Cerebral Palsy Introduction
Original Editor - Kim Jackson as part of Enablement Project
Top Contributors - Michelle Lee, Naomi O'Reilly, Admin, Laura Ritchie, Kim Jackson, Simisola Ajeyalemi, Vidya Acharya, Mande Jooste, Rucha Gadgil, 127.0.0.1, Lucinda hampton, Jess Bell, Rachael Lowe, Olajumoke Ogunleye, Evan Thomas, Scott Buxton, George Prudden, Pranay Jindal and WikiSysop
Definition[edit | edit source]
Cerebral Palsy (CP) is a disorder of movement and posture that appears during infancy or early childhood resulting from damage to the brain. The damage to the brain is permanent and cannot be cured but the earlier we start with intervention the more improvement can be made.Any non-progressive central nervous system (CNS) injury occurring during the first 2 (some say 5) years of life is considered to be CP. There are several definitions of CP within the literature, although these may all vary slightly in the way they are worded they are all similar and can be summarised to:
Cerebral Palsy is a group of permanent, but not unchanging, disorders of movement and/or posture and of motor function, which are due to a non-progressive interference, lesion, or abnormality of the developing/immature brain[1].
This definition specifically excludes progressive disorders of motor function, defined as loss of previously acquired skills in the first 5 years of life.
Time Frame of Brain Injury[edit | edit source]
A diagnosis of CP is given if the brain damage arises during one of the following periods:
- Prenatal Period - Conception to the onset of labour
- Perinatal Period - 28 weeks intrauterine to 7 days
- Postnatal Period -First two (and some say five) years of life
After the age of 5 we speak of stroke or traumatic brain injury.
Epidemiology and Aetiology[edit | edit source]
Unfortunately, it is difficult to access and clarify the prevalence and incidence rate of disabilities in poor-resource settings (Gladstone, 2010). Not only the prevalence of childhood disability is on the rise and CP is one of the costliest chronic conditions, but also life expectancies are improving, which increases the burden of CP (Papavasiliou, 2009). For comparison, in the USA, there are approximately 700'000 children with CP, 2-5/ 1000 born.
Cerebral palsy is the most common motor disability in childhood. The aetiology of CP is very diverse and multifactorial. The causes are congenital, genetic, inflammatory, infectious, anoxic, traumatic and metabolic. The injury to the developing brain may be prenatal, natal or postnatal. As much as 75%-80% of the cases are due to prenatal injury with less than 10% being due to significant birth trauma or asphyxia. The most important risk factor seems to be prematurity and low birth weight with risk of CP increasing with decreasing gestational age and birth weight.
Population-based studies from around the world report prevalence estimates of CP ranging from 1.5 to more than 4 per 1,000 live births or children of a defined age range. Recent advances in neonatal management and obstetric care have not shown a decline in the incidence of CP. With a decline in infant mortality rate, there has actually been an increase in the incidence and severity of CP. The incidence in premature babies is much higher than in term babies. Cerebral palsy is more common among boys than among girls and more common among black children than among white children.
Most of the children identified with CP have Spastic cerebral palsy (77, 4%). Over half of the children identified with CP (58, 2%) can walk independently, 11, 3% walks using a handheld mobility device and 30, 6% has limited or no walking ability. Many children with CP also do have at least one co-occurring condition (e.g. 41% Epilepsy).
The incidence of CP has not declined despite the improved perinatal and obstetric care. Even at centres where optimal conditions exist for perinatal care and birth asphyxia is relatively uncommon, the incidence of CP in term babies has remained the same.
The overall prevalence worldwide has increased during the last decades because of increased survival rates. Here are some facts on the epidemiology of CP:
- The incidence is 2-2,5/1000 live births in Western Countries
- The prevalence varies between 1-5/1000 babies in different countries.
- There are no reliable statistics from Asian countries.
- Some affected children do not survive
- Aetiology
Improved medical care has decreased the incidence of CP among some children. Medical advances have also resulted in the survival of children who previously would have died at a young age.
The type of cerebral palsy has also changed:
- In the 60’s Athetoid / Dyskinetic CP accounted for approximately 20% of children with CP.
- Today only 5 to 10% have this type, with spastic cerebral palsy now accounting for 80-90% of children with CP.
- This decrease is mainly due to advances in the treatment of hyperbilirubinemia (Bilirubin is toxic to cells of the brain. If a baby has severe jaundice, there's a risk of bilirubin passing into the brain ie. acute bilirubin encephalopathy. Prompt treatment may prevent significant lasting damage)[2].
