Iliopsoas Tendinopathy
Original Editor - Shejza Mino
Introduction and Background Information[edit | edit source]
The iliopsoas muscle is the strongest hip flexor and assists in external rotation of the femur, playing an important role in maintaining the strength and integrity of the hip joint[1]. It also acts as a stabilizer of the lumbar spine and pelvis[2]. Pathologic conditions of the iliopsoas have been shown to be a significant cause of hip pain and/or dysfunction and include asymptomatic snapping hip syndrome, tendonitis, bursitis and impingement[3]. Additionally, conditions related to the iliopsoas muscle have been implicated in lumbopelvic disorders, such as low back and gluteal pain, intense groin pain particularly in the athletic population, and even anterior thigh and knee pain[4].
Iliopsoas tendinopathy refers to a condition that affects the insertion of the muscle on the femur, and can occur with repetitive hip flexion and other deficits of the biomechanical system resulting in chronic degenerative changes of the tendon. Due to the close proximity of the Iliopsoas tendon and the related bursa, inflammation of one of these structures inevitably causes inflammation of the other. Therefore, iliopsoas tendinitis and iliopsoas bursitis are commonly described synonymously, as the clinical presentation, evaluation, and management are nearly identical[5].
Clinically Relevant Anatomy[edit | edit source]
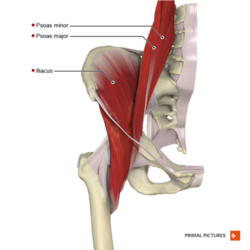
The iliopsoas muscle complex is made up of three muscles that include the iliacus, psoas major and psoas minor. There are many anatomical variations of the iliopsoas muscle, with the most common origin and insertion listed below[6][7].
Origin:
Psoas major: The transverse processes and lateral surfaces of the vertebral bodies of L1 - L4[6] or T12 - L5[7] and the path involves the intervertebral discs[6][7].
Psaos minor: It originates from T12 and L1 and lies anteriorly to the psoas major[6][7].
Iliacus: It originates on the upper two-thirds of the iliac fossa and the lateral parts of the wing of the sacrum.
Insertion:
Psoas major and iliacus: The psoas major and iliacus join together, pass under the inguinal ligament and insert onto the femoral lesser trochanter[6][7].
Psaos minor: It inserts onto the iliopectineal eminence after converging with the iliac fascia and the psoas major tendon[6][7].
Bursa: The iliopsoas or iliopectineal bursa lies between the bony surfaces of the pelvis and proximal femur and the musculotendinous unit. It is the largest bursa in humans. It has an average length of 5 to 6 cm and width of 3 cm and extends from the iliopectineal eminence to the lower portion of the femoral head[7]. The bursa has been reported to communicate with the hip joint in ~15% of patients[8].
Innervation:
Psaos major and minor: short collateral branches of L1 to L3[6]
Iliacus: femoral nerve or terminal nerve of L1 to L4[6]
Vascular supply: Common iliac artery and external iliac artery[6]
Function: Flexor of the thigh and trunk; Assists in external rotation of the femur; Lateral flexor of the lower vertebral column
Etiology[edit | edit source]
A tendinopathy is a structural change of the normal fibrillar tendon architecture and is proposed to be a result of the microtrauma that occurs from chronic overuse of the tendon[1]. Although the exact etiology is yet to be fully established, the two most commonly described causes of irritation to the iliopsoas tendon include either acute injury or overuse injury from repetitive microtrauma[5].
- Acute trauma is less common but may result in an injury to the musculotendinous unit or in an avulsion fracture of the lesser trochanter[3]. This typically results from eccentric contraction of the muscle or brisk flexion against an extension force that surpasses the capacity of the tendon[9].
- Overuse injuries involving the iliopsoas may result from any activity requiring repetitive hip flexion, repetitive external rotation or repetitive flexion of both the hip and trunk.
Activities that may predispose individuals to an iliopsoas injury include ballet, cycling, rowing, inclined running, track and field, soccer and gymnastics[5]. This injury is commonly referred to as "dancer's hip" or "jumper's hip", as the biomechanics of these movements (i.e.,repetitive hip flexion in an externally rotated position) may predispose an individual to injury[10]. In fact, one study found that more than 90% of ballet dancers report an audible click, pop or snap in the hip[11].
Adolescents during growth spurts have relatively decreased flexibility of the hip flexors, potentially putting them at greater risk[5].
Rheumatoid arthritis has been reported to be one of the main causes of Iliopsoas bursitis[12].
