Charcot-Marie-Tooth Disease
Introduction[edit | edit source]
Charcot-Marie-Tooth disease (CMT) is known as a hereditary motor and sensory neuropathy (HMSN) and is the most common inherited neuromuscular disease with a prevalence of approximately 1 in every 2,500 [1]. CMT involves the degeneration of nerve fibres in the body that results in muscle weakness and wasting along with a decrease in sensation [2][3]. CMT is a slowly progressive disorder and it encompasses a large group of clinically and genetically heterogeneous disorders.
Causes[edit | edit source]
CMT is caused by genetic mutations with approximately 1000 mutations in 80 genes that are related to the physical presentation of the disease. The diagnosis and classification of CMT is a very complicated process[2].The two main types are Type I which is known as demyelinating CMT (CMT1) and Type II which is known as axonal CMT (CMT2)[1]. CMT1A is the most common form of CMT and it is caused by a duplication of the 1.4 Mb region of chromosome 17 containing the peripheral myelin protein 22(PMP22) gene[1]. More information regarding the specifics about the different gene mutations can be found here [4].
Signs & Symptoms[edit | edit source]
The signs and symptoms of CMT are extremely variable between each different type due the extensive amount of different mutations possible. Symptoms most often begin in adolescence or early adulthood, but can also begin later in mid-adulthood[5]. It is a progressive disease so the symptoms change between earlier and later stages.
Some of these signs & symptoms may include[6][5]:
- Fatigue (most common to all those affected): This is a direct result of having to put in additional effort with daily activities
- Early Signs:
- Difficulty walking or an awkward walking pattern: A child may have trouble lifting their feet which may result in tripping
- Clumsiness at a young age
- Lack of agility
- Common symptoms
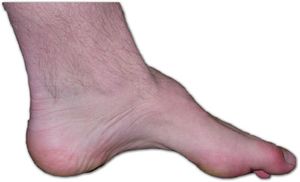
- Pes- Cavus, also known as highly arched feet: This can cause foot and ankle instability issues which may result in ankle sprains.
- Very flat feet
- Curled or hammertoes: This can be very uncomfortable for a child and may cause pain and difficulty finding an appropriate shoe.
- Lower legs are very thin, while the thigh muscles are a normal shape and bulk, or size:This characteristic is known as the inverted champagne bottle
- Some sensory loss and numbness in both the arms and legs :This is not usually a major problem for most individuals, but can result in unknown injuries if it is very severe
- Cold hands and feet due to poor circulation.
- Later symptoms
- Upper limbs including both the hands and forearms may be affected as the disease progresses
- Loss of fine motor control
- Loss of dexterity & overall hand strength
- Pain
- Tremors
CMT most often affects the distal limbs first, or those limbs further away from the body such as arms and legs. However, the lower limbs are usually affected before the upper limbs. The muscles in the lower part of the leg, ankle, and foot begin to atrophy as the disease progresses. This means the amount of muscle in these areas will decrease. Atrophy in the more proximal parts of the limbs or the parts closer to the body such as the thighs and upper arms is rare and usually only occurs in those more severely affected. As noted above, this muscle weakness along with a decrease in sensation can cause a lot of problems with both walking without any aid as well as problems with balance [7][8].
Medical Management[edit | edit source]
There is currently no cure or drug therapy for CMT. The main treatment options are rehabilitation therapy which will involve both a physiotherapist and an occupational therapist, and surgical treatment options[2].
Surgical Treatment[edit | edit source]
Surgical treatment is used for individuals with CMT with different skeletal deformities most often in their feet. Most individuals start out with flexible deformities in which the ankle begins to turn in, known as a cavovarus deformity. However, during the later stages of this disease, the deformity can become fixed. Treatment options are, therefore, soft tissue surgeries, osteotomies or removal of bone, and joint fusions. These can either be performed on their own or as a combination of a few. Research indicating who is appropriate for surgery and when this would be optimal is not yet conclusive as more in-depth long-term studies must be completed. For the upper limbs, tendon transfers may be beneficial to improve the ability to oppose the thumb and assist with wrist extension. In addition, scoliosis, also known as a curvature of the spine, is prevalent in about 15-20% of individuals with CMT and if severe enough, may need surgical intervention[2].
Physiotherapy Management[edit | edit source]
Physiotherapy is a key factor in a child’s management. It helps to improve the symptoms of CMT as well as decrease the risk of muscle contractures also known as the shortening of muscles. Physiotherapy will include low-impact exercises, posture and balance work, walking or swimming, and some strength training as well[9].
Physiotherapy along with occupational therapy should be started at the onset of symptoms. Starting physiotherapy early on can be beneficial because muscle weakness and sensory loss will be at a minimum[10].
The physiotherapist will also be involved in assessing the need for any additional aids or equipment. Many people with CMT may require high-top shoes or boots in order to provide more stability to the ankles and prevent injury. Others may need braces known as ankle-foot-orthoses (AFOs) which act similar to a cast, but they are removable. An AFO is a plastic brace, custom made for each individual to provide the necessary support and prevent tripping as a result of foot-drop. If individuals have more muscle weakness proximally or higher up the leg, then knee-ankle-foot orthoses are available.
The majority of individuals with CMT do not require to use of a wheelchair, however, in later stages of the disease some may choose to use one when going longer distances to reduce fatigue and the amount of stress on joints. The physiotherapist will work in conjunction with the occupational therapist and help with referrals to a podiatrist to ensure that all necessary equipment has been provided [7]. More information on different types of adaptive equipment can be found below.