- The increase of spastic cerebral palsy is predominantly a result of higher survival rates for (very small premature) babies.
- The most common cause of CP is idiopathic which means that the cause of damage to the brain during pregnancy is not known.
Risk Factors[edit | edit source]
There are different risk factors for each stage at which a child might develop CP. These can be broken down into Prenatal, Perinatal and Postnatal.
Prenatal[edit | edit source]
- Prematurity (Gestational age less than 36 weeks)
- Low Birth Weight (less than 2500 g), which could be due to poor nutritional status of the mother
- Maternal epilepsy
- Hyperthyroidism
Infections (TORCH = Toxoplasmosis, Other (Syphilis, Varicella-Zoster, Parvovirus B19,) Rubella, Cytomegalovirus (CMV), Herpes Simplex Virus)
- Severe Toxemia, Eclampsia
- Drug Abuse
- Trauma
- Multiple Pregnancies
- Placental Insufficiency
Perinatal[edit | edit source]
- Premature Rupture of Membranes
- Prolonged and Difficult Labour
- Vaginal Bleeding at the time of admission for labour
- Bradycardia
Postnatal (0-2 years)[edit | edit source]
- Central Nervous System infection (encephalitis,meningitis)
- Hypoxia
- Seizures
- Coagulopathies
- Neonatal Hyperbilirubinemia
- Head Trauma
There is no way to predict which child’s brain will be damaged by one of these factors or to what the extent of the damage will be. None of these factors always results in brain damage and even when brain damage occurs, the damage does not always result in CP.
For example: Some children may have an isolated hearing loss from their meningitis, others will have severe intellectual disability and some will have CP.
Classification of Cerebral Palsy[edit | edit source]
The practice of classifying conditions, such as cerebral palsy, is important because it allows cases with similar characteristics, to be grouped together. It is important to classifiy the different features of CP, as this helps to set realistic expectations and influences the treatment[3]. Cerebral palsy is often classified based on several factors, including severity, topographical distribution (which body parts are affected), muscle tone, and functional ability[4].
- Severity can be classified as mild, moderate, or severe. This classification is broad and lacks specific criteria, but it provides a simple way of communicating the scope of impairment.
- Topographical distribution refers to which parts of the body are affected. It is a useful classification when combined with motor function classification, as it provides a description of how and where a person is affected by cerebral palsy, which can guide treatment protocols.
- Muscle tone refers to the effects of cerebral palsy on muscle tone and how muscles work together. Two terms used to describe muscle tone are hypertonia (increased muscle tone, often resulting in very stiff limbs, associated with spastic cerebral palsy) and hypotonia (decreased muscle tone, often resulting in loose, floppy limbs, associated with non-spastic cerebral palsy).
A more recent development in the classification of cerebral palsy is the functional classification system, which focuses on the functional abilities of children in the domains of cognition, self-care, mobility, and social aspects. There are several classification systems within this, including the Gross Motor Function Classification System (GMFCS), the Manual Ability Classification System (MAC), and the Communication Function Classification System (CFCS)[5][6]. These systems can be used by professionals and parents alike to observe different developmental areas and develop goals and interventions.
The GMFCS, in particular, is a widely used tool that assesses self-initiated movements in sitting, walking, and wheeled mobility. This system classifies children into five ordinal levels across five age bands, with an emphasis on the child's typical performance in different settings. The age bands considered in this system are less than 2 years of age, 2 to 4 years, 4 to 6 years, 6 to 12 years, and 12 to 18 years. The levels of distinction focus on functional abilities and the use and type of aids to achieve mobility[7].
