Foundations for Ankle Foot Orthoses
Top Contributors - Carin Hunter, Jess Bell, Kim Jackson and Tarina van der Stockt
Introduction[edit | edit source]
An Ankle-Foot Orthosis is a specific type of assistive device that, as its name suggests, covers the foot and ankle. There are three main types of AFOs: flexible, rigid and jointed. Each device has specific advantages and disadvantages. The goal of the orthotist is to create an apparatus that ultimately enables the patient to achieve their highest functional level. Thus, the device should encourage maximal compliance of use and provide assistance for the patient to achieve their highest functional level - it should not hinder the patient.[1]
There are many different types of AFOs which will be discussed below. Each device has indications and contraindications, so an accurate assessment of the patient and their needs is vital. An AFO can be custom made or off-the-shelf, and both have their place in the rehabilitation journey.
Types of AFO[edit | edit source]
- AFO - Ankle-Foot Orthosis
- GRAFO - Ground Reaction Ankle-Foot Orthosis
- DAFO - Dynamic Ankle-Foot Orthosis
- SMO - Supramalleolar Orthosis
- Custom made
- Off-the-shelf
Orthotic Assessment [edit | edit source]
Passive Assessment:
- Range of motion (ROM)
- Muscle power
- Proprioception
- Sensation
- Leg length
Active Assessment:
- Level of mobility
- Gait pattern
- Compensation mechanisms of instability
- Risk of injury
- Pain
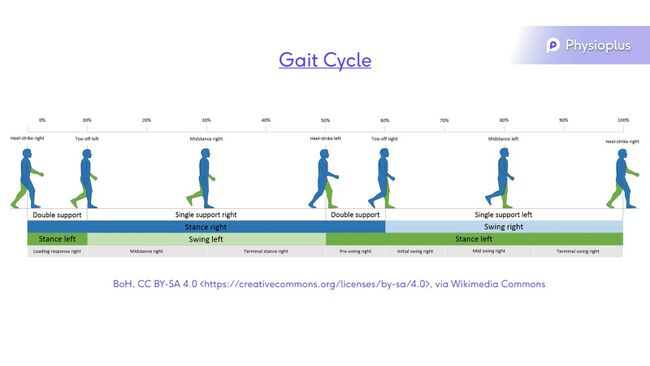
Gait Cycle[edit | edit source]
When the normal gait cycle is effected by a pathological condition, common complications emerge. These do vary from person to person, but often patterns can be found. The images below show a normal gait cycle and four pathological complications.
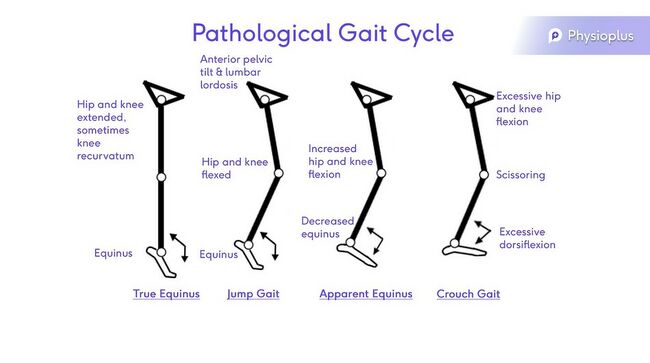
Pathological Gait Cycle:
There are various pathological gait conditions (see image below), including:[1]
- True equinus: the hip and knee are extended. Sometimes there is knee recurvatum, with an equinus foot (i.e. plantarflexed position).
- Jump gait: there is an anterior pelvic tilt and lumbar lordosis, the hip and knee are flexed with an equinus foot.
- Apparent equinus: there is increased hip and knee flexion, with decreased equinus.
- Crouch gait: there is excessive hip and knee flexion, scissoring at the knees and excessive dorsiflexion.
Changes in gait can be due to:
- Pain
- Joint ROM limitations
- Muscle weakness/ paralysis
- Neurological deficit
- Sensory deficit
- Leg length
Pathologies[edit | edit source]
- Paediatrics:
- Neural Tube Defect / Spina Bifida
- Cerebral Palsy
- Muscular Dystrophy
- Cerebral Vascular Accident (CVA)
- Sometimes individuals post-CVA may be fitted with an off-the-shelf device.
- Early intervention will produce the best outcomes and function.
- Late intervention often includes the accommodation of a fixed position. The goal is comfort and pain relief, and possibly to prevent worsening of the condition.
- Multiple Sclerosis
- This is a progressive condition. Initially an AFO can assist with slowing down the loss of function due to disease progression, but the use of splinting is reduced as the condition progresses further.
- Polio
- Early intervention will produce the best outcomes and function.
- Early intervention can prevent contractures caused by muscle weakness following the virus.