Epidemiology[edit | edit source]
In general, iliopsoas pathologic conditions, such as tendinopthy, bursitis, snapping and impingement, have been deemed to be the main cause of chronic groin pain in roughly 12-36% of athletes and in 25-30% of athletes with acute injury to the groin region[3].
- Most commonly presents in kicking athletes such as soccer players however, it may also occur in the nonathletic population[1].
- More commonly reported to effect young adults (peak age group is in the 30s)[1].
- Mildly more prevalent in females[5].
Clinical Presentation[edit | edit source]
The clinical presentation of an iliopsoas tendinopathy is variable, depending on various factors. An iliopsoas tendionopathy that is not symptomatic is often characterized by a palpable and audible snap that occurs from flexion and extension of the hip[11]. Persistent irritation of the tendon may lead to inflammation of the tendon, underlying bursa or both. Chronic irritation will likely not be associated with inflammation but is instead characterized by painful degeneration and fibrosis of the tendon[9].
History[edit | edit source]
A history of insidious deep groin or anterior hip pain is common[5]. Initially, pain is provoked with onset of activity, decreasing shortly after. Symptoms may progress to constant pain during activity that diminishes only with rest and lastly, to the presence of pain with both activity and rest[5]. Diagnosis is usually delayed and the average estimated time between initial symptoms and diagnosis is between 32-41 months[13].
- Intermittent groin pain, that typically described as a deep ache[1].
- Symptoms are worse with activity (especially kicking) and relieved with rest[1]. Other aggravating factors may include tying shoe laces, rising from a seated position after prolonged sitting and inclined walking[5].
- An audible clicking or catching sensation from the hip or groin area[1].
- Radicular symptoms along the anterior thigh down towards the knee may be reported[13].
- Dysfunction of the psoas muscle is commonly associated with various complaints to the lumbosacral region, which may include low back pain, discomfort into the gluteal or thigh region and the inability to stand fully erect[4].
Physical Examination[edit | edit source]
Observation:
- The patient may be holding the affected hip in a mildly flexed and externally rotated position (sign of psoas hypertonicity)[5].
- Postural observation may reveal an anteriorly tilted pelvis and increased lordosis of the lumbar spine[5].
- Gait: A shortened stride length may be obvious on the affected side. Additionally, increased knee flexion may be observed during heel strike and midstance phases[5].
Palpation:
- Increased tenderness with deep palpation of the iliopsoas muscultendionous junction within the femoral triangle. Palpation of the inguinal lymph nodes in this region should be unremarkable[13].
- Pain may be present at the insertion of the iliopsoas tendon onto the lesser trochanter, which can be palpated under the gluteal fold (with the patient in a prone position)[3].
Range of Motion:
- Passive hip extension may be limited and/or elicit pain (normal ~15 degrees)[13].
- Active or resisted hip flexion may reproduce pain.
Functional/Orthopedic testing:
- Thomas test or Modified Thomas test: can help identify excessive hypertonicity in the hip flexors[1].
- "Iliopsoas test": resisted hip flexion, with the hip in external rotation (performed with patient in a supine position). Any weakness and/or pain symptoms is a positive test[10].
- Ludloff's sign (isolated strength muscle assessment of the iliopsoas): in a seated position with the knees extended, the patient is asked to lift the heel of the affected side off the table. Any weakness and/or pain symptoms is considered a positive test[5].
- Stinchfield test: patient performs an active straight leg raise (SLR) to 45 degrees. Then, the patient resists a downwards force that is applied to the anterior thigh. Pain and/or weakness suggests involvement of the psoas muscle or intraarticular pathology[14].
- Snapping hip maneuver: the affected hip is positioned in a flexed, abducted and externally rotated position. The hip is passively moved into extension and internal rotation. A positive test is a palpable or audible snapping located in the inguinal region. Pain provoked with this maneuver may be suggestive of iliopsoas tendinitis or bursitis[5].
Other:
- Reciprocal inhibition of antagonist muscles and dysfunctions along the kinetic chain may be associated with psoas hypertonicity. Therefore, additional testing should include assessing for signs of hip abductor weakness, spinal instability, lower cross syndrome, increased foot pronation and dysfunctional breathing[15].