There are also other more recent tools for classifying cerebral palsy, such as the Swedish Classification (SC) and the Surveillance of Cerebral Palsy in Europe (SCPE), both of which require the clinician to identify the predominant motor disorder. Although the SC and SCPE tools can assist in describing a child’s presentation, they do not provide any criteria for recording the functional abilities of the child. Identifying, describing, and classifying a child’s functional abilities can also enhance the reliability of diagnosing children with cerebral palsy.[8]
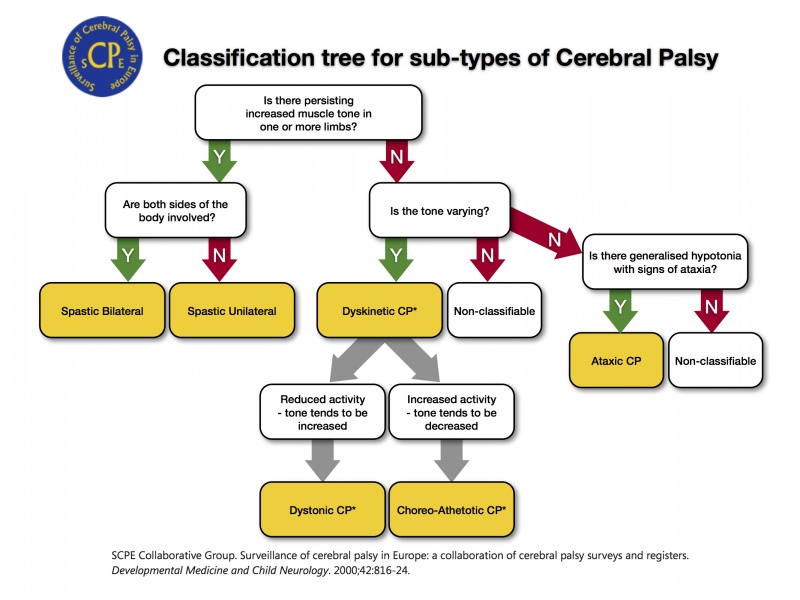
The Swedish Classification (SC) of Cerebral Palsy adopts a topographical descriptive approach. It describes the type of muscle tone (spastic, dyskinetic, ataxic, or mixed) and the number and distribution of the affected limbs (monoplegia, hemiplegia, diplegia, tetraplegia, and quadriplegia). The Surveillance of Cerebral Palsy in Europe (SCPE) further developed this concept and proposed a new classification of cerebral palsy subtypes in 2000. The SCPE classification system offers a decision flow chart to assist in classification into neurological and topographical categories, with well-defined symptoms and requirements provided for each neurological category. Unlike the SC, the SCPE system divides spastic cerebral palsy into either upper or lower limb divisions, with either bilateral or unilateral involvement.
However, there is still some uncertainty of the validity and reliability of these classifications. According to Rosenbaum et al., children with cerebral palsy should continue to be classified by the predominant type of tone or movement abnormality, such as spasticity, dystonia, choreoathetosis, or ataxia[9]. They also recommend any other tone or movement abnormalities observed be classified as secondary based on their anatomical distribution of features.
Sub-types of Cerebral Palsy[edit | edit source]
Many children with CP have a mixed form of cerebral palsy. Here the definition and classification used as agreed in Europe. More information on definitions, outcome of some studies, exchange of information on clinical practice on CP in Europe you can find, after registering here. The Surveillance of Cerebral Palsy in Europe was established in 1998.
Anatomical Classifications[edit | edit source]
Anatomical classification are as follows:
- Unilateral: One side of the body is affected
- Bilateral: Both sides of the body are affected
Spastic cerebral palsy: are used to distinguish between quadriplegia, diplegia and hemiplegia. Spastic cerebral palsy is either bilateral or unilateral.
Dyskinetic cerebral palsy and ataxic cerebral palsy: always involve the whole body (bilateral).
Spasticity [edit | edit source]
Spasticity is defined as an increase in the physiological resistance of muscle to passive motion. It is part of the upper motor neuron syndrome characterized by hyperreflexia, clonus, extensor plantar responses and primitive reflexes. Spastic cerebral palsy is the most common form of CP. Approximately 80% to 90% of children with CP have spastic cerebral palsy.
Spastic cerebral palsy is characterized by at least two of the following symptoms, which may be unilateral (hemiplegia) or bilateral:
- An abnormal pattern of posture and/or movement
- Increased tone (not necessarily constantly)
- Pathological reflexes (hyperreflexia or pyramidal signs e.g. Babinski response)
Traditionally we recognized three types of spastic CP:
- Hemiplegia
- Diplegia
- Quadriplegia.
