are also common in the setting of untreated infection signifying additional infection with opportunistic organisms
In modern medicine, FUO remains one of the most challenging diagnoses as it can be caused by over 200 neoplastic, infectious, inflammatory, and miscellaneous disorders. Diagnosing FUO requires a thorough history, repeated physical examinations, and selective diagnostic testing.[8]
References[edit | edit source]
- ↑ Balli S, Sharan S. Physiology, Fever (Hyperthermia). StatPearls [Internet]. 2020 Sep 10.Available from: https://www.ncbi.nlm.nih.gov/books/NBK562334/(accessed 28.1.2021)
- ↑ 2.0 2.1 2.2 2.3 MSD manual Fever Available from:https://www.msdmanuals.com/professional/infectious-diseases/biology-of-infectious-disease/fever?query=Fever%20in%20Adults#v997196 (accessed 28.1.2021)
- ↑ 3.0 3.1 Scientific America Fever Available from:https://www.scientificamerican.com/article/what-causes-a-fever/ (accessed 29.1.2021)
- ↑ 4.0 4.1 The Conversation Normal body temp Available from: https://theconversation.com/normal-human-body-temperature-is-a-range-around-98-6-f-a-physiologist-explains-why-139270 (accessed 29.1.2021)
- ↑ Abdelmaseeh TA, Oliver TI. Postoperative Fever. StatPearls [Internet]. 2019 Jan 23 Available from:.https://www.statpearls.com/articlelibrary/viewarticle/27530/ (accessed 29.1.2021)
- ↑ Mrozek S, Vardon F, Geeraerts T. Brain temperature: physiology and pathophysiology after brain injury. Anesthesiology research and practice. 2012 Jan;2012.Available from: https://www.hindawi.com/journals/arp/2012/989487/(accessed 29.1.2021)
- ↑ Health shots Toxins and sleep Available from:https://www.npr.org/sections/health-shots/2013/10/18/236211811/brains-sweep-themselves-clean-of-toxins-during-sleep%20harmful (accessed 29.1.2021)
- ↑ 8.0 8.1 Brown I, Finnigan NA. Fever of Unknown Origin (FUO).2018 Available from:https://www.ncbi.nlm.nih.gov/books/NBK532265/?report=printable (last accessed 29.1.2021)