- AFOs can be used in conjunction with other devices as the weakness can be in muscles proximal to the ankle.
- Neuropathy
- Hereditary Motor Sensory Neuropathy (HMSN), also known as Charcot-Marie-Tooth Disease
- A hereditary, progressive disease that affects the nerves. It presents as weakness and numbness which is usually more pronounced in the legs than the arms. The condition begins peripherally and advances up the length of the nerve.
- Diabetes
- Orthotics can cause damage to tissue as patients commonly have sensory and neuropathic problems. It is crucial that there is minimal pressure from a hard orthotic device on the skin.
- Tumour
- AFOs can assist with complications due to nerve damage.
- Hereditary Motor Sensory Neuropathy (HMSN), also known as Charcot-Marie-Tooth Disease
- Trauma
- Nerve injury
- Nerve damage may be permanent, or temporary.
- An AFO could assist with gait and falls prevention.
- Pain
- Movement can often cause pain in certain pathological conditions or trauma. An AFO can be used to restrict movements causing pain and therefore reduce pain.
- Instability
- Nerve injury
Goal Setting / Prescription[edit | edit source]
- Positioning
- Should be in the position that causes the least amount of pain
- Aim for the most functional position
- When neutral is not possible, always aim for the optimal position
- Provide support
- Prevent contractures
- If a contracture is present already, aim to accommodate these contractures
- Improve mobility
- Increase stability
- Decrease pain
- Patient needs
Design/ Manufacture[edit | edit source]
- AFOs are broken down to two main categories: Custom made or off-the-shelf
- Custom made
- Manufactured using a plaster cast
- Off-the-shelf
- When sizing an off-the-shelf AFO, either measure for a foot plate or the calf
- Designed in small, medium, and large
- Generally need to be slightly adjusted, especially if there is an underlying condition
- Custom made
- Mostly manufactured from a plaster model
- Polypropylene/ lamination/ carbon fibre
- Use a Three-Point Force System
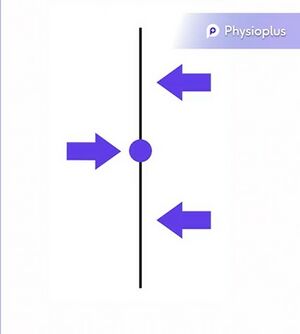
Three-Point Force System[edit | edit source]
This system is used to stabilise a joint or segment and it can reduce angular rotation. A force is often applied medio-laterally or antero-posteriorly.[2]
The Three-Point Force System (also known as the Three-Point Pressure System) is paramount to creating an orthosis.[3] In this system, a primary force is applied, generally at the joint to be corrected, and counterforces are applied both above and below the primary force. The sum of these three forces applied should be zero. The amount of force, and the position at which the primary force is applied, should be the point where movement needs to be increased or decreased. This will vary depending on the assessment and functional requirements of the patient, along with the established treatment goal.[4][5]
When applying a force, it is important to remember the scientific equation of: Pressure equals Force over Area.[6]
When creating an orthotic device, the longer the lever arm or the longer the orthosis is, and the further away the points of force are, the bigger the correction will be. As there is more surface area to spread the force over, the pressure can be reduced using this principle. This principle can be used to reduce discomfort when wearing an orthosis.
Foot / Ankle Position[edit | edit source]
When designing an AFO, the goal is to achieve the best foot and ankle position in conjunction with patient requirements. This means:
- The least painful position
- The best position possible
- The patient might not always be able to reach neutral, so the optimum available position is the most desirable outcome
- Highest functional level
Casting Procedure[edit | edit source]
When creating an AFO, a mould of the patient's foot and ankle is made using a plaster cast, a process requiring experience and skill. The cast is removed, creating a negative cast, which can be scanned or filled with plaster to create a positive model of the foot/ankle.. The custom device can be created using this new positive cast.
3D printing is occasionally used to create orthoses. However, a significant challenge associated with 3D printing is that it is difficult to maintain the optimum foot position long enough to take an accurate scan, which is needed to create an accurate device. Once this technology is improved, 3D printing might be an effective way of creating an AFO.[1]
Common Ankle-Foot Orthosis[edit | edit source]
- Flexible AFO
- Rigid/Solid AFO
- Jointed AFO
1. Flexible AFO[edit | edit source]
A flexible AFO has a certain amount of flexibility around the ankle area. This is achieved by cutting away part of the device around the ankle, reducing the surface area. This loss of surface area reduces the effect of the Three-Point Pressure System and as a result, this approach is not suitable for patients with mediolateral instability. A flexible AFO is useful in patients who have increased, uncontrolled movement in the ankle joint with good mediolateral stability. This type of device can allow for some roll over which encourages a natural gait pattern. It is easier to get out of chairs, and go up and down stairs. It is also easier for children to play on the floor and move around.