Hydrotherapy[edit | edit source]
Hydrotherapy is a highly beneficial option as exercise for individuals with CMT. Essentially, it is just structured exercise lead by a physiotherapist that takes place in a pool. Hydrotherapy pools are not always easily accessible, but have many benefits especially for those individuals with CMT. Some of the benefits include reducing the amount of stress on joints due to the buoyancy of the water but still adds some light resistance to exercises in order to help maintain muscle strength[10]. More Information on hydrotherapy can be found below.
Aerobic Exercise[edit | edit source]
Exercise can also be carried out in a gym or at home. Walking, cycling, swimming and mild weight-training are all appropriate exercises that are safe to carry out with CMT. Overall, any type of general exercise will be beneficial for individuals with CMT. As long as that person is comfortable and working at low-moderate intensity, research shows that aerobic exercise can help to reduce fatigue, improve mood, and increase a person’s endurance. The goal is to help keep a child as independent as possible for as long as possible [10]. However, it is important to avoid overworking and exhaustion. When carrying out any type of exercise fatigue and weakness should not be caused within 30 minutes of exercises and neither should any form of excessive muscle soreness or cramping. These are things that are strongly discouraged when exercising with CMT[11].
Stretching[edit | edit source]
Stretching is also a key part of physiotherapy. As noted above, individuals with CMT are at risk for muscle contractures and stretching assists in maintaining muscle length. When this is done slowly and gently it can provide comfort for individuals and reduce stiffness in the joints[11]. Physiologically. in a disease process such as CMT, where the progression of the condition is due to axonal and demyelinating factors in the peripheral nervous system, application of Proprioceptive Neuromuscular Facilitation (PNF) techniques with elastic or manual resistance, with low impact on the skeletal and muscular system could demonstrate improvement in the capacity of the muscle, without producing fatigue.
Balance and Posture[edit | edit source]
Balance is an extremely important ability in order to carry out daily tasks. It involves gathering sensory input from the body and its surroundings in order to accurately orientate itself with gravity and the environment. With CMT, sensation may be altered which will affect a person’s ability to balance and ultimately completely normal activities of daily living[12]. Tai Chi, Yoga, and Pilates are all very useful exercises for improving both balance and posture.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 REILLY, M., MURPHY, S. and LAURA, M., 2011. Charcot-Marie-Tooth disease. Journal of the Peripheral Nervous System. vol. 16, pp. 1-14
- ↑ 2.0 2.1 2.2 2.3 PAREYSON, D. and MARCHESI, C., 2009. Diagnosis, natural history, and management of Charcot-Marie-Tooth disease. Lancet Neural. vol. 8, pp. 654-657.
- ↑ LAFARGE, C., TALSANIA, K., TOWNSHEND, J. and FOX, P. 2014. Living with Charcot-Marie-Tooth Disease: a qualitative analysis. British Journal of Neuroscience Nursing. October/November, vol. 10, no. 5, pp. 226-235.
- ↑ NHS CHOICES., 2014. Charcot-Marie-Tooth disease-Causes [online]. [viewed 9 November 2014]. Available from: http://www.nhs.uk/Conditions/Charcot-Marie-Tooth-disease/Pages/Causes.aspx
- ↑ 5.0 5.1 PHYSIO.CO.UK., Charcot Marie Tooth [online]. [viewed 10 November 2014]. Available from: http://www.physio.co.uk/what-we-treat/neurological/conditions/charcot-marie-tooth.html
- ↑ CMT UNITED KINGDOM., 2013. Symptoms/Problems [online]. [viewed 10 November 2014]. Available from: http://www.cmt.org.uk/symptoms_problems.php
- ↑ 7.0 7.1 MUSCULAR DYSTROPHY ASSOCIATION., 2009. Facts About Charcot-Marie-Tooth Disease & Related Diseases. [online]. [viewed 8 November 2014]. Available from: http://mda.org/sites/default/files/publications/Facts_CMT_P-180_0.pdf
- ↑ THOMAS, F.P., GUERGUELTCHEVA, V., GONDIM, F. and JORDANOVA, A., 2014.Charcot-Marie-Tooth Diseases. In: B. Katirji ed. Neuromuscular Disorders in Clinical Practice.New York: Springer Science + Business, pp. 519-547.
- ↑ NHS CHOICES., 2014. Charcot-Marie-Tooth disease- Treatment [online]. [viewed 9 November 2014]. Available from: http://www.nhs.uk/Conditions/Charcot-Marie-Tooth-disease/Pages/Treatment.aspx
- ↑ 10.0 10.1 10.2 CMT UNITED KINGDOM., 2013. Exercise/Physiotherapy [online]. [viewed 10 November 2014]. Available from: http://www.cmt.org.uk/exercise-physiotherapy.php
- ↑ 11.0 11.1 GRANDIS, M. and SHY, M. 2005. Current Therapy for Charcot-Marie-Tooth Disease. Current Treatment Options in Neurology. vol. 7, no. 1, pp. 23-31.
- ↑ NARDONE, A., GODI, M., ARTUSO, A. and SCHIEPATTI, M. 2010. Balance Rehabilitation by Moving Platform and Exercises in Patients with Neuropathy or Vestibular Deficit. Archives of Physical Medicine and Rehabilitation. vol. 91, pp. 1869-1877.