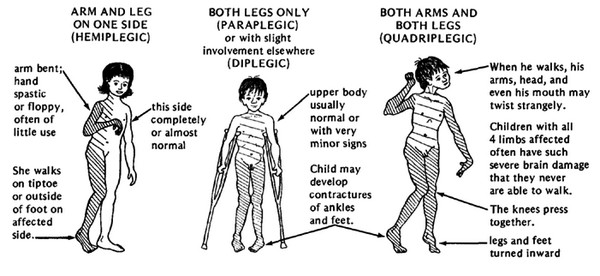
Hemiplegia (Unilateral)[edit | edit source]
With hemiplegia, one side of the body is involved with the upper extremity generally more affected than the lower. Seizure disorders, visual field deficits, tactile agnosia, and proprioceptive loss are likely. Twenty percent of children with spastic cerebral palsy have hemiplegia. A focal traumatic, vascular, or infectious lesion is the cause in many cases. A unilateral brain infarct with posthemorrhagic porencephaly (cysts or cavities within the cerebral hemisphere) can be seen on Magnetic Resonance Imaging (MRI).
Diplegia (Bilateral)[edit | edit source]
With diplegia, the lower extremities are severely involved and the arms are mildly involved. Intelligence usually is normal, and epilepsy is less common. Fifty per cent of children with spastic cerebral palsy have diplegia. A history of prematurity is usual. Diplegia is becoming more common as more low- birth-weight babies survive. MRI reveals mild Periventricular Leukomalacia (PVL).
Quadriplegia (Bilateral)[edit | edit source]
With quadriplegia, all four limbs, the trunk and muscles that control the mouth, tongue and pharynx are involved. Thirty percent of children with spastic cerebral palsy have quadriplegia. More serious involvement of lower extremities is common in premature babies. Some have perinatal hypoxic ischemic encephalopathy. MRI reveals Periventricular Leukomalacia (PVL).
Dyskinetic CP[edit | edit source]
Abnormal movements that occur when the child initiates movement are named Dyskinesias. Dysarthria, Dysphagia and drooling accompany the movement problem. Intellectual development is generally normal, however severe dysarthria makes communication difficult and leads the outsider to think that the child has intellectual impairment. Sensorineural hearing dysfunction also impairs communication. Dyskinetic cerebral palsy accounts for approximately 10% to 15 % of all cases of CP. Hyperbilirubinemia or severe anoxia causes basal ganglia dysfunction and results in Dyskinetic cerebral palsy.
Dyskinetic cerebral palsy is characterised by the following Symptoms:
- Abnormal pattern of posture and/or movement, and
- Involuntary, uncontrolled, recurring, occasionally stereotyped movements of affected body parts
Dyskinetic cerebral palsy may be either:
- Dystonic cerebral palsy, dominated by both hypokinesia and hypertonia, or
- Choreoathetotic cerebral palsy, dominated by both hyperkinesia and hypotonia
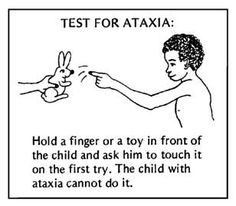
Ataxic CP[edit | edit source]
Ataxia is loss of balance, coordination and fine motor control. Ataxic children cannot coordinate their movements. They are hypotonic during the first 2 years of life. Muscle tone becomes normal and ataxia becomes apparent toward the age of 2 to 3 years. Children who can walk have a wide-based gait and a mild intention tremor (Dysmetria). Dexterity and fine motor control is poor. Ataxia is associated with cerebellar lesions. Ataxia is often combined with spastic diplegia. Most ataxic children can walk but some need walkers.
Ataxic Cerebral Palsy is characterized by the following symptoms:
- Abnormal pattern of posture and/or movement
- Lost of orderly muscular coordination, so that movements are performed with abnormal force, rhythm, and accuracy
 |
|
Mixed CP[edit | edit source]
Children with a mixed type of Cerebral Palsy commonly have mild spasticity, dystonia and/or athetoid movements. Ataxia may be a component of the motor dysfunction in children in this group. Ataxia and spasticity often occur together. Spastic Ataxic Diplegia is a common mixed type that often is associated with hydrocephalus.