Differential Diagnoses[edit | edit source]
- Hip labral tear[1]
- Sports hernia[1]
- Iliopsoas bursitis[1]
- Inguinal hernia[1]
- Osteitis pubis[1]
- Abdominal muscle tendinopathy/strain[1]
- Adductor tendinopathy/Groin injury[1]
- Osteoarthritis[1]
- Obturator nerve entrapment[1]
- Neoplasm[1]
Other reported causes of anterior hip pain:
- Inflammatory synovitis[16]
- Infection (septic joint)[16]
- Crystal-induced synovitis ("gout")[16]
- Stress fracture of the femoral neck[16]
- Avascular necrosis of the femoral head[16]
- Tendon avulsion
- Muscle Contusion
- Femoral Acetabular Impingement (FAI)
- Rectus femoris strain[16]
- Tight iliotibial band[16]
- Referred from lumbar spine (L1, L2)[16]
- Myalgia paresthetica[16]
- Slipped Capital Femoral Epiphysis (SCFE)
- Snapping Hip Syndrome[16]
- "Internal" snapping hip, like previously mentioned, is related to the iliopsoas tendon.
- "External" snapping hip is related to either the iliotibial band or gluteus maximus tendon traveling over the greater trochanter[17].
- "Intra-articular" snapping hip can be due to loose bodies, labral tears or recurrent dislocation[18].
Workup[edit | edit source]
Laboratory Analysis[edit | edit source]
Laboratory studies, only indicated if the diagnosis is unclear, may include a CBC count, erythrocyte sedimentation rate or C-reactive protein, rheumatoid factor, anticyclic citrullinated peptide antibody, antinuclear antibody, and urinalysis. These tests are useful when considering pathology to the abdomen and pelvis that may present as groin pain such as colon cancer, diverticulitis, prostatitis, salpingitis, renal calculi, appendicitis and psoas abscess[5].
Medical Imaging[edit | edit source]
- Radiography
- Typically not indicated for soft-tissue disorders and findings are unremarkable in cases of iliotendonitis however, radiographs may be used as an initial imaging study if other bony pathology is suspected (i.e., loose bodies, osteitis pubis etc.) or in the presence of "red flags" [16].
- Slipped capital femoral epiphysis should be ruled out in a child or adolescent presenting with hip pain[19].
- Ultrasonography
- Diagnostic ultrasound (US) is a noninvasive and accessible option to evaluate muscle-tendon injuries. Findings typically reveal a thickened tendon.
- Iliopsoas bursitis is associated with an excessive amount of fluid in the iliopsoas bursa, which is usually visualized on US.
- US allows a dynamic view of the muscle, therefore will reveal any "snapping" of the tendon that may be present[16].
- US is used for needle guidance with lidocaine and corticosteroid injections (discussed below)[16].
- Not always an optimal test for diagnostic accuracy as this imaging choice is highly user-dependent[5].
- Magnetic Resonance Imaging (MRI)
- Currently, MRI is the "criterion standard" when evaluating symptoms relating to the hip and pelvis.
- In one study that looked at imaging to determine the cause of hip pain in endurance athletes, radiographs, radionuclide bone scans and MRI scans were compared. The results revealed MRI to be the most sensitive imaging modality[20].
- Provides the most accurate assessment of the iliopsoas tendon and bursa[16].
- Currently, MRI is the "criterion standard" when evaluating symptoms relating to the hip and pelvis.
- MRI findings when evaluating musculotendinous injuries:
- Spin-echo T2-weighted images will show increased signal intensity that is associated with swelling and inflammation. A musculotendinous injury of greater severity with associated haemorrhage will display high-signal intensity with both the T1-weighted images and T2-weighted images[5].
- Peritendinitis evaluation - the peritendinous tissue will display increased fluid that is detected on the spin-echo T2-weighted images or short T1 inversion recovery (STIR) sequence as a focus of high-signal intensity surrounding a normal tendon[5].
- Tendinosis - the spin-echo T1-weighted images will demonstrate increased signal intensity within the tendon that is associated with myxoid degeneration or angiofibroblastic proliferation. The spin-echo T2-weighted images may show an abnormal signal (usually less than that seen on the T1-weighted images) or a normal signal[5].
Lidocaine Injection[edit | edit source]
- A "lidocaine challenge test" involves either an interventional radiologist or an orthopedic surgeon administering a lidocaine injection to the iliopsoas tendon via the anterior aspect of the femoral triangle (under US guidance). If pain relief is achieved after the injection, a diagnosis of iliopsoas tendinopathy is confirmed[3].
Management[edit | edit source]
Conservative management[edit | edit source]
- Conservative management of psoas tendinopathy supports relative-rest, activity modification as well as exercise[3].
- Soft tissue techniques such as myofascial release may be useful to assist in decreasing muscle tightness and may be beneficial due to the proposed neuromodulatory effect.
- Manual therapy for mobilization of the hip capsule, lumbar spine, pelvis and other joint mobility deficits[1].
- Range of motion, stretching and strengthening exercises should target the hip flexors and antagonistic muscle groups.