Prescription Criteria for a Flexible AFO[edit | edit source]
- Drop foot
- In order for the foot to clear the ground, a patient with drop foot will often flex excessively at their hip and knee, swing their leg into circumduction, or toe walk on the opposite side.[7] These compensatory movements lead to increased energy use, which tires the patient, and an increased falls risk.[8] A flexible AFO can correct the position to plantigrade but will allow some movement through midstance. This makes a more natural gait pattern but more importantly, also allows the foot to clear the ground.[9]
- Mobile foot/ankle
- No tendency to valgus or varus
Common Conditions Include[edit | edit source]
- CVA
- Nerve injury / dysfunction
- Paediatrics
Off-the-Shelf Flexible AFO[edit | edit source]
Also known as a posterior leaf spring (PLS) as they essentially have a spring at the back of the AFO.[10]
These AFOs are commonly used in the short-term while a custom splint is being designed or while the patient's condition improves. These are commonly used in hospital or trauma-type settings to maintain range.
2. Rigid AFO[edit | edit source]
A rigid AFO is an orthotic device, custom made for the individual, that allows no movement. They are often used in more severe situations and in conditions with some mediolateral instability. The rigid AFO allows the Three-Point Pressure System to function in the optimal way. It also influences the ground-reaction forces.
It is important to conduct a gait analysis when constructing these devices because we need to now what type of correction to apply.[11] If the AFO moves the ground-reaction force in front of the knee joint at mid-stance, it will create a hyperextension moment. Alternatively, if the ground-reaction force is moved or remains behind the knee joint, it will create a flexion moment at mid-stance.
A ground-reaction AFO (GRAFO) is essentially the same as a rigid AFO. The difference is that an anterior shell is attached, which will spread the load that is applied as part of the Three-Point Pressure System to the front of the shin. The force is applied at the front of the shin to extend the knee and to maintain the ankle in a plantigrade position.
Prescription Criteria for a Rigid AFO[edit | edit source]
- Slight tendency to flex at knee
- Muscle tightness
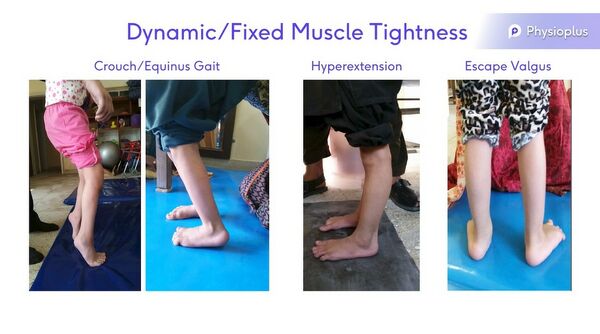
- Dynamic / fixed
- A tight muscle which is fixed requires accommodation as the ankle is not in a plantigrade position. The design of the AFO must, therefore, compensate for an equinus or plantarflexed position. This means that when the user of the AFO is standing, the ground-reaction force is in the correct position and the knee is not being pushed into hyperextension or flexion.[12]
- Crouch/ equinus gait
- Hyper-extension
- Escape valgus
- Dynamic / fixed
- Valgus deformities
- Often a compensatory movement
- Driven by tight tendon Achilles
- Can alter foot structure
- Can result in long-term issues
- Mediolateral instabilities - using a rigid AFO means that the Three-Point Pressure System can be applied
- Rocker bottom foot
- Needs to be supported to reduce pain and prevent deterioration
- Hyper-mobility
- Excessive dorsiflexion requires more stability. This is achieved by creating a more rigid base to stand on, and influencing the ground-reaction force which allows the knee and hips to extend
- Escape valgus
- Dynamic tightness can lead to an escape valgus, where the hindfoot moves into a valgus position because of the tightness in the tendon Achilles. This should be accommodated within a rigid AFO
- Rocker bottom foot
- Varus deformities
- Often difficult to control
- If a patient presents with a fixed deformity
- Accommodate the deformity
- If a patient presents with a flexible deformity
- Correct to the optimum position to allow the patient to function within the rigid AFO
- Crouch / excessive dorsiflexion
- Aim to produce an extension moment through the rigidity of the AFO, which can affect the flexion at the knee[12]
Common Conditions[edit | edit source]
- Cerebral palsy
- Neural tube defect
- Stroke
- Trauma
- Pain
3. Jointed AFO[edit | edit source]
A jointed AFO is made with a moving part, or joint, which hinges at the ankle joint. It is designed to allow motion at the ankle joint, but still offers the correction that the Three-Point Pressure System offers. The jointed AFO is a good tool to try to optimise a gait pattern.