| [10] | [11] |
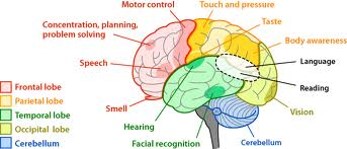
The Brain[edit | edit source]
Here is some of the clinical terminology used when talking about Cerebral Palsy:
- Tonus
- Lesion Site
- Spastic
- Cortex
- Dyskinetic
- Basal Ganglia - Extrapyramidal System
- Hypotonic / Ataxic
- Cerebellum
- Mixed
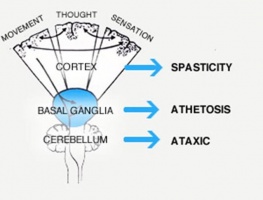
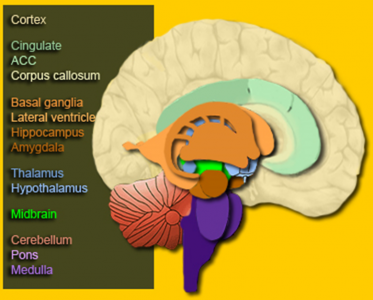
- Diffuse
Knowing where the damage could be located will not influence your interventions. Look at the following pictures of the brain to understand the relationship between the location of the damage and the symptoms.
Problems Regularly Seen with Children with Cerebral Palsy[edit | edit source]
This table highlights the problems that children with Cerebral Palsy experience in different areas.
| Neurological | Musculoskeletal | Associated Problems |
|---|---|---|
|
|
|
This image gives a nice pictorial overview of the problems experienced by children with CP.
Associated Problems[edit | edit source]
Cerebral palsy in itself can significantly impact upon the child. Many associated conditions also need to be managed. As a Health Care Professional, it is essential to also understand these associated conditions and think about how these might impact or influence your management strategies when working with the child.
Diagnosis[edit | edit source]
Cerebral palsy is one of the main causes of childhood disabilities, with many different signs, symptoms, and challenges. There is no one test to confirm if a child has cerebral palsy or something else. There is no blueprint of interventions for a child with cerebral palsy and each child is different and unique. Classification of gross motor, fine motor and communication will help medical professionals and the family to better understand the abilities of the child and what to focus on for interventions.
The diagnosis of cerebral palsy is based on a clinical description. The diagnosis is not based on the result of a (biological) test or on imaging findings. Consequently, the diagnosis can be subject to some degree of variability. This means that two paediatricians may disagree on a diagnosis of CP for the same child. It is sometimes difficult for even professionals to differentiate between bilateral spastic cerebral palsy and Dyskinetic cerebral palsy.
Ideally, a paediatrician or neurologist will give the diagnosis but some children with CP in developing countries have never seen a doctor. There are also many children in developing countries with CP who have seen many doctors previously but with no good explanation of the meaning and consequences of the diagnoses.
Life Expectancy[edit | edit source]
Mortality in CP is extremely variable. Life expectancy is normal in most diplegic and hemiplegic children who receive adequate medical care and have strong family support. Some severely affected quadriplegics die of malnutrition, infections or respiratory problems before reaching adolescence. In some very poor and poor resource areas children with cerebral palsy may not reach the age of 5 years.
Interventions with Cerebral Palsy[edit | edit source]
Outcomes in early childhood provide clinicians with development information about the children born extremely preterm (EP, <28 weeks’ gestation), but outcomes at school-age are more informative of life-long functioning. According to the review[12], children born extremely preterm at school age have substantially higher rates of intellectual impairment, more neurodevelopmental disability, poorer health-related quality of life, poorer executive, academic and motor function than term-born controls. Understanding and knowledge of a range of important school-age outcomes could help target interventions specifically, focusing periods before, during, after birth, and throughout the lifespan.
The aim and types of interventions are unique for each child with CP because their needs are all different depending on the level of disability. This table gives a great overview of the aims of treatment/interventions for each level of disability.
| Mild | Moderate | Severe |
|---|---|---|
| Intervention will focus of appearance and integration | Intervention will focus on independence and self-care skill | Intervention will focus on comfort and enhanced care |
Communication[edit | edit source]
Communication is necessary to express thoughts, feelings, and needs. Every individual with CP needs a way to communicate to be part of the family and the community. If the child can produce comprehensible sounds and syllables by 2 years of age, they will probably have normal verbal communication but considerations need to be made for those whose communication skills are severely affected. Alternative methods such as communication methods such as simple communication boards in children who have difficulty speaking.
Activities of Daily Living (ADL)[edit | edit source]
Activities of daily living are self-care activities such as feeding, toileting, bathing, dressing, and grooming in addition to meal preparation and household maintenance. Dyskinetic and total body involved children have problems of dexterity and fine motor control that prevent independence in activities of daily living. Hemiplegic and diplegic children can become functional in these areas. They sometimes need the help of (occupational) therapy. Family attitude is a critical factor determining the level of independence of a child. Overprotection results in a shy and passive individual who has not gained self-care abilities.