Rehabilitation[edit | edit source]
Acute Phase[edit | edit source]
- The main objective of the first phase is to decrease pain symptoms, reduce muscle spasm and decrease any swelling. If the patient has stopped engaging in activities of daily living, getting the patient back to these activities is also an important goal of this first phase.
- Acute rehabilitation phase includes relative rest (avoiding any pain-provoking activities), ice, medication and light stretching.
- Ice: Apply for 20-minutes, every few hours for the first 1-3 days.
- Medication: Short-term course of non-steroidal anti-inflammatory drugs (NSAIDs).
- Gentle stretching will aid in reducing muscle spasm. To avoid over stretching, do not stretch soon-after a period of icing as icing may increase the individuals pain threshold, making them less sensitive to pain.
- The chosen iliopsoas stretch is held for 20-seconds, followed by 30-seconds of rest, and repeated five times. The stretch should remain pain-free at all times and the patient should bring their awareness to taking dull, deep breaths while holding the stretch[21].
Recovery Phase[edit | edit source]
- The primary goal of the second phase is to restore range of motion (ROM), strength, endurance and proprioception. Eventually, sport-specific activity is included.
- ROM:
- Stretching routine for the iliopsoas complex is continued and engaging in proper warm-up and cool-down with exercise is emphasized.
- Injury to the iliopsoas muscle may be associated with increased lumbar lordosis and anterior pelvic tilt. Achieving neutral postural can be worked on by both stretching and strengthening the appropriate muscle groups.
- Stretching:
- Stretching the rectus femoris helps to bring an anteriorly-rotated pelvis into a more neutral position. Doing so will take tension off of the iliopsoas muscle, decreasing the likelihood of strain or spasm.
- All stretches in this phase are held as described in the acute phase (hold for 20-seconds, relax for 30-seconds, repeat 5x[21].
- Strengthening:
- Increasing strength of the hamstring muscle group will increase the posterior force on the pelvis, decreasing the stress of the iliopsoas pulling on the pelvis anteriorly.
- Abdominal strengthening exercises should be performed with knees and hips flexed to 90 degrees will allow the iliopsoas to relax and the pelvis to remain in neutral.
- Gluteus maximus strengthening also plays a role in achieving a neutral position of the pelvis.
- Strengthening exercises are performed daily (4 sets of 10 to 15 repetitions)[21].
- Endurance training:
- Improved muscular endurance of the iliopsoas can be achieved overtime with repetitive movements (hip flexion or external rotation of the femur) performed at a low resistance. Some examples include cycling, walking, machine stair climbing.
- Endurance exercises should result in no pain, and there should be sufficient periods of rest between endurance training sessions. Eventually, the individual should work up to performing endurance sessions daily, gradually increasing the duration of activity[21].
- Stretching:
Maintenance Phase[edit | edit source]
- Continue stretching the iliopsoas and rectus femoris muscles.
- Gradually increase resistance used with strengthening exerices (i.e., seated iliopsoas strengthening with ankle weight, supine hip flexion (straight leg raise) with ankle weight, seated external rotation strengthening with ankle weight, seated external rotation with resistance band).
- Advancing strengthening exercises for the iliopsoas and the hamstrings - gradually progressing resistance can be achieved by either increasing the number of repetitions performed or increasing the weight, as tolerated by the individual.
- i.e., Standing hip flexion (machine), prone and seated hamstring curls (machine), advanced lunges with step-up (lunges are performed at a slower pace ensuring smooth and controlled rhythm)[21].
Return to Sport (RTS)[edit | edit source]
- The patient should be asymptomatic, or able to tolerate pain before considering RTS.
- Range of motion, flexibility and strength of the hip flexors and antagonist muscles should be restored to the level of the contralateral side.
- Sport-specific activities/drills should be relatively pain-free[21].
Surgical Intervention[edit | edit source]
- Surgical intervention is only considered when minimal improvement is achieved with a prolonged trial of nonoperative management, which includes:
- At least 3-months of a dedicated conservative care plan including rest, activity modification, physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs) and corticosteroid injections[3].
- There are two surgical techniques reported in the literature which include either a complete or partial release of the iliopsoas tendon. Generally, good outcomes have been reported with both procedures, including decreased pain and with no significant residual weakness[5].
Other[edit | edit source]
- Peritendinous corticosteroid injection
- The injection consists of a local anesthetic that is combined with a corticosteroid.