Disadvantages:
- Tends to be bulkier, which can cause difficulty with footwear
- Can be noisy
- Parts can break
Advantages:
- Walking up and down stairs
- Getting up from a chair
- Moving around the floor, specifically for children
Prescription Criteria for a Jointed AFO[edit | edit source]
- ROM in ankle joint
- Tendency to valgus
- Tendency to varus
- Tendency to crouch
Prescription criteria for Jointed AFO and DAFO/SMO[edit | edit source]
- Hyper mobile foot/ankle
- Ankle to plantigrade
- Medio-lateral instability
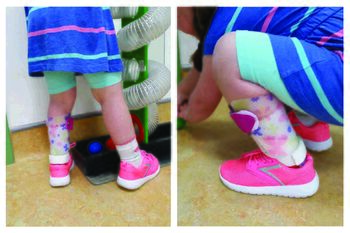
Tuning / Optimising AFOs [edit | edit source]
Once the AFO has been manufactured and fitted, optimisation can done in conjunction with footwear.[13] Walking in an AFO without footwear is dangerous and slippery. An AFO is always prescribed in conjunction with an appropriate type of footwear. This footwear will influence how the patient functions in the AFO and their gait pattern.[14] The orthotist needs to look at the footwear closely, and then optimise the angles of the AFO to influence the ground-reaction force.[15][16]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Fisher D. Introduction to Ankle-Foot Orthoses Course. Plus , 2022.
- ↑ Kadhim FM, Al-Din Tahir MS. Design and Analysis of Three-Point Pressure for Varus Foot Deformity. InJournal of Biomimetics, Biomaterials and Biomedical Engineering 2020 (Vol. 45, pp. 1-11). Trans Tech Publications Ltd.
- ↑ Condie DN, Meadows CB. Some biomechanical considerations in the design of ankle-foot orthoses. Orthot Prosthet. 1977 Jan 1;31(3):45-52.
- ↑ Lahr A. Design of a Modular Ankle-Foot Orthosis (Doctoral dissertation, The Ohio State University).
- ↑ Klenow T, Stevens P. Orthotic Management of the Mangled Extremity. InThe Mangled Extremity 2021 (pp. 243-255). Springer, Cham.
- ↑ Maxwell JC. On Faraday's lines of force. Good Press; 2021 Apr 11.
- ↑ Daryabor A, Arazpour M, Aminian G. Effect of different designs of ankle-foot orthoses on gait in patients with stroke: A systematic review. Gait & posture. 2018 May 1;62:268-79.
- ↑ Pongpipatpaiboon K, Mukaino M, Matsuda F, Ohtsuka K, Tanikawa H, Yamada J, Tsuchiyama K, Saitoh E. The impact of ankle–foot orthoses on toe clearance strategy in hemiparetic gait: a cross-sectional study. Journal of neuroengineering and rehabilitation. 2018 Dec;15(1):1-2.
- ↑ Choo YJ, Chang MC. Effectiveness of an ankle–foot orthosis on walking in patients with stroke: A systematic review and meta-analysis. Scientific reports. 2021 Aug 5;11(1):1-2.
- ↑ Saeedi H, Pourhoseingholi E. Comparison the effect of kinetic parameters of innovative storing-restoring hybrid passive (comfort gait) ankle-foot orthosis (AFO) with posterior leaf spring AFO in drop-foot patients: A prospective cohort study. Current Orthopaedic Practice. 2020 Sep 1;31(5):437-41.
- ↑ Totah D, Menon M, Jones-Hershinow C, Barton K, Gates DH. The impact of ankle-foot orthosis stiffness on gait: A systematic literature review. Gait & posture. 2019 Mar 1;69:101-11.
- ↑ 12.0 12.1 Butler PB, Farmer SE, Stewart C, Jones PW, Forward M. The effect of fixed ankle foot orthoses in children with cerebral palsy. Disability and Rehabilitation: Assistive Technology. 2007 Jan 1;2(1):51-8.
- ↑ Oudenhoven LM, Kerkum YL, Buizer AI, van der Krogt MM. How does a systematic tuning protocol for ankle foot orthosis–footwear combinations affect gait in children in cerebral palsy?. Disability and Rehabilitation. 2021 Sep 7:1-1.
- ↑ Stallard J, Woollam PJ. Transportable two-dimensional gait assessment: routine service experience for orthotic provision. Disability and rehabilitation. 2003 Jan 1;25(6):254-8.
- ↑ Jagadamma KC, Coutts FJ, Mercer TH, Herman J, Yirrel J, Forbes L, Van Der Linden ML. Effects of tuning of ankle foot orthoses-footwear combination using wedges on stance phase knee hyperextension in children with cerebral palsy–preliminary results. Disability and Rehabilitation: Assistive Technology. 2009 Jan 1;4(6):406-13.
- ↑ Owen E. The importance of being earnest about shank and thigh kinematics especially when using ankle-foot orthoses. Prosthetics and orthotics international. 2010 Sep;34(3):254-69.