Mobility[edit | edit source]
Children have to explore their surroundings to improve their cognitive abilities. Mobilisation is crucial for the young child with a disability to prevent secondary mental deprivation. The use of wheelchairs or other mechanical assertive devices can help to promote independent mobility in the community if the child cannot mobilize through walking. Mobility is important to function in fast-paced societies and people who have difficulty moving are always at a disadvantage. In the adult, becoming an independent member of the society and earning a living depends upon independent mobility. Families view ambulation as the most important issue during childhood. Every effort must be made to increase the child’s ability to walk; however, walking depends more on the extent of the child’s neurological impairment rather than the amount of physical therapy, surgery or bracing that they receive. The child can achieve his/her own maximum potential with practice.
Focus on ambulation should not result in neglecting communication and cognitive development. Priorities change in adolescence as they need education, independence, and active social life. Although ambulation is still important, it is needed less to function. Learning how to use computers may benefit the adolescent in the long term rather than being able to take a few assisted steps.
Mobility is important for the child, whereas social identity and independence are more valuable for the adolescent. A trial protocol aims to estimate the feasibility of a Dance PaRticipation intervention for preschool-age children (3 years corrected age) born extremely preterm (EP)/extremely low birth weight (EBLW) with motor impairment[13].
International classification of functioning, Disability, and Health (ICF) can be used to describe the treatment approach in CP. Please see the link below to understand better.
Additional Resources[edit | edit source]
- Child Development and Development Delay
- Cerebral Palsy
- Hambisela_Module_1_Introduction In: Getting to Know Cerebral Palsy: A learning resource for facilitators, parents, caregivers, and persons with cerebral palsy
References[edit | edit source]
- ↑ SCPE. Dev Med Child Neurol 42 (2000) 816-824
- ↑ Mayo clinic Infant jaundice Available from: https://www.mayoclinic.org/diseases-conditions/infant-jaundice/symptoms-causes/syc-20373865 (last accessed 1.11.2019)
- ↑ Chukwukere Ogoke C. Clinical Classification of Cerebral Palsy [Internet]. Cerebral Palsy - Clinical and Therapeutic Aspects. IntechOpen; 2018
- ↑ Morris C. Definition and classification of cerebral palsy: a historical perspective. Developmental Medicine & Child Neurology. 2007 Feb;49:3-7.
- ↑ Morris C. Development of the gross motor function classification system (1997). Developmental Medicine & Child Neurology. 2008 Jan;50(1):5-5.
- ↑ Palisano RJ, Avery L, Gorter JW, Galuppi B, McCoy SW. Stability of the Gross Motor Function Classification System, Manual Ability Classification System, and Communication Function Classification System. Dev Med Child Neurol. 2018 Oct;60(10):1026-32.
- ↑ Can Child. GMFCS - E&R Gross Motor Function Classification System - Expanded & Revised. Available from: https://canchild.ca/en/resources/42-gross-motor-function-classification-system-expanded-revised-gmfcs-e-r
- ↑ Bax M, Goldstein M, Rosenbaum P, Leviton A, Paneth N, Dan B, et al. Proposed definition and classification of cerebral palsy, April 2005. Dev Med Child Neurol. [Review]. 2005 Aug;47(8):571-6
- ↑ Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M, Damiano D, et al. A report: the definition and classification of cerebral palsy April 2006. Dev Med Child Neurol Suppl. 2007 Feb;109:8-14
- ↑ Emma Giles. Khan Academy - Types of Cerebral Palsy Part 1: Spastic. Available from: http://www.youtube.com/watch?v=cR_pX8RE95E [last accessed 13/08/16]
- ↑ Emma Giles. Khan Academy - Types of Cerebral Palsy Part 2: Dyskinetic & Ataxic. Available from: http://www.youtube.com/watch?v=Z7TwzSHnmCk [last accessed 13/08/16]
- ↑ Doyle LW, Spittle A, Anderson PJ, Cheong JL. School-aged neurodevelopmental outcomes for children born extremely preterm. Archives of Disease in Childhood. 2021 May 24.
- ↑ Cameron KL, McGinley JL, Allison K, Fini NA, Cheong JL, Spittle AJ. Dance PREEMIE, a Dance PaRticipation intervention for Extremely prEterm children with Motor Impairment at prEschool age: an Australian feasibility trial protocol. BMJ open. 2020 Jan 1;10(1).