- One study evaluated patient-outcomes after injection into the iliopsoas bursa in a case suspecting tendinopathy to the iliopsoas muscle. The results demonstrated relevant improvement at 1-month post-injection. Additionally, the study reported that most patients experienced a notable decrease in pain 15-minutes after the injection was performed[5].
Prognosis[edit | edit source]
- With correction of underlying biomechanical deficits, the overall prognosis is good.
- Identifying these deficits early can play a role in preventing the development of chronic symptoms. However, as previously mentioned, diagnosis of a iliopsoas tendinopathy is made approximately two-years after the development of symptoms[1]. Recovery may be delayed in these cases.
- The patient should not return to play until they have achieved full and pain-free range of motion[1].
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 Micheo W. Musculoskeletal, Sports and Occupational Medicine. Demos Medical Publishing; 2010 Dec 21.
- ↑ Radiopedia Iliopsoas Available:https://radiopaedia.org/articles/iliopsoas-muscle (accessed 15.1.2022)
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Anderson CN. Iliopsoas: pathology, diagnosis, and treatment. Clinics in sports medicine 2016;35(3):419-33.
- ↑ 4.0 4.1 Kuchera W, Kuchera ML. Diagnosis and manipulative treatment: Thoracic region.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 5.17 5.18 5.19 Garry JP. Iliopsoas tendinitis [Internet]. Background, epidemiology, functional anatomy. Medscape; 2019 [cited 2020Sep24]. Available from: https://emedicine.medscape.com/article/90993-overview
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 Bordoni B, Varacallo M. Anatomy, bony pelvis and lower limb, Iliopsoas Muscle. StatPearls [Internet]. 2021 Jul 21. Available:https://www.ncbi.nlm.nih.gov/books/NBK531508/ (accessed 15.2.2022)
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 Anderson CN. Iliopsoas: pathology, diagnosis, and treatment. Clinics in sports medicine. 2016 Jul 1;35(3):419-33.
- ↑ Varma DG, Richli WR, Charnsangavej C, Samuels BI, Kim EE, Wallace S. MR appearance of the distended iliopsoas bursa. AJR. American journal of roentgenology. 1991 May;156(5):1025-8.
- ↑ 9.0 9.1 Bencardino JT, Palmer WE. Imaging of hip disorders in athletes. Radiologic clinics of North America. 2002 Mar;40(2):267-vii.
- ↑ 10.0 10.1 Laible C, Swanson D, Garofolo G, Rose DJ. Iliopsoas syndrome in dancers. Orthopaedic journal of sports medicine. 2013 Aug 21;1(3):2325967113500638.
- ↑ 11.0 11.1 Winston P, Awan R, Cassidy JD, Bleakney RK. Clinical examination and ultrasound of self-reported snapping hip syndrome in elite ballet dancers. The American journal of sports medicine. 2007 Jan;35(1):118-26.
- ↑ Generini S, Matucci-Cerinic M. Iliopsoas bursitis in rheumatoid arthritis. Clinical and experimental rheumatology. 1993;11(5):549-51.
- ↑ 13.0 13.1 13.2 13.3 Morelli V, Smith V. Groin injuries in athletes. American family physician. 2001 Oct 15;64(8):1405.
- ↑ Reider B, Martel J. Pelvis, hip and thigh. In: Reider B, Martel J, eds. The orthopedic physical examination. Philadelphia: Saunders; 1999:159–1199.
- ↑ Sutherland WG. Teachings in the Science of Osteopathy. Sutherland Cranial Teaching Foundation; 1990.
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 16.13 Johnston CA, Wiley JP, Lindsay DM, Wiseman DA. Iliopsoas bursitis and tendinitis. Sports Medicine. 1998 Apr 1;25(4):271-83.
- ↑ Binnie JF. V. Snapping hip (Hanche a Ressort; Schnellende Hufte). Annals of Surgery. 1913 Jul;58(1):59.
- ↑ Walker J, Rang M. Habitual hip dislocations in a child: another cause of the snapping hip. Clinical pediatrics. 1992;31(9):562-3.
- ↑ Wunderbaldinger P, Bremer C, Schellenberger E, Cejna M, Turetschek K, Kainberger F. Imaging features of iliopsoas bursitis. European radiology. 2002 Feb 1;12(2):409-15.
- ↑ Shin AY, Morin WD, Germany JD, Jones SB, Lapinsky AS. The superiority of magnetic resonance imaging in differentiating the cause of hip pain in endurance athletes. The American Journal of Sports Medicine. 1996 Mar;24(2):168-76.
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 Somogyi DM. Functional Rehabilitation of Sports and Musculoskeletal. Medicine and Science in Sports and Exercise. 1999 Feb 1;31(2):356-7.